Using Indocyanine Green (ICG) to Identify Node for Breast Cancer Surgery
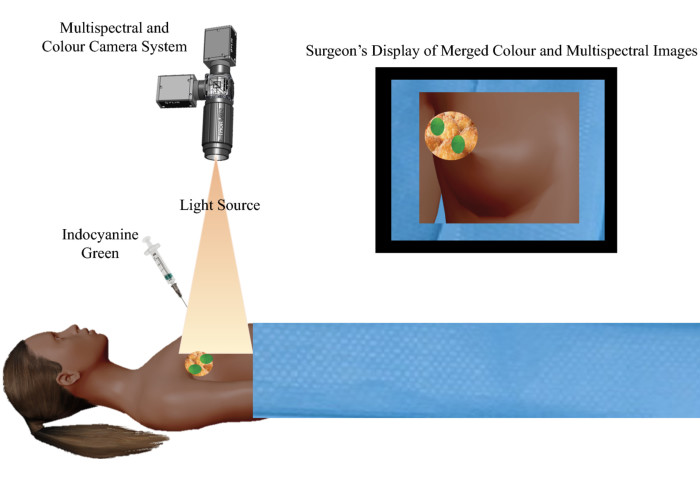
A Hamlyn-led project result suggests fluorescence-guided imaging for lymphatic mapping is superior to conventional methods for breast cancer surgery.
When it comes to breast cancer examination, the vast majority (around 90%) of clinically node-negative breast cancer patients undergo a sentinel lymph node biopsy (SLNB) staging procedure. The aim is to accurately identify the ‘sentinel’ or guardian nodes through lymphatic mapping.
However, conventional methods for axillary sentinel lymph node biopsy (SLNB) are fraught with complications such as allergic reactions, skin tattooing, radiation, and limitations on infrastructure. A novel technique, therefore, has been developed for lymphatic mapping utilising fluorescence imaging.
Meta-Analysis: Fluorescence-guided SLNB Using Indocyanine Green (ICG) versus Blue Dye and Radioisotope (BD-RI) technique
Collaborated with Department of Surgery and Cancer, our research team at the Hamlyn Centre generated a comparison meta-analysis report, aiming to compare the gold standard of [a conventional method] blue dye and radioisotope (BD-RI) technique, with [a novel technique] fluorescence-guided SLNB using indocyanine green (ICG).
Fluorescence imaging with currently approved exogenous fluorophores is a safe, non-ionising and rapid technique, with macroscopic visualisation capabilities to facilitate surgical guidance.
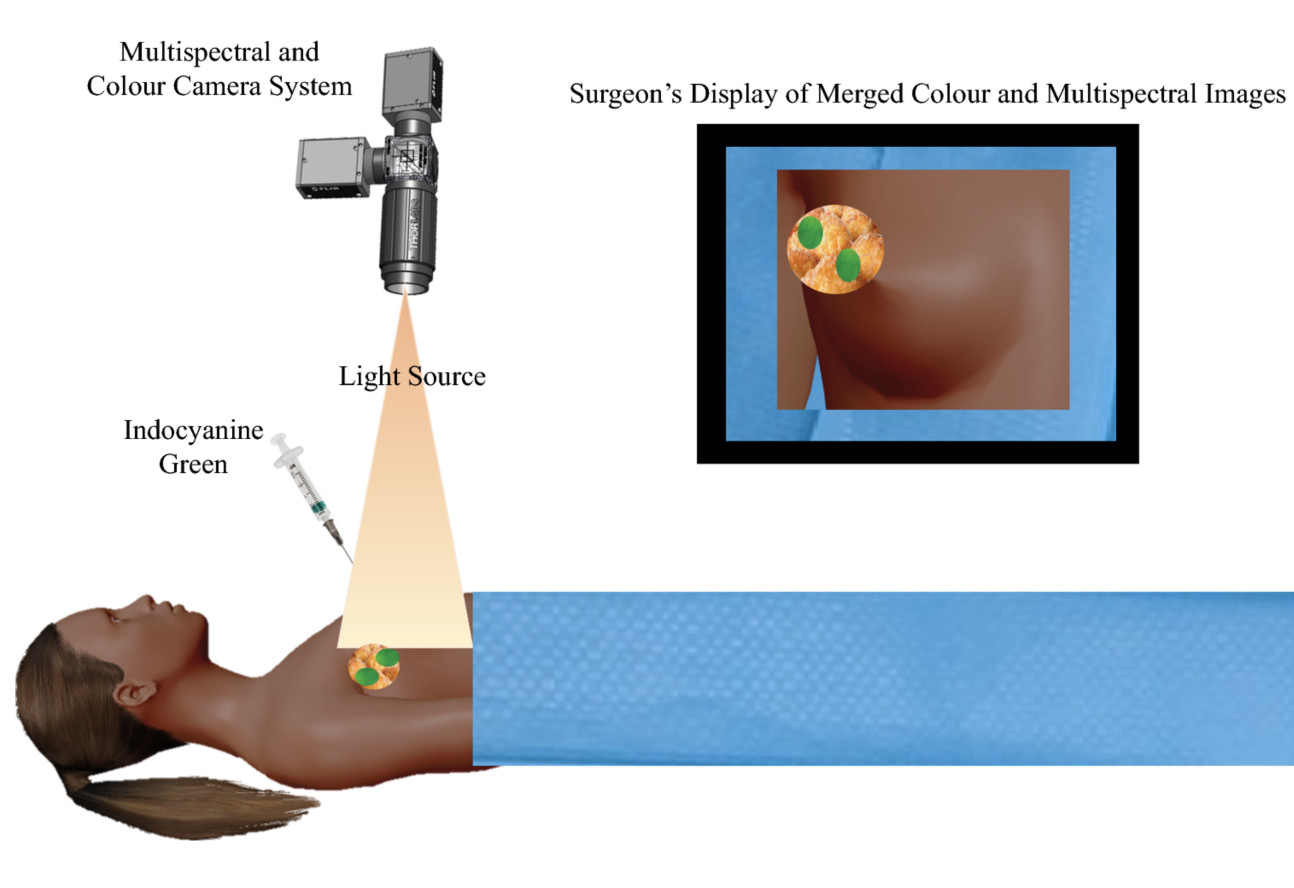 This method combines the use of a fluorescent contrast agent along with specialised cameras designed to capture the fluorescence (in the near-infrared spectral region), as well as visible light emitted from this agent.
This method combines the use of a fluorescent contrast agent along with specialised cameras designed to capture the fluorescence (in the near-infrared spectral region), as well as visible light emitted from this agent.
A fluorescent contrast agent is a special dye that is able to absorb and then emit light at specific wavelengths. The imaging system comprises a red/green/blue (RGB) camera that detects light in the visible spectrum, and a monochrome camera sensitive to near-infrared light to detect the light emitted by the fluorophore.
Images are then processed using software that enables the fluorescence image to be overlaid on to the normal visible image, enabling visualisation of the targeted specimen in relation to the surrounding tissue.
The research result of this study showed that fluorescence imaging for axillary sentinel node identification with ICG is equivalent to the single technique using RI, and superior to the dual technique (BD-RI) and single technique with BD.
Our researchers thus suggested that hospitals using RI and/or BD could consider changing their practice to ICG given the comparable efficacy and improved safety profile, as well as the lesser burden on hospital infrastructure.
This research was supported by the National Institute for Health Research (NIHR), Imperial Biomedical Research Centre (BRC), the Cancer Research UK (CRUK) Imperial Centre, and the Imperial Confidence in Concept (ICiC) Joint Translational Fund (Imperial College’s Medical Research Council [MRC] Confidence in Concept fund and the Engineering and Physical Sciences Research Council [EPSRC] Impact Acceleration Account scheme (Martha S. Kedrzycki, Maria Leiloglou, Hutan Ashrafian, Natasha Jiwa, Paul T. R. Thiruchelvam, Daniel S. Elson, and Daniel R. Leff, "Meta-analysis Comparing Fluorescence Imaging with Radioisotope and Blue Dye-Guided Sentinel Node Identification for Breast Cancer Surgery", Annals of Surgical Oncology, November 2020).
Article supporters
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Erh-Ya (Asa) Tsui
Enterprise