New imaging technique could detect fatty deposits that cause heart attacks
by Kerry Noble
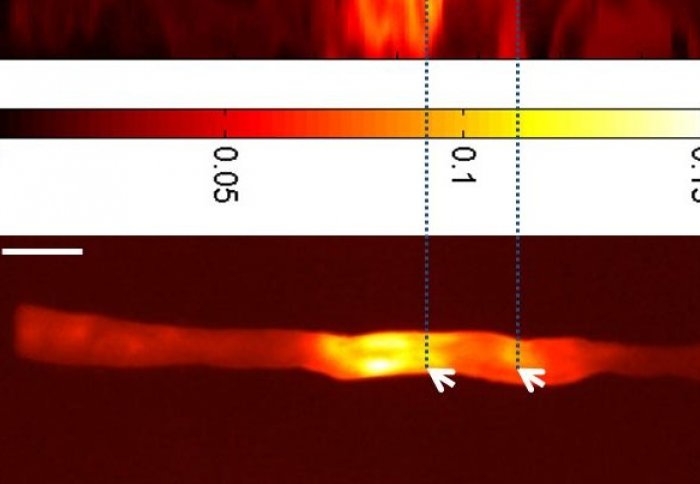
Scientists have found a new way to detect and visualise fatty plaques in arteries that can rupture and cause a heart attack or stroke.
The team at Imperial used a new imaging technique, called fluorescence molecular tomography, to determine the amount of a substance called oxidised low-density lipoprotein (OxLDL), within plaques in mice.
OxLDL is known to play a major role in atherosclerosis in humans and is present in high quantities in plaques most likely to lead to a heart attack or stroke.
Lead researcher Dr Ramzi Khamis from the National Heart and Lung Institute, explained: “With this research we’re trying to pick out the plaques that are most likely to rupture before they cause a heart attack. Our next step will be to modify the technique that we’ve used here so that it can be used in patients to detect dangerous plaques.”
We have not only found a possible new diagnostic tool, we may also have discovered a new way to treat this deadly disease.
– Dr Ramzi Khamis
Fatty plaques are particularly dangerous in the walls of the arteries that lead to the brain or heart because if they rupture, a deadly blood clot can form and block the blood supply, causing either a heart attack or stroke. Each year in the UK over 100,000 people die after suffering from these events.
If doctors can identify these plaques, they could treat them using targeted drugs or by implanting a stent in the affected areas.
In order to see how much OxLDL was present in the plaques the team used a specially designed antibody that targets OxLDL. A fluorescent marker was added to the antibody so that the researchers could visualise the areas of the plaque which contained large amounts of OxLDL.
During a second part of the research, performed in collaboration with Harvard Medical School, a special infrared catheter was used to look inside the artery and detect any fluorescently-labelled antibody. The researchers hope that this approach will make details visible which are usually invisible to doctors using current technology to look at atherosclerotic plaques.
The researchers are now working towards using the technique in people and can already detect the human form of OxLDL. The technique could eventually be used in hospitals to assess how likely an atherosclerotic plaque is to rupture.
This promising line of research now needs to be tested in patients
– Professor Peter Weissberg
British Heart Foundation
Dr Khamis added: “We are also looking at the possibility of using the same antibody that we’ve developed to image the plaque to deliver drugs directly to the plaque itself. So, we have not only found a possible new diagnostic tool, we may also have discovered a new way to treat this deadly disease.”
The research was funded by the British Heart Foundation. Professor Peter Weissberg, Medical Director of the British Heart Foundation, said: “Each year in the UK over 100,000 people die from a heart attack or stroke that has been caused by rupture of a fatty deposit, called a plaque, on the inside of an artery. Discovering which plaques are likely to rupture is a major objective of current research.
“If confirmed in humans with heart disease, this technique could lead to early intervention to prevent a heart attack. Furthermore, the homing antibody could be used to deliver drugs directly to unstable plaques. This promising line of research now needs to be tested in patients.”
Professor Dorian Haskard, the senior author and Head of Vascular Sciences at Imperial College London, said: “This exciting research breaks new ground in the molecular imaging of heart disease and could not have been achieved without funding from the British Heart Foundation.”
The study was published in the Nature open access journal Scientific Reports and was also funded by the Wellcome Trust/GSK TMT programme at Imperial College London and the British Atherosclerosis Society Binks Award.
Adapted from a British Heart Foundation press release.
Article supporters
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Kerry Noble
Department of Surgery & Cancer
