Severe infections wreak havoc on mouse blood cell production
Bone-forming cells called osteoblasts shown in green
Severe infections like malaria cause short and long-term damage to precursor blood cells in mice, but some damage could be reversed, find researchers.
A team led by researchers from Imperial College London and The Francis Crick Institute have discovered that severe infections caused by malaria disrupt the processes that form blood cells in mice. This potentially causes long-term damage that could mean people who have recovered from severe infections are vulnerable to new infections or to developing blood cancers.
These changes could cause long-term alterations, but we also found a way to significantly reduce the amount of damage and potentially rescue the healthy production of blood cells. Dr Myriam Haltalli
The team also discovered that the damage could be reduced or partially reversed in mice with a hormone treatment that regulates bone calcium coupled with an antioxidant. The research could lead to new ways of preventing long-term damage from severe infections including malaria, TB and COVID-19.
The research is published today in Nature Cell Biology.
First author Dr Myriam Haltalli, who completed the work while at the Department of Life Sciences at Imperial, said: “We discovered that malaria infection reprograms the process of blood cell production in mice and significantly affects the function of precursor blood cells. These changes could cause long-term alterations, but we also found a way to significantly reduce the amount of damage and potentially rescue the healthy production of blood cells.”
Unexpectedly fast changes
Blood is made up of several different cell types, that all originate as haematopoietic stem cells (HSCs) in the bone marrow. During severe infection, the production of all blood cells ramps up to help the body fight the infection, depleting the HSCs.
Now, the team has shown how infections also damage the bone marrow environment that is crucial for healthy HSC production and function. They discovered this using advanced microscopy technologies at Imperial and the Crick, RNA analyses led by the Gottgens group at Cambridge University, and mathematical modelling led by Professor Ken Duffy at Maynooth University.
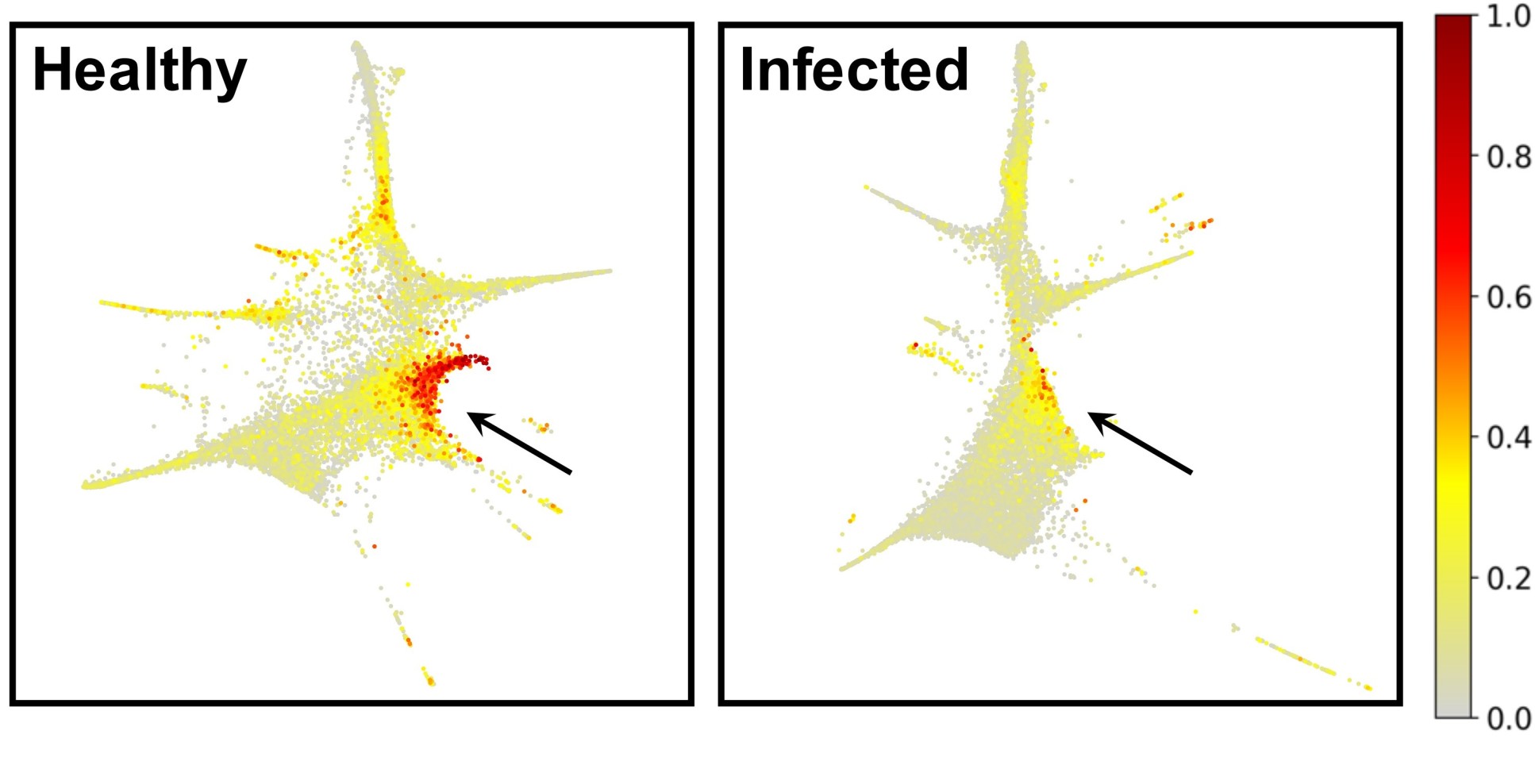
The mice developed malaria naturally, following bites from mosquitoes carrying Plasmodium parasites, provided by Dr Andrew Blagborough at Cambridge University. The researchers subsequently observed the changes in the bone marrow environment and the effect on HSC function.
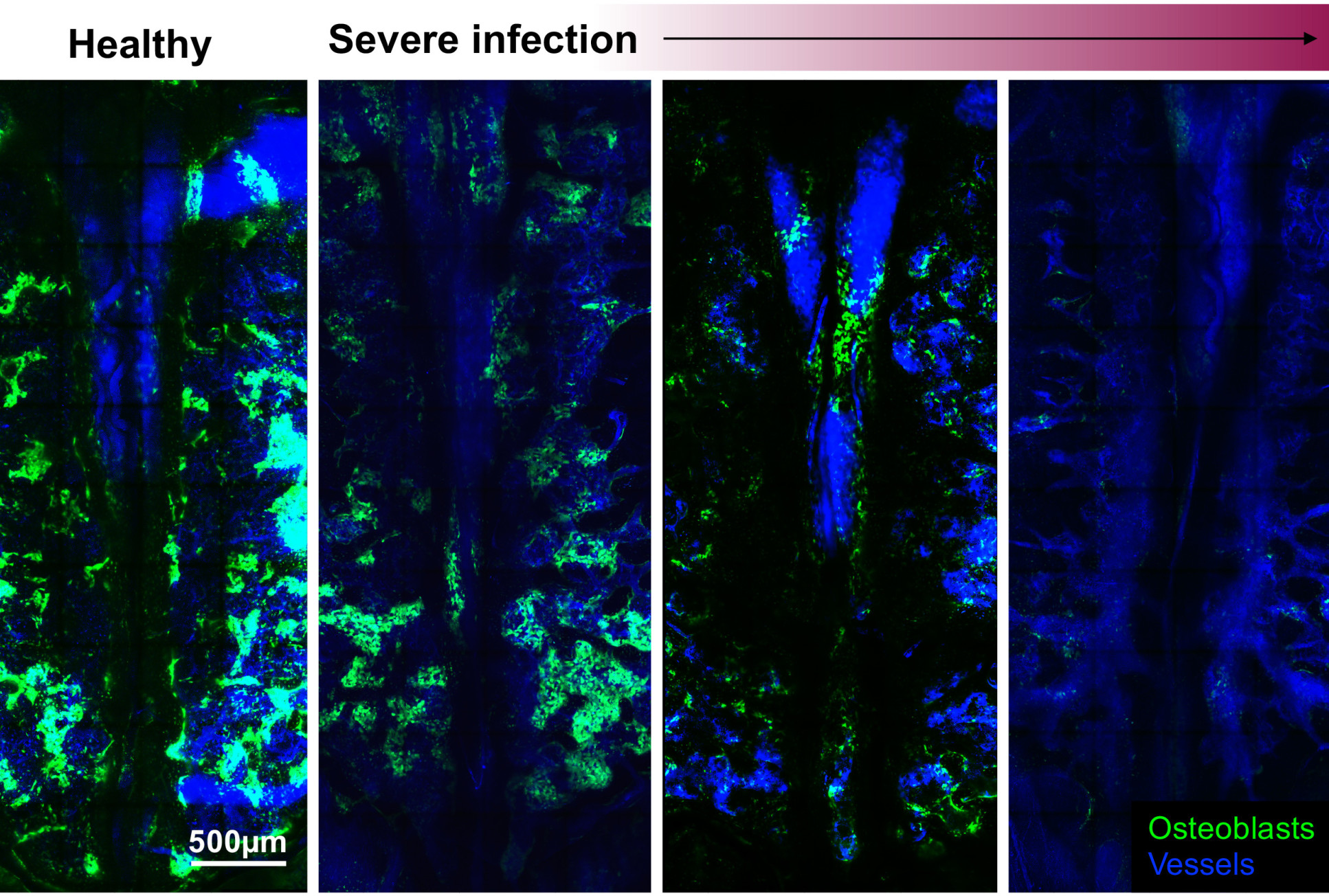
Within days of infection, blood vessels became leaky and there was a dramatic loss in bone-forming cells called osteoblasts. These changes appear strongly linked to the decline in the pool of HSCs during infection.
Lead author Professor Cristina Lo Celso, from the Department of Life Sciences at Imperial, said: “We were surprised at the speed of the changes, which was completely unexpected. We may think of bone as an impenetrable fortress, but the bone marrow environment is incredibly dynamic and susceptible to damage.”
Reducing the pool of HSCs can have several consequences. In the short-term, it appears to particularly affect the production of neutrophils – white blood cells that form an essential part of the immune system. This can leave patients vulnerable to further infections, with potentially long-term consequences for the functioning of the immune system.
In the long term, the pool of HSCs may remain below normal levels, which can increase the chances of the patient developing blood cancers like leukaemia.
By injecting fluorescent molecules (magenta) that would normally remain in circulation and taking a series of images over time, intravital microscopy revealed that infected mice had very leaky vessels – with the contents of the bone marrow blood vessels, lined by endothelial cells (green), escaping into the surrounding tissue. The red boxes highlight the areas compared in the analysis and the white lines mark the bone.
Mitigating the impacts
After determining in detail how severe infection affects the bone marrow environment and HSC function, the team tested a way to prevent the damage. Before infecting the mice, they treated them with a hormone that regulates bone calcium and an antioxidant to counter cellular oxidative stress, and then again after infection.
This process led to a tenfold increase in HSC function following infection compared to mice that received no treatment (around 20-40 per cent function compared to two percent function, respectively). Although this is not a complete recovery, the vast increase in function is a positive sign.
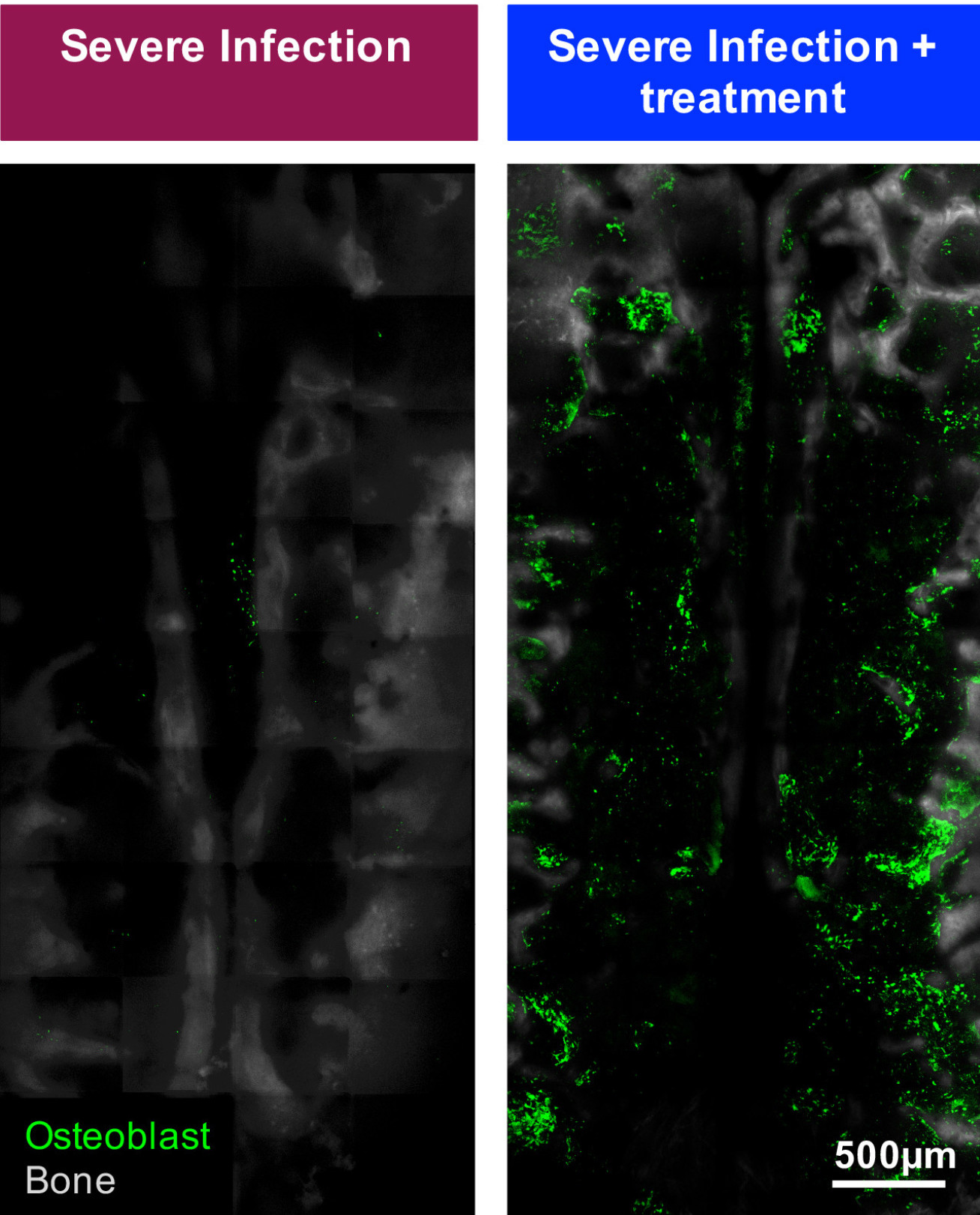
The team note that the requirement to start the hormone treatment before infection, combined with its expense and need to be refrigerated, make it unviable as a solution, especially in many parts of the world where severe infections like malaria and TB are prevalent.
However, they hope that proof that the impact of severe infection on HSC function can be significantly lessened will lead to the development of new treatments that can be widely administered.
Professor Lo Celso said: “The long-term impacts of COVID-19 infection are just starting to be known. The impact on HSC function appears similar across multiple severe infections, suggesting our work on malaria could shed light on the possible long-term consequences of COVID-19, and how we might mitigate them.”
Dr Haltalli concluded: “Protecting HSC function while still developing strong immune responses is key for healthy ageing.”
-
‘Manipulating niche composition limits damage to haematopoietic stem cells during Plasmodium infection’ by Myriam L.R. Haltalli et al. is published in Nature Cell Biology.
Article supporters
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Hayley Dunning
Communications Division