Why radar for health monitoring?
The increasing prevalence of neurodegenerative and chronic conditions, together with growing pressure on clinical services, has created a clear need for continuous, objective, and unobtrusive health monitoring beyond the clinic. Existing approaches such as wearable sensors, camera-based systems, and laboratory-based technologies face important limitations related to user burden, privacy, and scalability, particularly for long-term monitoring in real-world environments. These challenges are especially pronounced for older adults and individuals with cognitive or motor impairments, for whom sustained adherence, correct device use, and frequent clinical visits can be difficult. Radar sensing addresses these limitations by enabling contactless and privacy-preserving monitoring of movement, physiology, and sleep without requiring physical contact or active user engagement. By operating continuously and unobtrusively within everyday environments, radar allows clinically relevant changes, such as gradual movement deterioration or altered vital sign patterns, to be observed over time across daily routines, rather than during short, task-based assessments. This creates opportunities for earlier intervention and more informed clinical decision-making.
Within the NGNI Lab, our radar research is driven by a human-centred design philosophy. We focus on developing sensing systems that deliver clinically meaningful health metrics, are deployable in real environments, and are rigorously validated against established gold-standard measurements. Much of this work is conducted in close collaboration with the UK Dementia Research Institute Care Research & Technology Centre, where our team forms the Bioelectronic Systems Group, with a strong emphasis on ageing, neurodegeneration, and long-term care.
Radar Hardware Platforms
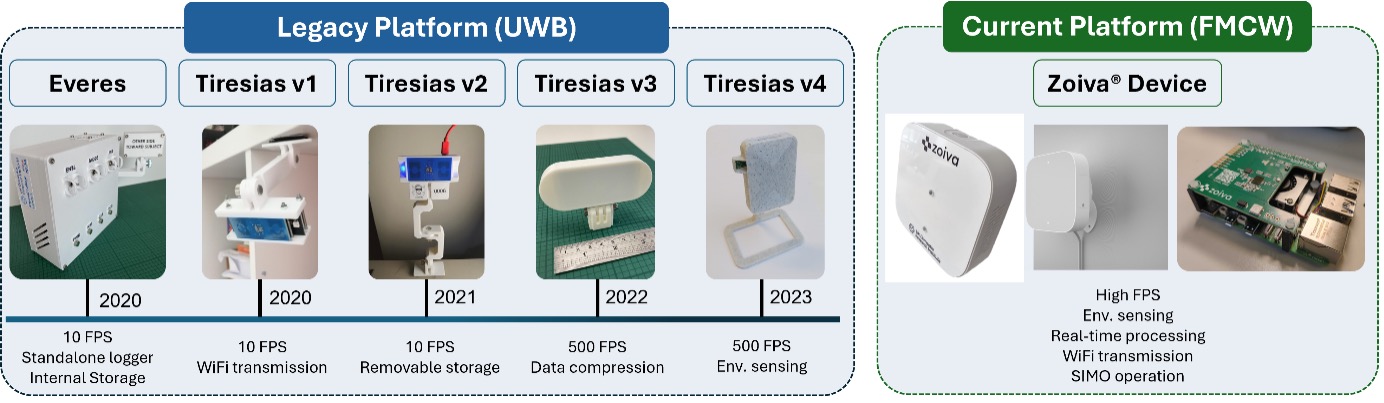
Our research spans multiple radar modalities, allowing us to explore trade-offs between resolution, coverage, cost, and deployability. We work with:
- Ultra-wideband (UWB) impulse radar for high-resolution physiological and motion sensing
- FMCW radar systems for compact, low-power continuous monitoring
- Networked radar platforms for multi-sensor indoor coverage
These platforms are used both in controlled laboratory validation studies and in real-world home deployments.
Signal Processing and Data-Driven Algorithms
A core focus of our research is the development of robust signal processing and machine-learning methods that transform raw radar measurements into clinically interpretable biomarkers. Our approach combines physics-informed radar processing with statistical and data-driven modelling, enabling reliable operation in cluttered indoor environments and across diverse real-world conditions.
Our methods extract clinically meaningful features such as respiration dynamics, gait timing parameters, movement variability, and sleep-related patterns directly from radar signals.
Current Validated Radar Capabilities
Physiological Monitoring
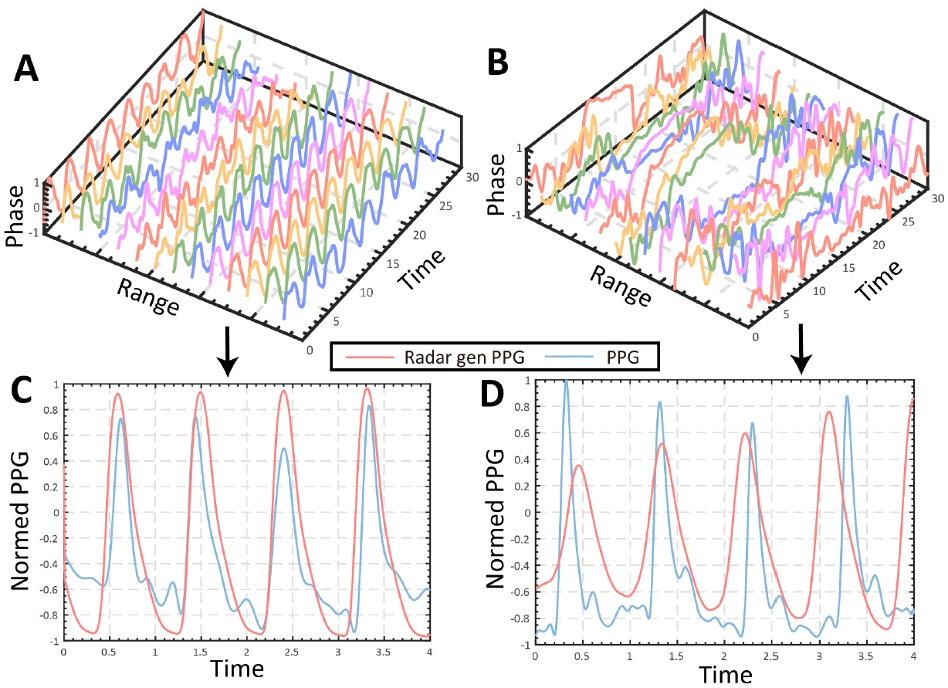
Our work demonstrates that radar can be used for contactless monitoring of respiration and cardiac-related micro-motions during rest and sleep. Using ultra-wideband radar, respiration rate, breathing patterns, and variability have been validated against reference sensors in both laboratory and real-world settings. In addition, we have demonstrated the reconstruction of photoplethysmography (PPG)-like signals from radar micro-motion, enabling contactless extraction of cardiac dynamics and forming the basis for continuous physiological monitoring without wearables.
Activity and Mobility Monitoring
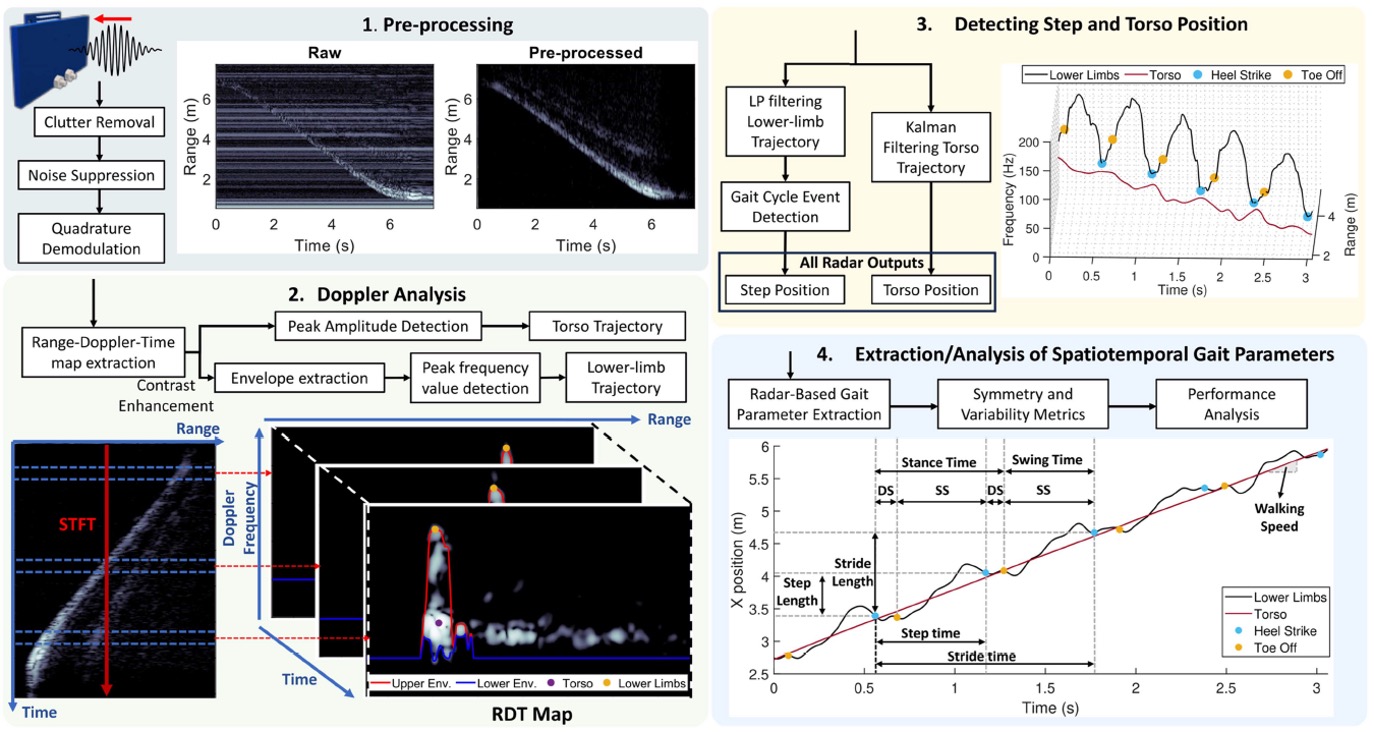
Radar-based activity and mobility monitoring has been validated across localisation, presence detection, and overground gait analysis. Using joint range–Doppler–time representations of radar data, we have shown that spatiotemporal gait parameters can be extracted reliably during natural and asymmetric walking, with performance benchmarked against motion capture systems. Complementary work on radar micro-Doppler signatures further demonstrates the feasibility of person identification and activity differentiation using motion patterns.
Sleep Monitoring
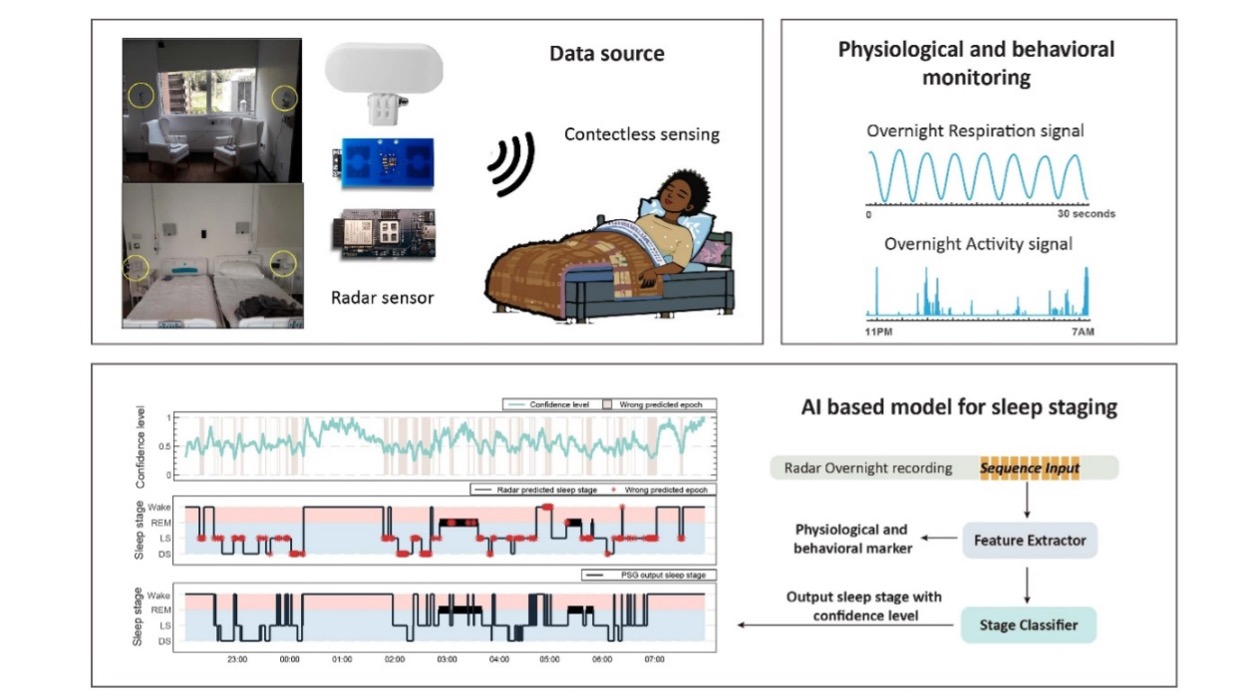
Our sleep research shows that radar can be used to assess sleep and nocturnal physiology unobtrusively in older adults and people living with cognitive impairment. By combining radar-derived motion and respiration features with machine-learning models trained using clinically annotated polysomnography data, we demonstrate the feasibility of sleep staging and detection of abnormal breathing patterns in settings where traditional sleep studies are impractical.
Real-Time and Deployable Systems
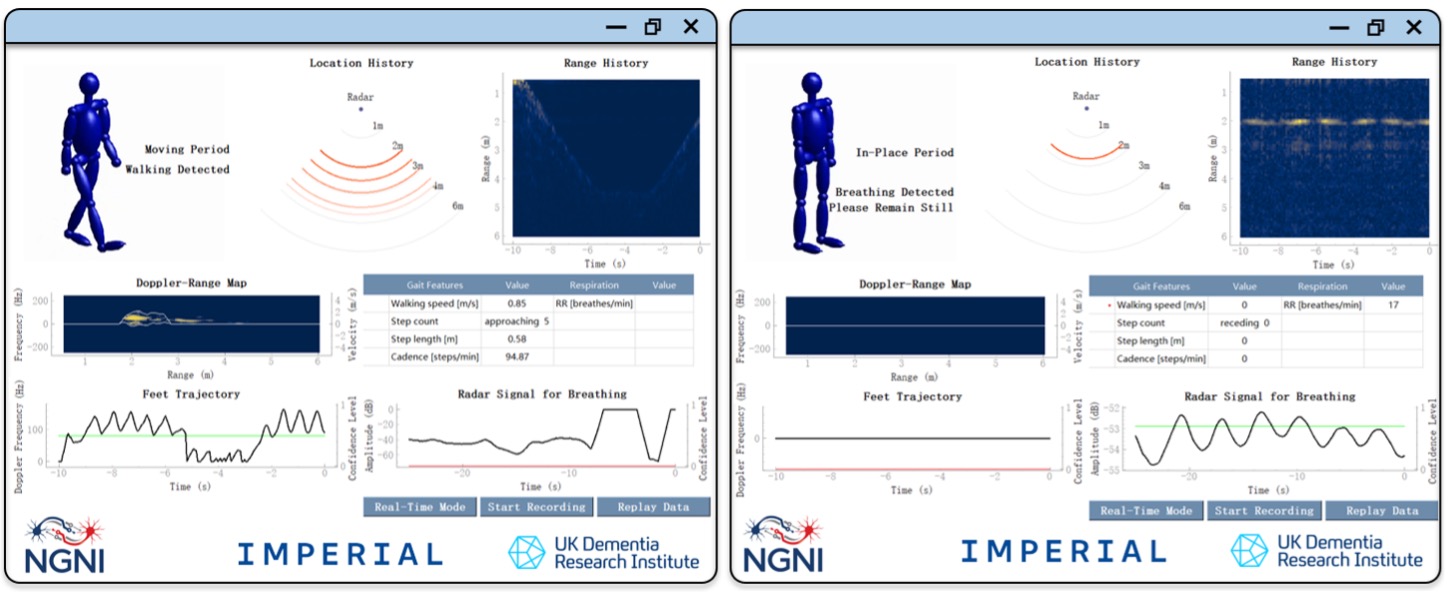
Beyond offline analysis, we have developed and demonstrated real-time radar systems capable of simultaneous gait and respiration monitoring. Live demonstrations and networked radar platforms show that these capabilities can operate continuously at high frame rates and low cost, supporting realistic indoor deployment and paving the way towards scalable health monitoring solutions.
Emerging Capabilities
Building on these validated foundations, we are actively investigating next-generation radar-derived biomarkers and automated assessments. Ongoing work includes contactless estimation of cardiovascular metrics (e.g. blood pressure), human activity recognition in free-living environments, and automated functional assessments such as components of the Short Physical Performance Battery. Disease-specific applications under investigation include tremor and gait freezing detection in Parkinson’s disease, gait balance and stability metrics, and longitudinal analysis of sleep–wake patterns and sleep disorders in neurodegenerative conditions. In addition, we are exploring the potential for early detection and monitoring of infections in people living with dementia, through subtle changes in physiological signals and daily behavioural patterns.
From Research to Real-World Impact
The long-term impact of radar sensing lies in its ability to deliver continuous, objective health information in home environments and care facilities with minimal burden on individuals. Translation and commercialisation are therefore essential steps to move beyond research prototypes towards scalable deployment, improved system reliability, and eventual integration into care pathways. To support this transition, we have secured intellectual property through international patent filings and are actively developing deployable radar systems designed for real-world use. This ongoing work focuses on creating robust, clinically interpretable systems that can operate as part of broader digital health ecosystems, supporting multi-modal sensing, clinical validation, and future regulatory pathways.
If successfully translated, these systems have the potential to provide individuals and their carers with timely insight of their health status, supporting reassurance, and informed decision-making outside the clinic. At a healthcare system level, radar-based monitoring could enable more proactive and personalised care, support longitudinal assessment of medication or treatments in natural environments, and contribute to more efficient use of clinical resources, particularly for people living with neurological and age-related conditions.
Publications
[1] M. Yin et al., “Motion-Robust Heartbeat Reconstruction from Radar Signals via Transfer Learning,” accepted for publication in Proc. IEEE Radar Conf. (RadarConf), Phoenix, AZ, USA, May 2026.
[2] M. Yin et al., “Using legacy polysomnography data to train a radar system to quantify sleep in older adults and people living with dementia,” arXiv preprint arXiv:2601.04057, 2026.
[3] H. Tu et al., “Multi-Person Sleep Monitoring Using UltraWideband Radar and Deep Learning,” under review for Proc. IEEE Eng. Med. Biol. Soc. (EMBC), 2026.
[4] C. Hadjipanayi et al., “Towards radar-agnostic gait analysis across UWB and FMCW systems,” arXiv preprint arXiv:2601.04415, 2026.
[5] J. J. Yun et al., “Passive Sensing of Gait and Medication-related Fluctuations in Parkinson's Disease,” medRxiv preprint, 2025, doi: 10.1101/2025.11.12.25340068.
[6] M. Yin et al., “Unobtrusive sleep health assessment using impulse radar: A pilot study in older people,” IEEE Trans. Biomed. Eng., 2025.
[7] A. Bannon et al., “Enabling low-cost ultra-high-framerate WiFi-networked UWB radar systems for indoor monitoring of physiology and activity,” in Proc. IEEE Int. Radar Conf. (RADAR), Atlanta, GA, USA, 2025.
[8] C. Hadjipanayi et al., “Remote gait analysis using ultra-wideband radar technology based on joint range–Doppler–time representation,” IEEE Trans. Biomed. Eng., 2024.
[9] C. Hadjipanayi et al., “Capturing gait parameters during asymmetric overground walking using ultra-wideband radars: A preliminary study,” in Proc. 46th Annu. Int. Conf. IEEE Eng. Med. Biol. Soc. (EMBC), Orlando, FL, USA, 2024.
[10] Z. Chen et al., “Live demonstration: Real-time gait and respiration analysis using ultra-wideband radar,” in Proc. IEEE Biomed. Circuits Syst. Conf. (BioCAS), Xi’an, China, 2024.
[11] M. Yin et al., “Identification of human gait using UWB radar micro-Doppler measurement,” in Proc. IEEE Eng. Med. Biol. Soc. (EMBC), 2024.
[12] T. Lauteslager et al., “Dynamic microwave imaging of the cardiovascular system using ultra-wideband radar-on-chip devices,” IEEE Trans. Biomed. Eng., vol. 69, no. 9, pp. 2935–2946, 2022.
[13] Z. Chen et al., “Towards robust, unobtrusive sensing of respiration using UWB impulse radar for the care of people living with dementia,” in Proc. 10th Int. IEEE/EMBS Conf. Neural Eng. (NER), Italy, 2021.
[14] A. Bannon et al., “Tiresias: A low-cost networked UWB radar system for in-home monitoring of dementia patients,” in Proc. 43rd Annu. Int. Conf. IEEE Eng. Med. Biol. Soc. (EMBC), Mexico, 2021.
[15] Y. Han, T. Lauteslager, T. S. Lande, and T. G. Constandinou, “UWB radar for non-contact heart rate variability monitoring and mental state classification,” in Proc. 41st Annu. Int. Conf. IEEE Eng. Med. Biol. Soc. (EMBC), 2019.
[16] T. Lauteslager, M. Tømmer, T. S. Lande, and T. G. Constandinou, “Coherent UWB radar-on-chip for in-body measurement of cardiovascular dynamics,” IEEE Trans. Biomed. Circuits Syst., vol. 13, no. 5, pp. 814–824, 2019.