Frontline insights
The Imperial academics at the centre of the NHS response to COVID-19
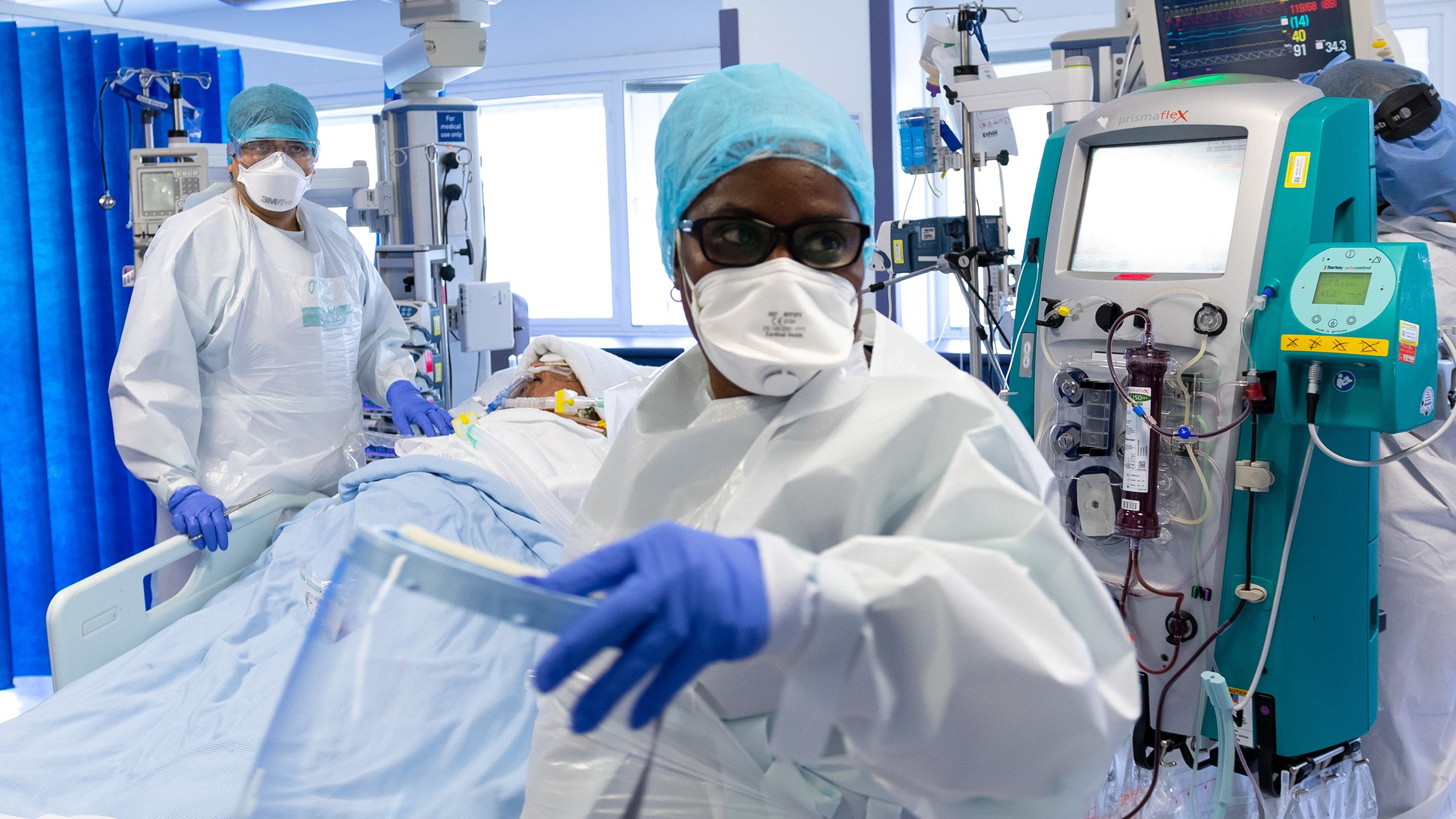
On 23 March the UK went into lockdown as cases of COVID-19 increased and the country headed towards the peak of the virus which has so far resulted in over 40,000 deaths.
As people were told to stay in their homes to contain the spread of the virus, hospital staff responded swiftly to the pandemic and the escalating crisis. More than 30,000 beds were freed up across England and non-urgent services paused to manage and treat the influx of COVID-19 patients .
Despite these efforts, more support was needed to ensure that there were enough members of staff at NHS hospitals to provide care for patients if staff became ill or needed to self-isolate.
Around 200 clinical academics at Imperial College London who work as researchers and clinicians have volunteered to be seconded full time to London hospital Trusts including Imperial’s NHS partners – Imperial College Healthcare NHS Trust, Royal Brompton & Harefield NHS Foundation Trust and Chelsea & Westminster Hospital Foundation NHS Trust Hospitals – to treat COVID-19 patients, conduct virtual outpatient clinics and to carry out research on the disease which could lead to new breakthrough treatments.
Eleven clinical academics have shared their experiences of joining the NHS frontline during the peak of the pandemic and how they are shaped by this experience. They talk about the many challenges and difficulties of working in hospitals during this time as well as the moments of hope, joy and camaraderie and how the public’s support has been gratefully received whilst tackling this pandemic.

"The team camaraderie is something positive that we can take away from all this"

Professor Waljit Dhillo
Professor in Endocrinology & Metabolism at Imperial and Consultant Endocrinologist at Imperial College Healthcare NHS Trust. He has been managing and treating COVID-19 patients at Charing Cross Hospital.
“I'm part of the medical team managing COVID-19 patients at Charing Cross Hospital, which is split into five specialist teams, known as pods. I’m working as an Acute Medicine Consultant in the blue pod and we have around 50 patients split across two wards. I lead a daily consultant ward round and also manage the team.
One of the most challenging aspects of the pandemic has been the fact that, due to the risk of infection, relatives are unable to visit their loved ones regularly. Normally, we would be talking to the relatives about the patients’ condition and involving them in decisions.
It’s a difficult time anyway for families when their loved ones go to hospital but now the anxiety is heightened when they can’t visit. The way we communicate with our patients’ families had to change completely overnight and the NHS has responded extremely quickly by establishing family liaison teams and by making use of IT solutions to facilitate video calls from the bedside.
Working with the same team every day has been great as everyone has got to know each other well – from consultant to junior level – which is important for the nature of the work we’re doing. The juniors are having more contact with the seniors than they normally would. The team camaraderie is something positive that we can take away from all this.
The team has been well-supported with medical students volunteering and the latest cohort of graduating doctors who recently joined the wards. As we’re faced with staff shortages, the volunteering students have been able to support with basic tasks like feeding patients, and they've been a tremendous help.
However, we’ve seen a substantial drop in daily cases of conditions such as heart attacks and strokes and people are presenting much later as they’re too scared to go into hospital. I would say to the public that the NHS is still open for its ‘usual’ service and if people have a serious medical problem, they should not avoid coming in.
The worry is all the other work we’re not doing – minimal outpatient work, and cancer diagnoses are all delayed as there are no new screenings.
The worry for all of us is that we may be coping with this emergency now, but we need to look at the impact on those with non-COVID related illnesses."

"It’s been a tough and unreal experience overall"

Dr Rahma Elmahdi
Honorary Research Associate at Imperial and Junior Doctor in General Medicine. She has been working on COVID-19 wards at North East London NHS Foundation Trust.
“I usually work full-time in epidemiology research and was aware of the impact the outbreak was having in the UK. Once lockdown started, and we were advised to work from home, I decided that the most useful contribution I could make as hospital pressures increased would be returning to clinical work. It wasn’t a hard decision but simply what I was trained to do.
It’s been a really tough and unreal experience overall. There has been a great deal of solidarity among the staff on the frontline and I’ve been consistently inspired and proud of the dedication and energy of all my colleagues on the wards; everyone from the student nurses recruited in the last year of their degree to the consultants on Intensive Therapy Units (ITU) providing (re)training for us.
Although the sheer pressures and confusion coupled with the suffering experienced by our patients has been hard to cope with, the public support and video calls with my friends and family have really been essential for staying positive and going back and doing the same again.
Despite the challenges, there are some really lovely patient stories. My favourite story was seeing a married couple in their seventies, who were admitted one after the other onto our COVID-19 ward – despite the husband being very ill with the infection, he never failed to ask about how his wife was doing on the daily ward round. The team were delighted when he was well enough to visit his wife while they were both inpatients and when we were finally able to discharge them together after three weeks on the ward.
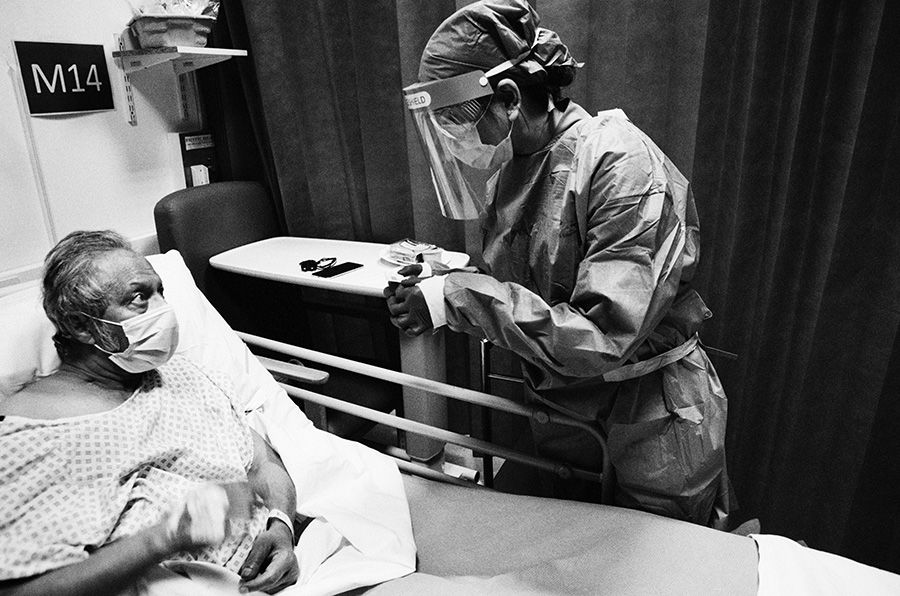
Clinician at a patient's bedside at Charing Cross Hospital A&E (Giles Duley)
Clinician at a patient's bedside at Charing Cross Hospital A&E (Giles Duley)
There are also painful stories, which are important to tell in memory of those patients. One man who was admitted to hospital from a care home told me how he wished to see his family before he passed. He tragically never had this opportunity as he deteriorated rapidly and the first time we were able to contact his family was to sadly inform them of his passing.
I’ve not been able to live at home with my family as my mother is in a high-risk group. I’ve been so grateful for the accommodation offered to me for free whilst I work on the wards and all the meals and cake that we’ve received to power us through our shifts. The real gems have been the hand cream we’ve had donated – fantastically useful for my dry and chapping hands after the constant washing.
One of the things that has worried me from the start of this outbreak is the disproportionate number of black and minority ethnic healthcare colleagues who have died.
The first doctors to die of COVID-19 were from Sudan, like me and my family, so this was felt acutely in our community. For anyone who works in health, the two to three-fold increased risk of death from COVID-19 in BAME colleagues is not surprising.
I suspect that a large contributor to this disparity is the racialised socio-economic hierarchy that manifests throughout our society. Sadly, no matter your seniority in the NHS, if you’re from a BAME minority group, your outcomes will be worse than your non-minority colleagues, and now the stakes are higher. Like many of my colleagues, I’m keenly waiting for the outcomes of the inquest led by Professor Kevin Fenton into this and hope for a recognition of the toxic impact of racialised inequalities in the NHS and real change that protects those of us who are most at risk and brings our voices to the fore in order to do so.”
"It is fantastic how everybody has rallied behind the NHS"

Dr Ruud Nijman
NIHR Academic Clinical Lecturer at Imperial in Platform Science and Bioinformatics and Registrar in Paediatric Emergency Medicine at the London Deanery. He has been working at St Mary’s Hospital to treat COVID-19 patients in intensive care.
“I was greatly looking forward to a period of academic time and working on two large European studies called PERFORM and DIAMONDS, looking at biomarkers in children with acute infections. When COVID-19 happened, I started off working in the paediatric emergency department at St Mary’s Hospital. Then, due to a large reduction in children attending the emergency department, I was asked to support the team in the paediatric intensive care unit, which was repurposed to look after critically unwell adults with COVID-19. In the paediatric intensive care unit, we have all had to adjust our way of working and retrain. Although we had experience in intensive care medicine, most of us didn’t have recent experience of caring for adults.
There were some very difficult times in the unit with very sick patients but the team has been incredible; everybody has really pulled together to make things happen. Looking after critically unwell children is different to looking after critically unwell adults, but a lot of the basic principles of intensive care medicine still apply.
The structure of clinical approach and things like using a ventilator and inserting central lines remain pretty much the same, but other aspects are ’new’: adults are a lot bigger, which makes the clinical handling different. We are used to using very small cannulas and lines and different dosing and types of drugs for children and we need to think about different side effects and blood markers in adults. There have been e-learning modules and webinars offered by the Trust and resources from the unit itself. It has been invaluable to experience the logistical challenge of restructuring and have this additional experience of looking after adults in intensive care.

Dr Ruud Nijman working on a COVID-19 ward at St Mary's Hospital (Thomas Angus)
Dr Ruud Nijman working on a COVID-19 ward at St Mary's Hospital (Thomas Angus)
Working in full PPE makes non-verbal communication really difficult.
It has been really challenging to show empathy for each other and for patients and their families whilst working with our equipment on. That is something that will stay with me: how did we look after each other in these difficult times, when you can’t show facial expressions? It makes you realise how special the way we look after patients is without PPE.
Over the past few weeks, we have seen some really sick children and initially we could not quite relate how they presented with the typical Coronavirus symptoms in adults. Most did not have respiratory symptoms, but they had multi-organ involvement and ended up needing specialised care from our infectious diseases team or even intensive care. This arising clinical syndrome, a hyperinflammatory response that we believed might be related to Coronavirus, was escalated to NHS England and the Royal College of Paediatrics, leading to national efforts to try to understand what was happening.

Staff on the night shift at St Mary’s paediatric ICU (PICU) check a patient’s monitor (Giles Duley)
Staff on the night shift at St Mary’s paediatric ICU (PICU) check a patient’s monitor (Giles Duley)
The paediatric infectious diseases and paediatric intensive care team have been instrumental in formulating a case definition of this Paediatric Inflammatory Multisystem Syndrome and driving recommendations for the clinical management of these children. The DIAMONDS study, led by Professor Michael Levin, is now recruiting children across sites in the UK and Europe and the team is undertaking essential research to better understand this new inflammatory condition in children. I am truly humbled to be part of these world-leading teams, both clinically and academically, where studies are integrated into day-to-day clinical care.
It is fantastic how everybody has rallied behind the NHS and how Imperial Health Charity has coordinated the charity efforts. I have not had a shift where I was not offered a hot lunch and often there is food to take home as well. Sometimes it is difficult to get the shopping done or you don’t have the energy to cook, so knowing that when you go to work that that has been provided has really helped.”
"As an oncologist,
I deal with a vulnerable group of patients"

Dr Rohini Sharma
Reader in Clinical Pharmacology and Medical Oncology at Imperial and a Consultant Medical Oncologist at Imperial College Healthcare NHS Trust. She has been managing cancer patients.
“As an oncologist, I deal with a very vulnerable group of patients many of whom are shielding and are not able to travel to hospital for their routine appointments. These patients are often scared both about catching COVID-19 and about their cancer getting worse during the pandemic. I feel that it is really important to try to support patients through this difficult time both clinically and emotionally.
My typical role within the NHS is to manage liver cancer and neuroendocrine cancer – a rare tumour that can develop in many organs of the body. Additionally, I lead the research efforts in liver cancer and I’m responsible for allocating patients to clinical trials. Since the onset of the pandemic our entire way of working has changed. It has become necessary to manage our patients remotely and conduct my clinics via telephone, something that has been challenging but to which we have had to adapt. A number of treatments have also had to stop as service provision has focused on allocating services to COVID-19.

Dr Rohini Sharma performing remote consultations during the COVID-19 pandemic (Thomas Angus).
Dr Rohini Sharma performing remote consultations during the COVID-19 pandemic (Thomas Angus).
My hospital-based clinical care has involved caring for inpatients and on-call provision for the oncology wards at Charing Cross Hospital. The remainder of my time has been spent off-site, which has allowed me to focus on my research, both within oncology and particularly the impact of COVID-19 on patients.
During the initial phase of the pandemic we had to have difficult discussions with patients regarding palliative therapy instead of chemotherapy – as chemotherapy can affect the immune system. These patients were most vulnerable to catching the virus. Surgical lists were also cancelled which obviously meant that many cancer patients could not undergo any surgical treatments during this time.
A lot of cancer patients decided to stop treatment and for many, we were simply unable to offer treatment.
I found these discussions very difficult, particularly as it became necessary to have a number of these conversations via telephone rather than in person and without the ability to directly support patients faced with such life-changing decisions.
A number of my colleagues have also been infected with the virus, some with significant symptoms and prolonged courses of sickness. It was very difficult hearing how sick they were and how little there was that could be done for them. Though thankfully for them and their families, they have managed to recover, it has been a very frustrating situation and I look forward and hope that we gain control of the pandemic soon.”
"We have seen a massive rate of coronavirus infection in patients with kidney failure"

Professor Jeremy Levy
Director of the Clinical Academic Training Office at Imperial and Consultant Nephrologist at Imperial College Healthcare NHS Trust. He has been managing the treatment of kidney patients as well as treating patients on COVID-19 wards at Hammersmith Hospital.
“Patients on dialysis often need to come in for treatment three times a week so cannot isolate themselves and kidney transplant patients need their bloods testing very regularly, which cannot be done remotely. We have also seen a massive rate of coronavirus infection in patients with kidney failure for unknown reasons. This has led to significant concern and anxiety among patients, and an enormous workload for NHS staff, such as trying to keep infected and non-infected patients separate.
I am doing many more telephone and video clinics now rather than seeing patients face to face, as well as more inpatient work, such as looking after patients sick enough to need admitting to hospital on our COVID-19 wards.
I have also been helping on our dialysis units with the actual preparation for dialysis and patient care – normally done by our nursing staff – as well as lots of work to support the change in the care we are delivering.
Over the last few weeks, there is a clear difference between some areas of the hospital being empty and quiet – no visitors, no routine hum and activity. This is in contrast to entering the COVID-19 wards where staff are so busy, anxious but coping.
Patients are often delighted we can undertake much work through telephone calls, but also have been telling me they miss out on social interactions, even in the normally over-stretched outpatient clinics.
Some patients are getting operations quicker than normal since the surgical teams have had to cancel their normal routine work, but sadly too many of my patients are coming into hospital very sick, and sadly dying, and not being able to have their families with them which is heartbreaking.
I have also been trying to support the hundreds of clinical colleagues undertaking research training at Imperial through this period. I have been leading programmes to ensure they don’t lose their research funding and that they can be primed to start their research careers in due course when things get easier."

Professor Jeremy Levy wearing personal protective equipment
Professor Jeremy Levy wearing personal protective equipment
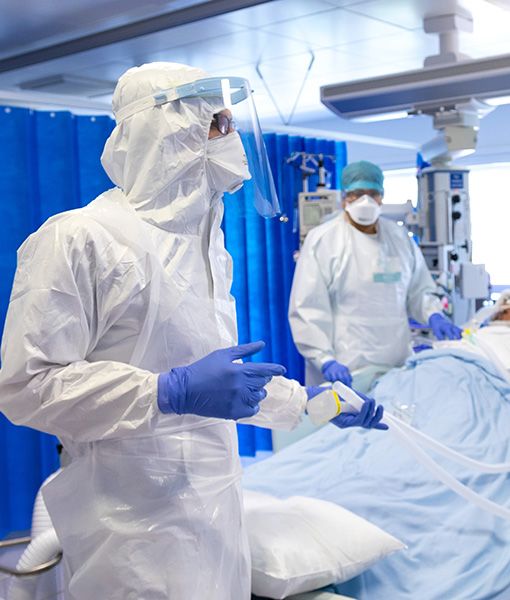
Clinical team at a COVID-19 Intensive Care Unit at St Mary's Hospital (Ben Pruchnie)
Clinical team at a COVID-19 Intensive Care Unit at St Mary's Hospital (Ben Pruchnie)
"I feel privileged to work alongside my general practice team"

Professor Sonia Saxena
Professor of Primary Care at Imperial College London and a GP at Chartfield Surgery in Wandsworth, is supporting primary care services.
“I feel my first duty is to the community I have served as a GP for over 25 years. Everyone has risen admirably to the challenges COVID-19 has thrown at us in our practice in south-west London. I am seeing both ‘hot cases’ in our practice and continuing usual care.
We have adapted to new ways of working with people at home and physically distanced staff rounds, cascading communications and a general willingness to do the right thing, whatever that is.
At the same time, I lead the Child Health Unit at the School of Public Health at Imperial. The initial weeks were difficult for some of my staff and students to grasp what was really happening. I think they variously went through shock, anger, denial and eventually some form of acceptance. We quickly organised ourselves with weekly crisis meetings, mid-week tea time catch-ups and morale-building activities.
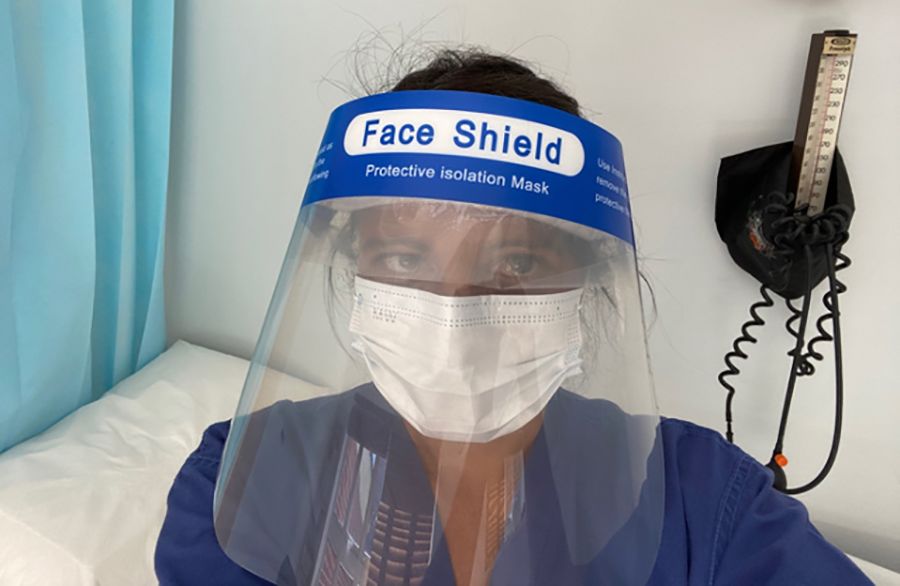
Professor Sonia Saxena wearing a protective face shield
Professor Sonia Saxena wearing a protective face shield
We have launched the Imperial Child Health COVID investigation working group. Our focus is to ensure that children and young people’s health is not compromised during the pandemic and its aftershocks. Especially with containment and school closure, they have lost their voice and become invisible to much of the research and policy agenda.
The main thrust of our work was to deploy our existing team to brainstorm priorities for urgent child health research, apply for real-time data to inform our hypotheses about health impacts and link with UK and European partners to join public health efforts to combat the virus' effects. So far, we have published several thought pieces on policy, and hope to continue with several projects in progress.
I feel privileged to work alongside my practice team and I am proud of my research teams for pulling together and being productive in difficult working conditions. I feel a great optimism for the lessons that we all have learned about ourselves, our values and priorities. Above all, this sharp shock will teach the next generation how to be resilient and bounce back."
"Only incredible team work has enabled the service to expand to its current levels"

Dr Antonio de Marvao
MRC Chain-Florey Clinical Lecturer in Cardiology at Imperial and Senior Fellow in Cardiovascular Imaging at Royal Brompton Hospital. He is supporting the intensive care team looking after COVID-19 patients.
“As part of the national response to COVID-19, non-emergency cardiac tests and procedures had to be postponed. Due to the respiratory and critical care expertise available on site, Royal Brompton — the largest specialist heart and lung centre in the UK — has seen a very significant increase in the number of patients transferred from other hospitals. The intensive care capacity was greatly expanded and I was redeployed from cardiology and research to the main ICU to support the intensive care team looking after COVID-19 patients.
Although I am approaching the end of my training in cardiology and general medicine, moving to such a specialised ICU required a very intensive period of learning new skills and ongoing support from the intensivists. I’ve received training in how to look after patients receiving Extracorporeal Membrane Oxygenation (ECMO) therapy, which is a very specialised machine that oxygenates the blood drained from the patient, which is then returned to the patient when their lungs are unable to do so.
Royal Brompton is one of only five ECMO centres in England for adults with severe acute respiratory failure.
During the COVID-19 pandemic this type of advanced care has been required in unprecedented numbers and only incredible team work across the entire organisation has enabled the service to expand to its current levels. The learning curve is steep and moving from one speciality to a completely different position in another takes some getting used to but the team spirit, mentoring and sense of purpose have been phenomenal.”

Dr Antonio de Marvao wearing full personal protective equipment
Dr Antonio de Marvao wearing full personal protective equipment
"Research is absolutely vital to our ability to fight this epidemic"

Professor Mark Thursz
Director of NIHR Imperial Biomedical Research Centre and Consultant in Hepatology at Imperial College Healthcare NHS Trust.
“Normally, I supervise the infrastructure for delivering clinical research across the Trust and across every speciality, but most of this research had to be closed down at the beginning of the outbreak, apart from a few studies with specific exemptions. All of our focus and resources needed to be used for dealing with the current epidemic. It is my role to participate, help coordinate and ensure the smooth running of any COVID-19 research.
It has been extremely busy, both clinically and from a research perspective. There have inevitably been tensions between the delivery of research and the delivery of clinical care because we anticipated being very short of resources. It became clearer, probably more than at any other time, the need for the two parts of NHS work to be integrated hand-in-hand. It is a completely new disease, so research is absolutely vital to our ability to fight this epidemic and reduce mortality. For example, when clinical services were overwhelmed, we encouraged research nurses to undertake phlebotomy and clinical observations – that level of integration mitigated against conflicts.
Communication is probably one of the key factors in any kind of success. We have managed to keep a good dialogue between the College side and the Trust side of the partnership.
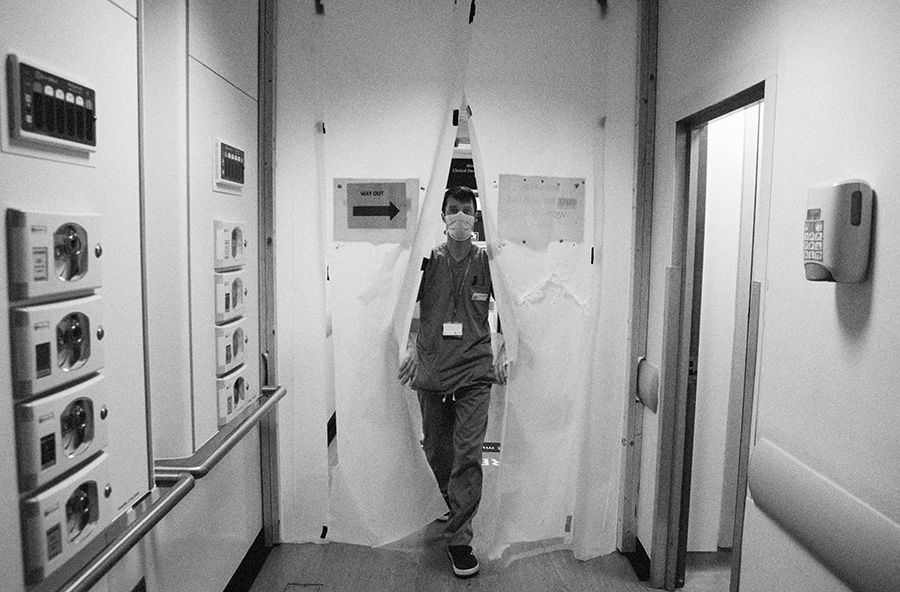
Emergency technical assistant steps into the ‘red zone’ at Charing Cross A&E (Giles Duley)
Emergency technical assistant steps into the ‘red zone’ at Charing Cross A&E (Giles Duley)
As a clinical academic, I have done my own time on the wards and have been running clinics remotely. Being on the wards is great in some ways; there is an excellent camaraderie amongst the clinicians, with people trying to help each other out and support each other. On the other hand, it is very frustrating not to have a specific therapy for the patients that we have been admitting.
We have had a number of patients with liver disease admitted during this COVID-19 crisis. Some were admitted for the usual complications of cirrhosis but unfortunately, some of them got infected while in hospital. This underlines what we have seen in the national and international statistics: people with co-morbidities, particularly in this case with cirrhosis due to obesity and diabetes, are incredibly susceptible to very severe COVID-19 infections. It is very sad that the transmission rate even within hospitals is very rapid.
We have been one of the largest recruiters to the platform trials analysing different treatments for COVID-19, with over 2,700 patients recruited into research studies. I have seen clinicians and academics across the Imperial College Academic Health Science Centre (AHSC) coming forward with mostly very sensible ideas, hypotheses, therapies and interventions.
It is wonderful to work in such a rich academic environment, where people are looking to do everything they can to improve clinical outcomes.
The support both inside and outside the hospital has been wonderful. However, if I had a choice between public adulation and having PPE, testing and a proper policy for dealing with the pandemic, I’d go for the latter. What the public can do to help most now is to hold the government to account, working through their MPs to question why we have had such appalling mortality statistics.”
"This experience has reaffirmed my faith in the medical profession"

Dr Victoria Salem
Senior Clinical Research Fellow at Imperial and Consultant in Diabetes, Endocrinology and Acute Medicine at Imperial College Healthcare NHS Trust. She has been working on the frontline at Charing Cross Hospital to treat COVID-19 patients.
“In my normal day job, 80 per cent of my time is laboratory-based and 20 per cent of my job is clinical, on the acute medical unit at Charing Cross Hospital. When the epidemic struck, my lab more or less closed down but it was a no-brainer to do much more work in acute medicine; the minute we knew this was coming, everybody turned their attention to how they could best support the NHS. Now, I am essentially working full-time in frontline patient care.
Some of my shifts are in the emergency department and others are on the acute medical unit, looking after patients who have come in with COVID-19 but also those who have other medical emergencies. We have had to completely restructure the hospital and I look after a ‘pod’ of junior doctors at Charing Cross Hospital who have pulled together to look after a group of COVID-19 wards. It has been absolutely fantastic to work with colleagues that we never usually come into contact with. There is a huge amount of camaraderie across disciplines and we are learning a lot from one another.
This experience has really reaffirmed my faith in the medical profession and reminded me why I did medicine in the first place. The sense of satisfaction and pride that you are doing an important job, making a difference and caring for people, is immense. Psychologically and emotionally it can be very challenging because it is remarkable how little we know about this disease and it is very different to anything we have ever seen before. I have never before in my twenty years of clinical practice worked in an environment where the guidelines are changing weekly, which is very difficult for a profession that is steeped in a culture of evidence-based practice.
One of the greatest tragedies of this disease is that people suffer alone with it.
We have made a real effort to try to engage with patients a lot more in ways we do not normally have the time to – reading the newspapers, even doing massages and shaving beards on our ward rounds – the sorts of things that family members would do when visiting their relatives in hospital. That has been a very positive experience, especially for the junior doctors, to remember that yes, we are academics, but ultimately, we are all carers as well."
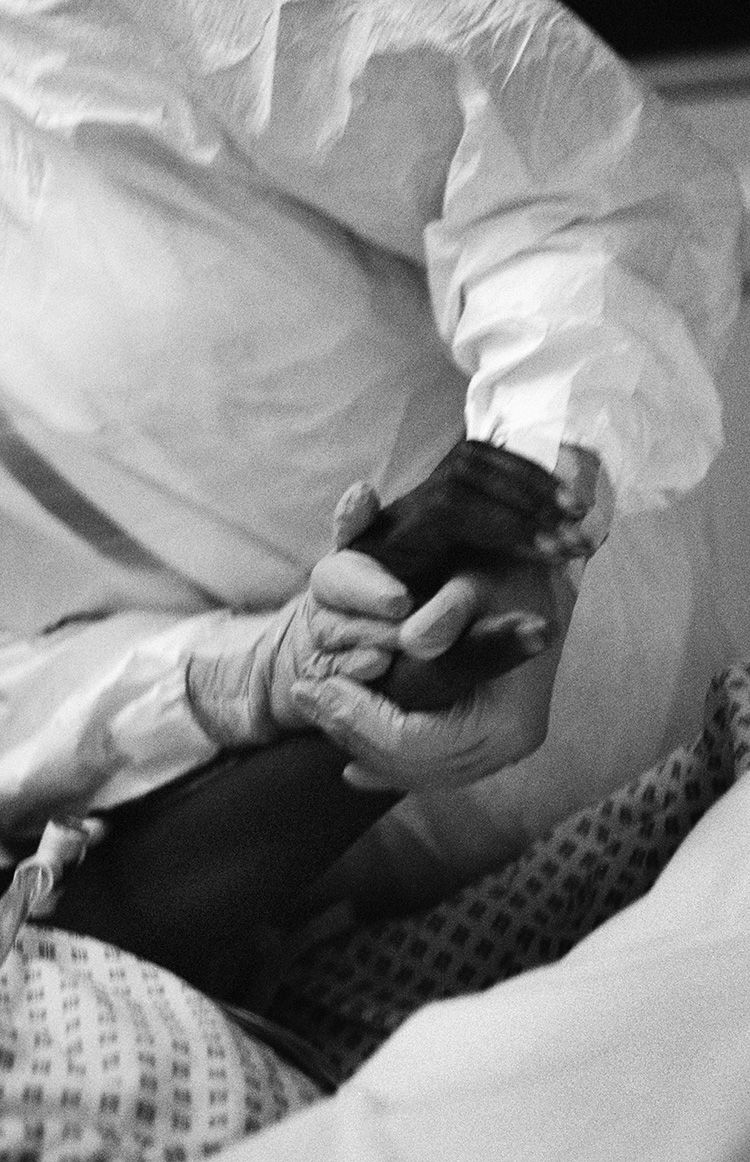
A doctor holds the hand of a ventilated patient in St Mary’s PICU (Giles Duley)
A doctor holds the hand of a ventilated patient in St Mary’s PICU (Giles Duley)
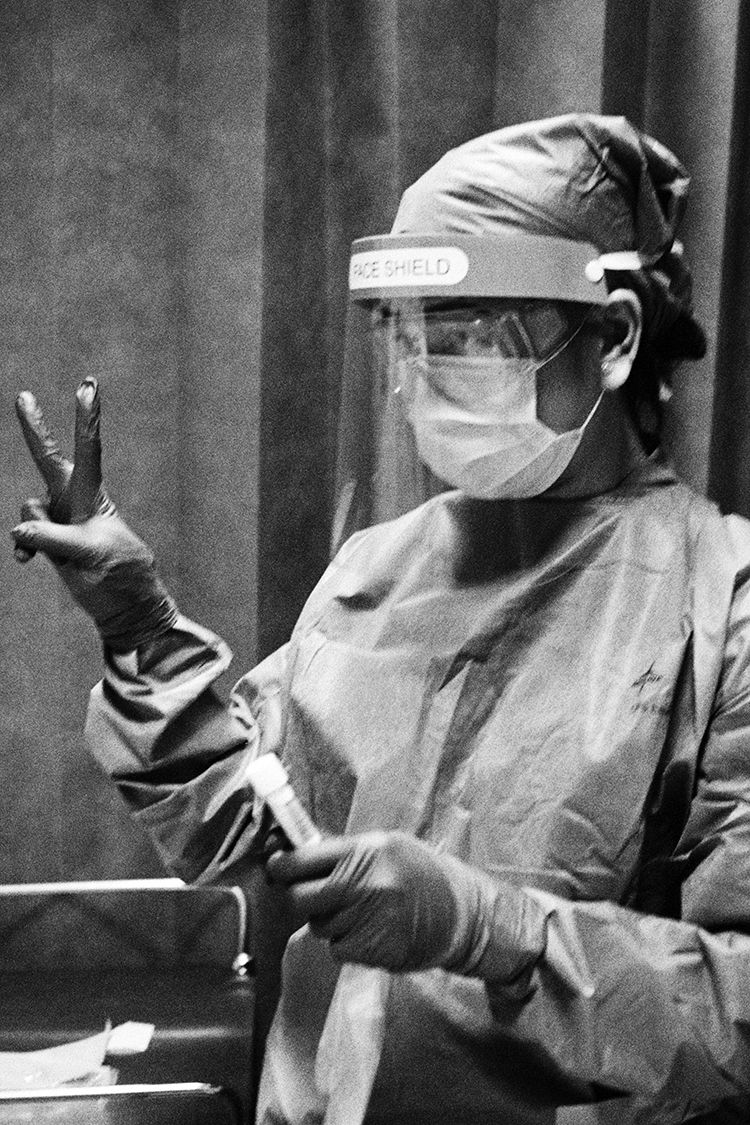
At Charing Cross Hospital A&E, a nurse prepares a patient for a swab test (Giles Duley)
At Charing Cross Hospital A&E, a nurse prepares a patient for a swab test (Giles Duley)
"I hope this level of support for our health service continues after the crisis is over"

Dr Harry Leitch
Head of the Germline and Pluripotency Group at the MRC London Institute of Medical Sciences at Imperial College London and Neonatal Registrar at Imperial College Healthcare NHS Trust. He is working at the Neonatal Unit at St Mary’s Hospital and Queen Charlotte’s & Chelsea hospitals.
“I volunteered to use my academic time to return to the Neonatal Intensive Care Unit (NICU), where I’ve been working as a neonatal registrar between St Mary’s Hospital and Queen Charlotte’s & Chelsea Hospital. Although babies and children seem to be overall less severely affected by COVID-19, some do still become unwell, and there have been a few premature deliveries due to maternal COVID-19.
There are also many staff members who are ill, self-isolating or shielding. Neonatal doctors have to attend deliveries from COVID-19-positive mothers, if the baby requires resuscitation or is premature – which perhaps explains some of the transmission to staff in this speciality. The work also involves difficult procedures and it is simply impossible to social distance when you are treating a tiny premature baby.
I am now essentially 100 per cent clinical - split 50:50 between Clinical Genetics and NICU, and also helping out on the on paediatric haematology/bone marrow transplant ward too.
There have been weeks when I’ve worked across three different specialities, and even some intermingling. For instance, I’ve helped out with some genetic diagnoses on the neonatal unit.
I’ve been really impressed with the support shown – both by the public and by lots of companies. I’ve often heard the Clap For Our Carers echoing in through the hospital windows, and I’ve enjoyed free or cheap rides to work and food from a number of companies. I hope this level of support continues after the crisis is over, and we can increase investment in the health service and its staff."

Dr Harry Leitch wearing personal protective equipment.
Dr Harry Leitch wearing personal protective equipment.
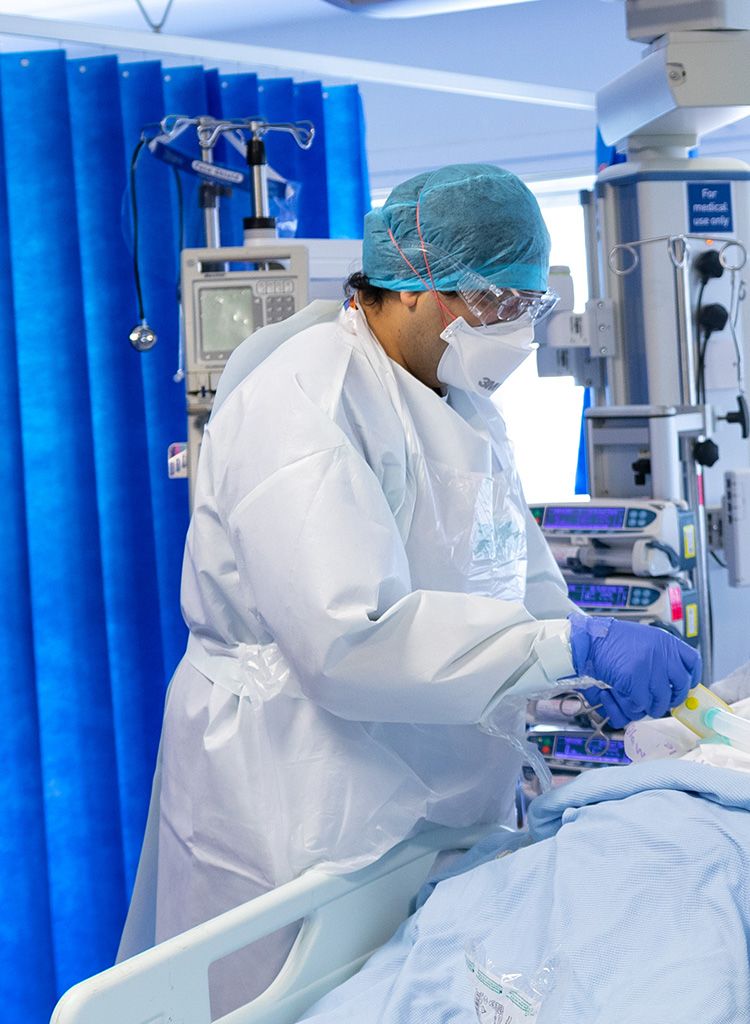
Doctor on an ICU COVID-19 ward at St Mary's Hospital (Ben Pruchnie)
Doctor on an ICU COVID-19 ward at St Mary's Hospital (Ben Pruchnie)
"As an obstetrician, the way I do my work has been turned upside down"

Mr Martin Lupton
Vice-Dean (Education) of the Faculty of Medicine at Imperial and Consultant Obstetrician at Chelsea and Westminster Hospital Foundation NHS Trust. He has been conducting virtual clinics with patients.
“Contributing to the NHS response to COVID-19 is a visceral thing. When you work in a team in a hospital you develop a very close professional relationship with your colleagues. These are the people that you have telephoned for advice at 2am or asked to help you with difficult cases. They are people who you have shared tragedy with and a lot of joy. When the chips are down you would literally do anything to help them.
In my head I know that I must do all that I can to support the NHS and the patients that walk through the door. In my heart I feel a tremendous loyalty toward my colleagues, I do not want to let them down.
As an obstetrician, the way I do my work has been turned upside down. Virtually all my clinical work is now conducted over the telephone. It is an entirely new skill and requires an extraordinary focus on listening. I am learning to hear anxiety, hear uncertainty and make sense of pauses and silences. It is exhausting and fascinating.
My experience at Chelsea and Westminster Hospital has been extremely good. It has been managed with great professionalism. I worry about a number of things, some of them about the well-being of the staff who have been on the frontline for many weeks now. I think for some there is an element of shell shock, and I am not sure how well the system is geared up to manage this.

Staff at Charing Cross Hospital A&E (Giles Duley)
Staff at Charing Cross Hospital A&E (Giles Duley)
As far as the public are concerned, I would ask that they reflect on the value of expertise, science and balanced judgement. I would also ask that they reflect on how we support the University sector and science in the future and consider what level of taxes they are prepared to pay to support the NHS so that it is better prepared for the next pandemic. Most importantly, I would ask that they reflect on the contribution that medical, nursing and other key workers have made to their safety, in particular those who are recent immigrants from the European Union and the rest of the world. We cannot use these people during times of crisis and try to ignore them in times of calm.”

Frontline insights
Words: Maxine Myers, Ellyw Evans and Siobhán Stack-Maddox
Photography: Giles Duley, Imperial College Healthcare NHS Trust | Ben Pruchnie, Imperial College Healthcare NHS Trust | Thomas Angus, Imperial College London | Andy Pritchard, Imperial College London
