Direction of needle penetration in brain affects drug uptake, finds new study
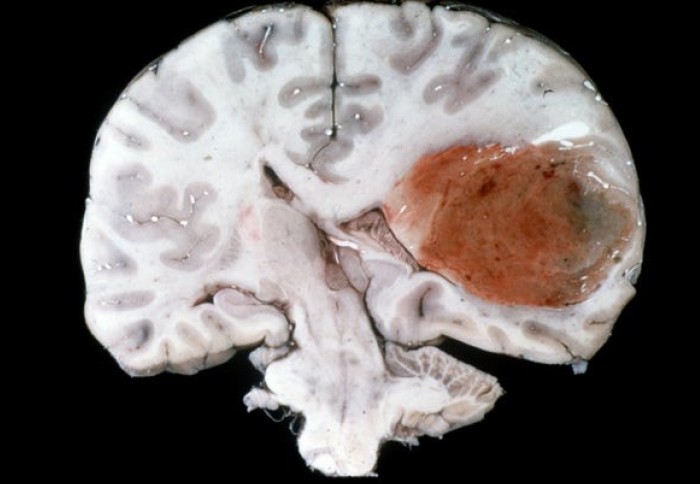
Glioblastoma causes 250,000 deaths per year worldwide and is notoriously difficult to treat
The direction at which drug-delivering needles enter the brain affects how well medicine permeates, a new Imperial study on sheep brains has found.
The study, led by Imperial College London as part of the Enhanced Delivery Ecosystem for Neurosurgery in 2020 (EDEN2020) consortium, looked at how well fluid injected into the brain permeated ‘white matter’ depending on the needle's direction.
Until now, brain injections were thought to uniformly distribute drugs in all directions. Our work challenges this and finds that needle direction could in fact be important in effective treatment. Dr Asad Jamal Department of Mechanical Engineering
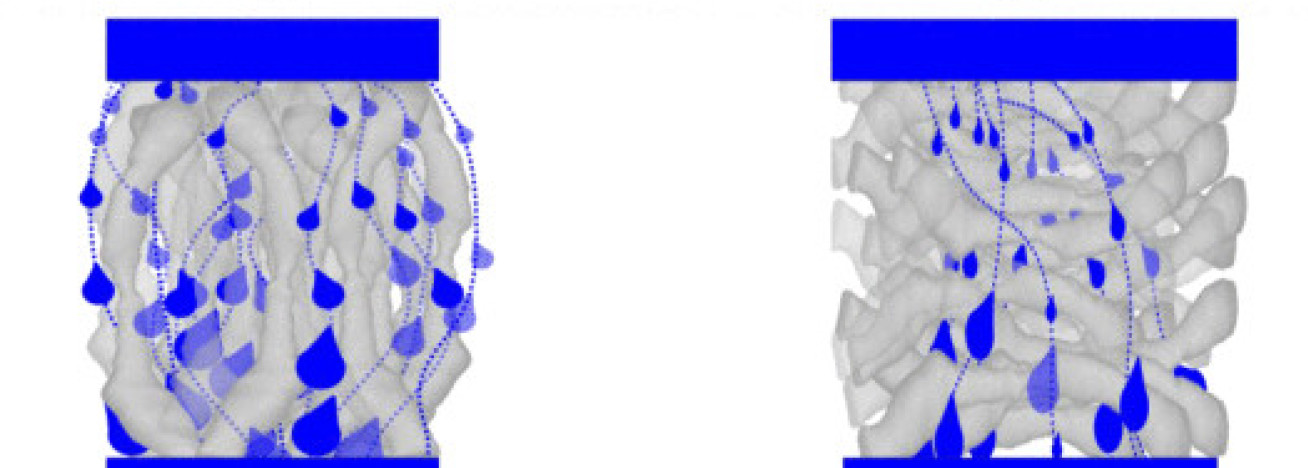
They found that needles entering parallel to brain fibres, called axons, led to better fluid uptake in targeted brain areas, while needles that entered perpendicular to axons resulted in reduced fluid uptake.
The findings, published in IEEE Transactions on Biomedical Engineering, could help inform future brain infusion treatments for aggressive white matter cancers like multiforme, which causes 250,000 deaths per year worldwide and is notoriously difficult to treat.
Lead author Dr Asad Jamal, of Imperial’s Department of Mechanical Engineering, said: “Our results confirm that directionality is important when infusing drugs into the brain, which in turn supports the use of a steerable needle for drug delivery. Until now, brain injections were thought to uniformly distribute drugs in all directions. Our work challenges this and finds that needle direction could in fact be important in effective treatment.”
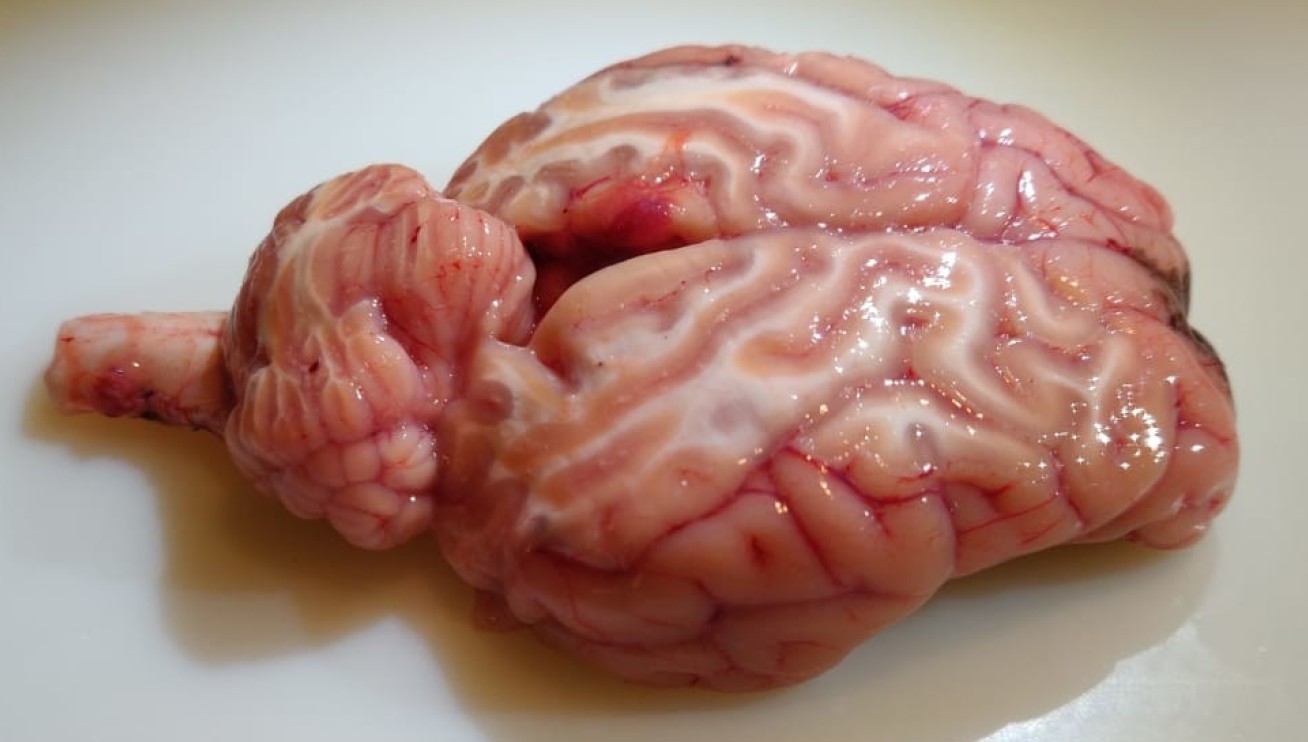
Nerve cells, known as neurons, resemble long spindly fibres with branch-like appendages at either end. The long spindly part of neurons, called axons, and the area surrounding them make up the brain’s white matter, which is where messages are relayed via the axons to different brain areas and the spinal cord.
White matter, which makes up most of the brain, can suffer aggressive tumours. Current treatments like radiotherapy and chemotherapy infused into patients’ veins are limited in their capacity to deliver therapeutic drugs to kill white matter cancer cells. This is because these cells can be buried deep in the brain and are hard to get to without also harming healthy cells and causing debilitating side effects.
As a result, doctors are increasingly turning to injecting therapeutic drugs directly into the brain, but not much is known about the way fluids move through the brain and how they could be directed to treat specific brain areas or cells.
In the new paper, Imperial researchers have tested for the first time how drugs travel through white matter depending on the arrangement of axons.
Using a setup called iPerfusion, the researchers looked at the axon arrangement in pieces of sheep brain and how a saline solution moved into and around them. They found that fluid injected parallel to axons permeates better into targeted areas than fluid injected perpendicular to axons.
To do this they suspended brain tissue from sheep in a saline solution-filled petri dish before infusing it with a needle from different directions. The iPerfusion setup measured both the pressure and flow of the infused fluid as it permeated the tissue.
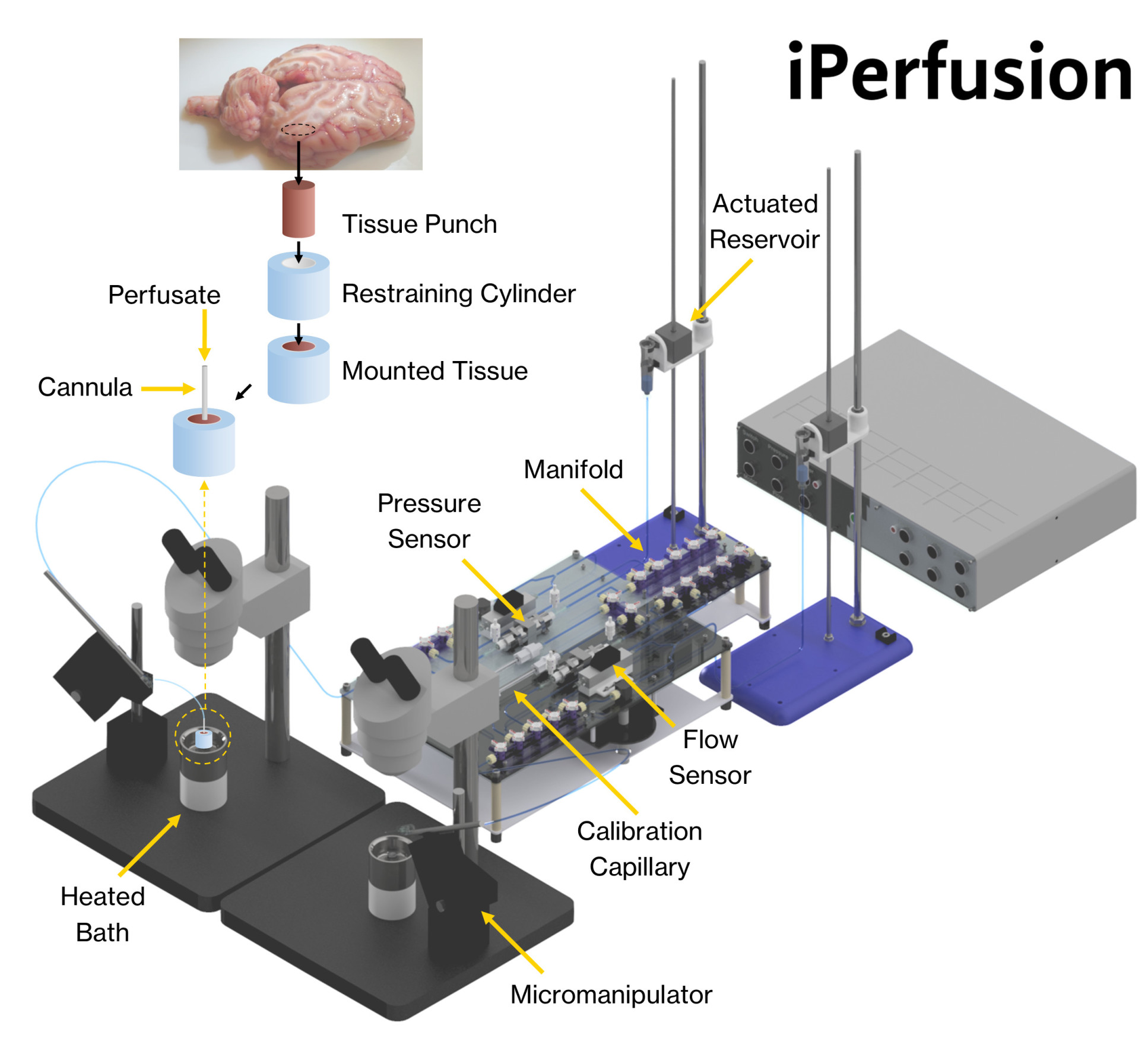
Drugs flow through tissue under a positive pressure gradient, like water being pushed through a hose using a pump. Although computer modelling studies have previously suggested directionality influences on drug flow, this is the first time experiments on real brains have been conducted.
These findings highlight the importance of using steerable needles to get the therapeutic drugs to where they are most needed Professor Bello Lorenzo University of Milan
The researchers say their findings could help surgeons know which direction to aim steerable needles when infusing drugs directly into the brain, and that the next step will be to confirm the findings in whole, human brains with anti-cancer drugs.
They also say the steerable nature of the technique means they can specifically target both the tumour bulk as well as the areas it might be infiltrating, improving its anti-cancer action.
Professor Bello Lorenzo of the University of Milan, who led the clinical team involved in the EDEN2020 project, said: “Glioblastomas and other white matter cancers are notoriously difficult to treat. These findings highlight the importance of using steerable needles to get the therapeutic drugs to where they are most needed, and could eventually help to improve patient outcomes.”
This work was funded under the EU’s Horizon 2020 programme.
"Infusion Mechanisms in Brain White Matter and their Dependence on Microstructure: An Experimental Study of Hydraulic Permeability," by Jamal et al., published April 2021 in IEEE Transactions on Biomedical Engineering.
Main image: Getty
Body images: Asad Jamal et al.
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Caroline Brogan
Communications Division