Transforming community health in north-west London

"The biggest health threats in the UK today are the long-term health conditions that are effectively lifelong and incurable," says Professor Azeem Majeed, Head of the Department of Primary Care and Public Health at Imperial College London. "The challenge now is about managing these conditions – and often, we’ve got the evidence of what works to help manage them, but there’s a long delay in getting that evidence put into practice."
Professor Majeed is a senior investigator for the National Institute of Health Research (NIHR) and heads up the NIHR Applied Research Collaboration (ARC) Northwest London. This is a five-year research partnership hosted by the College and Chelsea and Westminster Hospital NHS Foundation Trust working in one of the most diverse areas of the UK, both in terms of ethnicity and of income.
ARC's work covers all NHS Trusts, Clinical Commissioning Groups (CCGs), Acute, Community and Mental Health Trusts, GP Practices and Social Care in north-west London (NWL).
"We’re working with local partners from across the spectrum to try to improve quality of patient care and address inequalities between different patient groups,” he explains. “Our role is very much supplying the initial data, the evidence-base for the interventions, and then evaluating the results."
The programme has already made some significant impacts on local communities, from protecting people at risk of diabetes to addressing vaccine hesitancy – and it has also adjusted to circumstances and demands which were of course unimaginable at the time when it was set up.

One of the main datasets informing the ARC is the Whole Systems Integrated Care (WSIC) Programme, which contains data from 2.4 million people across primary care, acute, mental health, community and – unusually – adult social care. This generates an ‘integrated care record’ available to health and social care professionals. "This makes patient care safer, quicker and potentially more effective," explains Paul Aylin, Professor of Epidemiology and Public Health; and importantly, it has been done with a great deal of consultation, including with patients. "Every single GP practice across north-west London has signed up to this. It’s taken a lot of work but it’s been done absolutely in the right way, consulting across everyone across the NHS in the area."
Professor Paul Aylin, Professor of Epidemiology and Public Health at Imperial College London
Professor Paul Aylin, Professor of Epidemiology and Public Health at Imperial College London
"Access to health data, from patients, can save lives," Aylin says very firmly. "This isn’t collecting data for data’s sake; it is collecting patient data to improve patient outcomes and ultimately to save lives."
For instance, the information has made it possible to start assessing which older people are likely to require social care in future. "One of the few positive things to come out of the COVID-19 pandemic is the recognition that the only way to manage a response is through this kind of data collection, and by linking it within an integrated care system like the WSIC one," Professor Aylin adds.
Access to health data, from patients, can save lives.
The integration works both ways too. Dr Céire Costelloe is a medical statistician at Imperial whose team is looking at electronic patient records. "Because we work with quality improvement teams and patients themselves, we now hear the stories behind the information we are analysing," she explains. "Before this, I had no idea how the data was generated. We often talk about how we don’t appreciate what patients go through, and indeed the tough decisions that clinicians have to make; and how some digital technology is designed because we can, and not with the end user in view. Even though we can utilise sophisticated modelling approaches, we’re very aware we need to come up with something that is usable, acceptable and makes a difference."
Dr Céire Costelloe, Reader in Digital Health, Imperial College London
Dr Céire Costelloe, Reader in Digital Health, Imperial College London
The data is also available for research, in a version that has had all the identification markers (names, addresses, dates of birth and so on) removed. This is only available through a secure NHS system, for researchers who have been specifically approved to work on projects which have also been approved.



Preventing disease
The ARC has already had an impact on reducing the rates of type 2 diabetes and of sepsis using data. This area of north-west London has one of the highest national rates of type 2 diabetes and also of people whose glucose levels mean they are getting very close to diabetes.
"We’ve been able to identify people with higher levels (about 60,000 of them) and design interventions to contact them and work with them to reduce this,” says Professor Majeed. “The system pulls data from across all the different records, which meant a very straightforward analysis to see who had been registered with higher glucose levels."
Dr Costelloe’s team has been working on sepsis. "I lead a team of mainly quantitative researchers and users, making best use of routinely collected information, almost in real time. We have access, uniquely, to linked information from GP and hospital records on vital signs, medication usage, tests and so on. From that, we can begin to build much more precise patient-specific tools. We’ve now built an electronic alert that’s triggered when a patient’s symptoms reach a certain stage. We found that implementing this alert was associated with fewer sepsis deaths at Imperial College Healthcare NHS Trust as well as less time in hospital and much quicker treatment. I’ve been a statistician for 15 years; this is the first time I’ve been involved in a project that had a direct impact on reducing patient deaths."
Dr Costelloe and her colleagues are exploring related issues, including ‘long sepsis’. "The issue of what happens when patients go back into the community is serious, and it’s under-researched. One of the things we want to do is look at all the patients alerted to the Trust, follow their journey in the community and also when they come back to the medical professionals. That level of information and data hasn’t been seen before. We can follow patients’ journeys through different parts of the healthcare system. I think that’s what so crucial about the ARC project, that it links together all those different elements and makes the data available to researchers like me and my team." And again, user involvement is a key part of their work. "We are partnering with the UK Sepsis Trust, and also have a patient representative who is a core member of our research team. She is a sepsis survivor, and has come on board since the beginning and has been really crucial in shaping the project."
I’ve been a statistician for 15 years; this is the first time I’ve been involved in a project that had a direct impact on patient deaths.
Improving child health
Professor Sonia Saxena, Professor of Primary Care at Imperial College London
Professor Sonia Saxena, Professor of Primary Care at Imperial College London
Professor Sonia Saxena, Professor of Primary Care and Director for Child Health in ARC NWL, explains how research into child population health has drawn on the ARC data and approaches to inform a very wide-ranging programme. "As a local GP, I’ve spent most of my life living and working as part of the local community in London." She says. "My mission is to understand what primary care can do for populations at an early stage, if we can get in and intervene with preventive care such as vaccinations, shaping health behaviours, and support for parenting and help adolescents with long term conditions. Here, the great opportunity for me is being able to use the information that is used in electronic health records to study cohorts from birth and tackle health problems with interventions in early life."
Within that overarching theme, Professor Saxena and her Child Health Unit team focus on the first 1,000 days, health of school-aged children; and adolescents and young people with multiple long term conditions such as asthma, epilepsy and inflammatory bowel disease. They have demonstrated that social disadvantage in early life gives rise to poor health later for example leading to persistent asthma. Some of their work draws directly on ARC information; WSIC data, for example, has informed work on the uptake of maternal and childhood vaccinations against viral infections such as influenza, and bacterial infections such as whooping cough and pneumonia. In schools, they have launched a major cohort study iMprOVE across London to evaluate the potential health benefits of initiatives like the Daily Mile, where children run or jog for 15 minutes every day in one in five primary schools in England. "The work from ARC has fed into national and international studies for example examining COVID disruption to children’s access to health care." Explains Professor Saxena.
Here, the great opportunity for me is being able to use the information that is used in electronic health records to study cohorts from birth and tackle health problems with interventions in early life.



Multiple health conditions
The research team are also using the database to analyse multimorbidity - when long-term health conditions combine. "We know for instance that heart disease often combines with obesity and diabetes, but we’re hoping to be able to use this big database of 2.4m people to see if we can identify new clusters of conditions that haven’t been recognised before," says Aylin. "We’re particularly interested in the relationship with mental health and other diseases. We know that improving mental health can improve the outcome of some physical conditions as well: that anxiety can precipitate problems with breathlessness in people with chronic lung conditions. There may be other combinations of conditions that we will be able to identify and address."
Dr Dasha Nicholls leads the ARC's Multimorbidity and Mental Health theme
Dr Dasha Nicholls leads the ARC's Multimorbidity and Mental Health theme
We know that improving mental health can improve the outcome of some physical conditions as well: that anxiety can precipitate problems with breathlessness in people with chronic lung conditions.
Dr Dasha Nicholls, Clinical Reader in Child and Adolescent Psychiatry at Imperial, is leading the multimorbidity and mental health theme.
“Our remit is very much about assessing the impact of multimorbidity on the health burden of north-west London, and within that working out what are the things we can do as an ARC to improve the quality of care for everyone with multimorbidity. A particular area of interest for us is the interface between long term physical health conditions and mental health. For example, we are using WSIC data to look at indicators of quality care for people with multimorbidity, and our PhD student is exploring the impact of depression on health care utilisation in people with multimorbidity,” says Dr Nicholls.
She and her colleagues are working across various age groups and cohorts, including a big project with children and young people presenting at the Emergency Department at Chelsea and Westminster Hospital, looking at the overlap between physical and mental health problems. “The team has been invited to evaluate the new ‘Best for you’ model of care for children and young people presenting to the emergency department with mental health problems who also have medical needs, for example malnutrition secondary to eating disorders, or self-poisoning. The programme has three core elements. There is a digital hub, which is a set of bespoke digital tools that young people can be signposted to from the emergency department if they present, for example, with self-harm. There’s a rapid assessment adolescent unit with a 72-hour turnover, during which time they’re assessed and given a discharge plan developed by a team that’s been specially trained in both physical and mental health care. For those people who need ongoing care at quite an intensive level, there will be a day programme which we anticipate will be quite heavily focused on eating disorders," she says.
“It is intended for young people who need integrated physical and mental health care, and specifically aims to prepare families for how to support young people out of hospital. We anticipate most of them will have come through the emergency services but there may well be others who’re already using the hospital’s services who may find, for instance, that the day service is extremely valuable. The idea is that the team is dual-trained, and has the skills and competence to know who needs what. We hope this model might be taken up by other providers if it’s effective.”
The team has been invited to evaluate the new ‘Best for you’ model of care for children and young people presenting to the emergency department with mental health problems.
Coping with COVID-19
"We started in 2019, so of course we’ve added in a huge amount of work on COVID-19, which wasn’t in our original protocol," says Professor Majeed. The multimorbidity and mental health theme, for instance, has been looking at the mental health of frontline workers and the effectiveness of potential interventions to support them.
The datasets are proving invaluable here, in several different ways. "We’ve been able to look at local infection rates in order to predict the need for hospital beds a week or so in advance, which helps hospitals plan ahead," Professor Aylin says.
Even having a few days’ heads-up allows intensive care and acute beds to have some handle on the number of COVID patients they’re likely to be seeing, which means they also have an estimate of their capacity for non-COVID patients. This has important implications for other infectious disease such as flu in the future, too.
We’ve been able to look at local infection rates in order to predict the need for hospital beds a week or so in advance, which helps hospitals plan ahead
They’ve also combined this with work on vaccinations. The anonymised dataset allows other colleagues and practitioners to look geographically, by area and ethnicity and a whole range of other factors, to identify where a particularly intensive vaccination drive is required. "We’ve also been able to use the anonymised research dataset to look at efficacy of the vaccine, from first dose on," Professor Aylin adds. And in addition, they’re looking at patients who have had COVID to see if they have any longer-term health issues. "We’ve looked, for instance, at whether these people need more primary care, and if they have a different hospital readmission rate compared to people who’ve had flu. And we’ve been able to see if there are new patterns of people reporting mental health symptoms."
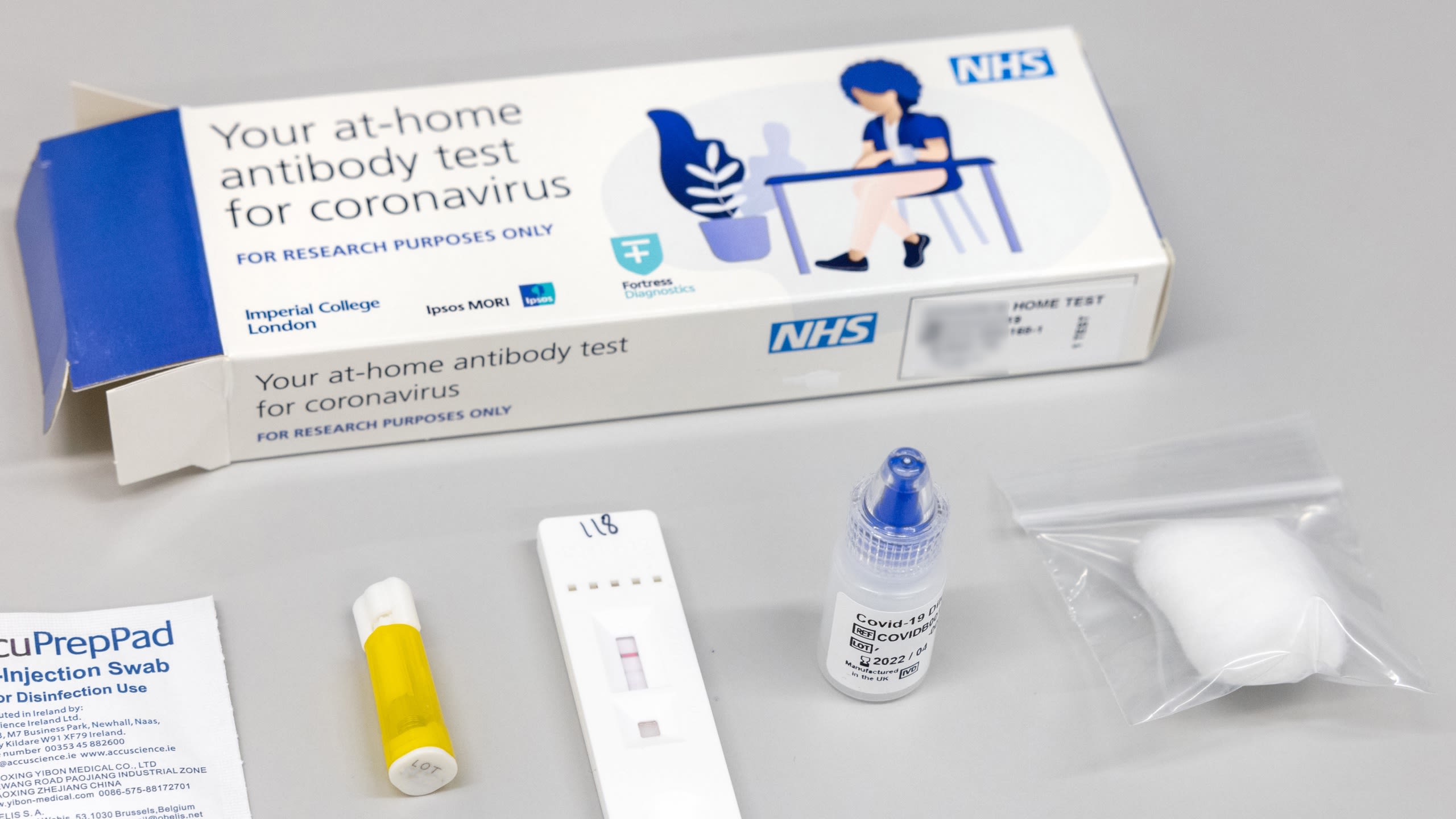
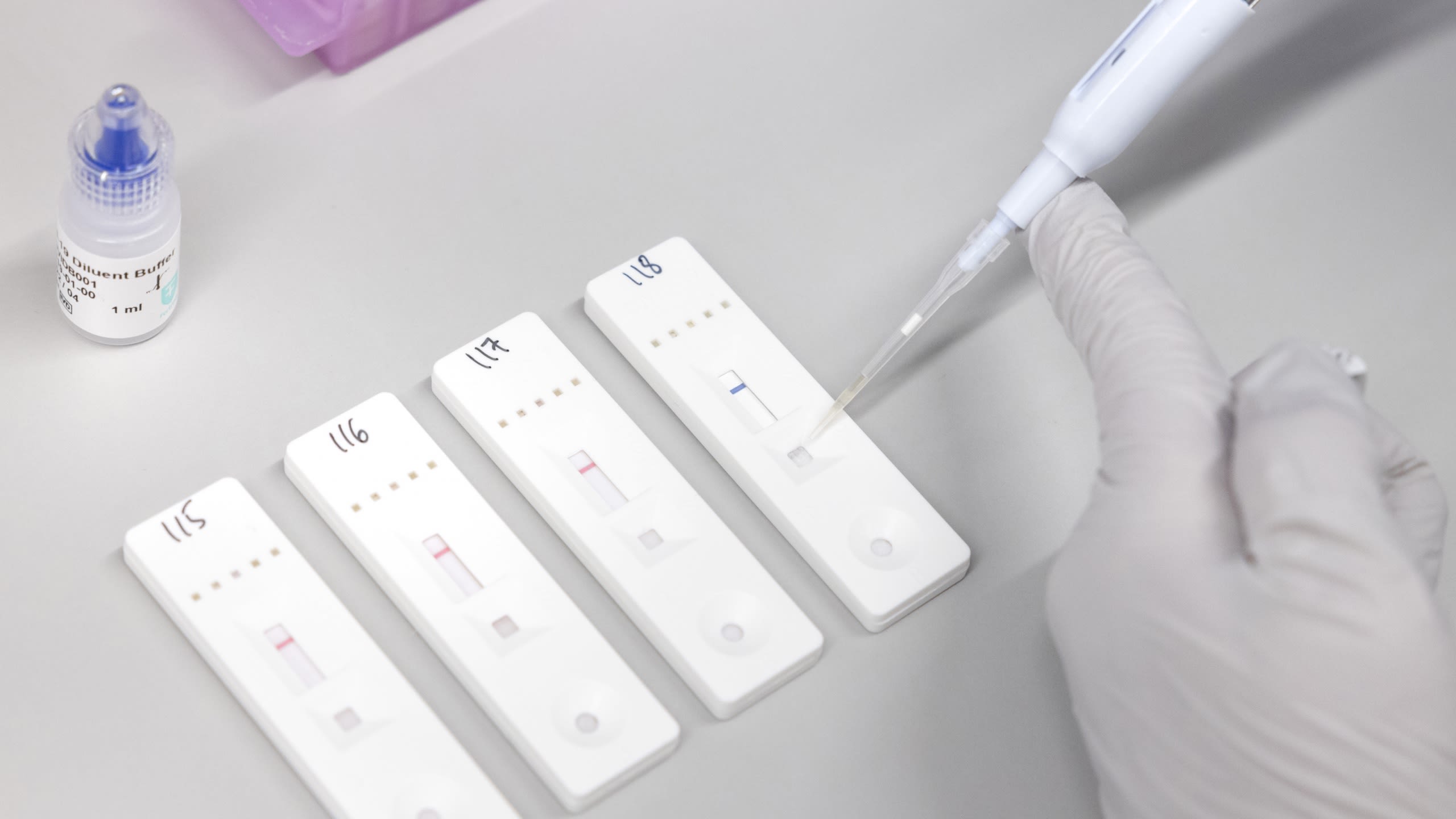
Professor Helen Ward is ARC NWL Theme Lead for the Patient, Public and Community engagement and Involvement Theme. She is working on the programme of home testing for COVID-19 known as the REACT.
Professor Helen Ward is ARC NWL Theme Lead for the Patient, Public and Community engagement and Involvement Theme. She is working on the programme of home testing for COVID-19 known as the REACT.
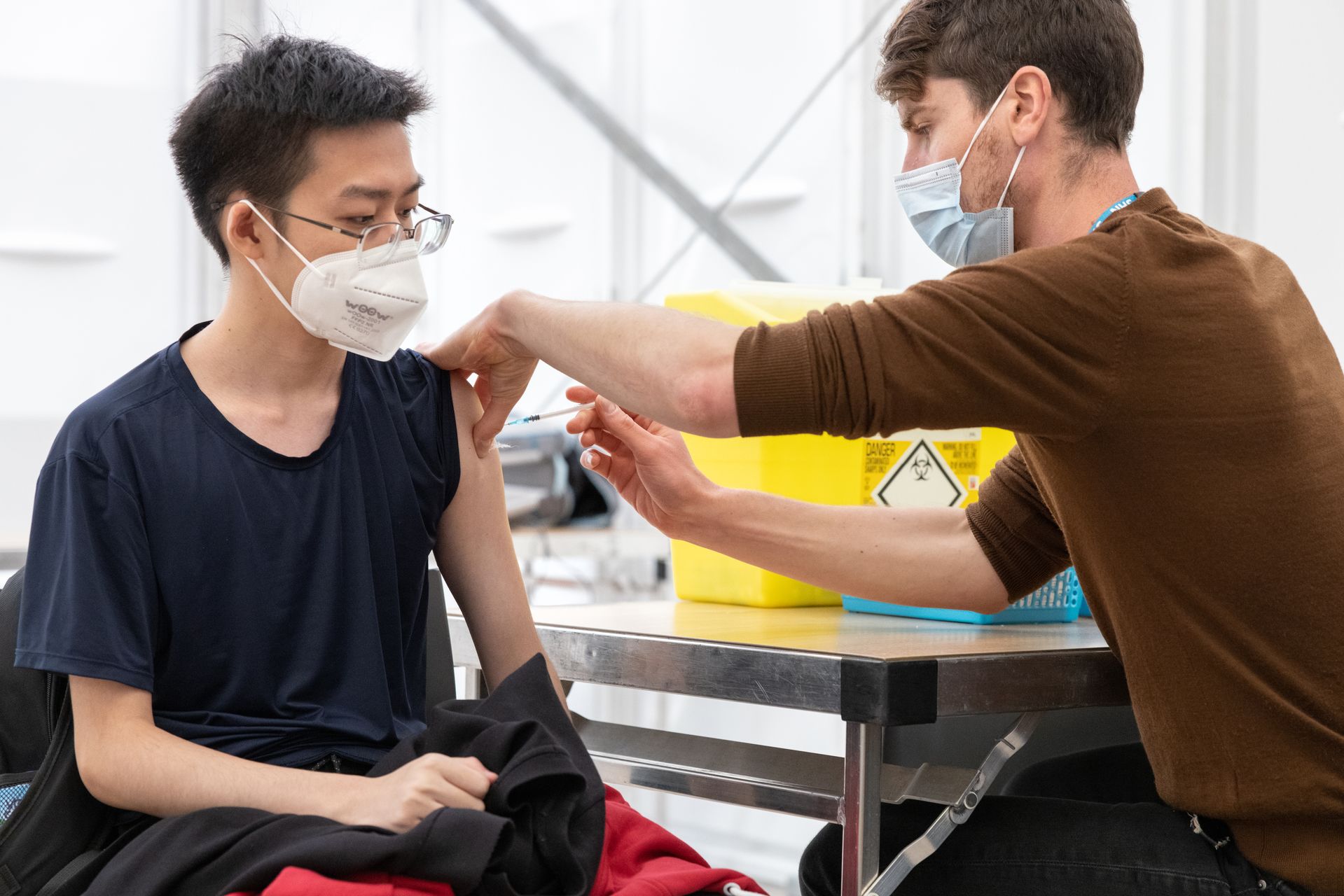
As ever, this is linked to other research being conducted at Imperial. Professor Helen Ward, Professor of Public Health, is ARC NWL theme lead for the Patient, Public and Community engagement and Involvement Theme. Professor Ward also directs Imperial’s Patient Experience Research Centre (PERC) and the Real-time Assessment of Community Transmission (REACT) programme of home testing for COVID. "The ARC theme that I lead is ensuring that patients and communities are closely involved in the work of all themes, while conducting our own research on how best to work with communities in an inclusive and effective way to improve population health,” she says. "The REACT work has many links to my work in the ARC, for example on vaccine uptake, where we had national data showing how vaccine confidence varied between groups, and we were able to explore the reasons people gave for hesitancy. That was in February 2021 when the vaccine roll-out was just getting up to speed, and we found a clear link between vaccine hesitance and deprivation, ethnicity, gender and age. Women, and some men, were expressing concerns about fertility, allergies, and interactions with other health conditions. That was useful to feed into local plans to address vaccine hesitancy in north-west London, where there are many communities with some reluctance and a lot of questions. I hope that the work in the ARC, where we have links with community organisations and public advisors, can directly address those questions and directly support interventions to improve vaccine uptake and confidence."
"That’s not all", Professor Ward explains. "We also have a major new study on long COVID, an extension of the REACT programme, and we’re recruiting some people from the local area to come into clinics and provide further samples so that we can look into biological factors involved in the development of long COVID. This study will involve of 10,000 people who’ve had COVID, some in north-west London where we’re doing a whole raft of studies and tests. At the same time we are doing surveys to see how common ongoing symptoms and problems are, and how those have been treated. We’re building strong links to patient groups and patient advisers, nationally and locally, to help shape the research and ensure that any findings are rapidly linked into health improvement. We are hoping that from that we can work through the ARC to develop interventions, support and awareness-raising to get people reporting their symptoms and seeking support for them."
I hope that the work in the ARC, where we have links with community organisations and public advisors, can directly address those questions and directly support interventions to improve vaccine uptake and confidence.

An amazing collaboration
The ARC brings together a whole range of clinicians and researchers from across different specialisms. "I am an infectious disease epidemiologist with a focus on participatory approaches to research and service improvement. The ARC team includes people from a range of backgrounds, as does the REACT team.
During the pandemic we have worked really closely together in an amazing collaboration. It’s been the most intense, but also the most rewarding, work I’ve ever done, often with daily virtual team meetings, and it’s been non-stop since early 2020," says Professor Ward.
Professor Saxena adds: “There’s an awful lot of work to do, and an awful lot of projects, but we have an amazing team. It’s when you get everyone together that the magic starts.”
Stay up to date with NIHR ARC Northwest London on Twitter @ARC_NWL