High-impact COVID-19 projects strengthened by Community Jameel fund

The custom-made masks being developed by Dr Connor Myant
A new fund supported by Community Jameel is driving the scale-up of projects that could have a major impact in the global fight against COVID-19.
The projects, which range from new diagnostic tools to custom PPE manufacturing, are advancing our understanding of the disease and its impact, as well as unlocking new avenues for international efforts to prevent, diagnose and treat it.
The £1 million Community Jameel Imperial College COVID-19 Excellence Fund provides financial support research into the impact, understanding, prevention, diagnosis, and treatment of COVID-19. It provides grants of up to £200,000 to rapidly scale up high-impact projects.
The fund is supported by donations from Community Jameel, the global philanthropy founded by Mohammed Jameel KBE, and Imperial’s President’s Excellent Fund. It sits alongside Imperial’s COVID-19 Response Fund, which provides rapid and flexible smaller pots of funding for projects across the College, as well as supporting staff and students working on the frontlines of the crisis in hospitals.
Understanding COVID-19

Dr Edward Mullins and Professor Christl Donnelly are leading a study evaluating the timing and extent of community spread of COVID-19 in North West London from December 2019 to June 2020 by anonymously testing existing serum samples that were taken as part of routine antenatal care for pregnant women in the region. The results will provide insights to community transmission risks over the course of the pandemic, as well as inform policy on the management of pregnant women in a future wave of the pandemic.
Neurological complications are common in respiratory viral infections, and there is growing concern that of the potential for COVID-19 to affect the nervous system as highlighted by reported symptoms such as a loss or change of taste and smell. Dr Javier Alegre-Abarrategui, from the Department of Brain Sciences, is investigating COVID- 19 in human brain and its potential role in triggering long term neurological disease.
Identifying new therapies
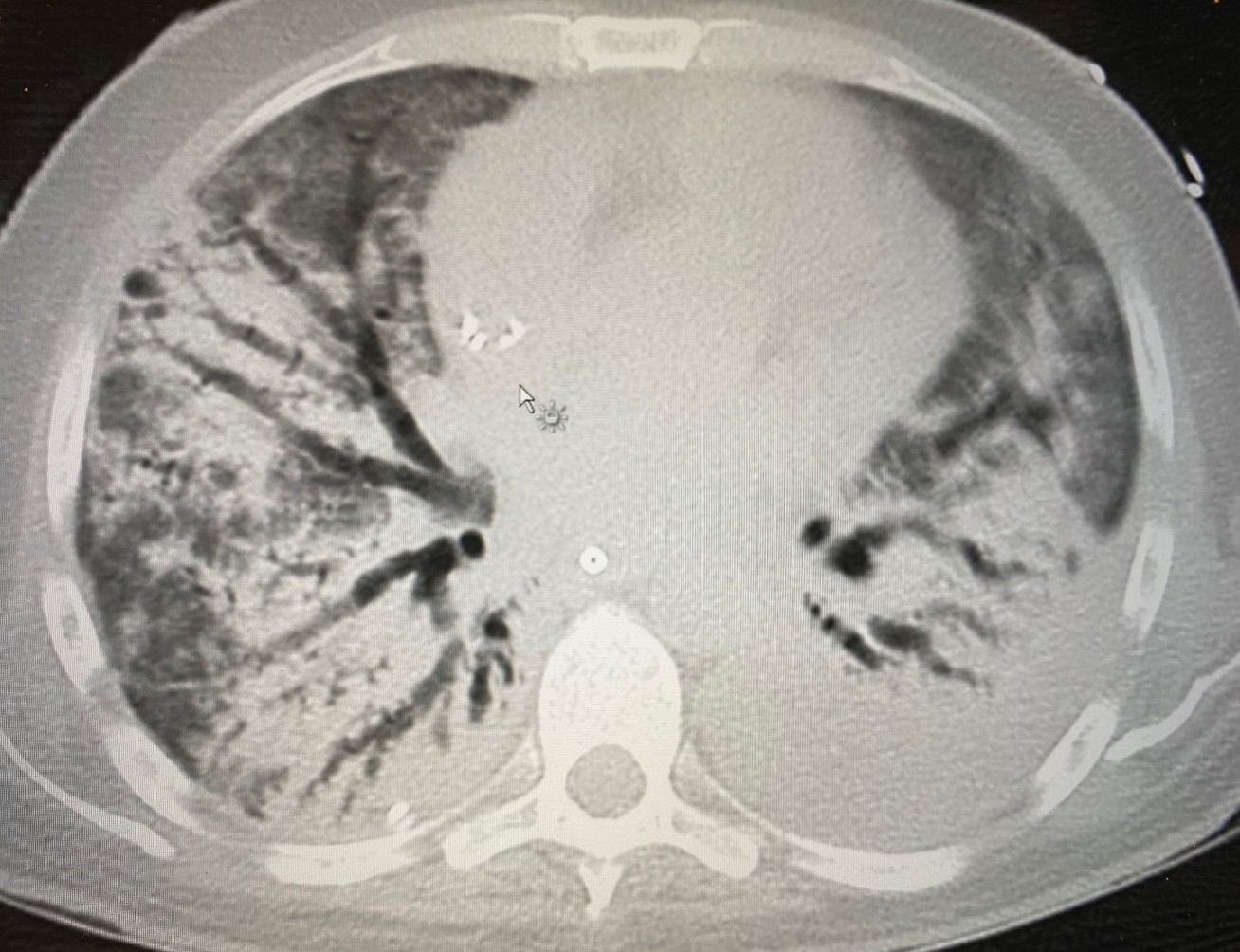
Professor Ian Adcock, from the National Heart and Lung Institute, aims to investigate the key driving signatures of fibrosis and necrosis in the lungs in COVID-19 patients and relate these to drug-response signatures. The study uses lung samples obtained from the ongoing DeVENT trial. This will identify whether it is possible to repurpose current drugs to treat specific groups of patients with severe COVID-19 patients in ICU or define pathways that are likely to respond to other currently available therapies.
Dr James Peters and colleagues from the Centre for Inflammatory Disease and the Imperial NHS Trust Renal and Transplant Centre are conducting a longitudinal study of patients with End-Stage Kidney Disease – a group at high risk of severe COVID-19 - measuring gene and protein expression signatures in immune cells to better understand the biological mechanisms underlying severe disease. They hope that this might help identify existing drugs that could be repurposed as safer and more effective treatments for COVID-19 than dexamethasone, which is the only drug shown to reduce mortality in randomised trials to date
Monitoring and testing
The difference in patient response to COVID19 infection is stark from mild to fatal. Professor Brendan Delaney, from the Department of Surgery and Cancer, is looking to develop and validate a score for predicting risk of deterioration in COVID-19 patients. The tool, known as RECAP (Remote COVID-19 Assessment in Primary Care) would help identify patients who need closer monitoring and escalation of care in primary care settings, such as GP surgeries. The project is a collaboration with Professor Trisha Greenhalgh from the Nuffield Department of Primary Care, University of Oxford.
 Dr Jethro Herberg, from the Department of Infectious Disease, and Dr. Pantelis Georgiou from the Department of Electrical and Electronic Engineering, in partnership with the Rosetrees Trust, are developing a cheap, accurate, geo-tagged point-of-care test for COVID-19 using Lacewing technology - a mobile-phone-linked handheld molecular diagnostic system. The uniqueness of their approach is that they will use the host response to discriminate a variety of infections with similar symptoms to COVID-19, in addition to SARS-CoV-2. This test will guide diagnosis, treatment and surveillance in the ongoing COVID-19 pandemic, producing rapid public health impact.
Dr Jethro Herberg, from the Department of Infectious Disease, and Dr. Pantelis Georgiou from the Department of Electrical and Electronic Engineering, in partnership with the Rosetrees Trust, are developing a cheap, accurate, geo-tagged point-of-care test for COVID-19 using Lacewing technology - a mobile-phone-linked handheld molecular diagnostic system. The uniqueness of their approach is that they will use the host response to discriminate a variety of infections with similar symptoms to COVID-19, in addition to SARS-CoV-2. This test will guide diagnosis, treatment and surveillance in the ongoing COVID-19 pandemic, producing rapid public health impact.
Innovative PPE
 Dr Connor Myant, from the Dyson School of Design Engineering, is developing an automated design-through-manufacturing pipeline that would allow for custom-made masks to be deployed to frontline healthcare workers at scale. His project aims to deliver a design platform that would see healthcare workers scanning their own face using a smartphone so that custom-fit PPE can be automatically designed for them. This aims to tackle the problem of poor-fitting PPE causing injury and discomfort to healthcare professionals and putting them at a greater risk of infection.
Dr Connor Myant, from the Dyson School of Design Engineering, is developing an automated design-through-manufacturing pipeline that would allow for custom-made masks to be deployed to frontline healthcare workers at scale. His project aims to deliver a design platform that would see healthcare workers scanning their own face using a smartphone so that custom-fit PPE can be automatically designed for them. This aims to tackle the problem of poor-fitting PPE causing injury and discomfort to healthcare professionals and putting them at a greater risk of infection.
These projects will all start immediately and will report back on progress over the coming months.
Article supporters
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Deborah Evanson
Communications Division