Robotic rectum may aid prostate cancer diagnosis
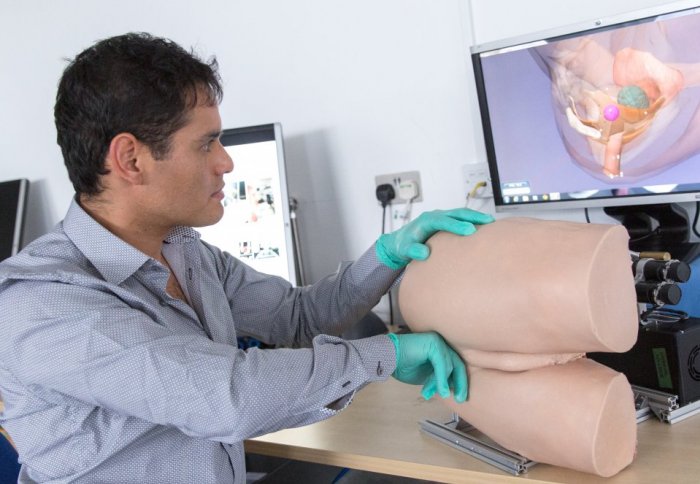
Dr Alejandro Granados demonstrates the robotic rectum technology
A robotic rectum may help doctors and nurses detect prostate cancer.
The technology, which consists of prosthetic buttocks and rectum with in-built robotic technology, has been developed by scientists at Imperial College London.
The idea is the device helps train doctors and nurses to perform rectal examinations by accurately recreating the feel of a rectum, as well as providing feedback on their examination technique. The device contains small robotic arms that apply pressure to the silicone rectum, to recreate the shape and feel of the back passage.
The technology, which is being presented at the Eurohaptics conference this week at Imperial, is now being adapted for gynaecological exams.
Rectal examinations are necessary to diagnose conditions such as prostate cancer and involve a medic placing their index finger into the anus, and feeling the prostate gland.
The walnut-size gland sits below a man’s bladder, and can be felt just inside the anus, through the rectal wall. Around one in eight men in the UK suffer from prostate cancer at some point in their lives. Furthermore, 75 per cent of men over 70 suffer from benign prostate enlargement, which although harmless can cause urinary problems.
A rectal examination is often the first test a doctor or nurse uses to recognise a problem prostate. This determines whether they send a patient for further tests.
Generally, cancerous prostates tend to feel hard and knobbly, but learning exactly what a potentially cancerous prostate feels like can be difficult, explains Dr Fernando Bello, from the Department of Surgery and Cancer at Imperial College London: "Internal examinations are really challenging to learn - and to teach. Because the examinations occur in the body, the trainer cannot see what the trainee is doing, and vice versa. In addition to this, medics rarely get the chance to practise the examination, as few patients would volunteer as practice subjects. In fact there is only one person registered in the country as a test subject, called a Rectal Teaching Assistant (RTA) in the UK.
“But the results of these examinations can have major implications for patients - they are very important for early diagnosis of various conditions such as prostate cancer."
Although plastic models exist to help train medical staff, these do not feel like living flesh and tissue, added Dr Bello. Therefore to help doctors and nurses practice how to perform these examinations - and to avoid patient discomfort as much as possible, Dr Bello and his team have created a robotic 'trainer rectum'.
When using the trainer, a doctor inserts his finger inside a silicone thimble attached to robotic technology able to recreate the exact sensation of the human rectum.

Dr Alejandro Granados with the robotic rectum technology
Furthermore, a computer screen behind the device can display a 3D model of the rectum and prostate, allowing the doctor, with the aid of 3D glasses, to see the anatomy while they perform the examination. The technology can be programmed for different scenarios, allowing the anatomy to be changed each time, explained Dr Alejandro Granados, also from the Department of Surgery and Cancer at Imperial and who is leading the development of the robotic rectum.
"We scanned a number of volunteers with an MRI scan and used this to perfect the shape and geometry of the anatomy."
He added: "We have already asked a number of doctors and nurses – including prostate specialists and cancer surgeons - to trial the technology. They commented on the great advantage of being able to alter the anatomy. The size and shape of the rectum and prostate can vary greatly from person to person, and this technology enables medics to practice their skills in many different virtual patients. They also observed that because these examinations are performed solely by feel, experiencing a realistic sensation is crucial.
Furthermore, the team are continuing to perfect the device, by collecting data from real prostate examinations in patients.
Dr Bello explained: "There is very little research into the exact pressure and trajectory a doctor needs to use for a successful prostate exam. Therefore we are asking doctors to wear a small pressure sensor on their fingertip, underneath their surgical glove, when they are examining real patients.
There is very little research into the exact pressure and trajectory a doctor needs to use for a successful prostate exam.
– Dr Fernando Bello
Department of Surgery and Cancer
Funded by the EPSRC, the team are now working towards building an affordable prototype for medical schools. Although each device may cost over £10,000, the team say a more affordable option may be to use the finger pressure sensors and 3D software on traditional plastic models, to enhance existing training facilities.
The device is being presented this week at the international Eurohaptics conference at Imperial, taking place 4-7 July.
Dr Bello added: “Haptics is one of the most exciting technology areas at the moment, and investigates the sensation of touch and how to integrate this into electronic devices. It has huge implications for the field of medicine and beyond. For instance, virtual reality technology is evolving at a rapid rate, but haptics is also crucially important – otherwise what is the point of immersing yourself in a virtual role if you can’t feel and interact with it.”
He commented that, although other high-tech prosthetic rectums have been developed, none have incorporated complex haptic technology, and allowed such detailed feedback to the medic performing the examination. “Previous models have had a few pressure sensors placed inside a model rectum, but none have provided the type of 3D modelling and detailed touch feedback available with this technology.”
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Thomas Angus [Photographer]
Communications Division
Martin Sayers
Communications Division
Kate Wighton
Communications Division