Our year, our progress
IGHI Annual Report 2022

A message from our Co-Directors at the Institute of Global Health Innovation.
The Institute of Global Health Innovation (IGHI) tackles the healthcare challenges of the present and the future. In 2022, our clinicians, scientists, designers, engineers, policy makers, developers, patient and public involvement specialists and more have been improving patient safety, reimagining healthcare design, educating future leaders, optimising medical innovations and championing healthcare for all.
2022 was a year of transition. COVID-19 ceased to be the dominant focus in healthcare. We concluded the REACT study into community prevalence and had the final report of the COVID-19 behavioural tracker, which had looked at public opinion on issues such as vaccinations and lockdowns.
New themes took their place including developing our programme of work on antimicrobial resistance, the mental health impacts of climate change and work on ensuring AI in health is used equitably and fairly. These will grow in prominence in 2023 and beyond.
As the themes of our work changed, so did how we worked. It was possible to collaborate more in person in 2022 with workshops and events. At the same time, we are now much more used to online collaboration and will continue to do this to work effectively with partners across the globe. Within this digital report, you will find examples of how we have done this and continue to transform health for all through evidence-based innovation.
Professor the Lord Ara Darzi
Professor Sir David Nabarro
Co-Directors, Institute of Global Health Innovation
Professor Sir David Nabarro, Professor the Lord Ara Darzi
Professor Sir David Nabarro, Professor the Lord Ara Darzi
Celebrating milestones

In 2022 we celebrated 12 years of solving healthcare problems.
Professor the Lord Ara Darzi, Co-Director, Institute of Global Health Innovation, said: “IGHI has always sought to identify opportunities before they become obvious to others. That is why we were the first research organisation to focus on patient safety. The first to focus on the fusion of engineering and surgery. The first to realise the potential of design in healthcare, and the first to introduce qualifications for policy makers.”
Our Themes
IGHI works in the following themes:

Prevention and early detection
COVID-19 Behaviour Tracker
The COVID-19 Behaviour Tracker is a global survey launched in partnership with YouGov which ran from April 2020 through March 2022. The survey explored compliance with physical distancing measures, life satisfaction, and trust in the government and health authorities, as well as attitudes towards COVID-19 vaccines. Its aim was to enable individuals, organisations, systems and governments to use the learning and insights gleaned in ongoing efforts against the COVID-19 pandemic, and in future health threats as they arise.
Our report reviews the full 2 years of survey results. This includes over 450,000 people across the 9 countries that have been a part of the survey. The reports notes change in trust and vaccine hesitancy across geographies and timelines of the pandemic.
Sarah Jones, Research Fellow at IGHI, said: “This programme brought together behavioural scientists, health researchers, data analysts, governments and policy experts to form a truly unique global dataset."
Research snapshot: Clinical Research Fellow
Joe Zhang is a Wellcome-funded PhD student at the Institute of Global Health Innovation.
My PhD is about overcoming data-related barriers to implementing AI for population health, looking across the spectrum of policy, infrastructure, data quality and bias, and 'Machine Learning Operations'.”
Joe is an intensive care specialist doctor alongside his fellowship at the IGHI and holds additional roles with commissioning organisations in London to lead clinical AI implementation. Through optimising how we use clinical data, his research can scale up AI usage for numerous risk prediction or demand forecasting use-cases. He is currently leading CHARM, an international study for designing some of these processes.
“We traditionally develop AI on curated datasets. However, deployment in the real-world requires different infrastructure, and attention paid to quality and bias in the data. Continuous processes and monitoring are needed to make sure AI is safe and effective.”
Joe is happy to be collaborating with the North East London Integrated Care Board, and his supervisors Professor Ara Darzi, Professor Brendan Delaney and Dr Hutan Ashrafian at Imperial are looking forwards to seeing the applications of his work.
Notable moment: Moderna lecture
In 2022, Imperial hosted Dr Noubar Afeyan, CEO of Flagship Pioneering and chairman of Moderna for a talk on innovation.
Dr Afeyan spoke of the need to break away from the traditional model of innovation. The talk focused on Moderna’s path to creating the mRNA vaccine for COVID-19, Flagship Pioneering’s unique approach to innovation and Dr Afeyan’s own reflections on the future of biotech.
Big Data and Analytical Unit
The Big Data and Analytical Unit (BDAU), housed within the Centre for Health Policy of the IGHI, provides a certified research environment to researchers working with sensitive patient data. Over years, the BDAU Secure Environment (SE) has been a vital tool enabling researchers to securely and efficiently store and analyse the data, in compliance with data regulations such as GDPR. We are proud of the role we play in important research that benefits the public by improving healthcare and potentially saving lives.
In 2022, BDAU supported a total of 87 users, including 21 users from IGHI and 66 users from other departments from across the College such as the Department of Primary Care and Public Health, Surgery and Cancer and Business School. We also facilitated 150 research projects that used data from more than 40 different data sources.
|
87 |
150 |
41 |
|
BDAU Secure Environment Users |
BDAU Secure Environment Datasets |
Data Providers/Sources |
Healthcare delivery

Brain Stimulation Project
The Helix Centre worked with the UK Dementia Research Institute to understand how best to develop an innovative new brain stimulation technology, which hopes to improve cognition in Alzheimer’s. Sophie Horrocks, Designer at Helix Centre, works to bring people with lived experience into the development process. At a workshop, attendees who either lived with dementia or cared for someone with dementia, shared their experiences to co-produce a design that could be used at home.
The Helix Centre has received renewed funding from the UK Dementia Research Institute of £800,000.
Global GP survey - virtual care
Data from over 1,600 primary care doctors across 20 countries, collected between June and September 2020, highlighted that while delivering care digitally brought a range of positive outcomes including lowering the risk of COVID-19 transmission and ensuring continuity of care during the pandemic, GPs also cited a number of concerns. The study was the first of its kind to explore GPs’ perceptions of virtual consultations, offering unique insight into how the pandemic-driven shift towards digital care has impacted patient and healthcare provider experience.
Learning from the experiences of GPs worldwide is imperative to shaping policies concerning these novel technologies and improving their use in our ever-changing healthcare environment."
Hamlyn Symposium
The annual Hamlyn Symposium on medical robotics is a world-leading conference, and one of its kind in bringing together engineers, industry, and clinicians. In 2022, the event focused on the theme of 'MedTech Reimagined'.
Programme highlights included a keynote by Professor Alexandra Golby, on optimizing surgery for patients with brain tumours, which requires a balance of aggressive oncologic therapy with preservation of neurological function. The Industry Forum focused on industrial orthopaedic robotics, a field that is becoming more mainstream thanks to recent technological developments, strategic mergers and acquisitions, and growing acceptance within the patient and clinical community.
The conference plays a key role in advancing medical robotics. The 2022 Funders Forum followed up on the “Recommendation H: SUPPORT” in the UK-RAS-sponsored White Paper on Surgical Robotics. This recommendation encourages funding agencies to explore joint funding schemes to facilitate further international collaborations in surgical robotics.
Health Secretary visit to Hamlyn Centre
The Health Secretary Steve Barclay MP visited the Hamlyn Centre at Imperial in July 2022 to see the future of surgery through the leading work of Imperial researchers in medical robotics and imaging - a key focus of the government Life Sciences Vision published in 2021.
He learnt about their work on technological innovation and clinical adoption of robotic, minimally invasive surgery - often done in partnership with major industrial leaders in medical devices and surgical robots.
Steve Barclay MP viewing imaging research at the Hamlyn Centre
Steve Barclay MP viewing imaging research at the Hamlyn Centre
Hamlyn Centre – research highlights
EDEN2020 focused on developing a bio-inspired, steerable catheter for use in diagnosing and treating diseases in the brain. This soft and flexible instrument can be used to navigate along complex paths while avoiding damaging brain tissue.
Professor Ferdinando Rodriguez y Baena, Director of the Mechatronics in Medicine Lab and Co-Director of the Hamlyn Centre said: "Our new precise, minimally invasive platform improves on currently available technology and could enhance our ability to safely and effectively diagnose and treat diseases in people, if proven to be safe and effective."
Dr Vyas of Imperial’s Department of Electrical and Electronic Engineering and Hamlyn Centre said: "A key focus of this EPSRC-funded work has been the development of hardware and accompanying tissue staining and classification protocols enabling the new system to generate diagnostic relevant tissue images at 120 frames per second – a huge leap forward in terms of image acquisition."
This research aims to transform early diagnosis and treatment of gut cancers using flexible endoscopy. It combines a soft robotic endoscope with a probe carrying a miniature surgical laser, and a powerful tissue analysis device. The device will be easier to use than standard endoscopes and will allow endoscopists with less experience to perform surgeries.
The MedTechONE framework (funded by the Wellcome Trust) will establish an infrastructure to accelerate the translation of research technologies for musculoskeletal health and surgical innovation across robotics, sensing and imaging, by supporting early career researchers, through mentoring, targeted training, funding, and access to local and national clinical networks.
The Multi-Scale Medical Robotics Centre (MRC) – Reshaping the Future of Medical Diagnosis and Treatment with Robotic Technologies, focusses on the development of technologies that enhance visual access and accuracy during minimally invasive surgeries through three research programmes:
- Endoluminal multi-scale robotic platforms for diagnostics and therapeutics,
- Magnetic-guided endoluminal robotics, and
- Image-based automation in robotic surgery.
Indonesia Ministry of Health visit
In July 2022, IGHI hosted a delegation from the Ministry of Health Indonesia’s Digital Transformation Office as part of their trip to the UK to learn about how the UK health sector designs and implements digital technology.
Children's palliative care
Families of children living with life-limiting conditions are the most incredible problem solvers.
Families of children living with life-limiting conditions are the most incredible problem solvers.
This policy report sets out an optimistic vision of what a world-class provider of children’s palliative care (CPC) could look like in the future. It proposes nine key features through which providers can innovate to improve access and quality over time, drawing on best practice and trends as described by 50 CPC service leaders in 27 countries, as well as insights from other healthcare sectors.
Recognising that there is huge variation among CPC providers and the systems they work in, this ‘blueprint’ is intended for inspiration and challenge, not prescription. In addition to key areas for future innovation it also highlights many areas in which CPC providers are already exemplars within the healthcare sector.
Digital Health: Future of Telemedicine
IGHI partnered with The Commonwealth Fund and the Organisation for Economic Co-operation and Development (OECD) to undertake a systematic review exploring the use of telemedicine since 2020 in OECD countries. The review focused on key areas including assessment of user satisfaction with services, the impact on patient safety, utilisation rates by demographic and socio-economic status, types of telemedicine utilised, and a cost analysis and pricing of services. Results of the review were published in "The COVID-19 Pandemic and the Future of Telemedicine" released in January 2023.
We’re excited about the potential of telemedicine to build on important progress made through the COVID-19 pandemic. With further research into quality and safety, as well as reimbursement and pricing models, we can improve services and accessibility for all patients."
Personalised Care Planning
Our Design Strategy Team worked with the Sussex Integrated Care System on two projects to support user centered digital transformation within Sussex.
Workshop to co-design methods to collect information about end-of-life care.
Workshop to co-design methods to collect information about end-of-life care.
The first project focused specifically on what information should be collected, stored and shared about people in order to deliver personalized end of life care. A series of workshops were run with members of the public and healthcare professionals in Sussex to co-design the methods and tools for collecting this information but to also transform national guidelines for ‘About Me’ data into a set of questions that could be used and understood by all.
The second project involved interviewing members of the public in order to create a set of user-centred requirements to help Sussex to procure a digital My Health and Care Record tool.
What Good Looks Like for Nursing
Our Design Strategy Team at the Helix Centre partnered with NHSX (now NHS Transformation Directorate) to develop a unified vision of digitally-enabled nursing care. With the success of the What Good Looks Like (WGLL) framework launched in 2021 and the critical role of nurses in driving digital transformation, there was the need to set a vision for digitally-enabled nursing care in the NHS. The What Good Looks Like framework, which the Helix Centre team also previously supported, is directed at all NHS leaders and establishes seven measures essential for digital transformation.
The Helix Centre worked alongside the Chief Nursing Informatics Officer (CNIO) team to co-design the Guidance for Nursing on What Good Looks Like, which aligns nursing practice with the wider WGLL framework and aims to support nurse leaders in digital transformation. Our team conducted discovery research and co-development sessions to inform, draft and iterate the guidance, working with nurse leaders from different regions and practice areas. The Helix Centre also provided a support offer following the launch of the guidance to drive its implementation. This support offer included:
- Library of ‘Snipits’ – short audio summaries of digital health information designed for nurses
- Series of learning ‘huddles’ providing peer support to digital nurses as they implement the guidance
Palliate
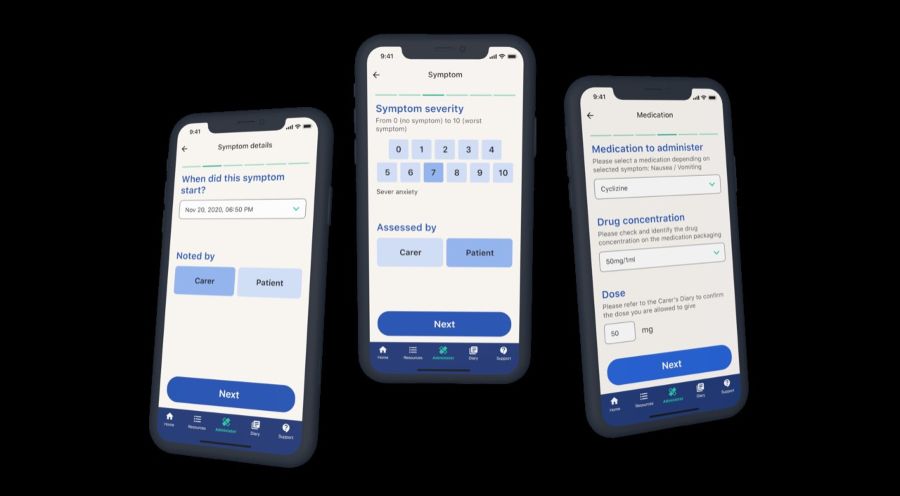
Palliate seeks to improve the access and quality of training and support for carers to administer as-needed injectable end-of-life medications in the home. Palliate provides medication administration recording and training, education modules and facilitation for lay carers to support their loved ones at home with on demand professional support. Our goal is to support patient preferences for a home death while also reducing pressure on community care teams.
Palliate includes an app that enables carers to record symptoms and prescribed medication
Palliate includes an app that enables carers to record symptoms and prescribed medication
The paper-based version has been adopted at Central and North West London (CNWL) NHS Foundation Trust. A lab-based simulation study is currently being developed to evaluate the safety, usability and acceptability of the current paper based version along with a number of updated versions, including a hybrid paper and digital version. A qualitative study exploring healthcare professionals and carers perceptions and experience of utilising the intervention will also be conducted to complement the simulation study.
OnTrack Stroke Rehabilitation
OnTrack is a digital rehabilitation system that uses a smartwatch to track arm movement and provide self-management coaching support for patients. The system encourages users to use their affected arm as much as possible during daily life activities in order to promote recovery and participation.
OnTrack smart watch
OnTrack smart watch
The system has been primarily developed for recovery after stroke but its potential applications go beyond neurorehabilitation, with recovery after breast cancer surgery being explored currently by the research team.
Since 2022 OnTrack has been funded by a technology development fund from SBRI Healthcare that aims to spread innovations with potential to improve outcomes in the NHS. During Phase 1 the team focused on refining the technology behind OnTrack – including making improvements to the Machine Learning algorithm used to detect and classify arm movement and testing a clinician-facing dashboard used to support patients in their recovery. In the current Phase 2, the team is preparing a multi-site feasibility clinical trial with 3 NHS Trusts that aims to recruit 42 stroke survivors with the objective of providing evidence for supporting a definitive trial, as well as preliminary evidence of clinical effectiveness and economic viability of the OnTrack intervention as a complement to usual care.
The work is being led by the Helix Centre at Imperial College and counts with a multidisciplinary group of academic and industry collaborators including St George's University, Cardiff University, Imperial College Health Partners and Bridges Self Management, as well as with an active lived-experience group of stroke survivors and carers.





Health equity

Networked Data Lab
In 2020 the Health Foundation launched the Networked Data Lab (NDL), a "collaborative network of analysts who use linked data, open analytics and public and patient involvement (PPI) to tackle the most pressing challenges in health and social care".
IGHI is part of the North West London lab together with Imperial College Health Partners and the North West London Integrated Care System. The NDL uses a federated approach to analytics, encouraging each of its labs from across the country to conduct one set of "central" analyses (which are the same across all labs) and one set of "satellite" analyses (which are decided based on local stakeholder priorities and informed by PPI), which are then published. The NDL then publishes key findings from the compilation of "central" analyses from across the labs, and each lab is able to publish its satellite analyses individually.
As the North West London lab, we leveraged Discover-NOW, a de-identified dataset that covers over 2.5 million people in North West London and includes linked data on primary, secondary, mental health, social care and other relevant datasets. During the first phase of the NDL (2020-2023) we used the Discover-NOW dataset to answer key questions on three key topics:
- COVID-19 and the clinically extremely vulnerable population
- Children and young people's mental health
- Understanding unpaid carers and their access to support
People with relevant experience, i.e. those who were shielding, young people and unpaid carers, were involved in coming up with questions to ask of the data and prioritising areas for research. The people involved also helped the team to make sense of the results. We did this through one-on-one phone calls, online workshops, prioritisation surveys sent to the local community and through setting up public steering groups to oversee a topic.
AI report
Our white paper highlighted the opportunities and barriers for artificial intelligence to improve the health of the UK’s minority ethnic groups. Our report, "Addressing racial and ethnic inequities in data-driven health technologies", called for further research and transparent discussion on the creation and use of these technologies in health care.
Centre for African Research and Engagement
Blood banks can save lives, but they often face shortages. This is a particular issue in Sub-Saharan Africa, where children often die waiting for a transfusion.
The ‘Transfusion and treatment of severe anaemia in African children’ (TRACT) trial began in 2013. By 2019, the study had shown that giving larger volumes of blood transfusions than current WHO guidelines could halve the number of deaths.
More recently, the study has revealed that children who received ‘packed blood cells’ – a more costly, processed form of blood – recovered more slowly than those who received cheaper whole-blood transfusions.
Photo by 愚木混株 cdd20 on Unsplash
Photo by 愚木混株 cdd20 on Unsplash
Photo by 愚木混株 cdd20 on Unsplash
Photo by 愚木混株 cdd20 on Unsplash
Photo by 愚木混株 cdd20 on Unsplash
Photo by 愚木混株 cdd20 on Unsplash
Safety and quality

National State of Patient Safety 2022
Keeping patients safe during their care and treatment should be at the heart of every health system. The report, “National State of Patient Safety 2022: What we know about avoidable harm in England”, produced by the NIHR Imperial Patient Safety and Translational Research Centre and Centre for Health Policy at the Institute of Global Health Innovation (IGHI) and funded by the charity Patient Safety Watch, explores progress and identifies areas for improvement in patient safety nationally, based on analysis of publicly available data over the past 15 years.
The data showed some warning signs in the pressures faced by the healthcare workforce, exacerbated by the COVID-19 pandemic, alongside issues with access to care such as increased waiting lists and regional variations in care. Key recommendations of the report included expanding the breadth of patient safety data, improving the accuracy of key patient safety measures, the need for a workforce plan across the NHS and social care, the key role of Integrated Care Systems in monitoring safety, and the need to accelerate progress in the safety of maternity services.
The launch of the report was recognised during a patient safety reception held at 11 Downing Street, in December 2022.
Global Patient Safety Collaborative
The Institute of Global Health Innovation has worked with WHO as academic partner within the frames of the Global Patient Safety Collaborative (GPSC) since 2019.
The GPSC is a strategic initiative to secure and scale up global action on patient safety, working in the key areas of leadership, education and training, and research.
We have supported the development of the ‘Patient Safety Fundamentals’ module of the WHO Patient Safety Curriculum Guide, developed a study to identify the global priorities for patient safety research, and contributed to expert consultations on patient safety in COVID-19 and the implementation of the Global Patient Safety Action Plan.
We have also organised and run a webinar series on a range of topics including reporting and learning systems, medication safety, research for patient safety, patient and family engagement, and safety culture alongside speakers and colleagues from a range of countries including Sri Lanka, Singapore, Canada, India, Pakistan, and Uganda, amongst others.
Renewed funding for PSRC
The National Institute for Health and Care Research (NIHR) announced that researchers at the NIHR Imperial Patient Safety Translational Research Centre (PSTRC) have received renewed funding, to become the NIHR North West London Patient Safety Research Collaboration (NWL PSRC), hosted by Imperial College Healthcare NHS Trust.
We are delighted to have our funding renewed, alongside additional centres being funded, and look forward to the extra opportunities for collaboration that this brings."
World Patient Safety Day
World Patient Safety Day 2022 focused on Medication Safety and for the IGHI event we were joined by keynote speakers including an introduction from Professor the Lord Ara Darzi and the Chancellor, the Rt. Honourable Jeremy Hunt MP, who delivered a closing keynote address surrounding his thoughts on the extent of medication errors as well as the upcoming developments for patient safety. Following an introduction to the challenges of medication safety from Professor Bryony Dean Franklin, we heard from patient partners and their experiences of participating in research, about the WHO Global Challenge ‘Medication without Harm’, and Mongolia’s experience of implementing safety interventions.
In 2022, the theme of World Patient Safety Day was Medication Safety: Medication Without Harm
Unsafe medication practices and medication errors are a leading cause of avoidable harm.
Medication is the most common healthcare intervention - nearly every hospital patient is prescribed at least one medication.
Patients and carers bring different experiential knowledge to researchers and practitioners.
Medication safety measures can be implemented at both national and organisational levels.
What action can be taken? Collect better data, increase electronic prescriptions, improve staffing levels.
Change Lab
The Change Lab is a collaboration between the IGHI, the NHS (Imperial College NHS Healthcare Trust – ICHT) and the Behavioural Insights Team (a behaviour change consultancy – BIT) who work together to apply knowledge from behavioural science to help us understand human behaviour and how user-centred design can help support healthy decision making.
Change Lab projects included:
Increasing COVID-19 Vaccination Uptake through Behavioural Insights Informed Letters. We demonstrated a significant increase in COVID-19 vaccination uptake. An abstract of this work was published in the Lancet and presented at the UK Public Health Science Conference in Glasgow.
Improving the use of Barcode Medication Administration technology at Charing Cross Hospital. A 22% increase of usage of the technology was achieved through a feedback intervention, co-designed with frontline staff. This work has been submitted for publication and presented at the UCL Centre for Behaviour Change Conference.
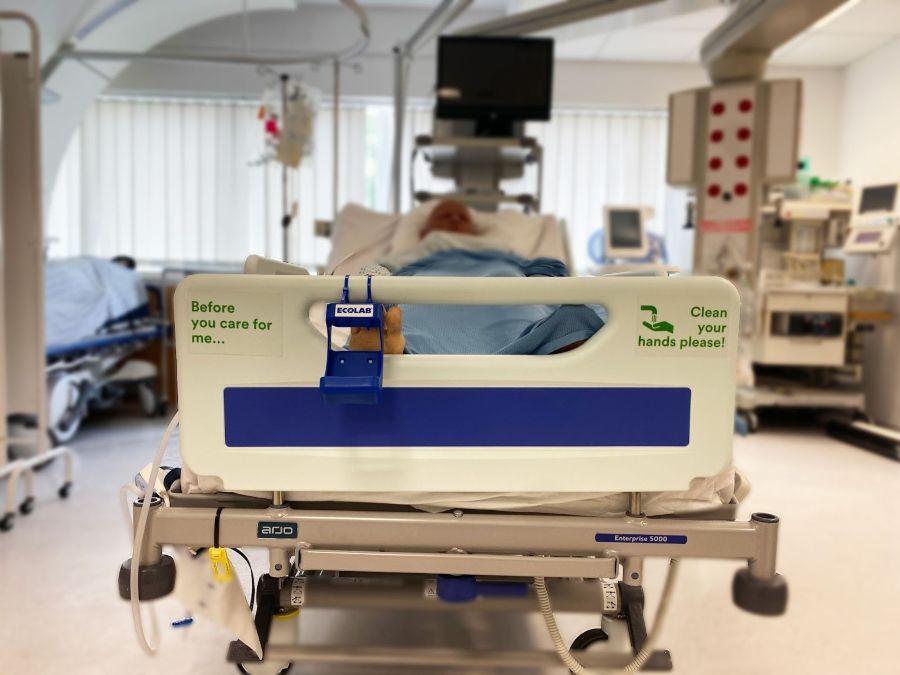
Working to improve hand hygiene behaviour and practices in line with WHO’s 5 moments of hand hygiene at Imperial College NHS Healthcare Trust, leading to the co-design of behavioural science informed nudges currently in place on 3 target wards.
A hospital bed with hand hygiene reminders
A hospital bed with hand hygiene reminders
Minder App
Our role in the Care Research & Technology Centre (CR&T) is to ensure that the participants in the study, and all future users of the technology have a strong voice in the way technologies are developed, so as to fit their needs and aspirations, and to use design techniques to ensure productive and rewarding relationships between the participants, researchers and clinicians.
In the last year we have been working towards making The Minder smart home platform fit for scaling up and for use by third parties, including preparing it as a UK Conformity Assessed marked medical device for use in the NHS.
Consultation for development for Minder App
Consultation for development for Minder App
Emerging global challenges

COP 27
The Climate Cares team, led by Dr Emma Lawrance from the Institute for Global Health Innovation (IGHI), were at COP27 in Egypt to launch COP squared (COP2). This new global network of organisations focuses on how to strengthen people's emotional and mental ability to endure and adapt to the trauma, vulnerability and change caused by our warming planet.
Climate Cares’ Dr Lawrance (first row, right) and Jessica Newberry Le Vay (back row, second from right) and colleagues from COP2 at their event in Egypt
Climate Cares’ Dr Lawrance (first row, right) and Jessica Newberry Le Vay (back row, second from right) and colleagues from COP2 at their event in Egypt
Climate Cares is leading the European Hub of COP2, which will collaborate with the World Health Organisation and the UN’s Race to Resilience, among others. It will work to develop tangible policies and actions that decision-makers can take to support mental wellbeing, as the impacts of climate change become more severe.
This network was founded following a recommendation for collaboration between climate change, mental health and emotional wellbeing experts in a briefing by the Grantham Institute and IGHI.
Even in the height of the COVID-19 pandemic in the UK, young people were at least as concerned about the climate crisis.
"Our study emphasises the importance of leaders taking urgent action on the climate emergency, and doing so in a way that meaningfully listens to the concerns and desires of young people.
"Climate education and mental health support, for example, must help young people cope with the compounding stressors they face while enabling appropriate opportunities for action."
Watch the film 'Nexus: The power of connections'
Nexus premiere at BFI
Nexus is a short film about the impact of COVID-19 on young people’s mental health, eating-related coping strategies, and the power of social connection. The film was co-produced with young people, and made from a collaboration between West London NHS Trust, Inner Eye Productions and Imperial College London, with thanks to funding from The Burdett Trust for Nursing. It premiered on 7 December at the British Film Institute (BFI) in London.
It is important that we not only empower patients and public members to get involved in research, but to also feel comfortable enough to do so ourselves.
"Co-production in mental health research has allowed young people to get involved in scientific research in creative, innovative and engaging ways, and build networks.
"These activities can help support their confidence, develop their skills and to invoke their authenticity to the work. Providing a voice for those who the research is about and a space for them to flourish is what it’s all about!"
REACT study
Data from the REal-time Assessment of Community Transmission (REACT-1) programme, led by Imperial College London with Ipsos MORI and commissioned by the Department of Health and Social Care, continued to inform Government decision-making.
I’d like to thank each and every REACT participant for contributing to what has been a vital study throughout the course of the pandemic in giving us insight into how COVID-19 has impacted the country."
Educating future leaders
Cutting across our themes of work are our education and training programmes

Digital Maternity Leaders programme launched September 2022
In 2022, our first cohort of 35 digital maternity leaders started the postgraduate certificate with a full-day leadership development and networking day at Imperial College London.
Our post-graduate certificate programme empowers maternity staff with digital leadership and healthcare transformation knowledge, skills and behaviours.
"We are very proud to be working with NHS England to develop a new generation of digital changemakers who will drive information and technology transformation in maternity services.”
Digital Maternity Leaders
Digital Maternity Leaders
Julia Anderson Training Programme
The Julia Anderson Training Programme is a scheme at IGHI that offers paid work experience to people who have no, or limited, prior work experience. In 2022 we welcomed our second cohort.

Sophie Pieters,
Operations Officer at IGHI
I lead on the Julia Anderson Training programme - It has been the most rewarding work I have ever done, and I feel like I’m making a difference to our trainees’ lives."
Big Data Analytics Unit Trainee
It is a great opportunity to gain a variety of skills and expand your network in a professional work setting, which is structured to support your development."
The Julia Anderson Training Programme: Supporting early career development in loving memory of Julia Anderson

Paula Bradley,
Digital Health Trainee
I have enjoyed feeling like a valuable member of the team and playing my part in all the projects I have worked on. The programme has grown my confidence."
Hamlyn Winter School on Surgical Imaging and Vision
The annual Hamlyn Winter School on Surgical Imaging and Vision is a week-long course focusing on both the technical and clinical aspects of surgical imaging and vision. Through invited lectures, workshops, and mini projects, this event helps researchers familiarise with the innovative research of this rapidly expanding field, which is empowering surgeons to "see," analyse, and treat conditions more accurately and efficiently through new sensing modalities that can be integrated into robotic instruments.
In 2022, the event was attended by 32 delegates, and included a range of speakers from academia, the NHS, and industry, including Intel Corporation and Google Zurich.
Cohort 5 of Digital Health Leadership Programme
The PGDip Digital Health Leadership Programme (DHLP) turned five in 2022, with a broader curriculum to attract diverse talent from across health and care professions. Complementing the largely online delivery, the Leadership Forums increase the emphasis on self-awareness and leadership development for participants to solidify their leadership styles and strategies, and provide opportunities to consider equality, diversity and inclusion.
Commissioned by Health Education England in partnership with NHS England, the DHLP is delivered by a partnership of Imperial College London’s Institute of Global Health Innovation, HDR UK and Imperial College Healthcare NHS Trust.
Undertaking the Digital Healthcare Leadership programme has been quite a transformative experience. As an NHS Chief Information Officer, the relevance of the course content to my role has been profound, equipping me with advanced knowledge and skills that have directly enhanced my effectiveness.
"I have found the programme not just to be about understanding digital healthcare in a broader sense; I also feel it's about cultivating leaders capable of driving change and innovation in a complex healthcare environment. I feel privileged to be part of this digital healthcare leadership journey and would certainly recommend it to current and future leaders."
At IGHI in the academic year 22-23, there were 447 postgraduate students excluding PhD students/Clinical Research Fellows.
Education Programmes
|
Programme |
Number of students (Academic year 2022-2023) |
|---|---|
|
MSc & PGDip in Digital Health Leadership |
123 |
|
PGCert in Digital Health Leadership for Maternity Leaders |
30 |
|
Foundation in Digital Health Leadership for Maternity Leaders |
73 |
|
MSc in Healthcare and Design |
26 |
|
MSc & PGDip in Health Policy |
140 |
|
MRes in Medical Robotics and Image Guided Interventions |
26 |
|
MSc & PGDip in Patient Safety |
29 |
Undertaking the Health Policy PGDip has been the highlight of my time on the NHS’s Graduate Management Training Scheme. The practical and theoretical insight it provides has allowed me to develop a robust and multi-faceted understanding of health and social care systems, and this learning has left me feeling fully equipped to tackle future policy challenges in my career.
"I couldn’t imagine a better way to kickstart my career in health policy, and I look forward to building on its teachings."
The Design Dash was fantastic. The organisation, the management, even all the administrative side of things was fantastic, super smooth flowing… I feel like the Helix team provided so much for us. I really appreciated that they brought in expert patients for bowel screening."
Look ahead

Building on our work of 2022, in 2023 IGHI will focus on our themes:
- Prevention and early detection
- Healthcare delivery
- Health equity
- Safety and quality of care
- Emerging global challenges – including food security, climate change and mental health, and antimicrobial resistance
We look forward to reporting on 2023 in spring of 2024.
Thanks
It is the people of IGHI who allow us to solve healthcare problems – who work collaboratively across disciplines, who come up with new ideas, who engage patients and the public to shape our research, and who keep us running. With thanks to everyone at IGHI.