25 years of advancing obstetrics and gynaecology research
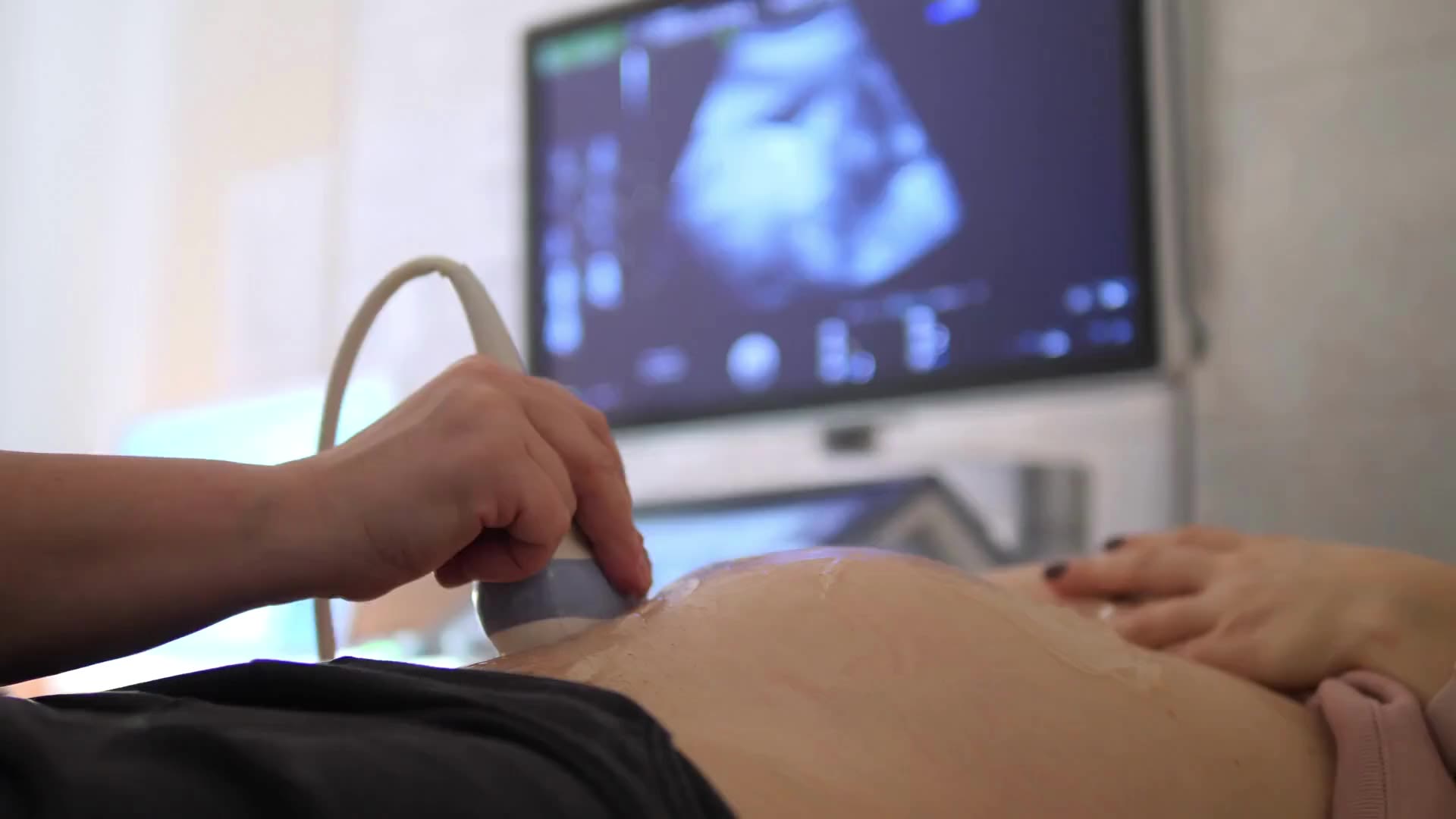
From research to better understand pre-term births, to breakthroughs in accurately diagnosing miscarriage, preventing recurrent pregnancy loss, pioneering improvements in IVF and safely delivering growth restricted babies, Imperial College London researchers have been at the forefront of many key research discoveries in obstetrics and gynaecology.
For the Faculty of Medicine’s 25th anniversary, we spoke to some of the researchers making crucial steps forward in this area.
A note on the use of language in this article
While in this article we refer to women, we recognise that some transgender men, gender-diverse people, and people who are intersex may be affected by some of the same issues. We also recognise that people who are trans, gender-diverse or intersex have specific needs, experiences and health issues that need addressing. The use of the term “women” in this article is not intended to exclude other groups or overlook the challenges they face.
Preventing recurrent miscarriage
Professor Lesley Regan

“In the 1990s, when I started my clinic helping women who had repeated miscarriages, miscarriage was seen as something that ‘just happens’. There was very little in the textbooks about it.”
Professor Lesley Regan now runs the largest specialist miscarriage clinic in Europe – the Recurrent Miscarriage Service at St Mary’s Hospital. In its 30 years, the clinic’s research has transformed the investigation, counselling and treatment of couples that suffer pregnancy loss.
Professor Regan says one of the most important discoveries her team has made was demonstrating that clotting abnormalities are an important cause of recurrent pregnancy loss and that they can be treated.
Affecting 15% of women who have recurrent miscarriages, anti-phospholipid syndrome (APS) causes people to produce harmful antibodies that attack cells in the body, causing inflammation and turbulent blood flow and then leading to the formation of blood clots.
The team ran a pivotal clinical trial for women with APS in the mid 1990’s.
“We found that the women taking aspirin and heparin had a 70% chance of having a baby, compared to a 10% chance in women taking only aspirin. This was a massive difference,” says Professor Regan.
“We were the first group to demonstrate this link and propose a treatment. Our paper was published in 1997 and it was on the front page of the British Medical Journal.”
The trial’s findings became medical guidance in the UK, USA, the Netherlands and Australia. The Arthritis Research Council (ARC), who funded the trial, estimate that treatment for these women has led to thousands of successful pregnancies every year in the UK alone.
Yet Professor Regan remained intrigued by APS and its effects in pregnancy. She later discovered that the condition prevents the early embryo from embedding the placenta to the optimal depth into the mothers’ womb lining – work that has helped unveil a new field of research explaining other pregnancy complications.
“We found that the way the embryo implants acts as a blueprint for how that pregnancy will progress at a later stage – the quality and depth of this implantation process is a major factor in determining pregnancy outcomes,” she says.
“If the placenta implants to the correct depth, it is more straightforward, but when it is more shallow, it can cause a heightened risk of miscarriage and stillbirth. This can also lead to foetal growth restriction, as it’s harder to get blood through the placenta to the baby, and to pre-eclampsia, because the mother’s blood pressure increases to pump blood and nutrients even harder through the placenta.”
Now as the Government’s first ever Women’s Health Ambassador for England, Professor Regan is keen that researchers and doctors develop a more rounded understanding of women’s health.
“Pregnancy is a little bit like a trial run and can help us predict what might happen to a woman’s health later in life, I don’t think we are good at using the information we gain from the mothers’ response to pregnancy to try to help prevent women from having problems in later life. For example, we know that women who develop pre-eclampsia or have babies with growth restriction have a greater risk of heart disease and stroke later on, which also develops at an earlier age compared to women who had uncomplicated pregnancies,” she explains.
“One of the things that I think Imperial research has highlighted repeatedly is that the way women physiologically respond to being pregnant is often like a putting on your L plates for later life.”


Improving early
miscarriage guidelines
Professor Tom Bourne
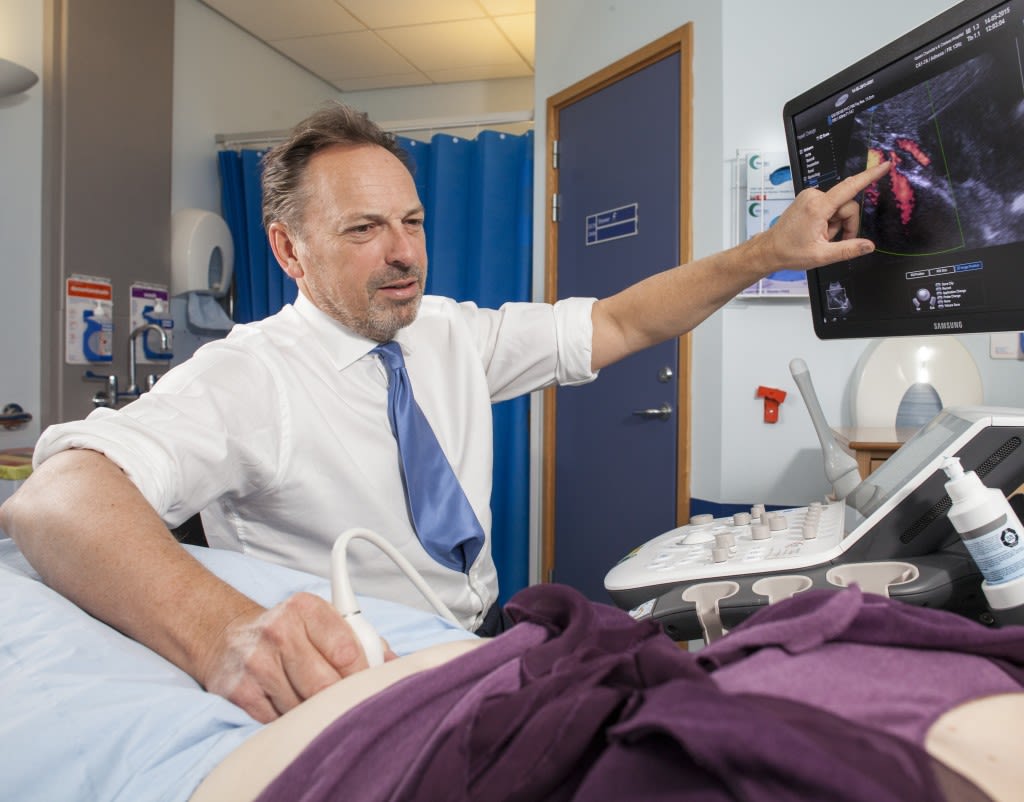
An international authority on the use of ultrasound in gynaecological disorders as well as the management of early pregnancy complications, Professor Tom Bourne’s research has been pivotal in setting the standard for the early diagnosis of miscarriage.
“For me the issue came to a head when I was chairing an early pregnancy session at the International Society for Ultrasound in Obstetrics and Gynaecology meeting in Prague in 2010. I asked the audience what they used as a cut-off value for mean gestation sac diameter to define miscarriage, and the answers ranged from a very worrying 2 to a more reassuring 20 mm.”
An accurate diagnosis in the first trimester (the first 12 weeks of pregnancy) is vital since a misdiagnosis could result in a healthy pregnancy being inadvertently terminated. However, for Professor Bourne, Chair in Gynaecology in the Department of Metabolism, DIgestion and Reproduction, it seemed that the then-existing criteria used to define miscarriage was “less than watertight”.
“From a patient’s perspective if there is one decision a women would expect clinicians to get right with absolute certainty, it would be whether their baby is alive or not.”
This prompted Professor Bourne and his team of collaborators to review the evidence behind the guidelines used to make these decisions.
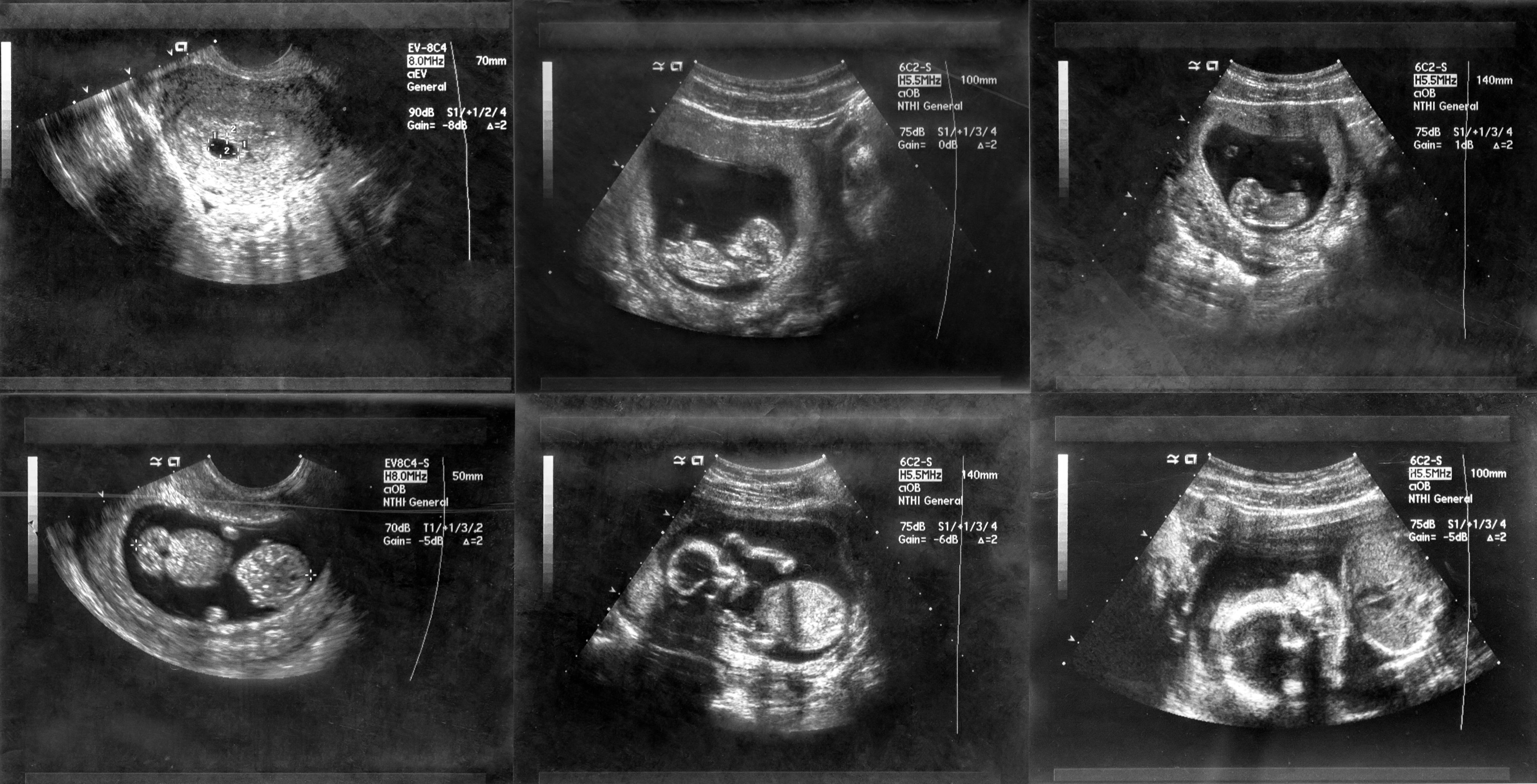
Between 2011 and 2015, the Imperial team led by Professor Bourne collected ultrasound data from over 3,000 women in the UK. They found that the risk of misdiagnosis using embryo size measurements and an apparent lack of a visible heartbeat on ultrasonography could be as high as 8% – just over 1 in 12 – potentially resulting in cases of unnecessary termination of a wanted pregnancy.
This prompted a publication in the New England Journal of Medicine that used the Imperial data to propose new safe diagnostic criteria. Their discovery led to a rapid revision of miscarriage guidelines across the world, including in the UK, France, Italy and the US.
Before this important research, it is possible that thousands of wanted pregnancies throughout the world may have had surgical or medical treatment for a miscarriage based on a misdiagnosis. Indeed, an American study suggests that as many as 12% of women may have been given an incorrect diagnosis of miscarriage using the guidance that existed in the US prior to the Imperial study.
“Just one misdiagnosis of miscarriage is too many. Our study provides us with better data to guide clinicians and improve diagnostic accuracy.”
During their studies, the Imperial team also became acutely aware of the persistent and severe psychological consequences of miscarriage, with many women experiencing post-traumatic distress symptoms. This influenced its inclusion in the National Bereavement Care Pathway, an initiative that is dedicated to ensuring that bereaved parents are offered equal, high quality, individualized, safe and sensitive care in all hospitals in the UK. More recently the work was also cited in the independent pregnancy loss review.
Their findings describing the psychological impact of miscarriage and ectopic pregnancy also attracted intense media interest, receiving one of the biggest media coverage of any story from Imperial. It was covered throughout the world, raising awareness of the important long-term psychological consequences of miscarriage.
Even a diagnosis of loss very early in the pregnancy may result in significant psychological distress later, and must be treated with compassion."

Safely delivering growth
restricted babies
Professor Christoph Lees
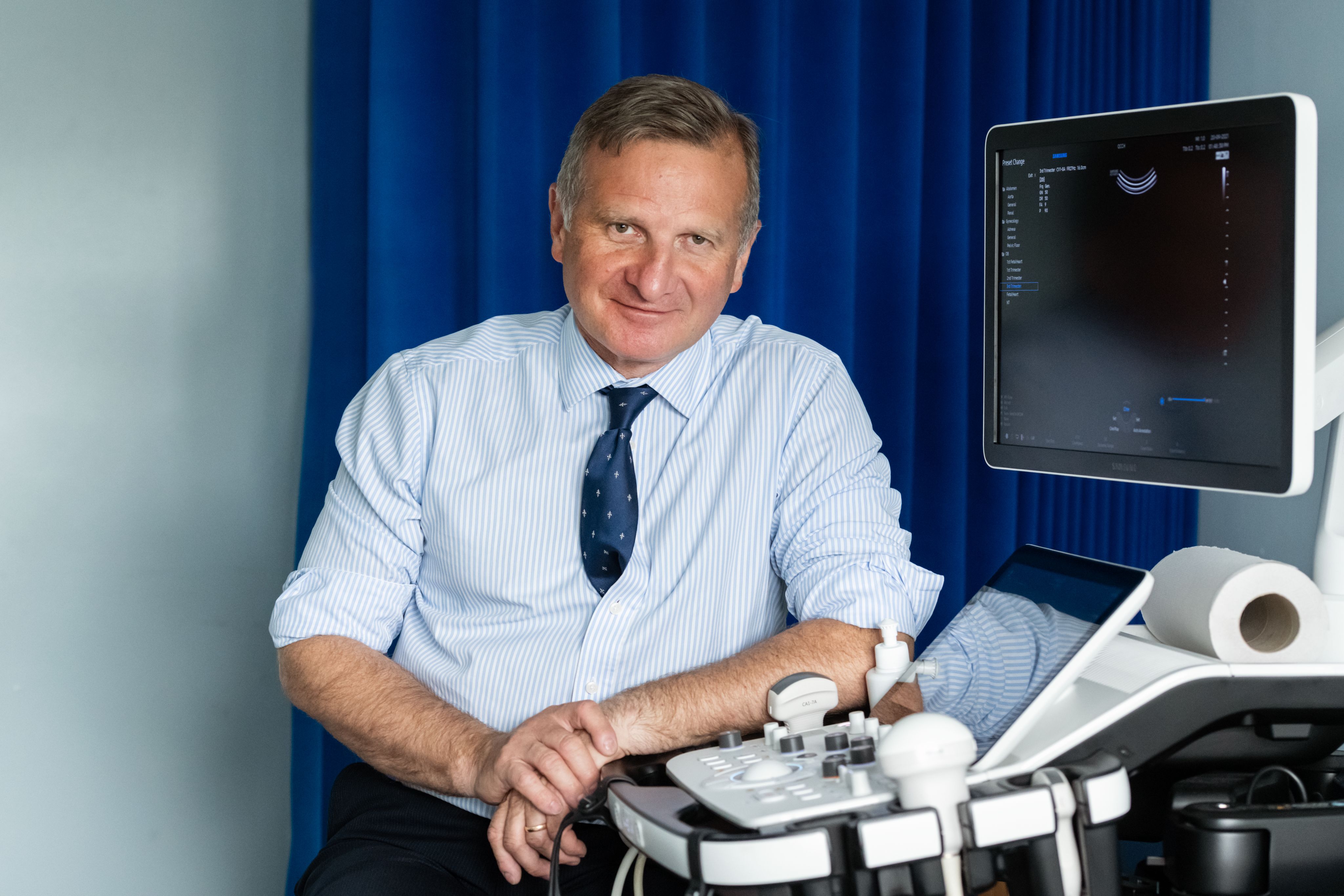
With research to help prevent pre-eclampsia, manage slow growth in babies during pregnancy, and use of sound waves to treat twin pregnancy complications, Professor Christoph Lees takes pride in the benefits his research holds for patients.
The treatments and technologies he and his team have developed are the result of a long gradual process to find answers and create solutions that benefit women and their babies. He believes Imperial’s vibrant interdisciplinary research culture is key to this.
“Collaboration is a very important attribute of Imperial,” the Professor of Obstetrics at Imperial and Head of Foetal Medicine at Imperial College Healthcare NHS Trust notes.
“We’ve got a lot of pretty accomplished people, but there’s no ego or politics between them like you can sometimes get. I hugely enjoy working with my colleagues because we all augment each other’s ideas. You open up a treasure chest of ideas, let people pick ideas out, polish them up to make them better and put them back in. That’s the value of collaboration.”
He also values Imperial’s open mindedness for new ideas.
“You can have fantastic ideas that other people might think just couldn't work, but here, you can find people who take it seriously and run with it, and you end up developing something that no one else has thought of. Imperial researchers have a genuine wish to embrace new thinking and see if it’s going to work,” he says.
One of the most important outcomes of his research has been finding ways to safely deliver babies with fetal growth restriction.
Caused by problems with blood flow through the placenta, foetal growth restriction is a condition where the baby’s growth is slower than expected or stops during pregnancy. This can lead to health complications for the baby, including stillbirth. Because of this risk, mothers and their babies have regular check-ups throughout pregnancy, with babies with foetal growth restriction sometimes delivered earlier than expected.
The TRUFFLE-1 (Trial of Randomised Umbilical and Foetal Flow in Europe 1) study that Professor Lees led aimed to identify the optimal time to deliver these babies between 26-32 weeks of pregnancy. It found that babies delivered following results from a technique that monitors blood flow in a small vessel below their heart – late ductus venosus changes – had better neurodevelopmental outcomes than babies delivered on the basis of two other techniques.
Countries around the world have since adopted this guidance on how to monitor and when to deliver these babies.
“Our work led to changes in many international guidelines, which we hope will have made a major impact on the outcome of these pregnancies by balancing unnecessary premature delivery while not allowing the babies to become compromised in the womb. We are now focusing on the NIHR-funded TRUFFLE 2 study of management of later fetal growth restriction."


Understanding the link between infection and pre-term births
Professor Phillip Bennett

After seeing many pre-term births in his first years as a doctor in the 1980s, Professor Phillip Bennett stepped into science to study why this happened and if it could be prevented.
“What attracted me into research was realising how interested people were in understanding disease. Imperial struck me as having a very healthy research environment where senior people were willing to admit what they knew and what they didn't know. There was a lot of honesty and integrity.”
Now a Professor of Obstetrics and Gynaecology and Director of Imperial’s Institute of Reproductive and Developmental Biology, he explains that back then doctors didn’t really know what caused pre-term births. Pre-term, or premature, birth is when a baby is born before 37 weeks of pregnancy.
Some of Imperial’s earliest research in this area was conducted by Professor Murdoch George Elder – a colleague of Professor Bennett’s who inspired his interest – who headed up the Institute of Obstetrics and Gynecology at the Royal Postgraduate Medical School (which later became part of Imperial’s Faculty of Medicine).
By studying how bacteria in the mother’s reproductive tract interacted with cells in the womb that triggered labour, Professor Elder’s work found a link between pre-term birth and what was then thought to be an infection.
This idea is what Professor Bennett has studied for the last 40 years. Over time, he and his research group moved into studying the balance of bacteria in the reproductive tract and found that this is an important factor that influences the risk of pre-term birth.
“Broadly speaking, there's a whole bunch of ‘good guy’ bacteria called lactobacilli that live in the vagina and protect against other bacteria coming in and causing trouble. So, if you don't have lactobacilli or have the wrong type, you get an imbalance in the bacteria that is linked to an increased risk of pre-term birth,” Professor Bennett explains.
His team also discovered a series of biochemical events essential to starting labour that can be triggered by a bacterial imbalance. This includes prostaglandins – molecules which help dilate the cervix and cause the womb to contract and move the baby through the birth canal.
Initially, Professor Bennett and his team tried to create drugs that blocked this biochemistry to prevent labour starting too soon. Now, they are trying to stop the early triggering of labour altogether by creating treatments that maintain a healthy bacterial balance.
“We’ve recently found that we can give the good bacterium to women and it displaces the bad bacteria. The next step will be to see if this also reduces the risk of pre-term birth, which we need to do clinical trials to understand. There have been no new treatments for pre-term birth in the last 20-30 years, so if our idea works this would be a major breakthrough,” he says.


Transforming
menopause treatment
Professor Waljit Dhillo

As someone who is excited by Imperial’s research infrastructure and the bright people that this attracts, Professor Waljit Dhillo’s research is a model for how this setup can turn basic science into medical benefits.
“20 years ago, we didn’t even know of the hormones I work with – kisspeptin and neurokinin B. It was only through genetic discovery that they were identified, and now, suddenly, we may have breakthroughs using them,” says the Professor in Endocrinology & Metabolism at Imperial and Consultant Endocrinologist at Hammersmith Hospital.
“Imperial is linked to the hospital, which makes it much easier to be able to go from the basic science in our lab all the way up to phase three clinical studies. You've also got the whole spectrum working together – clinicians, basic scientists, other healthcare professionals, chemists and engineers.”
Professor Dhillo heads up an internationally leading research group in kisspeptin and neurokinin B. Kisspeptin, in particular, has shown promise for people with infertility.
“We found that when you give men and women kisspeptin, you get a stimulation of reproductive hormones. This opened up the possibility that this could be a new way of treating patients with reproductive disorders,”
In the 2010s, Professor Dhillo and his team pioneered a new method of IVF for women at risk of severe ovarian hyperstimulation syndrome (OHSS) – a condition where IVF drugs cause the ovaries to produce lots of eggs, which requires specialist care and hospital admission for one in every 100 cases.
The new approach provides a safer alternative to conventional IVF by using kisspeptin to stimulate the eggs instead of standard drugs.
The first baby was born using it in 2013, and since then more than 30 babies have been born in a trial of the treatment at Imperial College Healthcare NHS Trust.
However, Professor Dhillo and his team are eager to explore even more uses of the naturally occurring hormone.
As well as studying kisspeptin as a potential treatment for low sexual desire in men and women, they have shown that it increases reproductive hormones in women whose periods have stopped and could help restore their fertility.
Professor Dhillo’s extensive work in neurokinin B (NKB), a brain chemical, has also provided much hope for women plagued by hot flushes during the menopause. In 2018, confirmatory trial data revealed that a new class of experimental drugs called MLE4901 could reduce the frequency of hot flushes by almost three-quarters, as well as the severity by over a third, in just three days.
These new experimental drugs are thought to work by blocking the action of NKB by activating temperature control areas within the brain, halting hot flushes and providing an alternative to Hormone Replacement Therapy – the current treatment for symptoms of the menopause. This offers a promising alternative for those women who cannot take HRT to relieve their menopausal symptoms.
“This type of drug will make a tangible difference to the lives of millions of women and excitingly in May of this year, the first drug which blocks the action of NKB has received FDA approval in the USA."
He says Imperial’s ambition drives him.
“I think Imperial is very good at creating an atmosphere of having no glass ceilings for researchers, so positively encourages us to go for gold, go for something challenging, go for something exciting and which will make an impact for patients and society – its an exciting place to work. This is why we are a world leading university. It’s a very aspirational approach of saying we want you to meet the biggest challenges and answer the biggest research questions worldwide.”


Clinical research at Imperial College London is supported by funding from the NIHR Imperial Biomedical Research Centre (BRC), a translational research partnership between Imperial College London and Imperial College Healthcare NHS Trust, which was awarded £95m in 2022 to continue developing new experimental treatments and diagnostics for patients.

