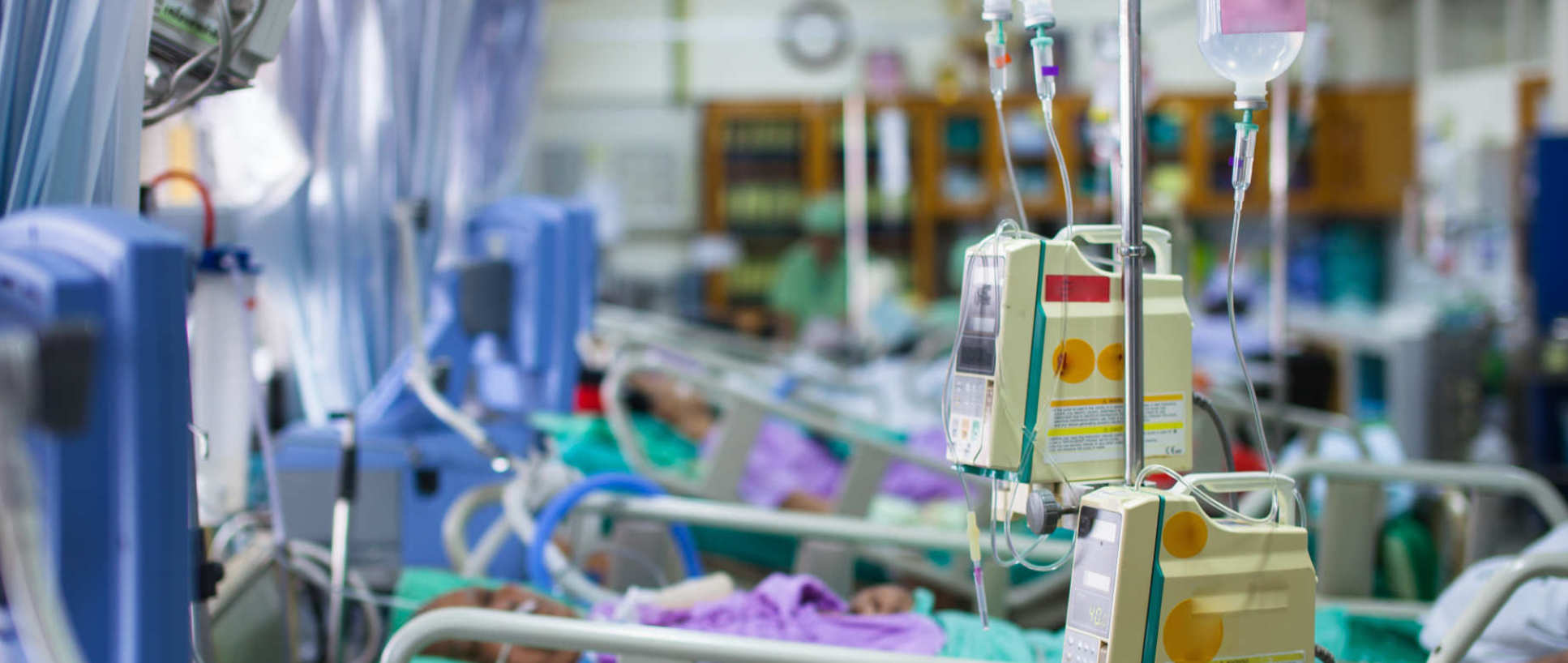
 Critical care involves the care of the sickest patients in the hospital. Critically ill patients have usually been through a significant insult to their body (such as trauma, infection, burn) and have developed organ failure and require life-support. Critical Care is the largest theme bringing together clinicians and scientists from diverse backgrounds and includes collaborative research from hospitals throughout north-west London. Investigations range from evaluating biological mechanisms of organ failure through to the development of innovative technologies which allow the short-term and long-term support and recovery of organs.
Critical care involves the care of the sickest patients in the hospital. Critically ill patients have usually been through a significant insult to their body (such as trauma, infection, burn) and have developed organ failure and require life-support. Critical Care is the largest theme bringing together clinicians and scientists from diverse backgrounds and includes collaborative research from hospitals throughout north-west London. Investigations range from evaluating biological mechanisms of organ failure through to the development of innovative technologies which allow the short-term and long-term support and recovery of organs.
Many people are exposed to the environment of an Intensive care unit (ICU) either personally or through a family member. It is often a life-changing event and our work aims to reduce this impact facilitating post-ICU recovery.
Research themes:
- Acute Respiratory Distress Syndrome (ARDS)
- Burn injury
- Extracorporeal life support
- Functional outcomes and health service research
- Sepsis
Results
- Showing results for:
- Reset all filters
Search results
-
Journal articleWilson MR, Wakabayashi K, Bertok S, et al., 2017,
Inhibition of TNF receptor p55 by a domain antibody attenuates the initial phase of acid-induced lung injury in mice
, Frontiers in Immunology, Vol: 8, ISSN: 1664-3224Background: Tumor necrosis factor-α (TNF) is strongly implicated in the development ofacute respiratory distress syndrome (ARDS), but its potential as a therapeutic target has beenhampered by its complex biology. TNF signals through two receptors, p55 and p75, whichplay differential roles in pulmonary edema formation during ARDS. We have recentlyshown that inhibition of p55 by a novel domain antibody (dAb™) attenuated ventilator36induced lung injury. In the current study we explored the efficacy of this antibody in mousemodels of acid-induced lung injury, to investigate the longer consequences of treatment.Methods: We employed two acid-induced injury models, an acute ventilated model and aresolving spontaneously breathing model. C57BL/6 mice were pretreated intratracheally orintranasally with p55-targeting dAb or non-targeting ‘dummy’ dAb, 1 or 4 hours before acidinstillation.Results: Acid instillation in the dummy dAb group caused hypoxemia, increased respiratorysystem elastance, pulmonary inflammation and edema in both the ventilated and resolvingmodels. Pretreatment with p55-targeting dAb significantly attenuated physiological markersof ARDS in both models. p55-targeting dAb also attenuated pulmonary inflammation in theventilated model, with signs that altered cytokine production and leukocyte recruitmentpersisted beyond the very acute phase.Conclusions: These results demonstrate that the p55-targeting dAb attenuates lung injury andedema formation in models of ARDS induced by acid aspiration, with protection from asingle dose lasting up to 24 hours. Together with our previous data, the current study lends support towards the clinical targeting of p55 for patients with, or at risk of ARDS.
-
Journal articleBurnham KL, Davenport EE, Radhakrishnan J, et al., 2016,
Shared and distinct aspects of the sepsis transcriptomic response to fecal peritonitis and pneumonia.
, American Journal of Respiratory and Critical Care Medicine, Vol: 196, Pages: 328-339, ISSN: 1535-4970RATIONALE: Heterogeneity in the septic response has hindered efforts to understand pathophysiology and develop targeted therapies. Source of infection, with different causative organisms and temporal changes, might influence this heterogeneity. OBJECTIVES: To investigate individual and temporal variation in the transcriptomic response to sepsis due to fecal peritonitis, and to compare with community acquired pneumonia. METHODS: We performed genome-wide gene expression profiling in peripheral blood leukocytes for adult patients admitted to intensive care with sepsis due to fecal peritonitis (n=117) or community acquired pneumonia (n=126), and non-septic controls (n=10). MEASUREMENTS AND MAIN RESULTS: A substantial portion of the transcribed genome (18%) was differentially expressed compared to controls, independent of source of infection, with EIF2 signaling the most enriched canonical pathway. We identify two sepsis response signature subgroups in fecal peritonitis associated with early mortality (p-value=0.01, hazard ratio=4.78). We define gene sets predictive of SRS group, and serial sampling demonstrates subgroup membership is dynamic during ICU admission. We find SRS is the major predictor of transcriptomic variation; a small number of genes (n=263) were differentially regulated according to the source of infection, enriched for interferon signaling and antigen presentation. We define temporal changes in gene expression from disease onset involving phagosome formation, NK cell and IL-3 signaling. CONCLUSIONS: The majority of the sepsis transcriptomic response is independent of source of infection and includes signatures reflecting immune response state and prognosis. A modest number of genes show evidence of specificity. Our findings highlight opportunities for patient stratification and precision medicine in sepsis.
-
Journal articleO'Dea KP, Porter J, TIrlapur N, et al., 2016,
Circulating microvesicles are elevated acutely following major burns injury and associated with clinical severity
, PLOS One, Vol: 11, ISSN: 1932-6203Microvesicles are cell-derived signaling particles emerging as important mediators and biomarkers of systemic inflammation, but their production in severe burn injury patients has not been described. In this pilot investigation, we measured circulating microvesicle levels following severe burns, with severe sepsis patients as a comparator group.We hypothesized that levels of circulating vascular cell-derived microvesicles are elevated acutely following burns injury, mirroring clinical severity due to the early onset and prevalence of systemic inflammatory response syndrome (SIRS) in these patients. Blood samples were obtained from patients with moderate to severe thermal injury burns, with severe sepsis, and from healthy volunteers. Circulating microvesicles derived from total leukocytes, granulocytes, monocytes, and endothelial cells were quantified in plasma by flow cytometry.All circulating microvesicle subpopulations were elevated in burns patients on day of admission (day 0) compared to healthy volunteers (leukocyte-microvesicles: 3.5-fold, p=0.005; granulocyte-microvesicles: 12.8-fold, p<0.0001; monocyte-microvesicles: 20.4-fold, p<0.0001; endothelial- microvesicles: 9.6-fold, p=0.01), but decreased significantly by day 2. Microvesicle levels were increased with severe sepsis, but less consistently between patients. Leukocyte- and granulocyte-derived microvesicles on day 0 correlated with clinical assessment scores and were higher in burns ICU non-survivors compared to survivors (leukocyte MVs 4.6 fold, p=0.002; granulocyte MVs 4.8 fold, p=0.003). Mortality prediction analysis of area under receiver operating characteristic curve was 0.92 (p=0.01) for total leukocyte microvesicles and 0.85 (p=0.04) for granulocyte microvesicles. These findings demonstrate, for the first t
-
Journal articleArulkumaran N, Harrison DA, Brett SJ, 2016,
Association between day and time of admission to critical care and acute hospital outcome for unplanned admissions to adult general critical care units: cohort study exploring the ‘weekend effect’
, British Journal of Anaesthesia, Vol: 118, Pages: 112-122, ISSN: 1471-6771Background. We aimed to identify any association between day and time of admission to critical care and acute hospital outcome.Methods. We conducted a cohort study using prospectively collected data from the national clinical audit of adult critical care. We included 195 428 unplanned admissions from 212 adult general critical care units in England, Wales and Northern Ireland, between April 1, 2013 and March 31, 2015 in the analysis.Results. Hourly admission rates for unplanned admissions varied more than three-fold during the 24 h cycle. Overall acute hospital mortality was 26.8%. Before adjustment, acute hospital mortality was similar between weekends and weekdays but was significantly lower for admissions at night compared with the daytime (−3.4%, −3.8 to −3.0%; P<0.001). After adjustment for casemix, there remained no difference between weekends and weekdays (−0.0%, −0.4 to +0.3%; P=0.87) or between nighttime and daytime (−0.2%, −0.5 to +0.1%; P=0.21). Delays in admission were reported for 4.3% of admissions and were slightly more common during weekdays than weekends and in the daytime than at night. Delayed admission was associated with a small increase in acute hospital mortality, but adjusting for this did not affect the estimates of the effect of day and time of admission.Conclusions. The day of week and time of admission have no influence on patient mortality for unplanned admissions to adult general critical care units within the UK. Ways to improve critical care and hospital systems to minimize delays in admission and potentially improve outcomes need to be ascertained in future research.
-
Journal articleEdey LF, O'Dea KP, Herbert BR, et al., 2016,
The local and systemic immune response to intrauterine LPS in the prepartum mouse
, Biology of Reproduction, Vol: 95, Pages: 1-10, ISSN: 1529-7268Inflammation plays a key role in human term and preterm labor (PTL). Intrauterine LPS has been widely used to model inflammation-induced complications of pregnancy, including PTL. It has been shown to induce an intense myometrial inflammatory cell infiltration, but the role of LPS-induced inflammatory cell activation in labor onset and fetal demise is unclear. We investigated this using a mouse model of PTL, where an intrauterine injection of 10 μg of LPS (serotype 0111:B4) was given at E16 of CD1 mouse pregnancy. This dose induced PTL at an average of 12.7 h postinjection in association with 85% fetal demise. Flow cytometry showed that LPS induced a dramatic systemic inflammatory response provoking a rapid and marked leucocyte infiltration into the maternal lung and liver in association with increased cytokine levels. Although there was acute placental inflammatory gene expression, there was no corresponding increase in fetal brain inflammatory gene expression until after fetal demise. There was marked myometrial activation of NFκB and MAPK/AP-1 systems in association with increased chemokine and cytokine levels, both of which peaked with the onset of parturition. Myometrial macrophage and neutrophil numbers were greater in the LPS-injected mice with labor onset only; prior to labor, myometrial neutrophils and monocytes numbers were greater in PBS-injected mice, but this was not associated with an earlier onset of labor. These data suggest that intrauterine LPS induces parturition directly, independent of myometrial inflammatory cell infiltration, and that fetal demise occurs without fetal inflammation. Intrauterine LPS provokes a marked local and systemic inflammatory response but with limited inflammatory cell infiltration into the myometrium or placenta.
-
Journal articleMa D, Zhao H,
The role of Nuclear factor-erythroid 2 related factor 2 (Nrf-2) in the protection against lung injury.
, American Journal of Physiology-Lung Cellular and Molecular Physiology -
Journal articleMobasheri MH, King D, Judge S, et al., 2016,
Communication aid requirements of intensive care unit patients with transient speech loss
, Augmentative and Alternative Communication, Vol: 32, Pages: 261-271, ISSN: 1477-3848Alert and transiently nonvocal intensive care unit (ICU) patients are dependent on augmentative and alternative communication (AAC). Unfortunately, the literature demonstrates that existent AAC devices have not been widely adopted, and unaided methods are often the primary modalities used despite being insufficient, and frustrating. We present the results of a qualitative semi-structured interview study with 8 ex-ICU patients, 4 ICU patient relatives, and 6 ICU staff, exploring their AAC needs and requirements. Participants identified important AAC hardware, software, and content requirements. Salient factors impacting on AAC adoption in the ICU setting were also highlighted and included the need for staff training and bedside patient assessment. Based on the study results, we propose a series of recommendations regarding the design and implementation of future AAC tools specifically targeted at this group.
-
Journal articleGordon AC, Perkins GD, Singer M, et al., 2016,
Levosimendan for the prevention of acute organ dysfunction in sepsis
, New England Journal of Medicine, Vol: 375, Pages: 1638-1648, ISSN: 0028-4793BACKGROUNDLevosimendan is a calcium-sensitizing drug with inotropic and other propertiesthat may improve outcomes in patients with sepsis.METHODSWe conducted a double-blind, randomized clinical trial to investigate whether levosimendanreduces the severity of organ dysfunction in adults with sepsis. Patientswere randomly assigned to receive a blinded infusion of levosimendan (at a dose of0.05 to 0.2 μg per kilogram of body weight per minute) for 24 hours or placeboin addition to standard care. The primary outcome was the mean daily SequentialOrgan Failure Assessment (SOFA) score in the intensive care unit up to day 28 (scoresfor each of five systems range from 0 to 4, with higher scores indicating more severedysfunction; maximum score, 20). Secondary outcomes included 28-day mortality,time to weaning from mechanical ventilation, and adverse events.RESULTSThe trial recruited 516 patients; 259 were assigned to receive levosimendan and257 to receive placebo. There was no significant difference in the mean (±SD) SOFAscore between the levosimendan group and the placebo group (6.68±3.96 vs.6.06±3.89; mean difference, 0.61; 95% confidence interval [CI], −0.07 to 1.29;P=0.053). Mortality at 28 days was 34.5% in the levosimendan group and 30.9%in the placebo group (absolute difference, 3.6 percentage points; 95% CI, −4.5 to11.7; P=0.43). Among patients requiring ventilation at baseline, those in the levosimendangroup were less likely than those in the placebo group to be successfullyweaned from mechanical ventilation over the period of 28 days (hazard ratio,0.77; 95% CI, 0.60 to 0.97; P=0.03). More patients in the levosimendan group thanin the placebo group had supraventricular tachyarrhythmia (3.1% vs. 0.4%; absolutedifference, 2.7 percentage points; 95% CI, 0.1 to 5.3; P=0.04).CONCLUSIONSThe addition of levosimendan to standard treatment in adults with sepsis was notassociated with less severe organ dysfunction or lower mortality. Levosim
-
Journal articleWilson MR, Takata M, John AE, et al., 2016,
Loss of epithelial Gq and G11 signaling inhibits TGFβ production but promotes IL-33–mediated macrophage polarization and emphysema
, Science Signaling, Vol: 9, Pages: 1-17, ISSN: 1945-0877Heterotrimeric guanine nucleotide–binding protein (G protein) signaling links hundreds of Gprotein–coupled receptors (GPCRs) with four G protein signaling pathways. Two of these,one mediated by Gq and G11 (Gq/11) and the other by G12 and G13 (G12/13), are implicated inthe force-dependent activation of transforming growth factor–β (TGFβ) in lung epithelialcells. Reduced TGFβ activation in alveolar cells leads to emphysema, whereas enhancedTGFβ activation promotes acute lung injury and idiopathic pulmonary fibrosis. Therefore,precise control of alveolar TGFβ activation is essential for alveolar homeostasis. Here, weinvestigated the involvement of the Gq/11and G12/13 pathways in epithelial cells in generatingactive TGFβ and regulating alveolar inflammation. Mice deficient in both Gαq and Gα11developed inflammation that was primarily caused by alternatively activated (M2-polarized)macrophages, enhanced matrix metalloprotease 12 (MMP12) production, and age-relatedalveolar airspace enlargement consistent with emphysema. Mice with impaired Gq/11signaling had reduced stretch-mediated generation of TGFβ by epithelial cells and enhancedmacrophage MMP12 synthesis, but were protected from the effects of ventilator-induced lunginjury. Furthermore, synthesis of the cytokine interleukin-33 (IL-33) was increased in thesealveolar epithelial cells, resulting in the M2-type polarization of alveolar macrophages independently of the effect on TGFβ. Our results suggest that alveolar Gq/11 signalingmaintains alveolar homeostasis, and likely independently increases TGFβ activation inresponse to mechanical stress of the epithelium and decreases epithelial IL-33 synthesis.Together, these findings suggest that disruption of Gq/11 signaling promotes inflammatoryemphysema but protects against mechanically induced lung injury.
-
Journal articleSoni S, Wilson MR, O'Dea KP, et al., 2016,
Alveolar macrophage-derived microvesicles mediate acute lung injury
, Thorax, Vol: 71, Pages: 1020-1029, ISSN: 1468-3296Background Microvesicles (MVs) are important mediators of intercellular communication, packaging a variety of molecular cargo. They have been implicated in the pathophysiology of various inflammatory diseases; yet, their role in acute lung injury (ALI) remains unknown.Objectives We aimed to identify the biological activity and functional role of intra-alveolar MVs in ALI.Methods Lipopolysaccharide (LPS) was instilled intratracheally into C57BL/6 mice, and MV populations in bronchoalveolar lavage fluid (BALF) were evaluated. BALF MVs were isolated 1 hour post LPS, assessed for cytokine content and incubated with murine lung epithelial (MLE-12) cells. In separate experiments, primary alveolar macrophage-derived MVs were incubated with MLE-12 cells or instilled intratracheally into mice.Results Alveolar macrophages and epithelial cells rapidly released MVs into the alveoli following LPS. At 1 hour, the dominant population was alveolar macrophage-derived, and these MVs carried substantive amounts of tumour necrosis factor (TNF) but minimal amounts of IL-1β/IL-6. Incubation of these mixed MVs with MLE-12 cells induced epithelial intercellular adhesion molecule-1 (ICAM-1) expression and keratinocyte-derived cytokine release compared with MVs from untreated mice (p<0.001). MVs released in vitro from LPS-primed alveolar macrophages caused similar increases in MLE-12 ICAM-1 expression, which was mediated by TNF. When instilled intratracheally into mice, these MVs induced increases in BALF neutrophils, protein and epithelial cell ICAM-1 expression (p<0.05).Conclusions We demonstrate, for the first time, the sequential production of MVs from different intra-alveolar precursor cells during the early phase of ALI. Our findings suggest that alveolar macrophage-derived MVs, which carry biologically active TNF, may play an important role in initiating ALI.
This data is extracted from the Web of Science and reproduced under a licence from Thomson Reuters. You may not copy or re-distribute this data in whole or in part without the written consent of the Science business of Thomson Reuters.