Imperial takes the fight to cancer in 2018

This year, researchers at Imperial made several important breakthroughs in understanding and potentially treating aggressive cancer types.
The past few decades have seen remarkable progress in the survival rates of some cancers – particularly in the developed world, and particularly for cancers of the breast, prostate, lung and bowel.
For example, in the US, breast cancer death rates declined 39% from 1989 to 2015 – with five year survival rates now at around 90% (85% in Western Europe).
Indeed, this year’s Nobel Prize winner in physiology or medicine, Tasuku Honjo, recently said that he believes most cancers will become treatable with immune therapy by 2050.
However, the reality is that for certain cancers such as pancreatic, liver and some lung cancers, survival rates have remained stubbornly low in both rich and developing countries and new effective treatments have not been forthcoming. Five year survival rates for pancreatic cancer have remained typically under 15%.
Yet there is hope on the horizon. Researchers around the world are slowly beginning to understand the complex mechanisms by which certain tumours spread or evade treatment. That has been a strong theme at Imperial this year and so we’ve rounded up four exciting studies looking at the mechanisms of cancer growth and spread in four different cancer subtypes.
Breaking the mould in liver cancer
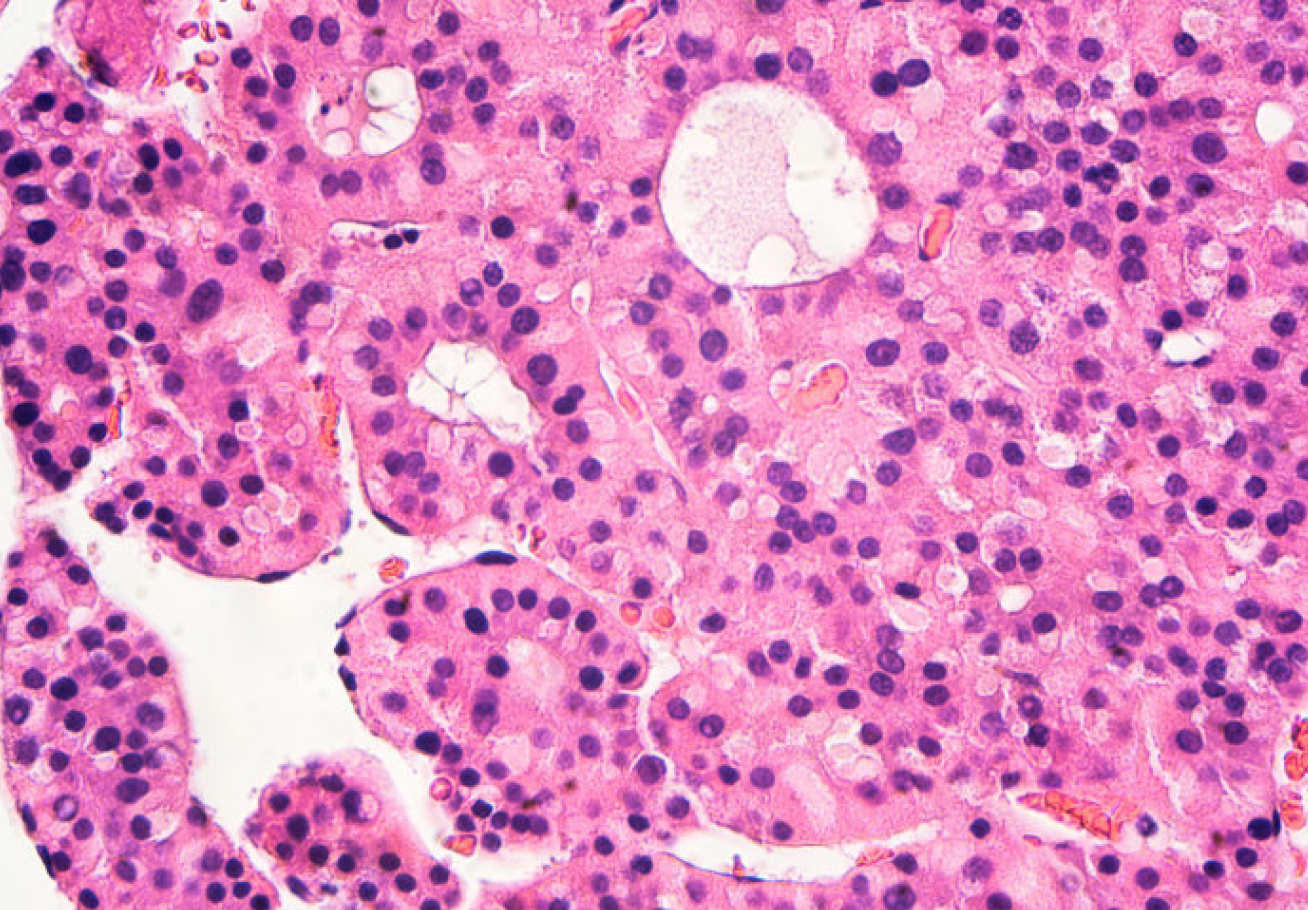
Under certain biological conditions, such as specific patterns of gene expression or a lowered immune system, cancer cells can migrate or ‘metastasise’ and invade other tissues, which spreads the cancer. Once cancer spreads to secondary sites in the body, it is much harder to treat. Cells’ inner structures, known as cytoskeletons, produce the forces that lead to cell migration in cancer cells. Looking at hepatocellular carcinoma (HCC) – the most common type of liver cancer – researchers in Imperial’s Department of Bioengineering uncovered the molecular mechanisms that drive cancer migration. Key to that pathway were two proteins – ‘deleted in liver cancer-1’ (DLC1), a tumour suppressor, and talin. The talin protein attaches to the cell membrane and creates a bridge between the outside and inside of the cell. It is coiled like a spring so that it can sense and respond to mechanical forces. These forces change the shape of talin, which deactivates DLC1 so that it cannot perform its tumour suppressing function. The researchers say their findings have implications for tissue engineering, cancer research, and drug testing using organ-on-chip technology.
Routing out ‘rabble rousers’ in pancreatic cancer
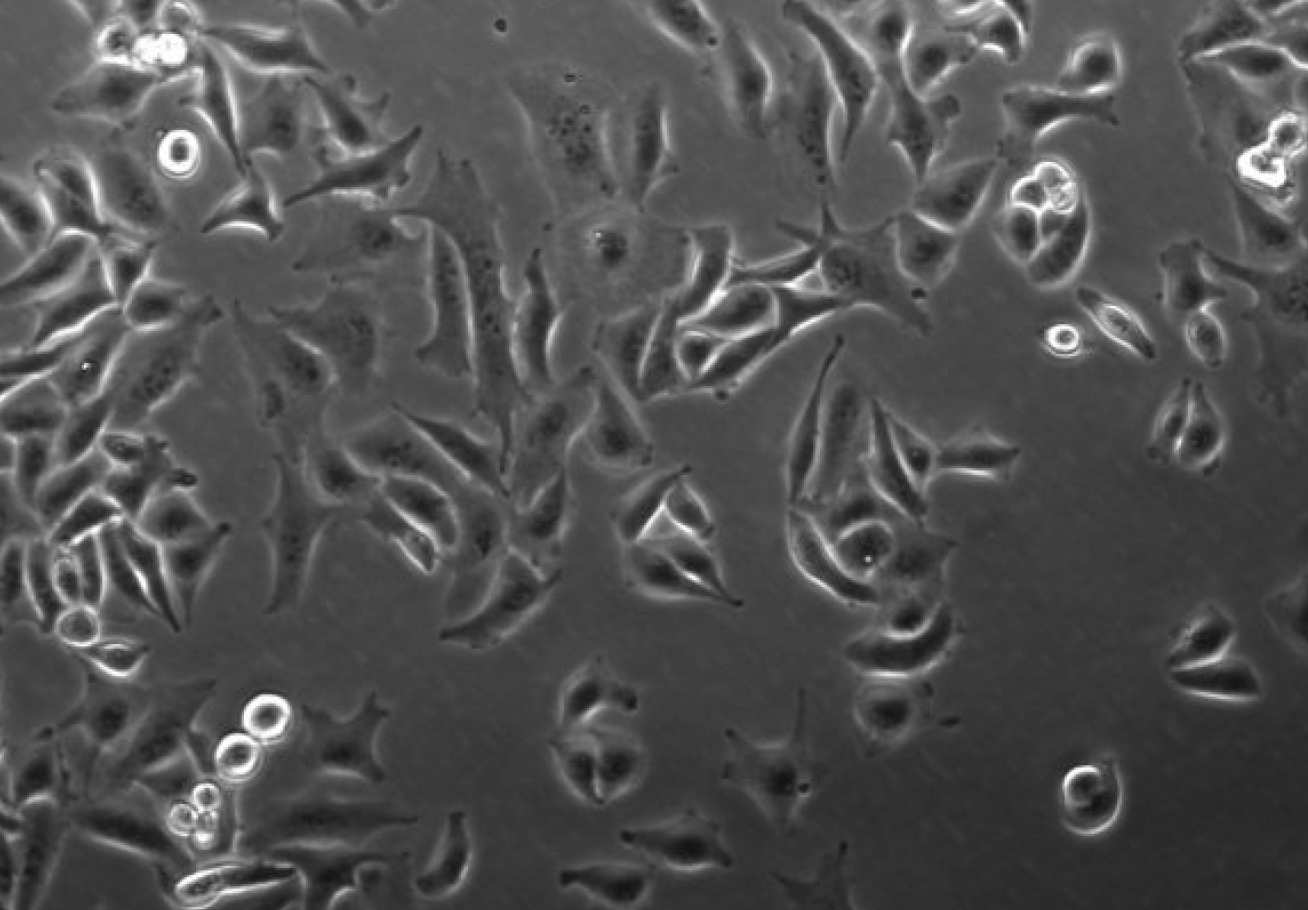
Another team at Imperial, from the Department of Surgery and Cancer, discovered a very different molecular driver of metastatic spread – this time in pancreatic cancer. MicroRNAs are short chains of nucleotides (similar in structure to DNA, but much shorter) which help control which genes are switched on and off in a cell. The researchers discovered that two microRNAs called miR-100 and miR-125b, work together with a molecule called Transforming Growth Factor Beta (TGF-b) to promote growth and spread of pancreatic cancer. They say that these molecules act like the ‘rabble-rousers’ in tumour cells – they drive a number of processes that cause cancer cells to become aggressive, and more likely to invade other areas of the body. The team are now planning further investigations on these two microRNAs, to find out if stopping the production of these molecules will slow pancreatic cancer growth, or make the cancer cells easier to kill with chemotherapy.
Hiding in plain sight in breast cancer
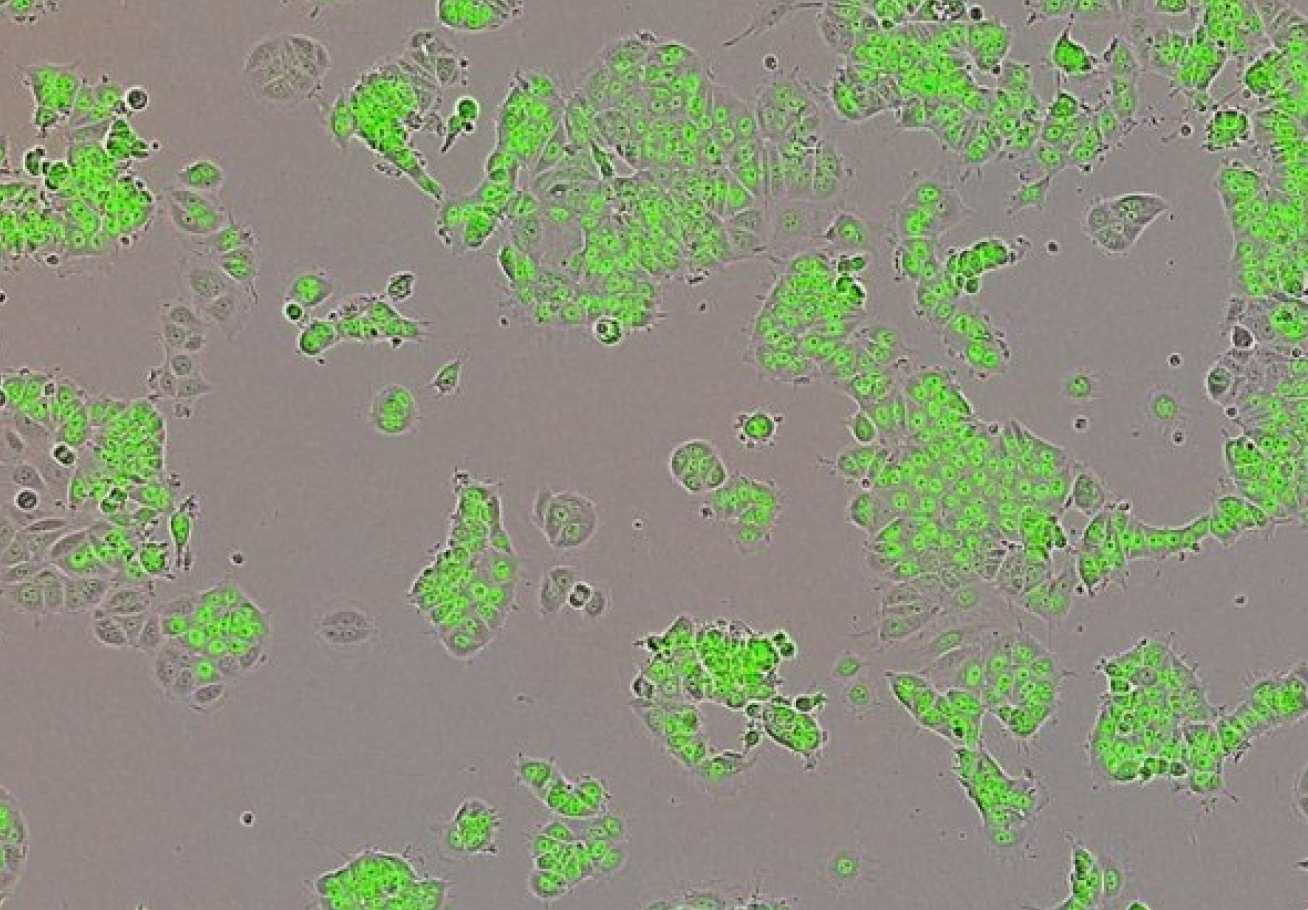
While great progress has been made in treating breast cancers, some tumours can become resistant to chemotherapy. A group of international scientists led by Imperial has now shown how tumours can change their ‘appearance’ to adapt to their environment, evade treatment and ultimately survive longer using a system called epigenetics. Yin Yang1 is a type of molecule called a transcription factor which can help activate genes. Although each cell contains around 25,000 genes, only a certain number are switched on at one time, depending on what functions the cell needs to perform. The team of scientists completed in-depth genetic profiling of breast tumours from 37 patients, using a variety of different techniques, including the gene editing technique CRISPR. The results revealed that cancer cells are much more reliant on Yin Yang1 than normal cells, and that it may drive breast cancer growth.
New weapons against brain cancers

This year brought a glimpse of an entirely new way to treat aggressive brain and lung cancers – using viruses. Human adenoviruses (HAdVs) are common microorganisms which can cause eye infections as well as respiratory and gastrointestinal infections in humans and animals. The HAdV-52 virus subtype binds to a specific type of sugar on the surface of cells, called polysialic acid. Polysialic acid is typically found in the developing brain, however, previous studies have shown that the sugar is also present in a number of cancer tissue samples. In these studies it was also frequently associated with tumours that are highly aggressive and fail to respond to traditional treatments, resulting in poor prognosis for the patient. Now a team of Imperial researchers have elucidated the mechanism by which the viruses use a protein to tether themselves to the surface of the host cell. According to the team, the discovery opens up new opportunities for the development of virus-based cancer therapies, which could potentially use this adenovirus to target and kill cancerous cells.
Further reading
For a wider selection of cancer news stories from Imperial in 2018, see the links below :
- Breast cancer drug could create chink in the armour of pancreatic cancer
- New class of drugs could help tackle treatment-resistant cancers
- Ovarian cancer genetics unravelled
- Breakthrough drug shows early promise for multiple myeloma
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Andrew Czyzewski
Communications Division