Keyhole surgery for ruptured arteries has longer-term benefits for patients
by Ryan O'Hare
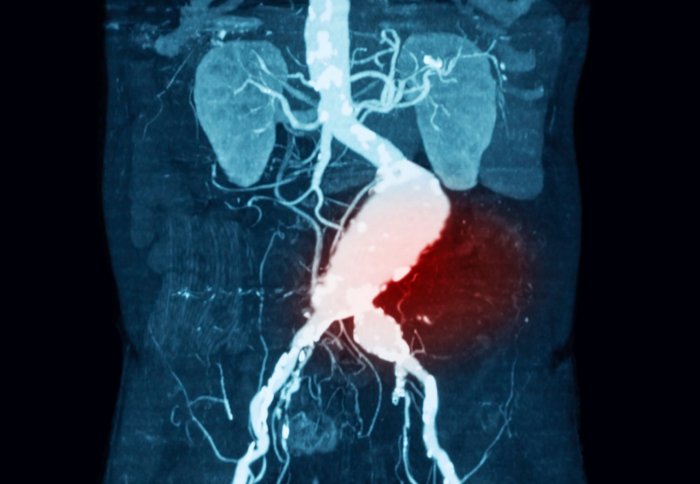
Abdominal aortic aneurysms can be fatal
More surgeons should opt for keyhole surgery to repair ruptured blood vessels in the abdomen rather than using open surgery, a study has found.
Abdominal aortic aneurysms occur when the aorta, the main vessel carrying blood from the heart to the rest of the body, swells and ruptures. If patients do not receive surgery to repair the artery they almost certainly will die from internal bleeding.
Previous trials following patients in the initial months after surgery had shown that keyhole repair does not reduce the high death rate compared with open repair. However, outcomes of keyhole repair procedures from three months to three years are still uncertain.
In the first randomised trial to compare the mid-term follow-up of the two treatments for patients with aortic aneurysms, researchers from Imperial College London and their partners found that using the keyhole approach, whenever possible, is both clinically and cost effective and should be adopted more widely.
Repairing arteries
Writing in a paper published this week in The BMJ, the authors report on three year clinical outcomes and cost effectiveness of keyhole repair for patients with suspected ruptured abdominal aortic aneurysm who were part of the IMPROVE trial.
The trial involved 613 patients from 30 vascular centres (29 in the UK, one in Canada) with a clinical diagnosis of ruptured aneurysm, of whom 316 were randomised to receive keyhole repair and 297 to have open surgery repair.
Deaths were monitored for an average of 4.9 years and were similar in both groups three months after surgery.
After three years, there were fewer deaths in the group that were allocated to keyhole surgery if possible compared with those who had open surgery repair, leading to lower mortality (48% vs 56% respectively). However, after seven years there was no clear difference between the groups.
They found the need for repeat surgery related to the aneurysm occurred at a similar rate in both groups, with about 28% of each group needing at least one repeat surgery after three years.
Quality of life gains
While average quality of life was higher in the keyhole group in the first year, by three years it was similar across the groups. This early higher average quality of life, coupled with the lower mortality at three years, led to a gain in average quality adjusted life years or QALYs – a measure of healthy years lived – at three years in the keyhole versus the open repair group. The keyhole group also spent fewer days in hospital and had lower overall costs.
The researchers point to some study limitations, such as sample size and limited data for some outcomes midterm data focusing on aneurysm-related events, however, they say compared with open repair: “an endovascular strategy for suspected ruptured abdominal aortic aneurysm was associated with a survival advantage, a gain in QALYs, similar levels of re-intervention, and reduced costs, and this strategy was cost effective”.
Commenting on the findings, Professor Janet Powell, from the Department of Surgery & Cancer at Imperial, said: “These latest findings from the IMPROVE study support increasing the use keyhole surgery to repair aortic aneurysms where possible."
"Making emergency endovascular repair available more widely could help to improve survival rates and longer-term outcomes for more patients,” she added.
-
'Comparative clinical effectiveness and cost effectiveness of endovascular strategy v open repair for ruptured abdominal aortic aneurysm: three year results of the IMPROVE randomised trial’ by the IMPROVE Trial Investigators is published in The BMJ.
This article is based on materials provided by The BMJ.
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Ryan O'Hare
Communications Division