Head injury effects halted by xenon gas, finds first ever lifelong study in mice
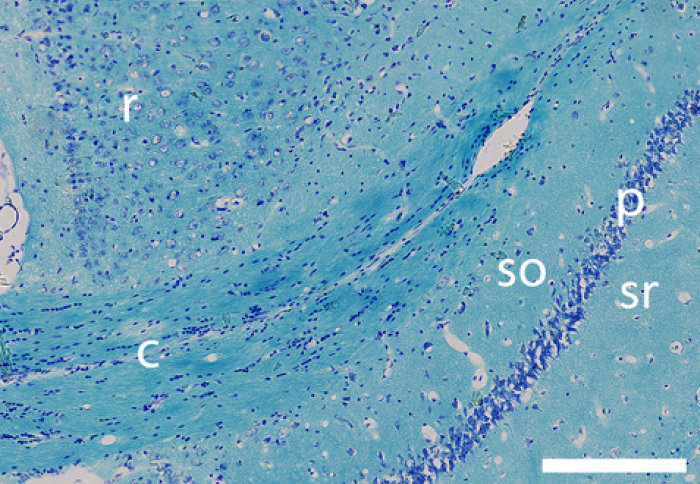
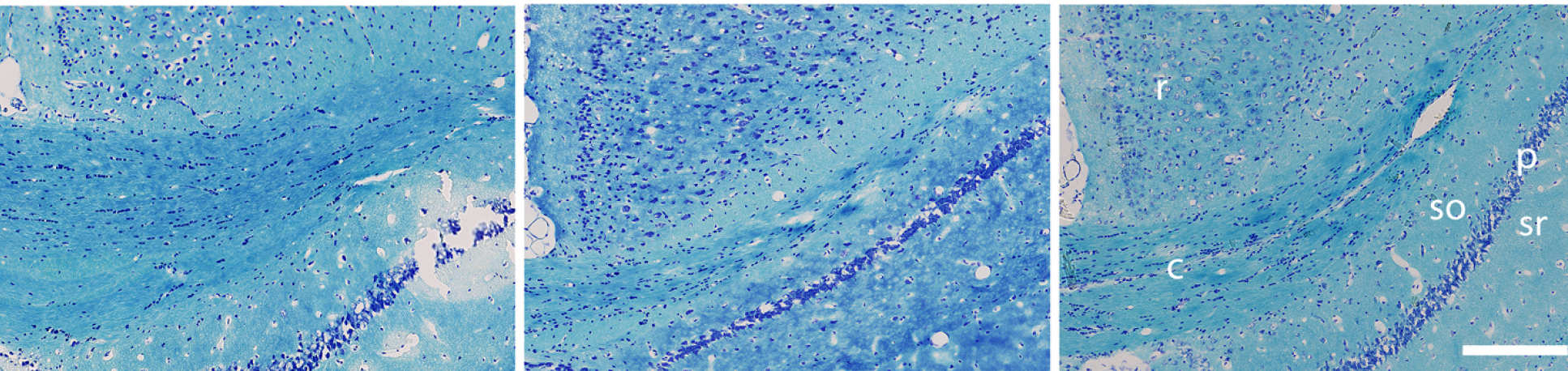
Xenon treatment prevented long-term degeneration of nerve fibres in the corpus callosum
Following traumatic brain injury (TBI), xenon prevented early death, improved long-term cognition, and protected brain tissue in mice in a new study.
TBI is the leading cause of death and disability in people under 45 in developed countries. The primary injury, caused by the initial force from a fall or car accident for example, is followed by a secondary injury which develops in the minutes, hours and days afterwards.
This secondary injury is largely responsible for the mental and physical disabilities associated with TBI – but there are currently no specific drug treatments that can be given after the trauma to stop it from developing.
TBI patients who survive the injury have a reduced life expectancy and an increased risk of developing Alzheimer’s disease or other dementias later in life.
Now, researchers from Imperial College London and Johannes Gutenberg University Mainz have found that the anaesthetic drug xenon, given shortly after a TBI, prevents early death and long-term cognitive impairment and protects brain tissue itself in mice. The xenon-treated mice had a similar life expectancy, cognitive function, and brain tissue integrity, to mice that had never sustained a TBI.
Although xenon has not yet been tested for TBI in humans, our findings add to the growing body of evidence that suggests it could be used after head injuries to prevent secondary injury developing. Dr Rita Campos-Pires Department of Surgery & Cancer
Previously, the same team led by Dr Robert Dickinson and colleagues at Imperial’s Department of Surgery & Cancer, showed xenon limited early brain damage and improved long-term motor function in mice with TBI. However, they had yet to look at xenon’s effect on life expectancy, long-term cognitive function and brain tissue degeneration after TBI.
This new study, published in the British Journal of Anaesthesia, looked at the effects of xenon over the whole lifespan of mice for the first time.
Animals were randomly allocated to one of three groups: TBI xenon, TBI control, and healthy control. Under general anaesthesia, and with long-acting pain relief, a controlled mechanical force was applied to the brains of the TBI control and TBI xenon groups. The healthy control group was given anaesthesia, but did not receive a TBI. The researchers gave xenon gas to one of these groups (TBI xenon group), while the other two received control gas for the same amount of time.
All three groups then underwent learning and memory tests at two weeks and 20 months after injury. The researchers also recorded their time of death and examined their brain tissues.
They found that:
- The TBI xenon group had the same life expectancy as the healthy control group which had not suffered a TBI.
- The TBI control group developed late-onset cognitive damage. Xenon treatment shortly after TBI appeared to prevent this.
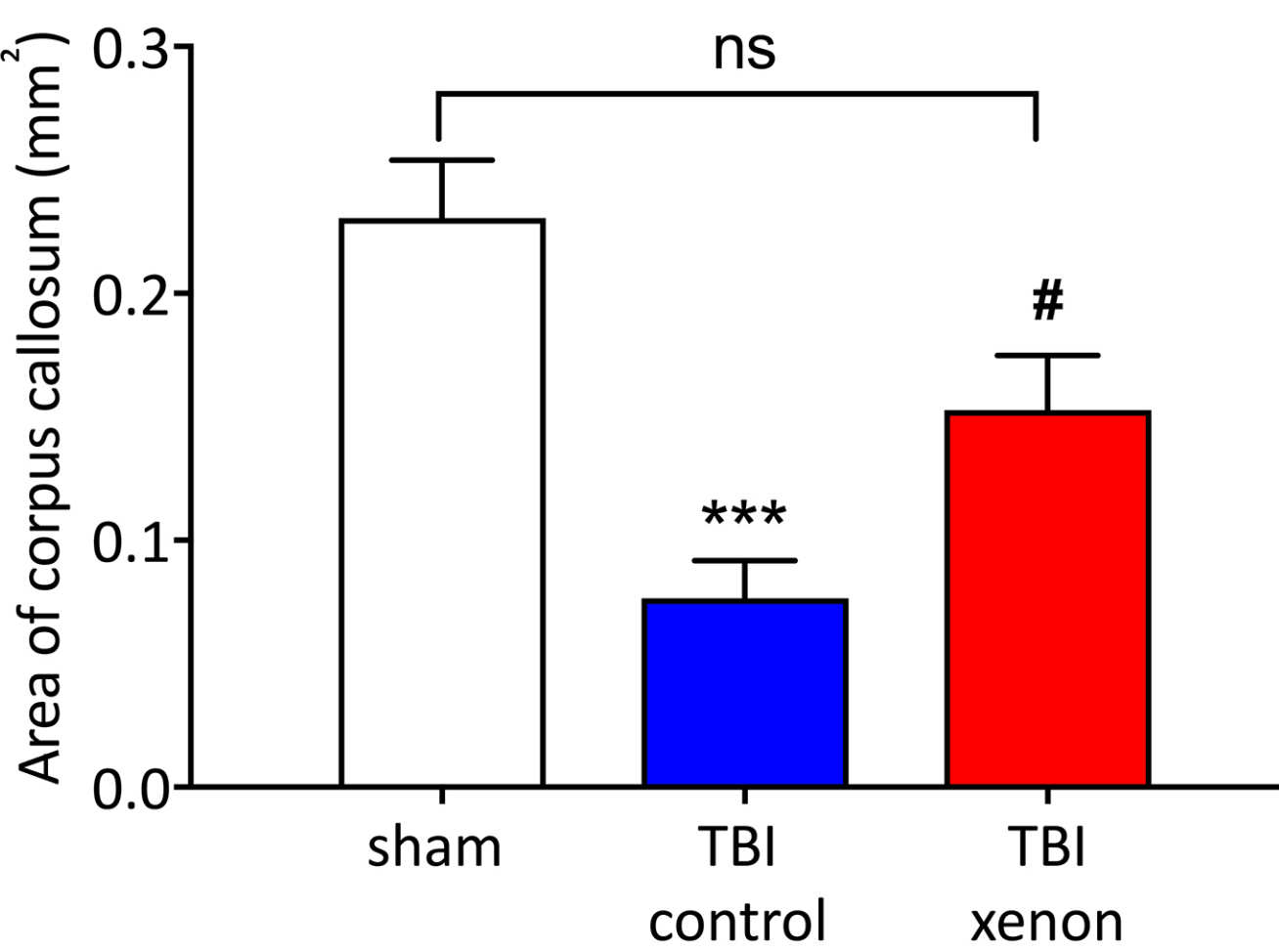
- Key brain areas involved in cognitive functioning were damaged in control TBI group. Xenon-treatment prevented or significantly reduced this damage.
There is currently a huge gap in what treatment we can offer to patients who’ve suffered TBI – an injury which can impact all areas of their lives. Dr Rita Campos-Pires Department of Surgery & Cancer
Xenon prevented the loss of brain cells in the hippocampus (an area of the brain associated with learning and memory), and prevented degeneration of nerve fibres in the corpus callosum (which connects the two brain hemispheres) that may explain the improvement in cognitive function.
Xenon was also shown to reduce long-term brain inflammation that is believed to be involved in cognitive impairment in Alzheimer’s Disease and other dementias.
We have looked at very long-term outcomes, up to 20 months after TBI in mice. This is very rarely done in animal studies and is equivalent to following up human TBI patients until their 80s. Dr Robert Dickinson Department of Surgery & Cancer
According to the group, the findings are important as they could offer insight into new treatments for patients with TBI. Patients with TBI early in life are eight times more likely to die early than people without and are more likely to develop Alzheimer’s Disease and other types of dementia later on. There is currently no specific drug treatment available for people who suffer a TBI – instead, the treatment is supportive and rehabilitative.
Lead author of the study, Dr Rita Campos-Pires, from the Department of Surgery & Cancer, said: “There is currently a huge gap in what treatment we can offer to patients who’ve suffered TBI – an injury which can impact all areas of their lives.
“Although xenon has not yet been tested for TBI in humans, our findings add to the growing body of evidence that suggests it could be used after head injuries to prevent secondary injury developing.
“Xenon appears to act in a variety of ways, but one of the most likely
mechanisms to explain its protective effects on brain tissue is by inhibiting receptors in the brain known as NMDA receptors, that become over-activated following a brain injury.”
Dr Dickinson added: “We have looked at very long-term outcomes, up to 20 months after TBI in mice. This is very rarely done in animal studies and is equivalent to following up human TBI patients until their 80s. The finding that only a short treatment with xenon can have beneficial effects on cognition, survival, and brain damage almost two years later suggests that xenon might in future prevent cognitive decline and improve survival in human TBI patients.”
Xenon is already used as a human general anaesthetic, is known to have few side effects and could be easily given via inhalation or to mechanically ventilated TBI patients in the intensive care unit.
Given xenon’s safety profile – and today’s findings – the researchers hope in future to evaluate the effectiveness of xenon in human TBI patients.
This study was funded by the Medical Research Council, the European Society for Anaesthesiology, the National Institute for Academic Anaesthesia, the Association of Anaesthetists of Great Britain & Ireland, and the Gas Safety Trust.
See Headway or TBI TALK for information and support on living with brain injury.
“Xenon improves long-term cognitive function, reduces neuronal loss and chronic neuroinflammation, and improves survival after traumatic brain injury in mice” by Rita Campos-Pires, Tobias Hirnet, Flavia Valeo, Bee Eng Ong, Konstantin Radyushkin, Jitka Aldhoun, Joanna Saville, Christopher J. Edge, Nicholas P. Franks, Serge C. Thal, and Robert Dickinson. Published 21 May 2019 in British Journal of Anaesthesia.
Images credited to Tobias Hirnet.
Graph credited to Robert Dickinson.
Article supporters
Article text (excluding photos or graphics) © Imperial College London.
Photos and graphics subject to third party copyright used with permission or © Imperial College London.
Reporter
Caroline Brogan
Communications Division