PET scans for Alzheimer's could bring benefit to more patients
by Ryan O'Hare
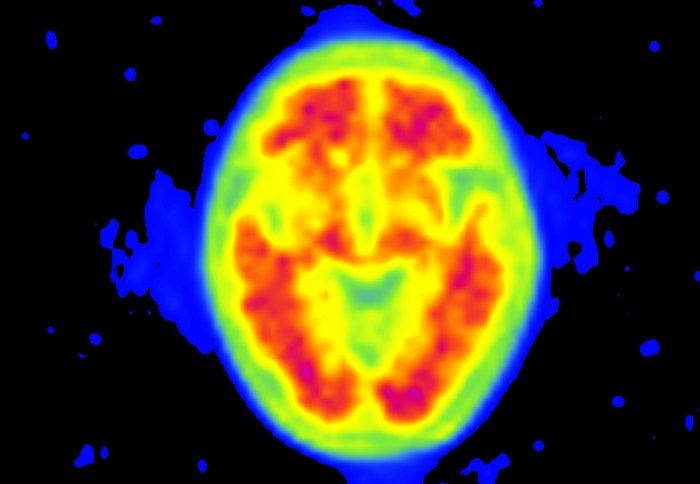
PET scans can spot amyloid in the brain (pictured)
An imaging tool honed to spot rogue proteins in the brain could benefit some patients with suspected Alzheimer's, according to a new study.
The technique, called positron emission tomography (PET), is already used in hospitals to generate 3D images of organs and internal structures, helping doctors to spot signs of disease and confirm diagnoses. However, its use in patients with Alzheimer’s disease has been largely limited to research studies until recently.
In a paper published this month in the Journal of Neurology, Neurosurgery and Psychiatry, a team from Imperial College has shown the scale of the real world impact the scans have in investigating patients with dementia, using one of the largest group of patients to date.
Our study is the first demonstration of how this tool can be used at this scale in hospital patients
– Dr Paresh Malhotra
Senior Clinical Lecturer and Consultant Neurologist
PET scans involve patients being injected with a specially designed radioactive tracer before they enter the scanner.
Depending on the design of the tracer, the scan can then highlight different parts of the body and different functions, such as how active a tissue is, based on the amount of oxygen or glucose it metabolises.
While PET scans have long been used to image tumours, clots and blood flow in the brain, scientists have also been able to adapt the tool to show the build-up of misshapen proteins, called beta-amyloid, which are characteristic of Alzheimer’s disease – the most common form of dementia.
By using a radioactive tracer designed to stick to the protein, the PET scans can detect this hallmark of disease, giving a visual confirmation of disease symptoms in the patient’s brain.
In the latest study, researchers reviewed data from 100 patients scanned as part of their diagnostic work-up, with scans carried out through the Memory and Cognitive Disorders Services at Charing Cross Hospital.
They found that using the modified technique, called Amyloid-PET imaging (API), had a significant impact on how patients were managed and in some cases was even enough to overturn a misdiagnosis of Alzheimer’s. In a number of cases they were also able to confirm Alzheimer’s in individuals who had not yet been given a diagnosis because, where their clinical features were not typical of the disease.
Data from the scans showed the presence of amyloid in 49 of the cases. It also led to a change in diagnosis of 30 patients, who had been diagnosed as Alzheimer’s, but lacked the amyloid build up in their brains – meaning they may have had a different form of dementia or another health condition altogether.
They suggest that using this approach in a clinical population is most useful in younger patients with suspected early-onset dementia, where the clinical features may not be as typical as in elderly patients with the disease.
In addition, using PET in patients with an uncertain diagnosis was able to reduce the need for other, more invasive clinical assessments used to spot amyloid, such as analysis of cerebral spinal fluid collected from the spine.
Clear benefit of amyloid PET
Commenting on the use of PET imaging for Alzheimer’s patients, study author Paresh Malhotra, a senior clinical lecturer at the College and a consultant neurologist at Charing Cross, said: “Our study is the first demonstration of how this tool can be used at this scale in hospital patients.
“While the scans were able to help tailor treatments for patients based on their pathology, we found that patients needed fewer investigations following their PET scan, as the diagnosis had already been confirmed.
"All cases were discussed by a team of Neurologists, Nuclear Medicine Physicians and Radiologists before having a scan, enabling us to make sure that we were scanning appropriate patients.”
According to the researchers, the study demonstrates the clear benefit of using API in the battery of tests used to diagnose patients with cognitive impairment.
They add that the high cost and limited availability of this type of PET scan make it unrealistic that it would be used as a standard test for patients on the NHS.
However, it could be applied to a subset of patients on the NHS who meet the relevant criteria, helping doctors to clarify their diagnoses and ensure they receive the right treatment and reducing the number of follow up tests they need to confirm their diagnosis.
Scanning was funded by the National Health Service and Imperial College NHS Healthcare Trust.
-
‘Clinical utility of amyloid PET imaging with (18) F-florbetapir: a retrospective study of 100 patients’ by Carswell, CJ et al. is published in the Journal of Neurology, Neurosurgery and Psychiatry.
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Ryan O'Hare
Communications Division