Research brings new evidence to the 10 year debate on COX-2 pain relief drugs
New research has challenged theories on side effects of COX-2 drugs, calling for different approaches to identify patients who could use them safely.
The controversial COX-2 inhibitors are potent pain relief drugs. Although effective and safe for the majority of people, development of COX-2 inhibitors stopped with the dramatic withdrawal of the blockbuster drug Vioxx in 2004 due to concerns about its link to stroke and heart attacks. There is still no unified understanding in this area and a team at Imperial College London has now taken important steps in explaining the side effects. This could lead to better methods to determine those who could safely benefit from these drugs.
Our results send a clear message that we need to look for new approaches to answer this old question of why side effects occur.
– Professor Jane Mitchell
Professor of Pharmacology in Critical Care Medicine
Published in PLOS ONE the new research overturns previous theories that propose the side effects are caused by a reduction in a hormone that protects blood vessels from cholesterol build-up. Instead the research demonstrates that the effects are caused by remote activity of COX-2 inhibitors, possibly in organs such as the brain, lungs, kidney or gut.
The team have also found a link between COX-2 and the RGL1 gene, which has no obvious role in heart attacks and strokes but has been implicated in cancer. COX-2 inhibiting drugs are known to have a potential clinical role in treating cancer which makes the RGL1 discovery very important in understanding how these drugs work.
Lead researcher Professor Jane Mitchell at the National Heart & Lung Institute, Imperial College London, said: “Our results send a clear message that we need to look for new approaches to answer this old question of why side effects occur. The previous hypothesis that COX-2 inhibitors remove local protection against atherosclerosis at the level of the blood vessels no longer holds. Currently we are prescribing and selling other non-steroid anti-inflammatory drugs (NSAIDs) that, at a therapeutic dose, have the same risk of cardiovascular side effects as the COX-2 drugs but with the additional danger of gastrointestinal side-effects.”
COX-2 inhibitors are potent pain relief drugs that were considered preferable to other NSAIDs such as ibuprofen and diclofenac because they cause less gastrointestinal problems. These older style NSAIDs block COX-2 to relieve inflammation and pain, but also block COX-1. Drugs that block both COX-1 and COX-2 increase the risk of gastric ulcers and bleeds. For this reason COX-2 selective drugs were developed with the aim that they would retain the therapeutic actions of NSAIDs but lose the gastric side effects, particularly for long-term pain such as those suffering arthritis.
The evidence that COX-2 inhibitors could help treat colon and other types of cancer is compelling but when concerns were raised in 2004 about a link between COX-2 inhibitors and the incidence of stroke and heart attacks Vioxx was withdrawn. The development of these drugs ceased and the potential for COX-2 inhibitors in cancer remains unexploited.
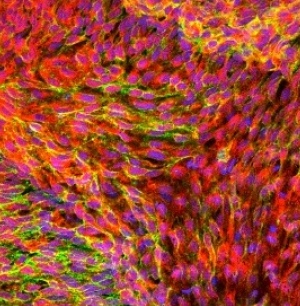
Atherosclerotic vessel showing abundant COX-1 expression (red)
Since the withdrawal of drugs such as Vioxx, a large research effort has been launched to try to establish the mechanisms by which these side effects occur and researchers at Imperial College London have made an important contribution to achieving this quest. The scientific jury is still out, but a widely held view is that COX-2 inhibitors prevent a protective hormone from dilating arteries when there is cholesterol build-up, leading to strokes and heart attacks. However using a mouse model the Imperial researchers have discovered that the release of this protective hormone is not driven by COX-2 but by COX-1, demonstrating that COX-2 inhibitors do not influence cholesterol build-up in arteries through this mechanism.
“Our research has re-opened a closed case in drug development,” said Dr Nicholas Kirkby also from Imperial’s National Health & Lung Institute and lead author of the paper. “When the side-effects were reported in 2004 Vioxx was withdrawn but perhaps more importantly there was a halt on the development of these drugs, meaning that some potentially excellent drugs never got to market. Our research has provided fresh insight into the effects of COX-2 drugs which we hope could inform future developments in profiling patients to assess if they can benefit from the COX-2 inhibitors and in defining a pathway to design better drugs with fewer side effects.”
Having ruled out the effect of COX-2 inhibitors on the hormonal protective system in the blood vessels the research team set out to establish how COX-2 inhibitors cause the clogging up of arteries, and discovered that this is through a more remote mechanism.
There are many candidate sites for this remote activity but the researchers focussed on the expression of the COX-2 gene in three important example regions: the liver, the lungs and the thymus, which is an organ in the chest associated with immunity. By removing the COX-2 gene the researchers mimicked the COX-2 inhibitors and studied the effects on tissues from the three sites. Rather than starting with a preconceived hypothesis the study investigated all genes from these three organs. In the tissues from all sites the researchers found that when the COX-2 gene was removed there was an alteration in the gene RGL1 suggesting a connection between the two. The RGL1 gene has been linked to cancer indicating a possible clinical role for COX-2 inhibitors and highlighting the need for more investigation into how exactly COX-2 regulates the expression of the RGL1 gene. It could be that this genetic pathway modulates cardiovascular side effects and potential therapeutic effects on cancer.
Professor Jane Mitchell said: “We’ve taken an unbiased approach to studying how COX-2 affects the body to supplement other hypothesis-driven studies. Instead of focussing on one pathway or one gene we’ve looked at the whole system so we’ve found innovative rather than pre-defined answers, which is why we discovered this completely new association of the RGL1 gene with the COX-2 gene. This finding is very exciting but requires future research to establish exactly what it means for clinical application. ”
The research was funded by the Wellcome Trust and Dr Kirkby is an Imperial College London Junior Research Fellow.
Reference: Kirkby, S. et al. (2014) COX-2 protects against atherosclerosis independently of local vascular prostacyclin: identification of COX-2 associated pathways implicate rgl1 and lymphocyte networks. PLOS ONE doi: 10.1371/journal.pone.0098165
Article supporters
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Franca Davenport
Communications and Public Affairs