With the rise of digital technologies, there are more data available than ever before. Healthcare is no exception. And not only are there more data, but they are coming from different places. Alongside the more traditional sources such as government, healthcare systems and academia, data are being churned out from medical devices, mobile apps and websites.
We need to be able to link up and consolidate these increasingly complex data, and turn them into useful information that can improve healthcare and inform policy, both locally and globally.
We were established in response to this need. We’re a strategic unit within the Institute of Global Health Innovation that aims to enhance patient care through a more effective use of health data. Our hub gathers, houses, interprets, and analyses health datasets, to make impactful discoveries about both individual people and whole populations. It also ensures that the data is stored and managed appropriately, in compliance with data protection regulations.
Our work
We use data science and analytics to answer big questions: Are we performing as well as other healthcare systems? How can we generate national approaches to disease prevention? How best can we use genetic data to make medicine more personalised?
These are just a few of the areas our team is interested in. Find out more about some of the work our researchers are doing to use data to influence policy and improve healthcare.
Find out more about our work
- COVID-19 behaviour tracker
- Data at doctors' fingertips
- Guiding patient data sharing
- The Networked Data Lab
- Improving road safety

In April 2020 we began tracking how people were responding to the coronavirus pandemic across 29 countries, areas or territories. Data from our global survey, run in partnership with YouGov, are made freely available through an open data dashboard, policy reports and GitHub (for more information see IGHI's response to COVID-19.)
As part of this project, we have partnered with the co-editors of the World Happiness Report, published by the UN Sustainable Development Solutions Network, to explore life satisfaction during COVID-19. We also acknowledge the contribution from the World Health Organization working group on measuring behavioural and social drivers (BeSD) of COVID-19 vaccination.
Data from the COVID-19 Behaviour Tracker have been used in a number of academic publications. A recent paper by our team found that vaccine hesitancy decreased considerably between November 2020 and January 2021 across surveyed countries.
The project was led by Sarah P Jones, IGHI doctoral researcher, Melanie Leis, Director of Policy and Analysis at the Centre for Health Policy, and Gianluca Fontana, Deputy Director of IGHI.
We’re grateful to our collaborators from the World Happiness Report, who are leading the analysis on life satisfaction levels: Professor John F Helliwell, Professor Jeffrey D Sachs, Professor the Lord Richard Layard, and Associate Professor Jan-Emmanuel De Neve.
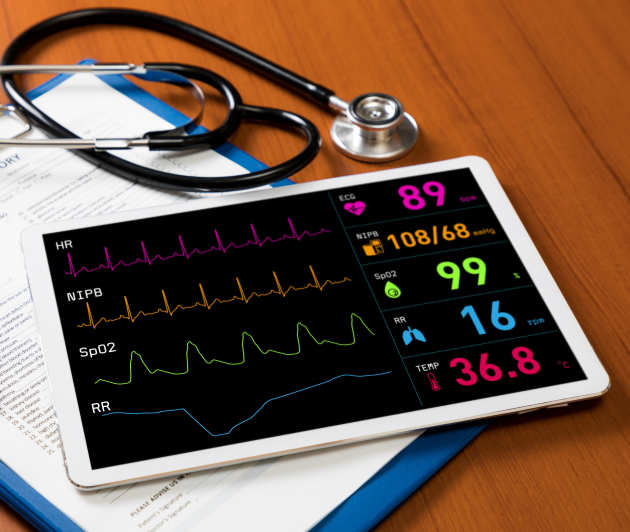
We helped develop Streams, a mobile app for medical information and alerting. Streams stores important patient data, like blood test results, in one easy-to-access place so that professionals have the information they need to act quickly should problems arise. Early studies showed how Streams leads to more efficient responses than traditional pager systems.
Now, as part of an HDR UK-funded study, we’re analysing new data from Streams as it’s trialled in hospitals. We’re looking at whether the app can reduce the length of time it takes for patients to receive treatment, compared with standard care. With more rapid responses, Streams could lead to better outcomes for patients and improve their care.
Contact Ravi Aggarwal to find out more about Streams.
 Within the NHS, hospitals are connected to one another by the patients they share. We’re examining connections between hospitals to optimise data sharing strategies, streamlining care for patients and potentially freeing up vital NHS resources.
Within the NHS, hospitals are connected to one another by the patients they share. We’re examining connections between hospitals to optimise data sharing strategies, streamlining care for patients and potentially freeing up vital NHS resources.
Hospitals and care providers often use different systems to hold electronic patient data, meaning records can’t easily be transferred. This frustrates patients, creates delays in treatment, and risks patient safety if vital information is missed or forgotten. But ensuring that all healthcare providers have systems that can work together would be a costly and lengthy process.
In collaboration with the EPSRC Centre for Mathematics of Precision Healthcare, our researchers have been using network analysis to identify groups of hospitals that share the greatest number of patients, highlighting areas where patients would benefit the most from having compatible systems. This work can help the NHS guide discussion on how to achieve better data sharing between hospitals, prioritising trusts that commonly share patients. This means that limited resources can be directed towards areas where they will have the most immediate positive impact on patients.
Read our latest research on advocating for improving data sharing between acute hospitals in England here and our study on managing elective surgery after COVID-19. For more information, contact Dr Jonathan Clarke.
 In the summer of 2020, Imperial College Health Partners, the Institute of Global Health Innovation and the North West London Collaboration of Clinical Commissioning Groups were successful in being named one of the five Networked Data Labs in the UK. The Networked Data Lab is a two-year programme funded by the Health Foundation to develop a collaborative network of five analytical teams across the country. These teams use linked datasets to answer questions on key issues facing health and care services locally and nationally. The overall aim of the Networked Data Lab is to improve health and care services and reduce health inequalities in the UK.
In the summer of 2020, Imperial College Health Partners, the Institute of Global Health Innovation and the North West London Collaboration of Clinical Commissioning Groups were successful in being named one of the five Networked Data Labs in the UK. The Networked Data Lab is a two-year programme funded by the Health Foundation to develop a collaborative network of five analytical teams across the country. These teams use linked datasets to answer questions on key issues facing health and care services locally and nationally. The overall aim of the Networked Data Lab is to improve health and care services and reduce health inequalities in the UK.
Covering North West London, we’re working together to use both our local linked data set and engagement with patients and the public to help uncover and address some of the inequalities currently faced by patients and the public as a result of the COVID-19 pandemic. The programme’s findings have helped inform recent Health Foundation initiatives around the demographics and hospital use of shielding patients, revealing the severe impact the pandemic has had on those with long-term conditions, particularly people from a socially deprived background.
For more information on IGHI’s work as part of the Networked Data Lab contact Melanie Leis, Director of Policy and Analysis at the Centre for Health Policy.

Our Road Traffic Injury – Analytics for Integrated Data (RTI-AID) project is using crowdsourced data to develop a road traffic injury surveillance tool to aid emergency medical systems and road safety interventions.
Good trauma system planning requires robust traffic collision and injury data, which can inform hospital care, reduce ambulance travel time, and reduce high-risk roads.
The World Health Organization’s Injury Surveillance and Trauma Care guidelines highlight the need for good data, particularly where resources are limited. Such data is sparse in developing countries, but the boom in digital technology in developing world cities offers a potential alternative data source to help capacity-building, injury care and risk reduction, in line with the UN’s Decade of Action for Road Safety.
We’re seeking to:
-
Collect and pool novel digital data sources relating to road traffic collisions, such as online media, news, mobile navigation apps and vehicle monitoring systems;
-
Assess the ability of these sources to identify the real-world location, timing and severity of road traffic collisions and injury;
-
Compare the accuracy of these sources for road collision and injury surveillance to well-established high-quality data from London’s transport, ambulance, and health services; and
-
Explore whether these sources could help developing world cities to overcome inadequate infrastructure, raise awareness and improve outcomes for people injured in a traffic collision.
Find out more about RTA-AID here or contact Seema Yalamanchili.
Our progress

Listen, learn, improve
Patients’ feedback on their experience of care is a hugely valuable resource that could guide measures to improve care quality. But it’s been largely untapped as free text is difficult to analyse en masse and extract meaningful insights from.
Our researchers have used a technique called Natural Language Processing to crunch huge swathes of feedback and gain a greater understanding of patient experience. This transformative project won a BMJ Award for Digital Innovation and could lead to new measures to improve the quality of healthcare.

Determining the true cost of sickness
With an ageing population and rising levels of obesity, more and more people in the UK are living with more than one health condition (multimorbidity). We’ve been working with the Business School to facilitate their research that’s examining the financial impact of multimorbidity on health systems.
This research combined primary and secondary care data to look at the impact and costs of having more than one non-communicable (can't be passed on) disease, compared with having one illness. The work involved more than 1 million patients and forms part of a trans-European study that’s comparing the cost of illness across the continent, helping us to better understand the economic burden of disease and inform future strategies that could mitigate these rising costs.
Contact us
If you’re interested in finding out more about our work or collaborating with us, get in touch with:
Melanie Leis
Director of Policy and Analysis
Centre for Health Policy
Institute of Global Health Innovation
Read our publications
International attitudes on COVID-19 vaccination: repeat national cross-sectional surveys across 15 countries, medRxiv, March 2021.
Public perceptions on data sharing: key insights from the UK and the USA, The Lancet, July 2020
NHS data: Maximising its impact on the health and wealth of the United Kingdom, February 2020
The effects and preventability of 2627 patient safety incidents related to health information technology failures, The Lancet, July 2019.
Evaluating the impact of organisational digital maturity on clinical outcomes in secondary care in England, Nature Digital Medicine, May 2019.
Assessing the Agreement of 5 Ideal Body Weight Calculations for Selecting Medication Dosages for Children With Obesity, JAMA Pediatrics, April 2019.
