Schools Transmission Studies
What is scarlet fever?
Scarlet fever is an infectious childhood illness with sore throat, body rash, and fever caused by Streptococcus pyogenes (group A strep, or ‘Strep A’) but easy to treat with antibiotics.
Scarlet fever is a notifiable infection; peaks of scarlet fever occur in the springtime. Rates in England have risen in the last 10 years to levels seen in the early 1960s for reasons no one is sure of.
Do we need to worry about it?
Although scarlet fever is treatable with antibiotics, rates of rarer but more dangerous group A strep infections can also increase when scarlet fever rates are high. Though very rare, these can be very serious for those affected through devastating effects of sepsis.

How can we stop the spread?
We want to stop transmission of Strep A in outbreaks of scarlet fever. The main age group affected are nursery and reception age children aged 4-6 years.
To do this, we first need to understand whether- and how- Strep A spreads in nurseries.
Could better hand hygiene or different treatments reduce spread? Or better ventilation? Better control of Strep A may ultimately reduce risk of rare but more dangerous infections.
We also need to understand how children become immune to Strep A, and work out if a vaccine against Strep A might one day be the main way of reducing spread of scarlet fever in the classroom.
 What is the study doing?
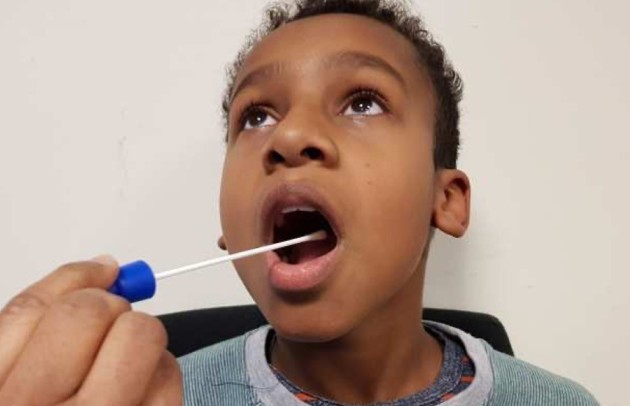
What is the study doing?
We are visiting homes & nurseries with scarlet fever or Strep A cases, to take swabs and other samples from children being treated for scarlet fever, their household contacts, and
healthy classmates. We are also taking samples from the environment to test for Strep A.
What are the findings so far?
Previous estimates suggested less than 4% of healthy children carry Strep A in their throats. In our first study conducted in 2018 and 2019, we found that over one quarter (26%) of healthy classmates carried the same strain of group A strep in the 3 weeks after children in the same class had been diagnosed with scarlet fever. About a quarter of those healthy children who were carriers, and who seemingly had no symptoms themselves, had the same strain of Strep A in their throats for 2-3 weeks and were able to spread it into the air, which might explain how outbreaks continue. Please use this link to read our report from our earlier study published in Lancet Microbe 2022.
333 (20%) of 1,703 households contacted took part in an online survey. All cases received appropriate treatment once scarlet fever was diagnosed. Prior contact with other children with both sore throat and scarlet fever was very common (58% and 67%). Although almost all children diagnosed with scarlet fever received the recommended antibiotic treatment, one-fifth of children were initially thought to have a virus, and so treatment was delayed, potentially leaving them infectious for a few days. From the swabbing study we know that children who are treated do clear the bacteria promptly. Please use this link to read about the results of the survey published in 2021 in BMJ Open.
What can be done?
We saw quite a lot of transmission of group A strep among healthy children, even if their classmates with scarlet fever were properly treated. This means that the infection had already spread by the time a child is diagnosed.
We know from the survey that most scarlet fever cases arose after contacts with either sore throat, which can also be caused by Strep A or scarlet fever (or both). So, detecting and treating sore throats due to Strep A in younger children may be just as important as detecting and treating scarlet fever. Making it easier for doctors to diagnose strep A throat in young children who are 'heavy shedders' with antibiotics too, as it is possible they may not be able to tell us they feel unwell and this may also reduce transmission.
We know that scarlet fever outbreaks are often terminated by school holidays. The COVID-19 pandemic had a marked effect reducing the rate of scarlet fever as well as rates of the rare but more dangerous Strep A infections. Closing schools and nurseries is not a long-term strategy for controlling Strep A, and we did see a rebound in Strep A infections after COVID-19 restrictions were relaxed, in 2022.

What next?
This study has taught us how to work together with schools and nurseries caring for younger children in order to do really important research into transmission of acute infection. Since the rebound in Strep A infections in 2022-2023, people are more aware of Strep A. Having found that transmission rates are much higher than we had expected, we now need to look more closely at how the bacteria are spread between children- taking samples from children and from their environment and people around them. We also need to understand whether some children might have better immunity to Strep A than others of the same age, possibly explaining why they do not get infected like their classmates.
The study is being done by Imperial College London together with UK Health Security Agency. The investigators are Professor Shiranee Sriskandan (Imperial College London), and Dr Deepti Kumar (UKHSA).
The research aspects of the study looking at immune responses are funded by the Leducq Foundation, while the environmental sampling is funded by the Medical Research Council (UKRI).
Our earlier Transmission Study on scarlet fever was funded by the charity Action Medical Research for children. Previous investigators include Dr Rebecca Cordery (UKHSA) and Dr Theresa Lamagni (UKHSA).
For information about data related to our study, please read our Transparency Statement
For more information about this study, contact us at ispy.project.support@imperial.ac.uk
How does COVID-19 affect children?

The TraCK study was a study conducted in 2020-2021 to find out if children were likely to transmit the virus causing COVID-19 in school or in households. Lots of studies have now shown that children are very unlikely to suffer unpleasant symptoms of COVID-19, and are highly unlikely to need hospital admission. Although there have been some cases of an inflammatory illness that followed the COVID-19 upsurge, these were extremely rare.
Children appeared less likely to act as the source of infection in outbreaks. This is very different to infections like scarlet fever or measles - during the lockdown period some of those infections in children became much rarer.
What did the TraCK study do?
TraCK was a research project that ran in addition to the normal public health responses. the work was only done if people agreed to take part. 
The team followed up children diagnosed with COVID-19 that had attended a school, to find out how long children carry infectious virus, and to see if it is present in body fluids like saliva, on skin, on other surfaces, and in the air around an infected child. The research team checked to see if any other people got infected among classmates and household members – even if no one had symptoms. They also checked the school and home environment for the virus. The study was quite intensive so gathered a lot of information from a small number of schools.
Why was it important?
The study showed that children did appear able to transmit SARS-CoV2 (the virus that causes COVID-19) in households. It also showed that the virus was frequently present in the air and on surfaces in people’s homes. This was in stark contrast to classrooms. When a case of COVID-19 had been diagnosed in a child attending school, we did not find any evidence of onward transmission among classmates. Of course, there were lots of restrictions in 2020-2021 and classrooms were not as full as normal; we also did not manage to recruit as many participants as we would have liked. Nonetheless, we concluded that classrooms at the time of the study were relatively safe environments in terms of exposure to the virus. The study taught us a lot about how to conduct research in schools during a pandemic, at a time when people were understandably anxious about their health and their families.
How did the study work?
The study was triggered if a single case of COVID-19 in a child was notified in any school in the London area; notification meant that UK Health Security Agency (UK-HSA) knew about the case. The school was asked to follow standard public health advice at this stage and the affected child’s contacts were asked to self-isolate.
Who approved the study?
The study has full ethical approval from a national Research Ethics Committee and was peer-reviewed and funded by UKRI.
The research was done by Imperial College London together with UK Health Security Agency. COVID-19 Research was funded by UKRI in partnership with NIHR. The investigators are, from Imperial College London: Professor Shiranee Sriskandan, Professor Wendy Barclay, and Professor Graham Taylor and from, UKHSA: Dr Rebecca Cordery, Dr Miranda Mindlin, and Dr Theresa Lamagni (all of UK-HSA).
Published TraCK report Lancet Microbe 2022
This report compares SARS-CoV-2 transmission by children and environmental contamination in schools versus households.
Note: this study is not currently open for recruitment.
For information about data related to our study, please read our Transparency Statement.

