Diagnosis at another (micro) level
Using nanomaterials and biosensors, Imperial is transforming the way diagnoses are made.
Early, and accurate, diagnosis is key to better patient outcomes. We know this to be true for treatment and, as the global pandemic has highlighted, for controlling the spread of infectious diseases. But it is incredibly difficult to achieve. Blood tests lack the required sensitivity, rare diseases may not be immediately recognised, and access to healthcare is not universal.
At Imperial, Molly Stevens, Professor of Biomedical Materials and Regenerative Medicine and recently elected Fellow of the Royal Society, and her team are making groundbreaking advances in the field of diagnosis .
Using their unique position at the interface of chemistry, engineering and medicine, they are working to develop new biomaterials. In the process, they hope to democratise access to healthcare across the globe.
“We want to highlight the opportunity not only to make sensitive diagnostics but to combine them with mobile technologies,” Stevens says.
“To have this connected approach that can feed into online healthcare pathways, and hopefully transform the way that we can treat people within their community – both in early detection, but also in treatment and disease surveillance.”
Molly Stevens, Professor of Biomedical Materials and Regenerative Medicine and the Research Director for Biomedical Material Sciences in the Department of Materials, Department of Bioengineering and the Institute of Biomedical Engineering.
Molly Stevens, Professor of Biomedical Materials and Regenerative Medicine and the Research Director for Biomedical Material Sciences in the Department of Materials, Department of Bioengineering and the Institute of Biomedical Engineering.
It all starts with diagnosis. Point-of-care, equipment-free tests – to detect disease at a molecular level – are already in use, but, as Stevens points out, they are simply not sensitive enough. So, she and her team want to go further.
Not only are they developing ultra-sensitive nanomaterials for biosensing, but they are also manipulating what those materials can do.
It’s not just about making something, it’s about making the right thing.
In the case of HIV, “we wanted to develop a test that could detect the virus itself, in particular some proteins on the surface of the virus called p24. That meant we needed new types of technology to give us really sensitive results.
“We work with nanoparticles: if you shrink the Sun down to the size of a football, then shrink it down by the same amount again, that’s the size we’re talking about.
“These particles can be made of different materials, but we are interested in creating materials that generate colour changes. Then you can take those particles and decorate the surface of them with molecules that bind to the virus, and you’ll be able to know if the virus is present.”
The tests look like a standard pregnancy test and work in a similar way, using biological material such as blood or urine to produce a colour change in the presence of disease-indicating markers.
Stevens’ lab also works with state-of-the-art microscopy, some of which, such as SPARTA, her team developed.
"You know you have a high-quality product if you can visualise it,” she explains, “so we use electron microscopy and chemical imagery. It’s not just about making something, it’s about making the right thing."
Microplate washer for immunosorbent assay experiments
Microplate washer for immunosorbent assay experiments
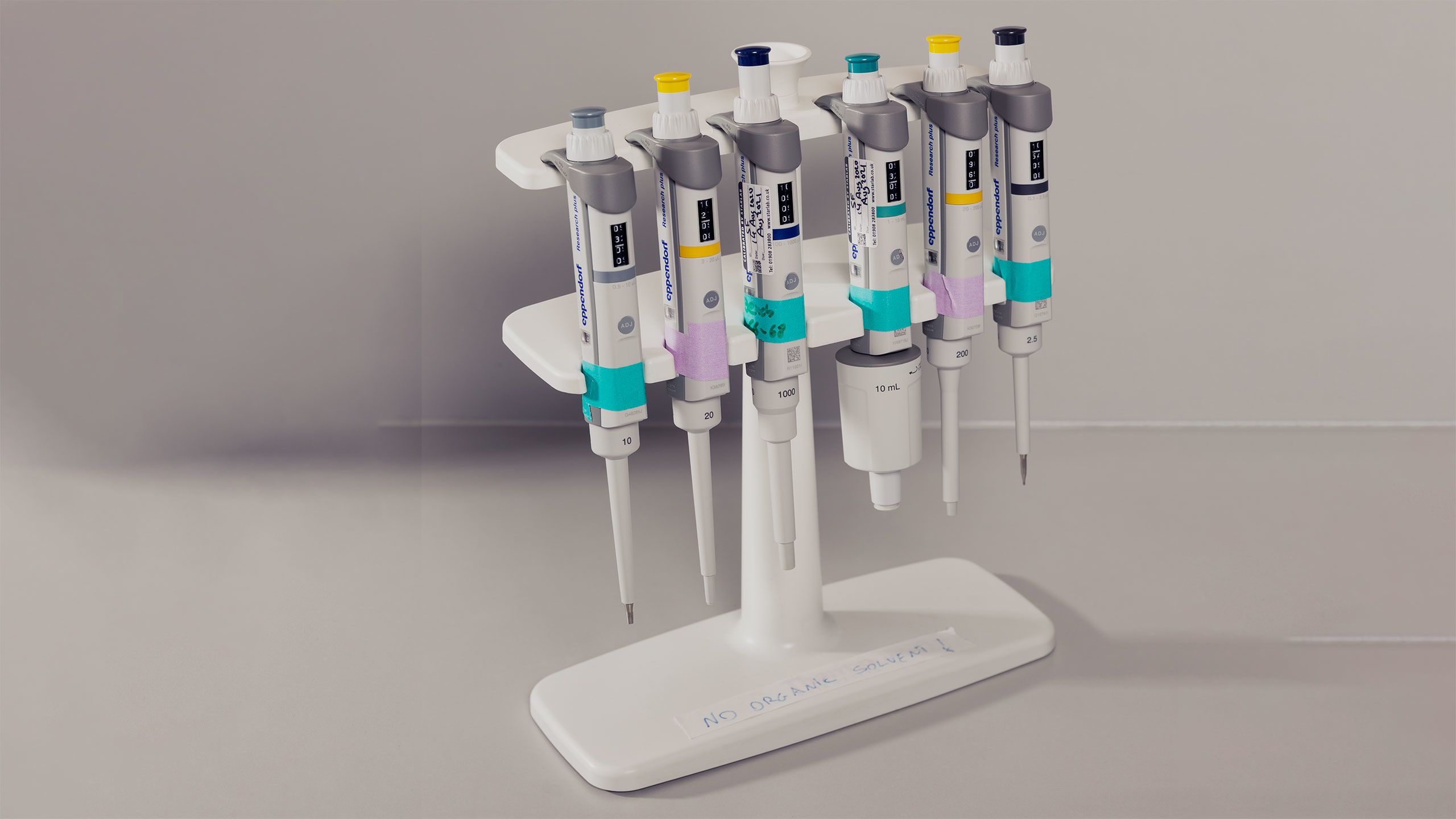
Mechanical pipette media dispensers
Mechanical pipette media dispensers
Elsewhere, in pre-clinical work involving animals, Stevens is using that same principle – manipulating molecular behaviour – but inside the body for non-communicable diseases.
“We are developing powerful biosensing particles that tell us about diseases inside the body,” she says, “such as cancer but also malaria, for example. It works by detecting enzymes – we know about enzymes for digesting, but they also have lots of different functions. If you have cancer, you have a different level of certain enzymes from the normal baseline level in a healthy person.
“Along with MIT in the United States, we have developed tiny gold particles that are held together in clusters, but when they come into contact with these cancer-indicating enzymes they break apart. Those particles then disperse and become small enough to be filtered through the kidney and passed out in your urine.
“Once in the urine, we can add simple chemicals and the urine will turn blue. We don’t need complicated equipment to read it; it can be seen by the eye, and the urine will turn blue less than an hour after you’ve done the test.”
It is a marker of Stevens’ work that this test is not only scientifically sophisticated, but is also easy to use, even in a remote healthcare setting.
“You can elegantly design materials that will be written about in scientific journals,” she reflects, “but what will you do with them? How will you make them useful to society? That’s always in my mind.”
The team (left to right): Brian Chen, Research Postgraduate; André Shamsabadi, Postdoctoral Research Associate; Leah Frenette, Postdoctoral Research Associate.
The team (left to right): Brian Chen, Research Postgraduate; André Shamsabadi, Postdoctoral Research Associate; Leah Frenette, Postdoctoral Research Associate.
As she told the World Economic Forum at Davos: “Infectious diseases disproportionately affect low- income countries. HIV, AIDS, malaria and Ebola all have a devastating effect on these countries. We need to come up with diagnostics that can be cheaper, simpler, more effective and globally accessible, which can help with democratising access to healthcare.”
The Stevens Group’s point-of-care tests, such as the one for HIV, are designed to cost less than a dollar, and work in conjunction with mobile phones .
“We are used to using mobile phones for web searches and social media,” she says, “but they can have really important applications when we use them connected to lab tests and as diagnostic tools; when we think of them as portable mini-computers.”
Stevens cites the eight billion mobile phone subscriptions worldwide – a number that is growing by the minute, even in places like sub-Saharan Africa.
In Uganda, for example, she says, 20 per cent of people live more than 5km from a healthcare centre, but many of them still have access to a phone signal, despite persisting inequalities of access to phones, such as in age and gender.
You can elegantly design materials that will be written about in scientific journals, how will you make them useful to society?
“We’re interested in the camera capabilities of the phone,” she says, “so you can read the test result with a mobile phone and transfer the data through wireless connectivity. The i-Sense centre that Stevens is deputy director of has developed an app to analyse test results.
“We can then work with healthcare professionals to place that patient into a healthcare pathway. In South Africa, for example, it can take a year after a test to get into a treatment programme.
“i-Sense has been working with partners at the Africa Health Research Institute who have trained community field workers to carry out tests and get the patients into care.”
Marta Broto Aviles, Postdoctoral Research Associate.
Marta Broto Aviles, Postdoctoral Research Associate.
Being able to build a very large dataset of people is also incredibly important for monitoring the way a disease spreads.
“In Uganda, we are looking at serological surveillance, at people who have had Ebola and survived, and detecting between three different species of the Ebola virus.
“This is important in understanding how the disease is spreading. We have developed a multi-marker test and an app that can generate geotag maps of spread.
“There are challenges around data and privacy, but we are engaged with ethicists and others in the community to get this right. It means we can then understand how to control the disease.”
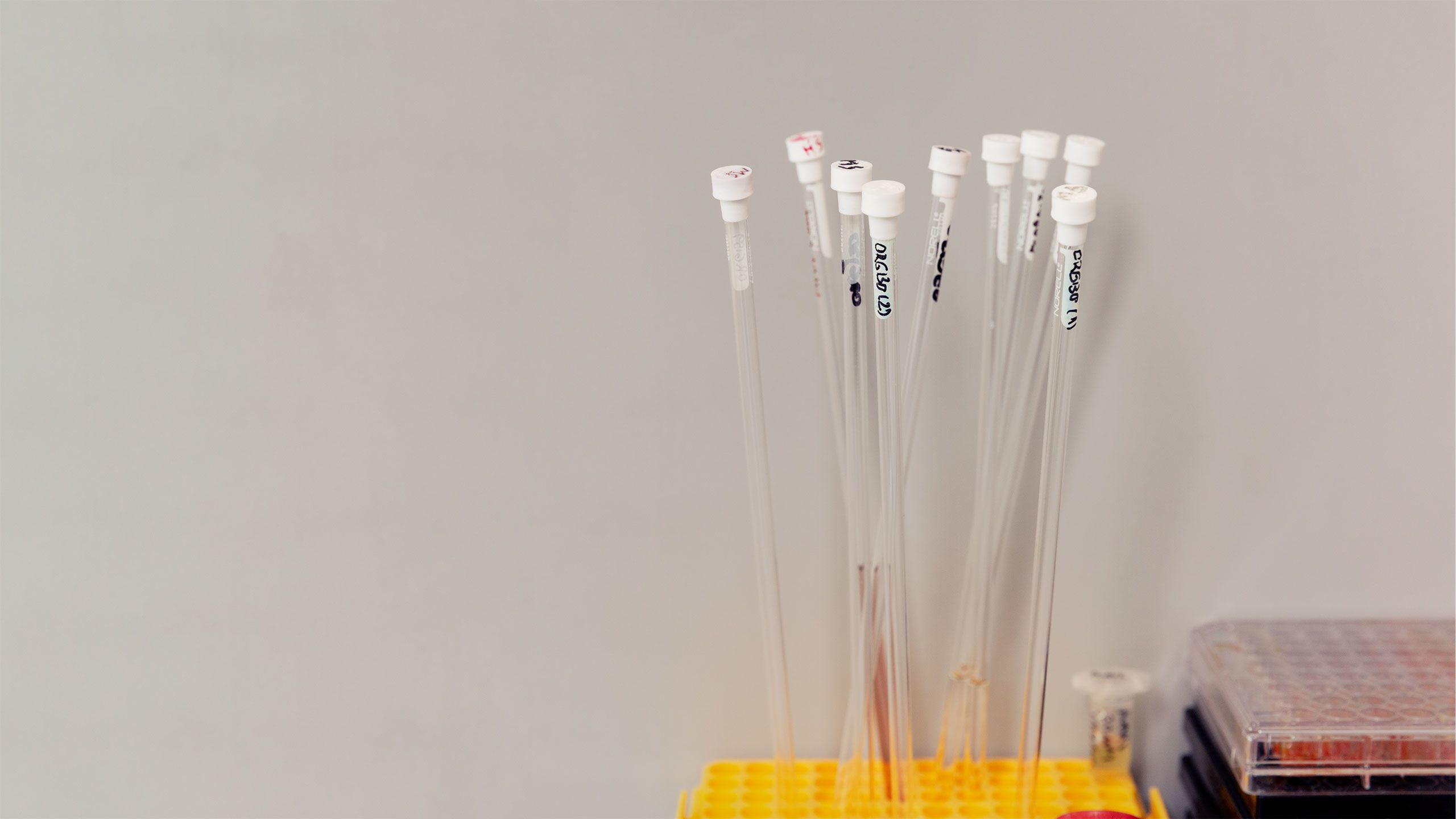
A machine showing a non-amplified LFIA dipstick assay with serial dilution of protein.
A machine showing a non-amplified LFIA dipstick assay with serial dilution of protein.
During the COVID-19 lockdown, Stevens assembled a crack team of volunteers from all over the world to work on a portable, point-of-care test called QwikZyme.
It is designed to detect coronavirus very early, even in asymptomatic people, and to allow ongoing immune-response monitoring.
“This work is in its very early stages,” she says, “but we have had an incredible response. We had a core team of 25 based at Imperial and we collaborate with different groups all over the world.”
COVID-19 may have brought home the importance of infectious-disease control to countries that are not used to having to worry about it too much, but Stevens’ approach is always global.
Technology is amazing, and, if you design it right, it can make a real difference
“There are many diseases that are not as prevalent in the developed world and it’s important to achieve control of these,” she says.
“It’s also important to prevent their spread, as has come to the attention of the developed world during COVID-19. Enabling all sectors of society to have access to early disease diagnosis, from cancer to cardiovascular disease to infectious diseases, is of massive societal importance.”
This is a motivation she has transmitted to her passionate and committed team at Imperial.
“I did a PhD in fundamental biophysics, about how molecules interact with each other, and I loved it,” she says.
“But, actually, being able to take the joy of science, and the interest of it, and make technology that really helps people, is something else.
“I travelled a lot in countries in the developing world before and after my PhD, and I saw a lot of inequality. I think technology is amazing, and, if you design it right, it can make a real difference.”
Imperial is the magazine for the Imperial community. It delivers expert comment, insight and context from – and on – the College’s engineers, mathematicians, scientists, medics, coders and leaders, as well as stories about student life and alumni experiences.
This story was published originally in Imperial 49/Winter 2020–21.