Global State of Patient Safety 2023
Institute of Global Health Innovation, Imperial College London
Patient Safety Watch

1. Executive Summary
The Institute of Global Health Innovation at Imperial College London, commissioned by Patient Safety Watch, presents this analysis of the Global State of Patient Safety 2023.
Patient Safety Country Ranking
Our novel patient safety country ranking compares the performance of OECD countries across four well-established patient safety indicators, following the methodology used by the Commonwealth Fund. Using this approach, Norway is at the top of the ranking. The UK ranks 21st out of 38 countries.
The ranking also highlights the variation that exists across comparable countries. Using only the four selected metrics, we see that the UK could have had 17,356 fewer deaths annually had it performed at the level of the top decile of OECD countries.
Broken down by indicator, this would have meant 15,773 fewer deaths classified as “treatable mortality” (where the cause of death can be mainly avoided through timely and effective health care interventions) per year, 776 fewer deaths due to neonatal disorders per year, 27 fewer maternal deaths per year and 780 fewer deaths due to adverse effects of medical treatment per year.
An important limitation of this ranking is that the four indicators included only represent a narrow aspect of health system performance, and do not consider the wider quality of life effects or long-term disability caused by unsafe care. More comprehensive, consistently collected and regularly shared data would significantly increase the opportunity for cross-country comparisons and shared learning.
Patient Safety Dashboard
Our patient safety data dashboard is undergoing an update May-June 2025. If you have any queries about the data while it is offline, please contact Melanie Leis.
Our Purpose-built patient safety data dashboard, provides a single point of access to publicly available global patient safety data. An analysis of this data paints a less than optimistic picture of global patient safety over the past decade.
Many of the indicators show very little overall improvement over time. An example is performance on retained item during surgery, despite being subject to significant focus and improvement efforts.
Many indicators also show a significant spread in performance, even between comparable groups of countries. One example is the rate of maternal sepsis, which shows a 437-fold difference between the top and bottom 10% of countries.
Rates of progress, and levels of variation, can to some extent be explained by improvements in reporting practices, or contextual differences between countries.
We present this analysis, and the accompanying data dashboard, to highlight the opportunities for improving patient safety by systematically comparing data and sharing examples of excellence between countries.
Our analysis is, however, limited by the lack of timely, relevant and comparable data at a global level. We find, for example, that:
- Three out of every five indicators are not available for low or low-middle income countries (LMIC).
- One in every six indicators consists of data more than three years old.
- Only one in every ten indicators comprises data directly reported by patients.
In addition, we would also want to see further work to collect data on:
- The patient’s trajectory of care through different care providers, and
- Any inequities in safe care on account of peoples’ demographic characteristics or socio-economic circumstances.
Case Studies
Our case studies showcase excellence in safety measurement and improvement from the patient, family and carer perspective. These insights from nine leading patient safety experts and practitioners provide optimism on how deficiencies in patient safety data can be addressed. The challenge remains in how to foster the effective adoption of these approaches and interventions globally.
Recommendations
Based on our findings, we set out three recommendations to improve the measurement of patient safety:
- Assessment: A more balanced and comprehensive set of global patient safety indicators is required to address the data gaps identified in this report, and to ensure comparable data is available for all countries. Consensus is required on the minimum set of indicators that all countries should report on.
- Adoption: A global repository of safety measurement and improvement interventions should be developed and made freely available to frontline teams of practitioners and researchers across the world.
- Activation: To ensure the faithful adoption of interventions, patients, families and carers must be given the agency to become active and equal partners in the delivery of safe care.
2. Introduction from Professor the Lord Ara Darzi and James Titcombe OBE
There are grounds for optimism in the ongoing journey to improve global patient safety. Inspirational work is actively happening at the local level, as shown in the case studies we have identified, ready for wider adoption. Thanks to international efforts, there is a strategic commitment to drive change and align activities across communities and countries.
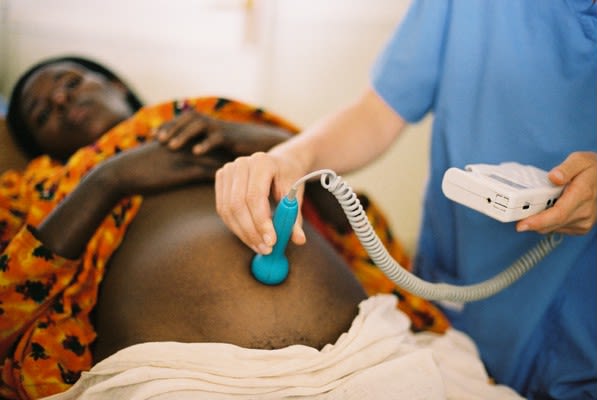
This has led to progress on key indicators such as the global reduction in maternal mortality. Yet there is still far to go; in 2020, 800 women died every day from preventable causes related to pregnancy and childbirth worldwide. More recent research, not yet evident in the routinely collected data, suggests that COVID-19 has worsened outcomes for mothers and babies, with disparities widening between high- and low-resource settings.
Data collected at a global level is an important part of monitoring progress in these key areas of patient safety. Laudable progress has been made to develop a significant body of indicators on patient safety at a global level, that are standardised and available for multiple countries – a long list of more than 250 by our reckoning, 89 of which are included in our dashboard. We are delighted to be able to bring these together into a single, accessible resource.
However, this indicator set leaves three important issues to contend with:
- It is a skewed set of indicators, made up of data disproportionately from higher income countries, rarely reported directly by patients, predominantly about the care provided in acute care, and relating to lagging indicators of harm rather than leading indicators of safety.
- It is an arbitrary set of indicators, which do not present a coherent picture, or even conceptualisation, of what is understood by patient safety.
- It is an incomplete set of indicators, which do not cover many of the essential components of a safe health care system, such as leadership, education, or staff wellbeing.
While current data limitations make international comparisons complex, in this report we have taken a first step by creating a patient safety country ranking of OECD countries. This ranking highlights that, even across comparable countries, there is notable variation and scope for improvement.
It is hoped that this report can act as a catalyst for future measurement and improvement activity, and provide a direction of travel on where future efforts should be focused – efforts that embody the spirit of 2023’s theme for World Patient Safety Day, engaging patients for patient safety.
To support this, we argue that patient safety must be measured and monitored in a way that conceptualises health care from the patient’s perspective, and improvement interventions that utilise the perspective of patients, families and carers must be more widely adopted.
We can only improve what we can measure. We need more real time data to tell us how safe care is today for patients. If we can do this, alongside the exciting work already underway from OECD and WHO to monitor safety processes, cultural indicators, and structural components of a safe health care system, it should be possible in future to better understand, and therefore improve, the global state of patient safety.
- Professor the Lord Ara Darzi, James Titcombe OBE
2.1 Opening remarks by Deborah E Prowse, KC, Patient Safety Advocate
Deborah Prowse, Patient Safety Advocate
3. Our Approach
Our patient safety data dashboard is undergoing an update May-June 2025. If you have any queries about the data while it is offline, please contact Melanie Leis.
3.1 Data Dashboard
To develop our data dashboard, we conducted a scan of the relevant literature and the main sources of international data, resulting in a long list of more than 250 indicators relevant to patient safety, compiled from the sources listed below:
- World Health Organization (WHO) – compiling data on health and health-related indicators for its 194 member states.
- WHO Regional Office for the Eastern Mediterranean (EMRO) – compiling data specifically across the 22 countries and territories in the Middle East, North Africa, and Central Asia.
- The Global Burden of Disease (GBD) Study – compiling data relating to premature death and disability from 370 diseases and injuries in 204 countries and territories.
- The Organisation for Economic Co-operation and Development (OECD) – compiling statistics on health and health systems across the 38 member countries.
- The World Bank – compiling data on health and population statistics from its 189 member countries.
Only data that were publicly available, standardised (i.e. taken from different sources and transformed into a standard format), and collected across multiple countries were included in the list, to support meaningful analysis. The views of global experts in patient safety and health care quality measurement were sought to refine the list of indicators for their relevance to patient safety, before a final list of 89 measures were included in this version of the data dashboard.
Some indicators were removed for technical reasons (for example, those which contained absolute figures rather than rates or proportions, and those which relied on survey questions where the wording has been changed over time). Our period of analysis begins in 2000, though data is available for some indicators before then.
The result is a dashboard that provides a unique, consolidated view of publicly available patient safety indicators at an international level.
3.1.1 Navigating the Dashboard
The dashboard provides access to a broad range of indicators, spanning multiple countries, to give a view of the global state of patient safety. The dashboard enables users to organise and view the data in different ways – such as heatmaps showing changes within countries over time, or line graphs displaying multiple metrics for a single country. In each tab, we have included an information icon, providing details about how to navigate each section.
The indicators are categorised in several ways – such as into structure, process, and outcome indicators – to support analysis (see Section 5.1 for more information). A selected analysis of the indicators is included in Section 6. The main structural measures, such as those concerning health care facilities and workforce are not included in our analysis, but they can be used with caution to explore possible associations with the process and outcome measures.
3.2 Country Ranking
Comparing healthcare systems based on publicly available data is challenging and complex, particularly in patient safety. Nevertheless, rankings are a helpful way to assess how health care systems are performing and where they can improve. To this end, we have created a patient safety country ranking which illustrates the variation that exists across a comparable group of countries for a selection of well-recognised patient safety measures.
The patient safety country ranking uses a methodology derived from the Commonwealth Fund’s ranking of health systems. Countries are ranked based on their distance from the average of all countries, measured in standard deviations (i.e. the country at the top of the ranking is the country with the largest positive distance from the average in standard deviations). Only OECD countries were included for comparability.
This ranking uses four patient safety indicators, selected from the 89 indicators included in the dashboard:
- Maternal mortality (deaths per 100 000 live births): Maternal deaths, all causes.
- Treatable mortality (deaths per 100 000 population): Causes of death that can be mainly avoided through timely and effective health care interventions, including secondary prevention such as screening and treatment (i.e. after the onset of diseases, to reduce case-fatality).
- Adverse effects of medical treatment (deaths per 100 000 population): Deaths sustained as the result of undergoing a procedure, treatment, or other exposure to the health-care system. This exposure can occur in inpatient admission, outpatient facilities, emergency care, or during home treatment.
- Neonatal disorders (deaths per 100 000 live births): This aggregate indicator covers five main causes of death and disability: preterm birth complications; neonatal encephalopathy due to birth asphyxia and trauma; neonatal sepsis and other neonatal infections; haemolytic disease and other neonatal jaundice; and other neonatal disorders.
The rationale for inclusion of these four metrics is outlined below:
- These metrics measure rates of deaths, which tend to be more consistently and reliably reported.
- These metrics are relatively well defined, which reduces the likelihood of differences in reporting across countries.
- These metrics are available for all OECD countries, allowing for comparisons.
- While these metrics are a limited proxy for health system safety, the inclusion of treatable mortality broadens the scope of what is traditionally viewed as patient safety by considering causes of death that can mainly be avoided through timely and effective health care interventions, including secondary prevention and treatment.
3.3 Case studies
As explored later in this report, the data included in our dashboard provide an incomplete picture of global patient safety. This report, therefore, includes case studies of excellence from around the world in the measurement and improvement of patient safety, which, if adopted more widely, would go some way towards completing this picture. The case studies are based on interviews with the practitioners and researchers who have led this work, alongside a review of the publications and resources they have provided. We are extremely grateful for their support with this work. The case studies include examples of efforts to:
- Capture patient, family and carer insights into safety and harm.
- Utilise patient, family and carer insights to respond to unsafe systems and processes.
- Address inequities in the provision of safe care from the patient, family and carer perspective.
The case studies are incorporated throughout the report, each with a map illustrating where they originated and where they have been adopted.
- Involving patients in safety investigations – supporting patients to take a more involved and proactive role in safety investigations.
2. Restorative responses to harm – using mutual healing approaches in response to adverse events.
3. Safety measurement and monitoring framework – adopting an approach to support a culture of measurement and the proactive identification of risks.
4. Situational Awareness for Everyone (S.A.F.E.) – developing a shared understanding of safety across professionals, patients and families, and adopting a range of tools to understand and improve safety in real time.
5. Family-activated medical emergency teams – improving the timely recognition of clinical deterioration and reducing preventable adverse events in paediatric care.
6. No-fault maternity compensation schemes – providing timely financial redress following injury without proving negligence and using investigation reports to improve learning and transparency.
7. Addressing racial disparities in maternal morbidity – stratifying data by ethnicity to address inequalities in outcomes for mothers experiencing harm from haemorrhage.
8. Patient measure of safety – capturing patient experiences of safety in hospital and primary care.
9. Partners at care transitions measure – capturing patient perceptions of preparedness for discharge from hospital, and safety at home following discharge.

4. Global patient safety movement – where are we now?
The notion of patient safety can be dated back through history, from the beginning of the idea “to do no harm” in the Hippocratic Corpus, to its modern day conceptualisation in publications such as To Err is Human. Since the turn of the twenty first century, significant attention has been paid first to quantifying the nature and extent of avoidable harm, and later to mitigating the risks within health care systems. This has led to a dramatic increase in efforts designed to raise awareness, initiate research, and deliver programmatic activities, to improve patient safety.
These efforts have taken the form of national policies and frameworks, education and training programmes, new and specialised roles, discreet safety interventions, large-scale improvement programmes, and national reporting and learning systems. But despite some notable gains, there has been a general recognition that the patient safety movement hasn’t lived up to its early promise, and that progress has subsequently stalled. In some regions, ensuring patient safety is placed as a public health priority remains challenging.
A positive and just patient safety culture remains an elusive concept in many countries, while the involvement of patients as active participants in care has been slow to spread, particularly in LMICs. Hierarchy often still overpowers the option to speak up, and organisational reputation can overshadow the importance of transparency or candour when an incident occurs. The COVID-19 pandemic made it even more challenging for resource poor settings to prioritise patient safety over other essential needs such as water and sanitation, or vaccine rollout.
The COVID-19 pandemic also exacerbated the health worker crisis which has been growing over recent years. Alongside increasing shortages and poor retention of workforce, and the movement of staff from the global south to middle-and high- income countries, burnout and mental health challenges are overwhelming the workforce, with global burnout rates estimated at 54%.
Queen's Tower, Imperial College London, on World Patient Safety Day
Queen's Tower, Imperial College London, on World Patient Safety Day
4.1 The global burden of harm
Estimates of the global burden of harm caused by heath care emphasise the scale of the problem. In 2019, research estimated the prevalence of preventable patient harm across medical care settings to be 6%, translating to around 1 in 20 patients being exposed to harm. In 2013, estimates suggested that at least 43 million injuries each year were due to medical care, with 23 million lost DALYs (Disability-Adjusted Life Years, each one representing the equivalent of losing one year of full health), the majority of which occurring in low- and middle- income countries and economies in transition. One in 10 dollars spent on health care globally is diverted to treating the effects of unsafe care and reduces global economic output by trillions of dollars each year.
In some areas progress in patient safety has stalled, with the decline in maternal deaths slowing from an annual rate of reduction of 2.7% between 2000 to 2015, to 0.04% between 2016 and 2020. The COVID-19 pandemic has had a significant effect on progress and also served to deepen inequities. For example, in the US, the number of maternal deaths rose from 754 in 2019 to 1,178 in 2021. The maternal mortality ratio for non-Hispanic black women was 68.9 per 100,000 live births in 2021, and 26.1 for non-Hispanic white women.
Alongside the ever-increasing demands being placed on the health care workforce to meet the needs of patients and populations, there are several reasons for this plateauing in safety improvement. They include:
- A realisation that Quality Improvement methods are not a panacea, and often do not lead to the wider cultural change required for substantive impact, or stand up to evaluation in a wider context;
- An enthusiastic, but superficial, embrace of principles and methods from the safety sciences, without the deeper work they often require, as demonstrated in other safety-critical industries;
- A lack of recognition and prioritisation of the importance of quality and safety as a key component of universal health coverage, resulting in limited investment and attention particularly in resource constrained settings and;
- The impact of the COVID-19 pandemic, putting the workforce and entire health and care system under almost unimaginable stress, leading to re-directed attention and resources, and significant backlogs in care for cancer and other specialised treatments.
There has also been an increasing recognition of the nature and extent of compounded harm that can arise following injury, as a consequence of the way that health and care services respond to a patient safety incident (see case studies 1 and 2 below). Responses to harm that are not open or transparent, or do not seek to understand what patients and families need to support their healing and recovery, are entirely avoidable. Responses to harm must focus on learning to prevent future harm, but this need not be at the expense of decent, and empathetic, involvement of all those affected.
Case study 1: Involving patients in safety investigations.
The Learn Together project aims to develop guidance to ensure more meaningful involvement in the investigation of serious healthcare incidents. The idea was that, by working relationally between patients, families and staff, the likelihood of compounded harm – where the harm relating to a patient safety event is compounded by the processes that follow it – is reduced.
A series of resources, free to download, have been designed for patients and families, and those investigating safety incidents, based on a set of common principles co-developed with these groups. These include a guide providing support for patients and families going through the process of a safety investigation, which includes space for patients and families to record key information about the investigation. Additional resources include a guide for investigators, as well as videos and links to other support and resources.
Case study 2: Restoration and healing from harm
Jo Wailling, Co-Chair, National Collaborative for Restorative Approaches in Health
There is also a widening gap between countries at different stages of their patient safety journeys, and between those from high- and low-resource settings. Some of this is evident in the data dashboard. As countries strive towards achieving the Sustainable Development Goals (SDGs), the benefits of having access to health services is undermined by unsafe and low-quality care. The COVID-19 pandemic has reinforced the need for all countries to be able to provide a standard of safe universal health coverage, acknowledging that “having access to health care is plainly not enough.”
4.1.1 WHO Patient Safety Friendly Hospital Initiative
In Pakistan, efforts are being made to put patient safety onto the national agenda through a series of interventions. A national framework and standards for patient safety and quality have been developed, providing a focal point for patient safety at the Ministry of Health. The Patient Safety Friendly Hospital Initiative (PSFHI) has also been implemented in 12 tertiary care hospitals, providing training to more than 300 hospital managers.
The PSFHI is intended to help institutions to develop patient safety programmes, with support from the World Health Organization. The PSFHI is a voluntary process whereby institutions undergo a process of assessment against international best practice standards. It involves a self-assessment exercise alongside guidance from experts, site visits and interviews across the following strategic areas:
· Leadership commitment
· Clear policies and guidelines
· Competent and compassionate health professionals
· Engaging patients and families
· Using data to drive improvements.
Crucial to its implementation in Pakistan has been the support from the Ministry of Health and provincial health department, demonstrating the need for action through patient stories, and providing incentives and motivation in the form of certification.
The number of fragile, conflict- affected and vulnerable (FCV) settings has accelerated, with 50% of the global poor expected to live in these contexts by 2030. In addition, the damage caused by conflicts around the world have heavily impacted the development of health systems. It is imperative that health services are allowed to operate safely in these settings.
Set within this context of diminishing returns and widening disparities, this work explores the opportunities afforded from what are, in our view, two underutilised assets:
- Analysing what we know, and what we don’t know, from the publicly available global patient safety data, and
- Sharing examples of excellence (or ‘positive deviance’) from local teams who are measuring or improving safety in ways that utilise the unique perspectives and assets of patients, families and carers.
5. Understanding the data

Our analysis of the global patient safety data begins with an understanding of the type and range of available data, their completeness and reliability, and how useful they are in assessing the safety of health care services.
5.1 Data classification
We organised the indicators into structure, process and outcome measures, based on Avedis Donabedian’s classic approach to measuring quality in health care – (see Figure 1 for a breakdown of the indicators by category):
- Structure measures reflect the context in which care is delivered, such as the make-up of the workforce or the availability of hospitals and beds.
- Process measures reflect the way that the systems and processes work to deliver an outcome for patients, such as whether patients are involved in their care, or how long they have to wait to receive their treatment.
- Outcome measures reflect the impact of all activities on patients, such as whether they experience safe care when delivering a baby, or develop an infection following surgery.
The indicators are also sub-divided into the following areas of care, to support interrogation of the dashboard in particular areas (see Figure 2):
- Maternal and neonatal health.
- Health care workforce.
- Access to care.
- Waiting times.
- Surgical and post-operative safety.
- Staff perceptions of safety.
- Medication safety.
- Adult mortality and morbidity.
- Mental health.
- Health care facilities.
As illustrated in Figure 2, the most populated category of indicators relate to outcomes in maternal and neonatal services (28%), which may in part reflect their focus in the Sustainable Development Goals. Somewhat surprisingly, given its prominence in patient safety campaigns in recent years, standardised data on the prevalence of Healthcare Acquired Infections (HAI) are not available.
5.2 Data completeness
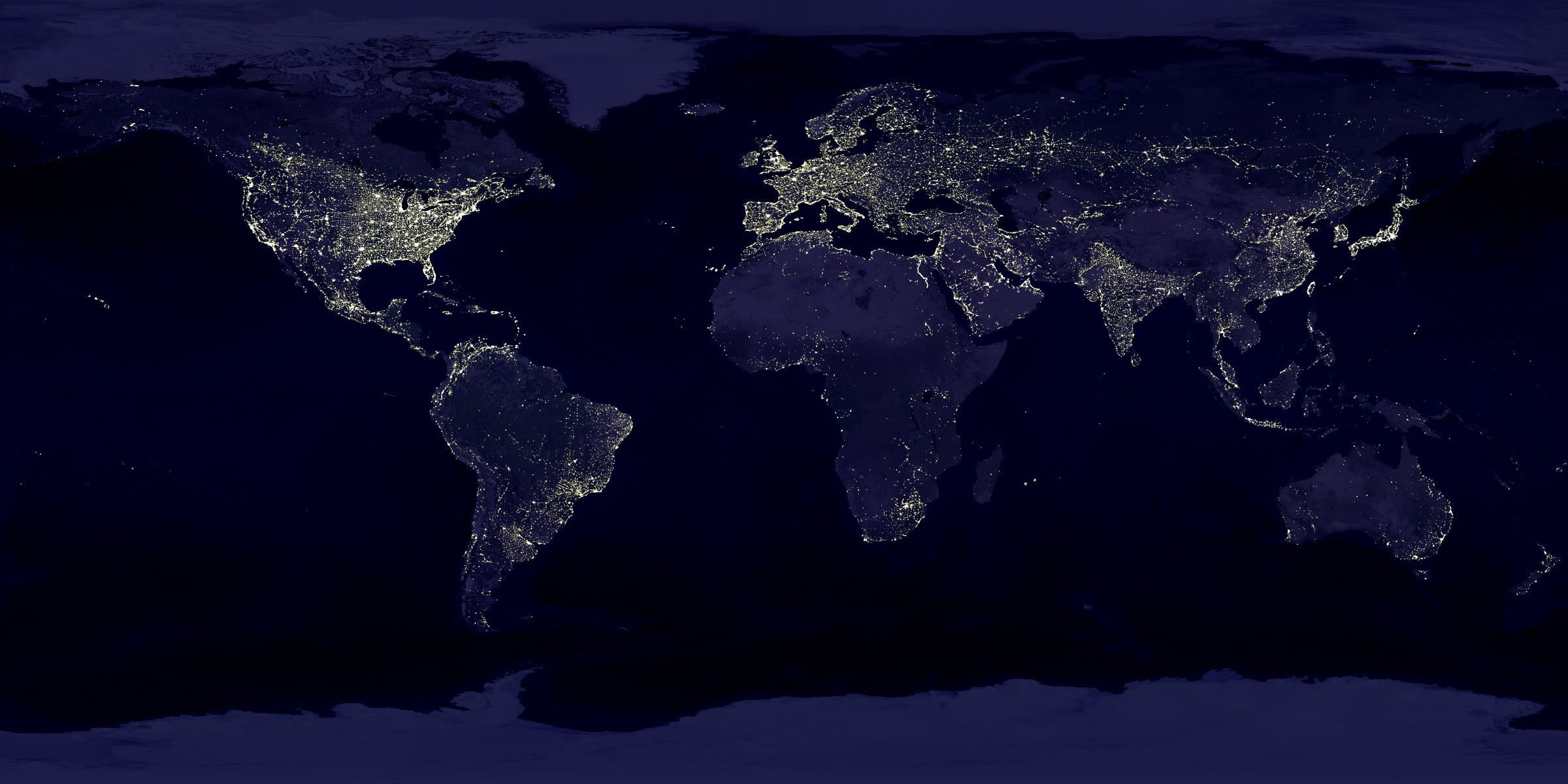
A significant proportion of the patient safety indicators (41%) are only available for High or Upper Middle-Income countries. Around a third of the indicators (32%) include data from East Asia and Pacific, Europe and Central Asia, and North America regions, which represents nearly three quarters (74%) of the world population.
Across many indicators, data is collected infrequently. For example, for one in six indicators, the most recent data is more than three years old. Of the 89 metrics we have selected for inclusion in the dashboard, no countries have all indicators populated. Australia, New Zealand and Norway are the countries with the highest availability of data with 75 populated indicators. The UK has 68 populated indicators. Changes in methods of data collection, and in the wording of some survey questions, makes comparisons and trend analysis challenging. Aside from recently piloted data by OECD, no new widely applicable patient safety indicators have been introduced for routine data collection in the past ten years.
Even looking at a subset of indicators, for a selection of comparable countries, differences in data completeness are stark. To illustrate this, we examined data completeness across OECD countries for 17 internationally recognised and collected indicators. These metrics were selected based on the following criteria:
- Internationally recognised and collected across a wide range of countries
- Closely linked to preventable harm
- Representative of different parts of the health system
- Aligned with the global patient safety movement towards a broader understanding of harm
The results are shown in Figure 3. Of the 17 metrics selected, only six are available for all OECD countries. Of these six, four are related to maternal and neonatal incidents. A key medication safety indicator (the proportion of the population who are chronic opioid users) is available for less than half of OECD countries.
At a country level (Figures 4 and 5 below), we see that only four countries report data on all 17 metrics. The UK reports data on 14 of the 17 – the three indicators missing are those related to medication safety. For the UK, and many other countries, data on these indicators are most likely available internally. Nevertheless, the lack of reporting at a global level represents a missed opportunity for benchmarking and shared learning. It is worth noting, however, that countries may be hesitant to report because they question the international comparability of some indicators. Improvements in coding practices and a nuanced approach to international comparisons are needed to reassure countries of the value of reporting at a global scale.
5.3 Data reliability
Even when indicators are reasonably well populated, there can remain challenges in determining whether lower rates of harm (or the contributors to harm) reflect better performance or poorer reporting. For example, for the Global Burden of Disease study to compile data on adverse effects of medical treatment, each eligible injury has to first be correctly documented and coded by each provider organisation within each country. Although each country is subject to the same methodology and process, variation is inevitable, and when this variation is unwarranted, it weakens confidence in the conclusions that can be drawn from the data.
5.4 Data usefulness
In 2022, we published a report on the national state of patient safety in England. The report highlighted a disproportionate number of lagging indicators (relating to outcomes after an event has occurred) compared to leading indicators (relating to the precursors to harm). Research has shown the value of collecting a variety of data – on harm, reliability, operations, anticipation and learning – to provide a fuller picture of safety within organisations, with work done to put this into practice in several countries (see case studies 3 and 4 below).
The global patient safety data include an array of lagging indicators, including data on mortality (and to a lesser extent morbidity and disability), and safety in surgery and post-operative care. It is encouraging to see the presence of some leading indicators around staff perceptions of safety and patients reporting a medical mistake, but these have only recently been introduced as pilot measures and still form the minority of indicators.
Case study 3: Safety measurement and monitoring framework
The Safety measurement and monitoring framework (SMMF) resulted from a research study which sought to answer the question, how safe is care today? The framework identified five questions that are necessary to ask to give a complete picture of an organisation’s safety: Has patient care been safe in the past? Are our clinical systems and processes reliable? Is care safe today? Will care be safe in the future? Are we responding and improving?
Case study 4: Situational Awareness for Everyone (S.A.F.E.)
Situation Awareness For Everyone (SAFE) is a collaborative programme developed by the Royal College of Paediatrics and Child Health UK, enabling clinical teams to improve communication, build a safety culture and improve outcomes for children.
The concept behind the programme is that patient safety should be about managing risk, not simply about responding to incidents. SAFE involves teaching clinical teams in a practical, jargon-free way, supporting them to understand what they do well, what needs to improve, and how they can measure the impact of changes they make.
Only 10 (11.1%) of the 89 indicators are compiled from data reported directly by patients, families or carers, or by members of the public (two of which are part of a pilot programme of data collection). This is a notable deficit, given the unique insights that the users of services have on the safety of services, and the role that feeling safe has on the patient’s overall experience of care. However, innovative work is happening at a local level to build on these insights, and to ensure patients and families have the agency to use them to help keep themselves safe. An example of this work is at Cincinnati Children’s Hospital, where families are supported to identify signs of deterioration in children on the wards and use that to trigger a rapid, specialist clinical response (see case study 5 below).
Case study 5: Family-activated medical emergency teams
Rapid response systems, comprising tools to identify deteriorating patients (such as monitoring of physiological markers) and a multi-disciplinary team (typically based within ICUs) to respond to medical emergencies, have been shown to reduce arrests and deaths in children in hospital. Typically ‘activated’ by clinicians, a team at Cincinnati Children’s Hospital developed a model where the emergency response team could be triggered by the families of hospitalised children.
There are no indicators that relate to more strategic, policy or leadership aspects of patients safety, but it is welcome to see work underway from WHO to survey countries on their progress in these areas, following publication of the WHO Global Patient Safety Action Plan 2021-2030 (see table below).
5.4.1 Monitoring progress against the WHO Global Patient Safety Action Plan 2021-2030 (GPSAP)
The WHO GPSAP provides a framework for countries to develop their national plans for patient safety and will help to ensure a strategic and coordinated approach to patient safety at a global level. To help monitor progress against the seven strategic objectives in the GPSAP, and the implementation milestones within them, WHO surveyed member states throughout 2022 and early 2023 on the extent to which they have the necessary systems and processes in place to progress patient safety. This includes, for example, whether there exists a national policy or framework for patient safety, and whether there is an integrated educational curriculum for patient safety. The final report, to be produced in 2023, will provide key insights into progress of member states in developing the necessary leadership, strategic and infrastructural elements for the delivery of safe care.
WHO published an interim report in April 2023, compiled of responses from 102 countries across all six regions. Progress against achieving the core indicators from the WHO GPSAP were measured:
· 27% of countries have developed a national patient safety action plan or equivalent
· 36% of countries have implemented a system for reporting of never events
· 18% of countries have signed up for implementation of the WHO Health Worker Safety Charter
· 31% of countries have established national targets on reducing health care-associated infection rates
· 13% of countries have a patient representative on the governing board (or an equivalent mechanism in 60% or more hospitals).
The dashboard includes indicators that may not traditionally be associated with patient safety, such as timeliness or patient-centredness. Discussions abound in the literature about where the line should be drawn between safety and quality; however, there can be little doubt that how people experience and feel about their care can result in psychological harm, and delays in receiving treatment can result in physical impairment or premature death, both of which are safety-critical issues.
Our patient safety data dashboard is undergoing an update May-June 2025. If you have any queries about the data while it is offline, please contact Melanie Leis.
6. Insights from the data
This section includes some selected highlights, trends, and opportunities for meaningful comparisons from the data, for the purposes of learning from those countries and regions performing well on different aspects of patient safety. This is far from a comprehensive analysis – instead, users are encouraged to explore the dashboard for insights most relevant to you. Our analysis is organised into our patient safety country ranking, overall observations, areas of improvement and areas of concern.
6.1 Patient safety country ranking
Using the methodology outlined in Section 3.2, Norway is at the top of the ranking for patient safety. The UK ranks 21st out of 38 countries, very close to the average across selected metrics, as shown in Figure 6.
In interpreting this ranking it is helpful to consider the following:
- Higher than average: The differences across the 23 countries that perform better than average are marginal – they are all within one standard deviation of the mean. The relative position of a country within this group should be considered with caution.
- Lower than average: Of the 15 countries that perform worse than average, only two (Colombia and Mexico) are beyond 1 standard deviation of the mean. The relative position of a country within the group of the remaining 13 countries should be considered with caution.
Additionally, this methodology has important limitations:
- The four indicators included only represent a small aspect of health system performance, with overrepresentation of maternal and newborn care. A more meaningful ranking would look at a broader range of indicators, but currently this is not possible because the data is not consistently reported.
- The indicators included only look at rates of deaths. The global patient safety movement has tried to move towards a broader understanding of harm including morbidity and psychological harm, but data across these other areas is still limited and inconsistently reported.
The patient safety movement has worked hard to encourage a cultural shift from blame to shared learning. We hope this ranking is a step in this direction, mobilising action and encouraging better data collection.
6.2 Overall observations
Two overall observations can be made by taking a high-level look at the global patient safety indicators:
- Many of the indicators show very little improvement in performance over time, often stretching back further than the data period under analysis in this report. In some cases, improvements in performance may be offset by improved reporting and data coding practices, but in others, this trend warrants further examination to better understand the causes. For example, there has been little overall improvement in performance on retained surgical item or device fragment – an area that has been subject to significant focus and improvement efforts in recent years (Figure 7).
- There is significant spread in performance, even between comparable groups of countries. Variation is, to some extent, to be expected between countries, allowing for contextual differences and the stage at which different countries may be on their patient safety journey. Significant variation between countries should act as a trigger for further enquiry, for example in the case of rates of maternal sepsis, Figure 8, to understand how much of the variation may be unwarranted – in other words, that which cannot be explained by, for example, population differences.
Our patient safety country ranking also highlighted the variation that exists across comparable countries. One way to illustrate the opportunities for improvement is to quantify deaths and DALYs (Disability-Adjusted Life Years) avoided if the UK performed at the level of the best performing decile of OECD countries. DALYs are defined as ‘the sum of years lost due to premature death (YLLs) and years lived with disability (YLDs). DALYs are also defined as years of healthy life lost’. In this instance they can help us to quantify the impact of death or disability from the adverse effects of medical treatment.
Using only the metrics included in the patient safety country ranking, we see that using the latest data available the UK could have had 17,356 fewer deaths and 15,835 fewer DALYs had it performed at the level of the top decile of OECD countries. Specifically:
- The UK had 48,482 deaths classified as treatable mortality in 2020. If the UK had matched the top decile this would have meant 15,773 fewer deaths.
- The UK had 1,484 deaths due to neonatal disorders in 2019. If the UK had matched the top decile this would have meant 776 fewer deaths.
- The UK had 34 maternal deaths in 2019. If the UK had matched the top decile this would have meant 27 fewer deaths.
- The UK had 1,266 deaths due to adverse effects of medical treatment in 2019. If the UK had matched the top decile this would have meant 780 fewer deaths.
- The UK had 25,883 DALYs due to adverse effects of medical treatment in 2019. If the UK had matched the top decile this would have meant 15,835 fewer DALYs.
6.3 Areas of improvement
6.3.1 Treatable mortality
Treatable mortality, as defined by OECD, refers to ‘causes of death that can be mainly avoided through timely and effective health care interventions’, and includes adverse events, sepsis, venous thromboembolism (VTE), and some forms of cancer. As shown in Figure 9, age-standardised deaths per 100,000 people due to treatable causes has, on average, fallen from 93.3 to 82.2 between 2010 and 2019 (pre-pandemic). Treatable mortality in the UK is below the OECD mean, but falls in the bottom half of OECD countries for this measure (Figure 10).
As described above, if the UK matched the top decile of countries, this would equate to 15,773 fewer deaths from treatable causes per year.
6.3.2 Maternal and neonatal deaths
The provision of safe maternity and neonatal services is a key priority for health systems globally, where birthing preferences for expectant parents must be balanced with ensuring safe outcomes for mothers and babies, often in time-sensitive situations. Expectant parents can be anxious about the delivery of their baby, with major institutional failings of care often adding to this concern. Several health systems, such as in Sweden, New Zealand and Japan, have developed schemes to both expedite the compensation process for families when a tragedy occurs during the delivery of a baby, and also to maximise the learning to prevent similar tragedies from occurring in future.
In 2021, the UK Parliament Health and Social Care Committee published its report on the safety of maternity services in England. The Committee heard evidence about the Swedish approach to compensation for medical injuries, which is awarded based on an expert assessment of whether an incident was considered avoidable, rather needing to prove negligence. The Committee reported that this approach, combined with increased transparency and a willingness to learn from incidents, has contributed to a 50% reduction in serious avoidable birth injuries from 2000 to 2016 in Sweden. The example of Japan also shows that such approaches provide better, and more timely resolution for families, and can be done so without any corresponding increase in the number of lawsuits (see case study 6 below).
Case study 6: No-fault maternity compensation schemes
Professor Shin Ushiro, Professor and Director of Division of Patient Safety, Kyushu University Hospital
As shown in Figure 11 below, overall rates of maternal deaths have fallen steadily from around 272 per 100,000 live births to around 157 between 2000 and 2017. This is a fall of nearly 42% worldwide, representing a major global achievement. However, inequities remain (see section 6.3.1), and there is still a long way to go to achieve the SDG Target of reducing maternal deaths to less than 70 per 100,000 live births.
During the same period, rates of neonatal deaths have fallen from around 33 per 1,000 live births to around 20 per 1,000 live births (Figure 12) and rates of stillbirths have fallen from 15 per 1,000 births to 11. During this time, the proportion of women receiving at least four visits as part of their antenatal care, and births attended by skilled health staff, has steadily risen overall (Figures 13 and 14). While the challenge in middle and high-income countries centres on providing safe and high-quality care, in many LMICs, access to skilled health staff remains a major challenge.
6.3.3 Safety in surgery and post-operative care
Surgical care is often cited as being a forerunner to developments in patient safety, from Semmelweis’s pioneering discovery of hand hygiene methods to the early adoption of non-clinical safety scientists in delivering improvements in anaesthesia. Six indicators within the dashboard relate to surgical or post-operative safety, collected by OECD.
Comparing the latest data available to that of 2010, the OECD average rates of post-operative wound dehiscence (separation) and deep-vein thrombosis have improved, while the rates of post-operative sepsis (abdominal discharges) and pulmonary embolism (hip and knee replacement) have remained broadly steady (see Figure 15).
The UK has fared slightly worse during this time, with a notable rise in cases of post-operative sepsis (abdominal discharges) from 1,604 to 4,298 cases per 100,000 hospital discharges between 2011 and 2020 (Figure 16), before falling to 2,708 cases per 100,000 hospital discharges in 2022.
6.3.4 Safety in mental health services
There are relatively few patient safety indicators that relate directly to mental health services, the most relevant of which is rates of inpatient suicide amongst patients diagnosed with a mental disorder, collected by OECD (Figure 17). Each inpatient death by suicide is a tragedy, with significant effect on both their family, and staff caring for the individual. Indicators are also included for suicide with 30 days (and 1 year) of discharge among patients diagnosed with a mental disorder.
A recent article, based on a Freedom of Information request, discovered 26,000 recorded sexual abuse incidents in mental health trusts over a five year period in England. The paucity of routinely collected data, combined with estimates of the scale and breadth of safety issues, makes the improvement of patient safety data in mental health settings a priority.
6.4 Areas of concern
6.4.1 Adverse effects of medical treatment
The Global Burden of Disease (GBD) Study collects data on adverse effects of medical treatment, which includes death or disability ‘sustained as a result of undergoing a procedure, treatment, or other exposure to the healthcare system’. In 2019, this led to 106,000 deaths worldwide. As illustrated in Figure 18 below, deaths caused by adverse effects of medical treatment have, on average, increased – from 1.5 per 100,000 in 2000, to 1.8 per 100,000 in 2019. During this time, rates in the UK have risen, from 1.3 to 1.9 per 100,000. The average disability adjusted life years (DALYs) lost due to adverse effects from medical treatment remained relatively stable, from 40.3 in 2000 to 41.1 in 2019, while in the UK this increased from 28.4 to 38.5 during the same period (Figure 19).
6.4.2 Inequities in maternity safety
Despite the overall progress noted earlier in maternal and neonatal deaths, 800 women around the world still died from preventable causes related to pregnancy and childbirth each day in 2020. A recent WHO report found that progress in tackling maternal and newborn deaths since 2015 has stalled, owing to the impact of COVID-19, rising poverty, and worsening humanitarian crises.
Progress in reducing maternal deaths is also offset by a steady overall rise in late maternal deaths (those that occur between six weeks and one year after delivery), suggesting greater levels of social inequality across many countries (Figure 20). However, work has been done at a local level to better understand how women from black and minority ethnic backgrounds suffer harm disproportionately during their delivery, and how improvement efforts can be targeted accordingly (see case study 7).
Case study 7: Addressing racial disparities in maternal morbidity
Dr Christina Davidson, MD, maternal fetal medicine physician at Bayler College of Medicine and Texas Children's Hospital.
6.4.3 Waiting times
In our 2022 report, we argued that the challenges of increasing waiting lists for planned care, falls in the diagnosis of some long-term conditions, and significant pressures on emergency services - all exacerbated by the pandemic – meant that “the lack of timely and equitable access to care should be considered an urgent patient safety issue”. There is, however, no standardised data collection that seeks to capture people’s levels of safety while they experience delays in their care. The closest proxy for this is data on waiting times, from specialist assessment to treatment for seven procedures, collected by OECD.
Across all of these procedures, the average waiting time has either remained steady, or worsened. The UK is broadly in line with these trends. One of these measures is for Percutaneous transluminal coronary angioplasty (PTCA), a procedure to open a blocked artery to the heart.
Analysis of data shows that, overall, these waiting times have remained broadly steady before increasing sharply in 2019 (before falling in 2020).
Rates in the UK have increased consistently during the whole period, from an average wait of 39 days in 2010 to 57 days in 2019 (Figure 21).
6.4.4 Patient experience
While ensuring access to care has become a preoccupation for every government’s health agenda, it is important that this is access to high quality care. One way to conceptualise this is the sufficiency of a patient’s interaction with their doctor during their consultation.
Overall rates across OECD countries in patients who feel that their regular doctor spends enough time with patients during their consultation have fluctuated, with satisfaction falling notably in 2020 (Figure 22), likely due to the impact of the COVID-19 pandemic. Since 2016, the proportion of satisfied patients fell from 89 patients per 100 surveyed in 2010, to 73 in 2020.
6.4.5 Medication safety
The risks to patient safety presented by medication errors led the WHO to select ‘Medication without harm’ as its third Global Patient Safety Challenge for 2017-22. However, harm caused by medication can also come, not from errors, but from decisions made about the best course of treatment. For example, opioids are effective analgesics for people experiencing acute pain or nearing the end of their life, but can be of limited use for people experiencing chronic pain, with such patients at risk of developing a long-term dependency on them.
Research has found significant heterogeneity across regions and countries in opioid prescription, which is reflected in the routine data on the chronic use of opioids is collected by the OECD (Figure 23). England (not shown in the chart) has recently begun a national safety improvement programme to reduce high dose prescribing of opioids for non-cancer pain by 50% by March 2024.
6.4.6 Staff and patient perceptions of safety
Perceptions of safe care, whether reported by staff or patients, is an important source of insight about the extent to which unacceptable risks exist within care systems and processes. While several regional or country level systems are in place to gather this important source of process data, very little data exists at a standardised, international level.
The OECD has recently piloted some measures, examining health worker perceptions of handoffs and transitions, safety culture, and overall perceptions of safety, and patients experiencing a medical or medication-related mistake. These are excellent examples of leading indicators, that, when used appropriately, can help to identify risks before they result in poor outcomes for patients. Patient perceptions of safety and risk, including at the point of discharge from hospital, have also been developed at a local level (see case studies 8 and 9).
Case study 8: Patient measure of safety
Professor Rebecca Lawton, Professor in the Psychology of Healthcare, University of Leeds, NIHR Yorkshire and Humber Patient Safety Research Collaboration.
Figure 24 illustrates significant variation across the participating countries for patients reporting a medical mistake during their treatment, while Figure 25 reports differences in health worker perceptions of handoffs and transitions and overall perceptions of safety. Both indicators offer valuable opportunities for countries to learn from what others are doing well in these areas.
Case study 9: Partners at care transitions measure
The Partners at Care Transitions Measure (PACT-M) is a patient-reported questionnaire to assess the quality and safety of care transitions from hospital to home for older patients (over 65 years old). The measure has been adopted by teams around the world, including in Denmark, China, Sweden and Bahrain, primarily for research or service evaluation purposes.
7. Conclusions and recommendations
Several insights can be drawn from our interviews with people who have developed innovative, patient-driven ways to measure and improve patient safety. First, patients, families, and carers offer insights into safe and unsafe care that cannot be obtained from existing sources – in the words of one interviewee, this is “novel not redundant information”. Second, patients, families and carers need to be empowered and encouraged by staff, and the wider system, to take a more positive and proactive role in patient safety – simply creating the opportunities alone is unlikely to be sufficient. Third, to ensure more widespread and effective adoption of patient, family and carer led improvement interventions, the practical steps involved need to be systematically recorded and shared – publishing findings in research papers is not the only route to achieving this.
In our 2022 report, we made several recommendations, including the need to increase the breadth of patient safety data collected at a national level. The report states:
“Data should reflect the reality of people’s journey through the NHS, capturing information on preventable harm across the entire continuum of care, not just when they go to hospital. Data should be collected in real time, and used routinely to trigger alerts into emerging safety issues. Data should better reflect how safe patients, families and carers feel, not just how safe they are clinically. Data should be targeted to understand whether some people are less safe than others, particularly those from disadvantaged or minority ethnic groups.”
Based on our analysis for this report, similar deficits in the global patient safety data can be observed. If data are to be used for understanding the current state of patient safety, for targeting improvement efforts, and for assessing the impact of these efforts, they need to better reflect the care journeys, perceptions, and experiences of patients – particularly for those patients who are our most vulnerable or disadvantaged members of society.
Our patient safety country ranking highlights existing variations in performance and clear opportunities for shared international learning. Nevertheless, better reporting is vital. Due to variations in reporting, currently a country with a strong incident reporting culture may have a higher number of patient safety incidents and hence appear lower in the ranking. It is imperative that improved data collection efforts are accompanied by a patient safety culture shift to address this.
Recent work by Vincent and Marang-van de Mheen (2023) challenges us to give less attention to the merits of individual indicators, and more consideration to the criteria and desirable characteristics of sets of indicators:
“Rather than accumulating and aggregating multiple individual indicators, in the hope that they will meet the needs of users and health systems, we could endeavour to define the fundamental purpose of indicator sets and then choose relevant component indicators.”
The authors pose a series of questions that ought to be addressed to shape and refine an indicator set, including: Who will be using it? What questions does it need to answer? How many indicators are needed? Will it have any unintended consequences? Most fundamental of all, the authors ask, what is the underlying construct?
In the context of a global indicator set for patient safety, and supporting 2023’s theme for World Patient Safety Day, this must now include consideration of the patient’s perspective of patient safety, their trajectory of care through complex health care systems, and any inequities in safe care on account of their demographic characteristics or socio-economic circumstances. Alongside the introduction of measures that offer insight into the fundamental components of a safe health care system, and other vital cultural measures, it should be possible in future to better understand the global state of patient safety.
Based on these conclusions, we make the following recommendations:
- Assessment: A more balanced and comprehensive set of global patient safety indicators is required to address the data gaps identified in this report, and to ensure comparable data is available for countries across all income levels. Consensus is required on the minimum set of indicators that all countries should report on. This work should involve key stakeholders including WHO, Ministries of Health, expert bodies, people with lived experience, and healthcare workers. The Ministerial Summits have highlighted the need for sustained and supported implementation of initiatives. National and civic leaders should support their systems, providers and frontline teams to ensure the data provided is as accurate and complete as possible.
- Adoption: A global repository of safety measurement and improvement interventions should be developed. Interventions should be recorded and uploaded using a common reporting framework, such as an adapted version of the TIDieR framework, to ensure consistency and support their effective adoption. Healthcare workers and researchers should be supported and encouraged to report their interventions to the repository as a matter of routine. This repository should be freely available to decision-makers at the health system, hospital and practice level, with the ability for each to action as relevant to their specific context.
- Activation: The adoption of patient-driven safety measurement and improvement interventions, including those featured in this report, must be accelerated. To ensure the faithful adoption of interventions, patients, families and carers must be given the agency to become active and equal partners in the delivery of safe care. Leaders within healthcare organisations must therefore ensure there is a culture of patient and family involvement across all safety improvement efforts.
Acknowledgements
This report was produced by Imperial College London's Institute of Global Health Innovation. It was made possible by the generosity of the charity Patient Safety Watch founded by the Rt Hon Jeremy Hunt MP, chaired by James Titcombe OBE.
The authors would like to thank the following people who have provided valuable input and advice in the production of this report: Niek Klazinga, Mike Durkin, Bryony Dean Franklin and Paul Aylin.
Special thanks go to the practitioners, advocates and experts who kindly gave their time to be interviewed for this work: Pat Brady, Christina Davidson, Peter Lachman, Rebecca Lawton, Anne MacLaurin, Afifa Munawar, Jane O’Hara, Deborah Prowse, Shin Ushiro and Jo Wailing.
Thank you to the team within the Institute of Global Health Innovation who reviewed and supported the production of the report: Amish Acharya, Sarra Khadir, Emily Medcalf, Victoria Murphy and Brittany Rae.
The authors received infrastructure support from the NIHR North West London Patient Safety Research Collaboration. Patient Safety Watch would like to thank Joe Kiani for Masimo Foundation’s financial support.
Suggested Citation
Illingworth J, Shaw A, Fernandez Crespo R, Leis M, Fontana G, Howitt P, Darzi A. Global State of Patient Safety 2023. Imperial College London (2023).