Women’s Health
Women's health is in crisis; Imperial experts are calling for a fairer system that works for everyone.
By Dr Anna Ploszajski for The Forum, Imperial's policy engagement programme.

Women’s healthcare in the UK is in crisis.
Although women slightly outlive men, women in the UK spend a greater proportion of their lives in ill health or disability compared to men – around a quarter for women and a fifth for men1. And these figures are getting worse – healthy life expectancy at birth has fallen for women since 2014, but has remained stable for men. A woman born between 2017 and 2019 could expect to live an additional year in suboptimal health than a woman born in the UK between 2014 and 2016. There was no significant change for males across the same period. In other words, these numbers show that women are suffering in a health service not designed for them.
How did we get here?
“Some years ago, I pushed the Secretaries of State Jeremy Hunt and then Matt Hancock to have a Women’s Health Task Force”, says Professor Dame Lesley Regan, Professor of Obstetrics and Gynaecology, Imperial College London and newly appointed Women’s Health Ambassador for England, Scotland and Wales, “I argued that women had been disproportionately disadvantaged by many of the funding cuts since the 2012 Health and Social Care Act, which accelerated after 2014 when Public Health England lost 40% of their budget.
I argued that women had been disproportionately disadvantaged by many of the funding cuts...
“The net result is that we now have a 45% unplanned pregnancy rate, cervical screening is at an all-time low, while abortion rates are at an all-time high, mostly explained by the fact that women face numerous barriers when trying to access routine health maintenance services,” Professor Regan exclaims.
She blames these figures on a lack of accountability in how healthcare is funded. “Women’s health services like cancer screening, contraception, abortion and maternity services have been in three silos of commissioning – Clinical Commissioning Groups, local authorities and NHS England… None of those three funding pots picks up the pieces when they don’t get it right; the people that don’t give you contraception aren’t the ones to pick up the maternity bills or the abortion bills.
Professor Dame Lesley Regan, Professor of Obstetrics & Gynaecology, Imperial College London.
Professor Dame Lesley Regan, Professor of Obstetrics & Gynaecology, Imperial College London.
St Mary's Hospital, member of the Imperial College Healthcare NHS Trust
St Mary's Hospital, member of the Imperial College Healthcare NHS Trust
“So, I started the Task Force and co-chaired it with Jackie Doyle-Price MP. We got an enormous amount of traction and dealt with very taboo subjects: problem periods, mental health, domestic violence… At the end of 2019 we published the Better for Women report which included 23 recommendations [to the government]. We started on a few of them and then three months later, lockdown came.”
Jackie Doyle-Price MP for Thurrock and former health minister
Jackie Doyle-Price MP for Thurrock and former health minister
And there, it seems, action on women’s health stalled. Fast forward to today and the government has just published its Women’s Health Strategy for England which seeks to resume this action and address inequities in the lives of women. It focuses on a number of themes, such as understanding women’s changing healthcare needs over the life course, strengthening women’s involvement in research, and understanding the impacts of COVID-19.
To inform the Strategy, the government issued a Call for Evidence in March 2021, aimed at members of the public from all ages and backgrounds. They hoped that by collecting the lived experiences of women, they would be “re-setting the way in which the government understands women’s health, with a renewed focus on listening to women’s voices,” according to Nadine Dorries’ ministerial foreword to the Call.
As well as the public consultation on personal experiences, the Call also invited written submissions from individuals and organisations with professional expertise in women’s health. A consortium of experts at Imperial compiled a submission, from gynaecological Clinical Professors and Readers in HIV medicine to policy engagement professionals, global health experts and medical statisticians. I spoke to ten of them from across the university to paint a fuller picture of the context of women’s health in the UK, to hear about the work being done at Imperial to improve women’s lives in this area, and to find out what work is still left to do.
The UK government released a call for evidence for its Women's Health Strategy earlier in the year.
The UK government released a call for evidence for its Women's Health Strategy earlier in the year.
Dr Ed Mullins, Clinical Lecturer at Imperial and The George Institute for Global Health, coordinated Imperial’s response.
“The idea of doing this had two edges. First, to get the research being done at Imperial onto a minister’s desk with a series of small, ready to go policy initiatives based on each research area. The second was to get Imperial to have a look at its own women’s health research. There’s a lot of it going on but there’s a lack of strategy, a lack of cohesiveness. That’s what we’re hoping to springboard off by doing this…”
Dr Ed Mullins, Clinical Lecturer at Imperial and The George Institute for Global Health.
Dr Ed Mullins, Clinical Lecturer at Imperial and The George Institute for Global Health.
Women’s involvement in research

One of the central themes which arose in my conversations with Imperial’s academics was the negative impact of excluding women from research. Professor Neena Modi, Professor of Neonatal Medicine at Imperial and Consultant in Neonatal Medicine at Chelsea and Westminster NHS Foundation Trust and the immediate past-president of the UK Medical Women’s Federation, gave me a recent example.
“It was a triumph of science to produce so many COVID-19 vaccines so quickly. Scientists really saved the world,” she says, “but no one who was pregnant, might become pregnant or were breastfeeding were included in the original vaccine trials.
“No one who was pregnant, might become pregnant, or was breastfeeding were included in the original COVID-19 vaccine trials..."
“This meant that those who were pregnant or breastfeeding were prohibited from taking the [COVID-19] vaccine when it first became available in December 2020, and the advice didn’t change until April 2021,” she says. “So, a woman who was breastfeeding had to make this completely unacceptable choice pitting her own wellbeing against the wellbeing of her baby. To place anyone in that kind of situation is quite frankly unethical. And yet it is exactly what happened.”
I – like, I suspect, many members of the public – assumed that this exclusion was for the health and safety of women and their babies. In fact, those who are pregnant or breastfeeding wouldn’t usually take part in the higher-risk first-in-human or early drug studies for these very reasons. But Professor Modi tells me their exclusion from the COVID-19 vaccine trials was due to something else entirely.
Professor Neena Modi, Professor of Neonatal Medicine at Imperial and Consultant in Neonatal Medicine at Chelsea and Westminster NHS Foundation Trust
Professor Neena Modi, Professor of Neonatal Medicine at Imperial and Consultant in Neonatal Medicine at Chelsea and Westminster NHS Foundation Trust
“It harks back to the old paternalistic view of research, which was built on the view that women and children and other vulnerable groups need to be ‘protected’ against the ‘dangers’ of research.
“There is some justification for this, but it’s not absolute. Firstly, the WHO have made a very strong case that the inclusion of these groups should be the default, unless there is a very good biological reason for their exclusion. If you don’t include them by default, then this paternalistic protectionism means that they miss out on benefiting from research, which is exactly what happened during COVID.
It harks back to the old paternalistic view of research, which was built on the view that women and children and other vulnerable groups need to be ‘protected’
“The UK government was the first in the world to licence the use of the COVID-19 vaccine, but it wasn’t made available to those who were pregnant, might become pregnant or were breastfeeding. That’s totally ludicrous! Firstly, to conflate breastfeeding with pregnancy is embarrassingly bad science; they are two physiologically very distinct periods in the reproductive life of a woman. There were no good biological reasons to exclude lactating women. There was possibly reason to exclude someone who was pregnant on the grounds that they might be more vulnerable to acute respiratory complications of COVID-19 vaccines. But there was no a priori reason on the basis of the nature of the vaccines; mRNA types of vaccines [like the Pfizer COVID-19 vaccines] have been previously safely used in pregnancy, so there was no reason to fear on biological grounds that the vaccine would affect the foetus.”

A Specialist Biomedical Scientist at Imperial Healthcare NHS Trust.
A Specialist Biomedical Scientist at Imperial Healthcare NHS Trust.
Professor Graham Taylor, Professor of Human Retrovirology in Imperial’s Department of Infectious Diseases
Professor Graham Taylor, Professor of Human Retrovirology in Imperial’s Department of Infectious Diseases
It’s a common story in women’s health; by excluding women from clinical trials, dose, efficacy and safety data on drugs used in pregnancy are not ascertained in the safe and controlled environment of a clinical trial, but only slowly emerge from clinical use; this exposes women and their babies to many hazards.
“This means many drugs we use to treat conditions in pregnancy are being used off-licence,” says Professor Phil Bennett, Professor of Obstetrics and Gynaecology, “in other words, the drug company doesn’t recommend you use it for that purpose, not because they think it will be bad, but because they don’t know that it won’t be bad.”
Where does that leave clinicians? “Some treatments have been used for so long in so many people that we know they’re safe, even though the drug companies have never done studies on that,” says Bennett.
We need to change the whole way in which not just academia, not just pharmaceutical companies, but regulators and ethics committees think about pregnant women.”
And where does that leave women? “Hugely disadvantaged,” says Modi.
“You only get the data when they’re not in the study,” says Professor Graham Taylor, Professor of Human Retrovirology in Imperial’s Department of Infectious Diseases, “and when the data happens by chance when a woman gets pregnant randomly in the community, if you get the data at all. We need to change the whole way in which not just academia, not just pharmaceutical companies, but regulators and ethics committees think about pregnant women.”
Data and disaggregation

Women’s participation in clinical trials is only the first step. There also needs to be improvements in how that data is handled to draw the most scientific conclusions. This is the area of study of Professor Mark Woodward, Chair of Statistics, Epidemiology and Women’s Health in Imperial’s School of Public Health and The George Institute. It all started back in 2005…
“It was more than 15 years ago that I noticed that a lot of the risk factors for coronary heart disease acted more strongly in women than in men. For example, women were found to have roughly a 50% higher risk for coronary heart disease than men if they had diabetes. In other words, having diabetes approximately doubled the chance of a future heart attack in men, but tripled the chance for women.”
Back then it was all a weekend job for me, I never had any funding for it. I applied many times but nobody seems to recognise this area of work very well.....
This is called disaggregating data – analysing data from women and men separately. Without disaggregation, the data would show that having diabetes increased the risk of a heart attack for the average person by 2.5 times, masking the elevated dangers for some women.
“Back then it was all a weekend job for me, I never had any funding for it. I applied many times but nobody seems to recognise this area of work very well.”
That Professor Woodward couldn’t get further funding after such a staggering finding speaks volumes about how unimportant women’s health research was thought to be in the scientific community, including the research councils who allocated funding, and Professor Woodward’s own scientific peers who would have reviewed his proposals for the funders.
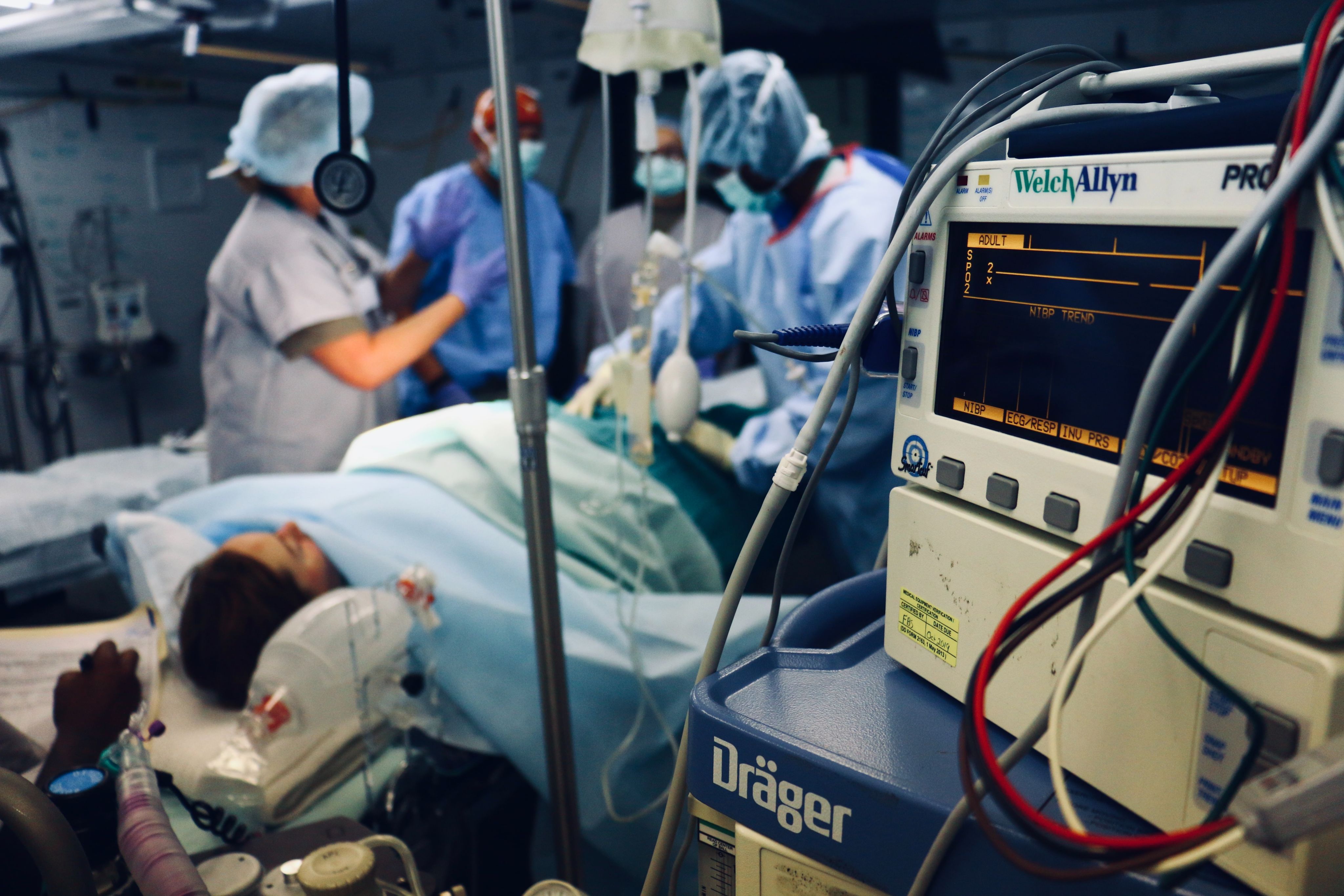
Professor Woodward’s methodology of disaggregating sex and gender data was relatively rare in medical research at the time, because it treated differences between women and men as a subject of primary importance, rather than as an inconvenience that could be adjusted away in the numbers to draw a general conclusion about risk factors associated with diseases.
He published his findings in 2006 and found it was the same story for women’s risk associated with smoking and heart disease. “We’re now looking at sex and gender differences in lung cancer, dementia and kidney disease and finding similar sex and gender differences in risk factor associations,” he says.
Dr Carinna Hockham, a Postdoctoral Research Associate in Epidemiology at The George Institute for Global Health, Imperial College London.
Dr Carinna Hockham, a Postdoctoral Research Associate in Epidemiology at The George Institute for Global Health, Imperial College London.
These diseases all fall into the category called non-communicable diseases (i.e. non-infectious), and I spoke to The George Institute’s Dr Carinna Hockham about her post-doctoral research into sex and gender differences in this family of diseases.
When it comes to data interpretation, adding both a sex and gender lens is really important but the data don’t always allow us to do this well.
“We wanted to broaden how we talk about women’s health, and recognise that women’s health is more than just maternal and reproductive health. In fact, non-communicable diseases are the leading causes of death and disability in women worldwide,” she tells me. “When it comes to data interpretation, adding both a sex and gender lens is really important.”
Biomedical data collection has traditionally followed a historical binary definition of sex and gender. Yet research is starting to recognise the importance of recognising how a spectrum of these characteristics can impact healthcare experiences. How are sex and gender differences approached in this sort of research? Sex, Dr Hockham tells me, is rooted in a person’s anatomy or physiology and is assigned at birth based on their genitalia or reproductive organs. On the other hand, gender is a social construct, reinforced through societal expectations of what it means to be a particular gender, and played out in a myriad of ways – from lifestyle and health-seeking behaviours to how other people treat them. This can all have a hand in health outcomes.
“More often than not, a participant’s sex is collected with no distinction between this and their gender. Without having data on gender as well, it can be hard to draw conclusions. You end up with this big tangle of biological factors and social factors, and people who fall outside of the binary are invisible,” says Dr Hockham.
Professor Robyn Norton, Principal Director of The George Institute for Global Health and Chair of Global Health at Imperial
Professor Robyn Norton, Principal Director of The George Institute for Global Health and Chair of Global Health at Imperial
“Frankly this is all about doing better science,” says Professor Robyn Norton, Principal Director of The George Institute for Global Health and Chair of Global Health at Imperial, “but could potentially improve the health of women and other disadvantaged populations. We’re looking at current policies across medical research that will help us to ensure that people are undertaking, producing, analysing, disseminating, and using research that disaggregates data, to understand the biological and sociological contributions to health. We’re working with major UK health funders to co-create policies that would ensure women are appropriately included in research and that data is disaggregated by sex and/or gender. It’s exciting for us to be part of the academic team to be bringing about change in this area.”

Women’s health and the economy

“Women’s health has for far too long been kept in a little box marked Women’s Health, and its broader relevance to society, the economy and national wellbeing hasn’t been recognised,” says Professor Neena Modi.
“From a biological and scientific perspective alone, women’s health is far broader than the health of women; it directly affects the health of the population, and the health of the population is critical to any nation’s resilience. We saw this played out during COVID-19. There was this incredibly superficial and naïve dialectic which pitted the economy against health in an extraordinarily ignorant way. If you have an unhealthy population, you’re clearly not going to have a healthy economy.”
It is what the government’s Women’s Health Strategy means by a ‘life course approach’; paying closer attention to the wider determinants of health and taking preventative actions to improve healthy lifespan. Professor Phil Bennett gave me an example from his field of Obstetrics and Gynaecology.
Professor Phil Bennett, Professor of Obstetrics and Gynaecology and Honorary Consultant in Obstetrics and Gynaecology to Imperial Healthcare NHS Trust
Professor Phil Bennett, Professor of Obstetrics and Gynaecology and Honorary Consultant in Obstetrics and Gynaecology to Imperial Healthcare NHS Trust
“The birth of a pre-term baby is the beginning of a long and expensive journey,” he says. “People think of the expense of being in the neonatal unit – which costs thousands of pounds a day – but, of the babies that survive from the limits of viability (around 24 weeks), about a quarter of them will be seriously handicapped. That’s an enormous social cost to the parents as the child grows up and becomes an adult. You could probably dramatically reduce all those costs if you just kept the baby in the uterus for another four weeks. We have programmes trying to identify why babies are born pre-term and develop treatments to prevent it and the big knock-on that follows.”
These interventions all cost money in the short term – like funding Professor Bennett’s research into the vaginal microbiome’s influence on pre-term births – and the payoffs may often not be seen for a long time. But the Imperial submission also identifies a lot of low-hanging fruit where the benefits of short-term investments could be felt much sooner.
Public Health England have calculated returns of £16 for every £1 spent on contraception administered in the hospital post-delivery, simply because the women are already in the service"
“You can save money by spending a little, it’s pretty stunning,” says Dr Ed Mullins. He gives me the example of a new initiative which he and colleagues have launched across the Imperial College Healthcare NHS Trust, providing women (and others) who have just given birth the option of going home with the contraception of their choice, rather than leaving them with the instruction to go their GP. “Public Health England have calculated returns of £16 for every £1 spent on contraception, simply because the women are already in the service,” he says.
This initiative is one example of where the COVID-19 pandemic actually had a positive impact on women’s healthcare. “It took me 30 years of arguing for this and I always got ‘no’,” says Professor Lesley Regan, “then we got it over the line in a week during the lockdown. People who knew what they were doing on the frontline were able to just say ‘this is how we’re going to solve the problem’. I don’t think it was to do with money or the virus, it was the exit stage left of all the middle manager tape.”

When it comes to policy, Professor Regan makes the economic argument for overhauling the way that women access health services to do what she calls ‘maintenance stuff’.
“At the moment you can’t go to a single clinic appointment and get your smear, STI check, breast check and get your contraception sorted. You should be able to go for a half an hour appointment, take your underwear off once and get three of those things done. Instead, we make the women go round the services which are incredibly expensive in a structure that disincentivises women – why would you want to go to four different appointments when you could do it all in an hour?
“Policymakers need to think of the cost-benefit analysis of getting it right, by having Well Women centres that can do all of these things. It’s one of my real contentions with the way we deliver health services to women – most of the time they’re not sick, they’re just trying to do normal things like access contraception or have a baby. Being pregnant is not an illness.”
Professor Marta Boffito, Clinical Reader at Imperial in HIV medicine
Professor Marta Boffito, Clinical Reader at Imperial in HIV medicine
Fragmented services were also a central theme in my conversation with Professor Marta Boffito, Clinical Reader at Imperial in HIV medicine. “We’re not understanding the needs of women living with HIV. The majority of women living with HIV in the UK are from particularly marginalised populations, and they experience incredibly high levels of stigma. This means their access to care is limited, they’re fearful, and they struggle to engage with HIV and other types of healthcare. This is because the care is fragmented, leaving them having to face telling their HIV story every time they need help, so they just don’t seek help anymore. It’s very complicated, but it’s actually also quite simple to understand.”
Professor Boffito welcomes the government’s consultation because in her view it could be a good way of involving patients when redesigning or restructuring services. “You often hear ‘give women a voice’, well we’re actually a step before that. We don’t even know how to listen to their voices, that’s how behind we are. We have set up services for white MSM [men who have sex with men] and we’re very good at delivering that care. The number of new HIV infections in MSM is falling very rapidly. But in heterosexual cis-gendered women it’s stable, because we don’t have the right tools and the knowledge to target them.
“In my experience, women from the HIV community want clinics dedicated to women. They need peer support from women and integrated mental health services with HIV services. We need funding for campaigns to break down societal, medical and internalised stigma. The advice [the women] give you is key to understanding how services should be structured and where the funding should go.”
Fragmented care for transgender women
Fragmented care seems to be a recurring theme in women’s health and is certainly true for transgender and gender-diverse people accessing the full spectrum of healthcare. And a 2022 report from the London Assembly Health Committee suggests we have a long way to go…
In the UK, there are just 16 NHS Gender Identity Clinics currently set up to provide gender-affirmative healthcare. Up until last month, there had been 17, but the recent closure of the only dedicated clinic for children and young people means that already long waiting times between referral and first appointment will only increase further.
A portion of the remaining clinics also provide sexual health, HIV and mental health services. But what of transgender women’s health needs outside of this narrow view of trans experiences? The grim truth is we don’t really know. NHS IT systems do not allow a person’s trans history to be captured in a consistent way. As a result, unless a transgender woman decides to disclose their trans status at every interaction with the health service, it is difficult for them to receive the right medical advice for their needs, and invitations to attend relevant life-saving screening programmes are easily overlooked.
To truly address gender-based disparities in health and healthcare, we mustn’t forget the unique inequalities faced by transgender women and gender-diverse communities and we must push for better and consistent reporting of sex and gender information in NHS systems. Without this, they will remain invisible, and we will have failed in our quest for gender equality.
The Women’s Health Strategy is a collation of women’s views and expert testimonies to decide what needs to be done to improve women’s health.
The Women’s Health Strategy is a collation of women’s views and expert testimonies to decide what needs to be done to improve women’s health.
The big question now is: will this time be any different?
Dr Mullins, despite coordinating Imperial’s response to the Call, is sceptical. “I have to say that a problem with women’s health has never been a lack of evidence about what we should be doing, rather the willingness and the priority to do it. In [the Imperial response’s] summary, there’s a lot of blindingly obvious things that need to be done, but a huge amount of inertia on doing it. So, I really have no idea how useful this is going to be,” he shrugs.
I have to say that a problem with women’s health has never been a lack of evidence about what we should be doing, rather the willingness and the priority to do it.
But Professor Boffito is more hopeful, “I think this [government consultation] was incredibly well done. Hopefully it will increase equity in access to care for women who don’t have the same chance to access services. It’s really unmasking and highlighting what their needs are.”
I think this [government consultation] was incredibly well done. Hopefully it will increase equity in access to care for women who don’t have the same chance to access services.
The task ahead of overhauling the current health system and reversing the downward trends in women’s health is mammoth. It will require a coordinated effort from experts across institutions like Imperial, direct lines of communication between researchers and policymakers in government and funding bodies, and commitment by those policymakers to act.
“My optimism says at least there has been a consultation”, says Professor Regan, “but my impatient side says ‘well we knew all this nearly two years ago’. All these same people contributed to the Better for Women report too, but I suppose that’s what happens in politics…”
Useful links:
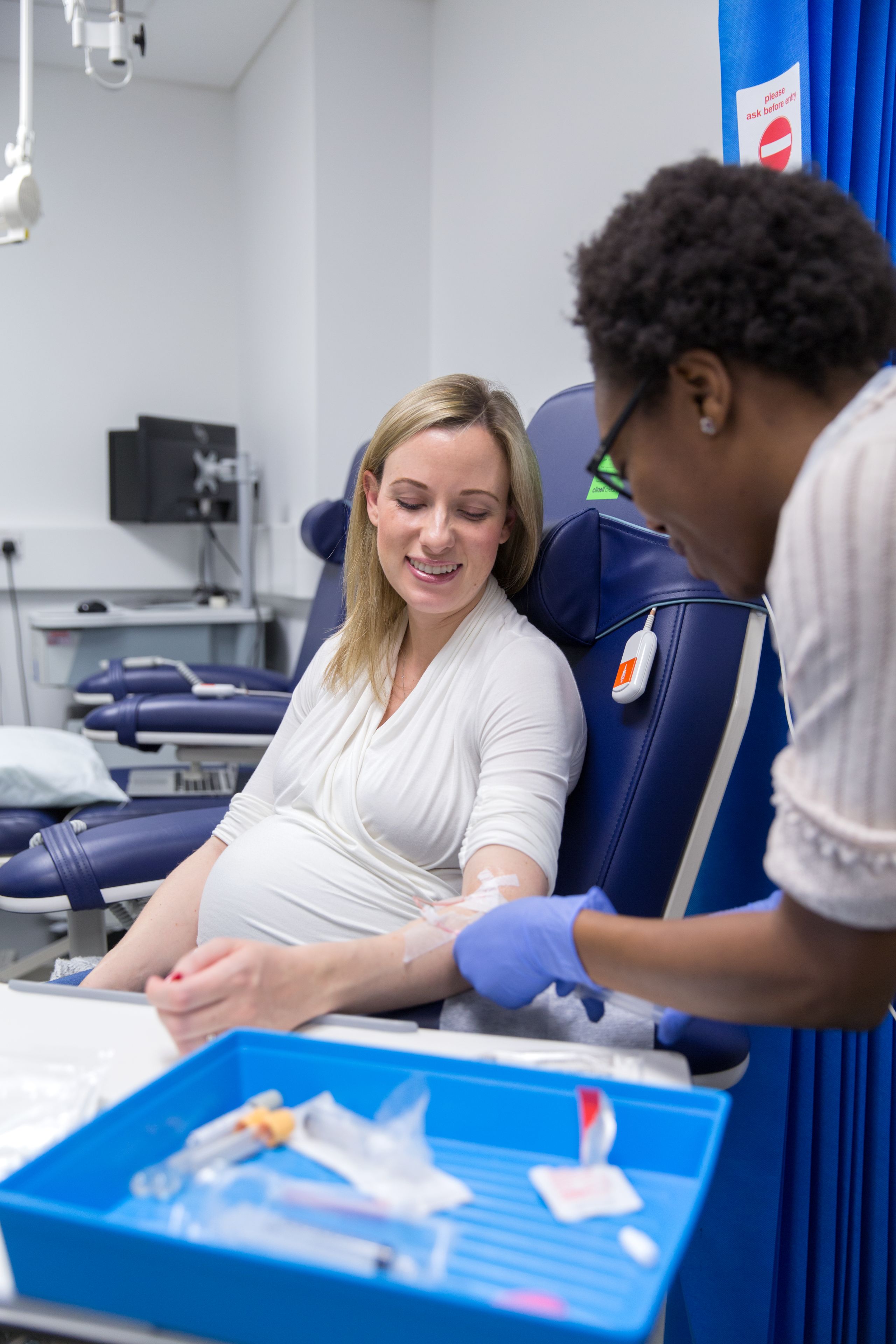
The Forum is Imperial’s policy engagement programme. It connects Imperial researchers with policymakers to discover new thinking on global challenges. Our features provide a shop window into the world leading research taking place at Imperial and provide insight into how it can inform and contribute to public policy debates.













