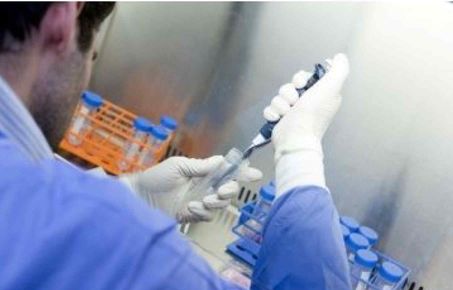
Apply now for a new PhD Opportunity with MARC
Applications for the Clinical Research Fellow (MARC Training Programme) role are now being accepted! If you are interested in joining the MARC team and contributing to the future of addictions research apply here:
Clinical Research Fellow (MARC Training Programme) job application
Closing Date: 4 August 2019
PhD Opportunities within MARC
Are you a clinician? Are you looking to undertake a PhD to build your academic career?
The MRC Addiction Research Clinical (MARC) Training programme is led by Prof Anne Lingford-Hughes at Imperial College London, with Prof Colin Drummond at King’s College London and Prof Matt Hickman at University of Bristol. The vision of the MARC programme is to develop the future UK clinical research leaders in addiction to build and sustain capacity in this vital area of clinical neuroscience and address the gap in clinical research capacity in the addictions field in the UK. MARC can support clinicians (eg psychiatrists, psychologists etc) to undertake a PhD to train in a range of research approaches and techniques to effectively translate basic and epidemiological evidence into the clinical environment using early (T1, T2) experimental medicine studies in patients for the benefit of clinical populations and their treatment.
For more information contact the MARC Team marc@imperial.ac.uk or contact the MARC leads directly Anne Lingford-Hughes (Imperial College London), Colin Drummond (King's College London) or Matthew Hickman (University of Bristol).
Imperial College Contacts
| Who | Area of Expertise | |
|---|---|---|
| Professor Anne Lingford-Hughes (MARC Lead) | Neuroimaging, pharmacology, clinical trials, experimental medicine | anne.lingford-hughes@imperial.ac.uk |
| Professor David Nutt | Pharmacology, experimental medicine, neuroimaging | d.nutt@imperial.ac.uk |
| Dr Jim Myers | PET neuroimaging methodology | j.myers@imperial.ac.uk |
| Professor David Sharp | Brain inflammation, traumatic brain injury, neuroimaging | david.sharp@imperial.ac.uk |
| Dr Henrietta Bowden-Jones | Lead clinician for National Gambling Clinic, neuropsychology | h.bowdenjones02@imperial.ac.uk |
| Dr Tony Goldstone | Endocrinology, appetite and eating behaviours, cognitive assessment, neuroimaging | tony.goldstone@imperial.ac.uk |
King's College Contacts
| Who | Area of Expertise | |
|---|---|---|
| Professor Colin Drummond (MARC Lead) | Alcohol clinical and experimental research | colin.drummond@kcl.ac.uk |
| Professor John Strang | Drugs clinical and experimental research | John.Strang@kcl.ac.uk |
| Professor Gunter Schumann | Addiction biology, genetics, brain mechanisms of addiction | gunter.schumann@kcl.ac.uk |
| Professor John Marsden | Psychology of Addiction, experimental studies, clinical trials | john.marsden@kcl.ac.uk |
| Professor Michael Lynskey | Genetic and environmental influences on addiction, twin studies | michael.lynskey@kcl.ac.uk |
| Professor Ann McNeil | Tobacco addiction, psychology of addiction, tobacco control policy | ann.mcneill@kcl.ac.uk |
| Dr Paolo Deluca | Novel psychoactive substances, e-health interventions, prescription drug dependence | Paolo.Deluca@kcl.ac.uk |
University of Bristol Contacts
| Who | Area of Expertise | |
|---|---|---|
| Professor Matt Hickman (MARC Lead) | Public health and addiction epidemiology | matthew.hickman@bristol.ac.uk |
| Professor Marcus Munafo | Experimental Psychology, genetics of alcohol and tobacco. | Marcus.Munafo@bristol.ac.uk |
| Professor Stan Zammit | Clinical Epidemiology and genetic epidemiology of psychiatric disorders | Stan.Zammit@bristol.ac.uk |
| Dr Tim Williams | Addiction psychiatry and psychopharmacology | Tim.Williams@bristol.ac.uk |
| Professor Graeme Henderson | Heroin addiction, opioid tolerance, psychopharmacology | Graeme.Henderson@bristol.ac.uk |
| Dr Emma Robinson | Psychopharmacology | Emma.S.J.Robinson@bristol.ac.uk |
| Professor Caroline Relton | Genetic & Epigenetic Epidemiology | Caroline.Relton@bristol.ac.uk |
| Professor Kate Tilling | Medical Statistics, Causal Modelling, Longitudinal Modelling incl epigenetic data | Kate.Tilling@bristol.ac.uk |
| Professor John Macleod | Primary care and addiction epidemiology, record linkage | John.MacLeod@bristol.ac.uk |
Other opportunities
Partner consortia
Contact us
5th Floor, Burlington Danes Building
Department of Medicine
Imperial College London
Hammersmith Campus
Du Cane Road
London W12 0NN
Administrator - April Haesler
marc@imperial.ac.uk
+44 (0)20 3313 8282