Injected vaccine could help eradicate polio
by Sam Wong
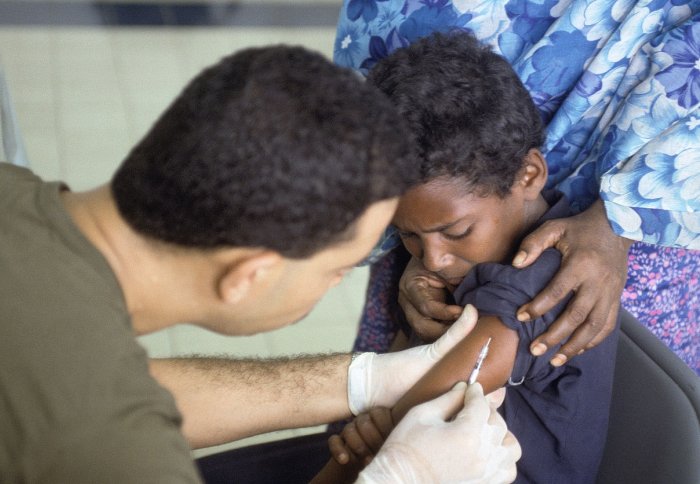
A Somali boy receives a polio vaccination in Mogadishu. Photo: PV2 Andrew W. McGalliard
Re-introducing a type of polio vaccine that fell out of favour in the 1960s could hasten eradication of the disease, according to new research.
The study, by Imperial College London and the Christian Medical College in Vellore, India, suggests that the injected polio vaccine (IPV), which is rarely used today in countries affected by polio, could provide better and longer lasting protection against infection if used in combination with the more commonly used live oral polio vaccine (OPV).
The findings are published today in The Lancet.
Vaccination protects an individual against contracting polio, but they can still be infected by the virus, which replicates in the gut and can be passed to others through contact with infected faeces. This has led to serious polio outbreaks in Asia, Africa and Europe over the last 10 years and is hampering efforts to eradicate the disease.
This implies that the IPV could be used to boost immunity in people travelling from or to polio-infected countries, such as Afghanistan, Pakistan and Nigeria.
– Professor Nick Grassly
MRC Centre for Outbreak Analysis and Modelling
Most vaccination campaigns use multiple doses of OPV that provide some gut immunity, although this wanes over time.
“Because IPV is injected into the arm, rather than taken orally, it’s been assumed it doesn’t provide much protection in the gut and so would be less effective at preventing faecal transmission than OPV,” explains Dr Jacob John, Associate Professor at the Christian Medical College, who led the study. “However, we found that where the children already had a level of immunity due to OPV, the injected vaccine actually boosted their gut immunity.
“In the 1960s there was extensive rivalry between the scientists who developed the two vaccines, with OPV eventually becoming the most popular. But it looks as if the strongest immunity can been achieved through a combination of the two.”
The study involved 450 children from a densely populated urban area in Vellore, India, all of whom had received the oral polio vaccine as part of a standard vaccination programme. Half of the children were given a dose of the injected vaccine and half given nothing. One month later, the children were given a ‘challenge’ dose of the live oral vaccine to simulate reinfection.
Their stools were tested after seven days to see if the virus was present, specifically the two remaining serotypes of the virus which are resisting eradication – serotype 1 and serotype 3. In the children who had received the IPV, the researchers found that 38 per cent fewer had serotype 1 in their stool and 70 percent fewer had serotype 3, compared to those who had not been given the injected vaccine.
“Our findings show that an additional dose of the injected vaccine is more effective at boosting immunity against infection than the oral vaccine alone,” says Nick Grassly, Professor of Vaccine Epidemiology at Imperial College London, senior author of the study. “This implies that the IPV could be used to boost immunity in people travelling from or to polio-infected countries, such as Afghanistan, Pakistan and Nigeria. It could also replace some of the OPV doses in immunisation campaigns to boost gut immunity, particularly in areas of poor sanitation.”
In another study, published this week in Proceedings of the National Academy of Sciences, Imperial researchers from the same group looked at whether expanding the age range of vaccination campaigns to include older children and adults would help to prevent polio transmission. Using a mathematical model to examine disease transmission in two major polio outbreaks in Tajikistan and the Republic of Congo in 2010, they found that older ages contributed significantly to transmission in Congo but not Tajikistan, which might be related to standards of sanitation and hygiene. However, launching mass immunisation campaigns more quickly in response to outbreaks would have a much bigger impact than expanding the age range, the study reported.
Lead author Dr Isobel Blake from the Medical Research Council Centre for Outbreak Analysis and Modelling at Imperial College London said: “It can take over 70 days to send stool samples to the lab and get back a diagnosis of polio, which means by the time authorities discover an outbreak, many more people are already infected. These findings suggest that methods to detect outbreaks earlier would be hugely beneficial to eradication efforts.”
The Lancet study was funded by the Bill & Melinda Gates Foundation. The PNAS study was supported by a grant from the Polio Research Committee of the World Health Organization, the Royal Society, and Centre funding from the Medical Research Council.
References
John et al. “Effect of a single inactivated poliovirus vaccine dose on intestinal immunity against poliovirus in children previously given oral vaccine: an open-label randomised controlled trial” The Lancet, 10 July 2014 D-14-02958R2 S0140-6736(14)60934-X
Blake et al. ‘The role of older children and adults in wild poliovirus transmission.’ PNAS, 7 July 2014. doi: 10.1073/pnas.1323688111
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Sam Wong
School of Professional Development