Delaying second doses of vaccine reduced COVID-19 hospitalisations and deaths
by Ryan O'Hare
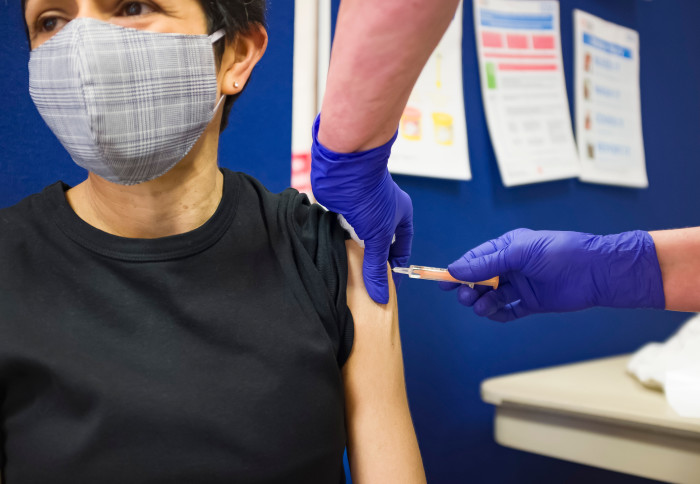
Delaying people’s second COVID-19 vaccine dose likely prevented tens of thousands of hospitalisations and thousands of deaths in England.
These are the findings of a retrospective analysis from the Imperial College London COVID-19 Response Team which aimed to quantify the impact of delaying the delivery of second vaccine doses on the epidemic in England.
Their analysis estimates that this may have prevented an average of 58,000 hospital admissions and 10,000 deaths between 8th December 2020 and 13th September 2021.
Increasing the interval between the first and second doses of COVID-19 vaccine from three to 12 weeks enabled a greater number of people to receive a first dose and gain partial protection from this, say the researchers.
This included younger age groups who were less vulnerable to severe disease, but who contributed more to transmission; therefore vaccinating them early indirectly protected the most vulnerable groups. As vaccine-induced protection wanes over time, the 12-week strategy also had the added benefit of maintaining a higher population-level immunity during the Delta wave in summer 2021.
The findings, from researchers at the MRC Centre for Global Infectious Disease Analysis and Jameel Institute at Imperial, are published in The Lancet Public Health.

Dr Anne Cori, from the MRC Centre for Global Infectious Disease Analysis at Imperial and senior author on the paper, said: “Our analysis finds that in England, the early switch to a 12-week vaccine dose interval saved thousands of lives and prevented tens of thousands of hospitalisations from COVID-19, highlighting the benefits of being able to react swiftly as new data become available. This study demonstrates the value of mathematical models, calibrated to detailed epidemic data, to investigate control options not only prospectively, as our team has done continuously since early 2020, but also retrospectively.”
"The early switch to a 12-week vaccine dose interval saved thousands of lives and prevented tens of thousands of hospitalisations from COVID-19" Dr Anne Cori MRC Centre for Global Infectious Disease Analysis
The UK government began the rollout of COVID-19 vaccines in December 2020, with the initial guidance to administer the first and second doses three weeks apart in line with clinical trial protocols.
Following real-world evidence that a single dose of vaccine was effective and the emergence of the more transmissible Alpha variant over the 2020/21 winter, the policy was changed,[1] increasing the interval between doses to up to 12 weeks – delaying the second dose for most people in order to offer partial vaccine-induced protection to a greater number of people as quickly as possible.
Using a previously established model, the researchers used available data from the Department of Health and Social Care[2] to estimate the transmission rates and model infections, hospital admissions and deaths in the population in England from the start of the vaccine rollout to just before the start of the booster campaign (8th December 2020 to 13th September 2021).
They estimate that following the original three-week interval strategy would have resulted in more hospital admissions and deaths compared to the 12-week strategy. Under the three-week strategy, there was a higher number of daily hospitalisations, peaking at an estimated 2,030 people hospitalised with COVID-19 on 22nd July 2021. Over the entire study period, the three-week strategy resulted in an estimated cumulative 291,000 hospitalisations and 64,800 deaths from COVID-19, compared to 233,000 hospitalisations and 54,700 deaths under the 12-week strategy.[3]
Adapting guidelines
According to the team, the findings highlight the benefit in carefully considering and adapting guidelines in light of new emerging evidence. However, they caution that the results are specific to England, and the analysis includes a number of assumptions which limit the findings. For example, the model assumes a simplified pattern of waning immunity, as well as assuming that social mixing remained similar under both the three- and 12-week strategies. It also does not take into account the emergence of other variants of concern than those seen in England.
The analysis also highlights how mathematical modelling can provide important insights into strategies to limit epidemic spread despite multiple uncertainties e.g. regarding vaccine effectiveness and waning immunity over time. The team investigated many scenarios to explore such uncertainty and found that the 12-week strategy resulted in fewer hospitalisations and deaths across all scenarios.
Dr Natsuko Imai, an Honorary Senior Research Fellow within the MRC Centre for Global Infectious Disease Analysis, and joint first author on the paper, said: “For the public, it can be confusing when policy seems to change frequently. But analyses like ours show the importance of being able to adapt health guidance when informed by new evidence and that continuous surveillance and reassessment is crucial to making informed decisions during health crises.
"Studies like this one we’ve conducted help to inform future pandemic preparedness strategies...they provide greater evidence for future vaccine delivery decision making" Dr Thomas Rawson Jameel Institute
“Most people will be familiar with modelling as a ‘what if’ tool and understand it can’t predict outcomes, but models can help to guide future decisions based on a range of possible scenarios. This study highlights how modelling can also be a valuable retrospective tool, enabling us to review previous data and trends. Overall, our findings reinforce the need for early data collection, analysis, and constant re-evaluation.”
Dr Thomas Rawson, based within the Jameel Institute at Imperial and joint first author of the paper, said: “This retrospective analysis is based on previous models used to simulate COVID-19 scenarios during the pandemic, but now looking backwards rather than forwards. These significant policy decisions have to be made in the face of considerable unknown factors – ‘what new variants will emerge?’, ‘How long will vaccine effectiveness hold up?’. Studies like this one we’ve conducted help to inform future pandemic preparedness strategies by investigating how these vaccination schedules shaped the real-world pandemic trajectory in England. They provide greater evidence for future vaccine delivery decision making.”
The research was funded by the National Institute for Health and Care Research (NIHR), the UKRI Medical Research Council, Jameel Institute, Wellcome Trust and the UK Foreign, Commonwealth and Development Office (FCDO).
-
‘Quantifying the impact of delaying the second COVID-19 vaccine dose in England: a mathematical modelling study’ by Imai N, Rawson T, Knock ES, et al. is published in The Lancet Public Health. DOI: 10.1016/S2468-2667(22)00337-1
[1] The JCVI guidelines were amended on 30th December 2020, with the UK’s chief medical officers agreeing: “prioritising the first doses of vaccine for as many people as possible on the priority list will protect the greatest number of at risk people overall in the shortest possible time and will have the greatest impact on reducing mortality, severe disease and hospitalisations and in protecting the NHS and equivalent health services.”
https://www.gov.uk/government/news/statement-from-the-uk-chief-medical-officers-on-the-prioritisation-of-first-doses-of-covid-19-vaccines
[2] The analysis used data from numerous sources including the National Health Service (NHS), Department of Health and Social Care (DHSC), UK Health Security Agency (UKHSA) and the Real-time Assessment of Community Transmission (REACT) study. Vaccine effectiveness was modelled on the AstraZeneca and Pfizer vaccines, assuming Moderna mRNA vaccine had the same vaccine effectiveness as Pfizer mRNA vaccine.
[3] Estimated number of people hospitalised daily with COVID-19 on 22nd July 2021 peaked at 2,030 (95% credible interval, CrI: 1,690–2,360). The three-week strategy resulted in an estimated cumulative 291,000 hospitalisations (95% CrI: 275,000–319,000) and 64,800 deaths (95% CrI: 60,200–68,900) from COVID-19, compared to 233,000 hospitalisations (95% CrI: 229,000–238,000) and 54,700 deaths (95% CrI: 52,800–55,600) under the 12-week strategy.
Article supporters
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Ryan O'Hare
Communications Division