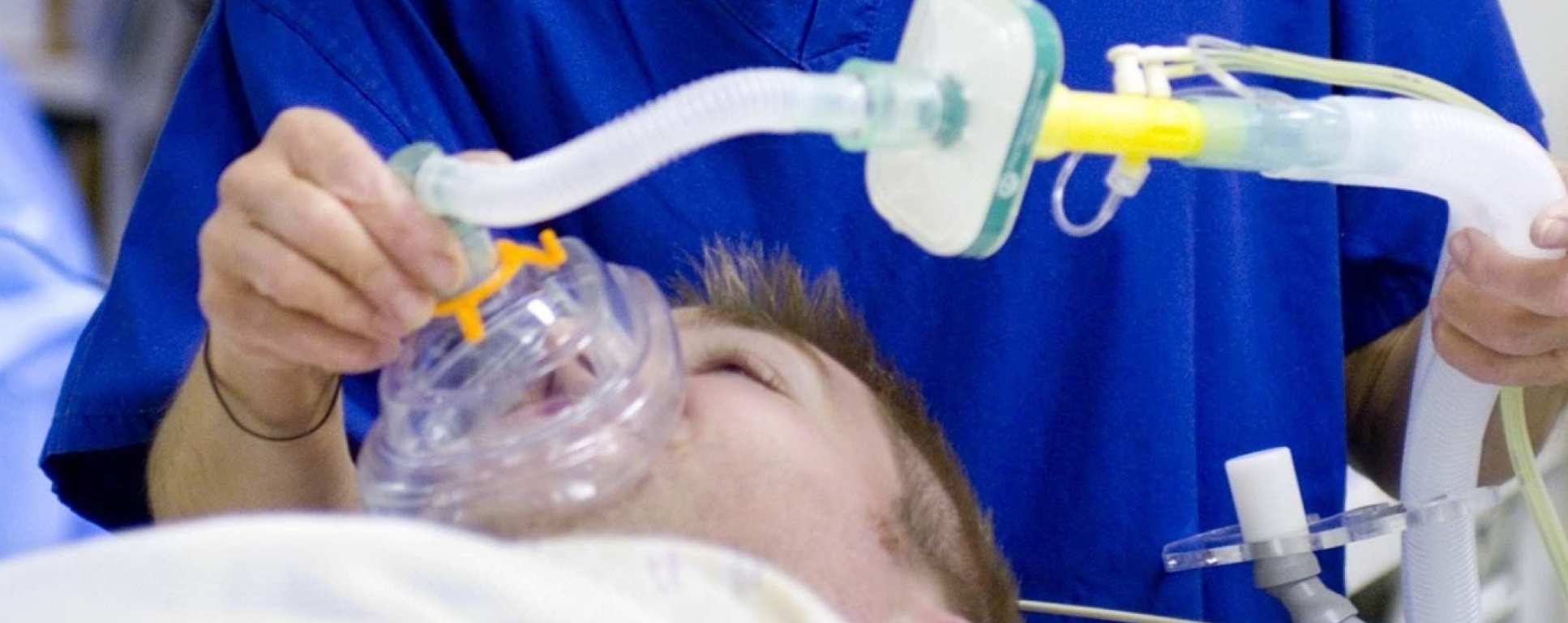
 Anaesthesia makes up the largest hospital speciality and has a huge role to play in nearly every aspect of any hospital from operating theatres to accident and emergency, to the labour ward, and to intensive care. Our research ranges from basic molecular research into mechanisms of anaesthesia to investigating the clinical impact of novel anaesthetic agents.
Anaesthesia makes up the largest hospital speciality and has a huge role to play in nearly every aspect of any hospital from operating theatres to accident and emergency, to the labour ward, and to intensive care. Our research ranges from basic molecular research into mechanisms of anaesthesia to investigating the clinical impact of novel anaesthetic agents.
Our research covers the entirety of patient’s perioperative journey and through this, we aim to deliver the greatest impact. The section has been pioneering in the development of novel technologies to facilitate the delivery of anaesthetic agents and has also made pivotal in-roads into the mechanism of action of anaesthetic agents and their wider application to other diseases (such as their protective roles in brain injury and in cancer).
Research themes:
- Anaesthesia mechanisms and effects
- Brain and neuroprotection
- Cardiothoracic anaesthesia and transplantation
Results
- Showing results for:
- Reset all filters
Search results
-
Conference paperCampos-Pires R, Armstrong S, Sebastiani A, et al., 2018,
Xenon treatment improves short-term and long-term outcomes in a rodent model of traumatic brain injury
, British Journal of Anaesthesia Research Forum, Publisher: Elsevier, Pages: e21-e21, ISSN: 0007-0912 -
Journal articleVizcaychipi MP, Hua, Loganathan, et al., 2017,
Assessment of haemodynamic response to induction of general anaesthesia in healthy adult patients undergoing elective orthopaedic surgery by using a continuous non-invasive cardiovascular monitoring
, Open Anesthesiology Journal, Vol: 11, Pages: 75-82, ISSN: 1874-3218BackgroundContinuous cardiovascular monitoring as part of management of high-risk surgical patients is widely practiced, however continuous monitoring as part of routine management in low-risk surgical patients is unclear. Detailed monitoring of cardiovascular parameters from the pre-induction stage allows clinicians to individualise anaesthetic management in the perioperative period. Our aim was to investigate haemodynamic and Bispectral Index (BIS) changes in healthy patients undergoing surgery following induction of anaesthesia with propofol using a continuous non-invasive blood pressure device (LiDCOrapid™).MethodsThis prospective, observational single-centre study was conducted at a London teaching hospital between June-November 2014. Patients aged between 18-45 years, American Society of Anesthesiologists grade I-II undergoing elective lower-limb arthroscopic procedures were included. Variables including heart rate (HR), mean arterial pressure (MAP), stroke volume (SV), cardiac output (CO), systemic vascular resistance (SVR) and BIS were recorded continuously prior to induction and up to 3-minutes after. ResultsThe following relative haemodynamic changes were noted between baseline and 1-minute post-induction with propofol: CO +15.2%, HR +10.1%, SVR -22.9% and MAP -10.1%(p<0.001 for each parameter). There was a mean change of: HR -10.1%, CO -14% and MAP -18.0%(p<0.001 for each parameter) between baseline and 3-minutes post-induction. Median change of BIS was -61.7%(p<0.001) between baseline and 3-minutes post-induction. Significant, positive correlations noted between MAP and BIS at 30-seconds(r=0.60, p<0.001) and 1-minute post-induction (r=0.61, p<0.001).ConclusionOur study shows that healthy patients undergoing continuous minimally invasive orthopaedic surgery experience significant haemodynamic and BIS changes following induction of anaesthesia. Our findings highlight the importance of baseline cardiovascular and BIS monitoring as part
-
Journal articleWu X, Cui F, Zhang C, et al.,
Low-dose dexmedetomidine improves sleep quality pattern in elderly patients after noncardiac surgery in the intensive care unit: a pilot randomized controlled trial
, Anesthesiology, ISSN: 1528-1175Background: It has been shown that dexmedetomidine sedation can improve sleep architecture in mechanically ventilated patients. We hypothesized that low-dose dexmedetomidine infusion could also improve sleep architecture in non-mechanically ventilated elderly patients in the Intensive Care Unit (ICU) after surgery. Methods: This was a randomized, double-blind, placebo-controlled, parallel-arm pilot trial. Seventy-six patients of 65 years or older who were admitted to the ICU after non-cardiac surgery and did not require mechanical ventilation were randomized to receive dexmedetomidine (continuous infusion at a rate of 0.1 μg kg-1 h-1, n = 38) or placebo (n = 38) for 15 hours, i.e., from 5:00 PM on the day of surgery until 8:00 AM on the first day after surgery. Polysomnogram was monitored during the period of study drug infusion. The primary endpoint was the percentage of stage 2 non-rapid eye movement (stage N2) sleep. Results: Complete polysomnogram recordings were obtained in 61 patients (30 in the placebo group and 31 in the dexmedetomidine group). Compared with placebo, dexmedetomidine infusion significantly increased the percentage of stage N2 sleep (mean difference ***, 95% confidence interval **-**, P = ***); it also significantly prolonged the total sleep time, decreased the percentage of stage N1 sleep, and increased the sleep efficiency. However, the incidence of hypotension of all enrolled patients were significantly higher in the dexmedetomidine group than in the placebo group (39.5% [15/38] vs 13.2% [5/38], P = 0.009). Conclusions: In non-mechanically ventilated elderly patients who were admitted to ICU after non-cardiac surgery, the prophylactic low-dose dexmedetomidine infusion may improve sleep architecture but increases hypotension.
-
Journal articleCampos-Pires R, Edge CJ, Dickinson R, 2016,
Argon: A Noble Foe for Subarachnoid Hemorrhage
, Critical Care Medicine, Vol: 44, Pages: 1456-1457, ISSN: 1530-0293 -
Conference paperCampos-Pires R, Armstrong S, Sebastiani A, et al., 2016,
Xenon provides short-term and long-term neuroprotection in a rodent model of traumatic brain injury
, International Brain Injury Association’s Eleventh World Congress on Brain Injury, Publisher: Taylor & Francis, Pages: 653-653, ISSN: 1362-301X -
Conference paperHarris K, Armstrong S, Campos-Pires R, et al., 2016,
Neuroprotection against traumatic brain injury by xenon, but not argon, is mediated by inhibition at the N-methyl-D-aspartate receptor glycine site
, International Brain Injury Association’s Eleventh World Congress on Brain Injury, Publisher: Taylor & Francis, Pages: 606-606, ISSN: 1362-301X -
Journal articleZhao H, Mitchell S, Koumpa S, et al., 2016,
Heme Oxygenase-1 mediates neuro-protection conferred by argon in combination with hypothermia in neonatal hypoxia-ischemia brain injury
, Anesthesiology, Vol: 125, Pages: 180-192, ISSN: 1528-1175Argon–hypothermia treatment reduced both neuronal death in an in vitro neuronal culture model and brain infarct size in an in vivo rat model of neonatal asphyxia. The protective effects of argon–hypothermia involve both inhibition of apoptosis and neuroinflammation mechanisms and activation of cell survival pathways.
-
Book chapterCampos-Pires R, Dickinson R, 2016,
Modelling Blast Brain Injury
, Blast Injury Science and Engineering A Guide for Clinicians and Researchers, Editors: Clasper, Bull, Mahoney, Publisher: Springer, Pages: 173-182, ISBN: 9783319218670The consequences of blast traumatic brain injury (blast-TBI) in humans are largely determined by the characteristics of the trauma insult and, within certain limits, the individual responses to the lesions inflicted (1). In blast-TBI the mechanisms of brain vulnerability to the detonation of an explosive device are not entirely understood. They most likely result from a combination of the different physical aspects of the blast phenomenon, specifically extreme pressure oscillations (blast-overpressure wave), projectile penetrating fragments and acceleration-deceleration forces, creating a spectrum of brain injury that ranges from mild to severe blast-TBI (2). The pathophysiology of penetrating and inertially-driven blast-TBI has been extensively investigated for many years. However, the brain damage caused by blast-overpressure is much less understood and is unique to this type of TBI (3). Indeed, there continues to be debate about how the pressure wave is transmitted and reflected through the brain and how it causes cellular damage (4). No single model can mimic the clinical and mechanical complexity resulting from a real life blast-TBI (3). The different models, non-biological (in silico or surrogate physical) and biological (ex vivo, in vitro or in vivo), tend to complement each other.
-
Journal articleMohite PN, Sabashnikov A, Patil NP, et al., 2016,
The role of cardiopulmonary bypass in lung transplantation
, CLINICAL TRANSPLANTATION, Vol: 30, Pages: 202-209, ISSN: 0902-0063- Author Web Link
- Cite
- Citations: 21
-
Journal articleMa D,
Is volatile anesthesia during cancer surgery likely to increase the metastatic risk?
, Anaesthesia, ISSN: 1365-2044
This data is extracted from the Web of Science and reproduced under a licence from Thomson Reuters. You may not copy or re-distribute this data in whole or in part without the written consent of the Science business of Thomson Reuters.