Critical Care
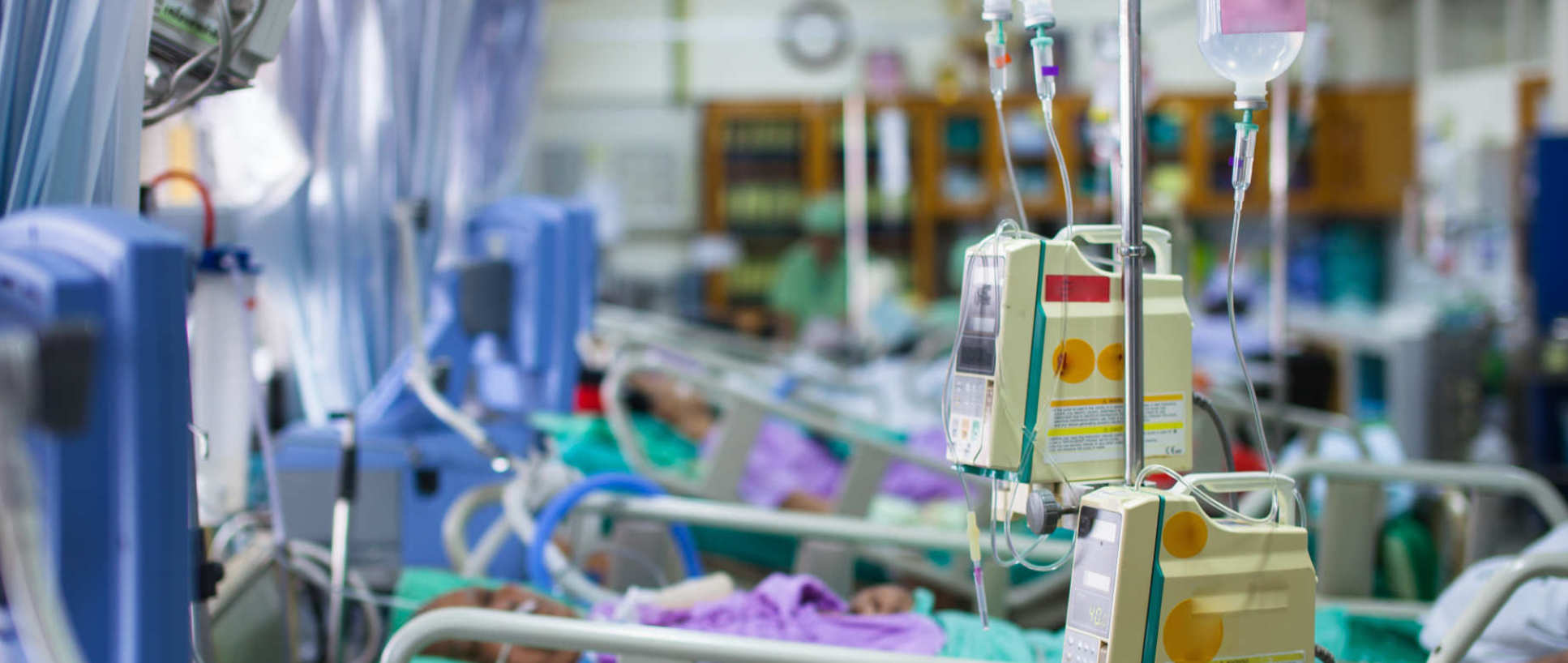 Critical care involves the care of the sickest patients in the hospital. Critically ill patients have usually been through a significant insult to their body (such as trauma, infection, burn) and have developed organ failure and require life-support. Critical Care is the largest theme bringing together clinicians and scientists from diverse backgrounds and includes collaborative research from hospitals throughout north-west London. Investigations range from evaluating biological mechanisms of organ failure through to the development of innovative technologies which allow the short-term and long-term support and recovery of organs.
Critical care involves the care of the sickest patients in the hospital. Critically ill patients have usually been through a significant insult to their body (such as trauma, infection, burn) and have developed organ failure and require life-support. Critical Care is the largest theme bringing together clinicians and scientists from diverse backgrounds and includes collaborative research from hospitals throughout north-west London. Investigations range from evaluating biological mechanisms of organ failure through to the development of innovative technologies which allow the short-term and long-term support and recovery of organs.
Many people are exposed to the environment of an Intensive care unit (ICU) either personally or through a family member. It is often a life-changing event and our work aims to reduce this impact facilitating post-ICU recovery.
Research themes:
- Acute Respiratory Distress Syndrome (ARDS)
- Burn injury
- Extracorporeal life support
- Functional outcomes and health service research
- Sepsis
Results
- Showing results for:
- Reset all filters
Search results
-
Journal articlePerner A, Gordon AC, De Backer D, et al., 2016,
Sepsis: frontiers in diagnosis, resuscitation and antibiotic therapy
, Intensive Care Medicine, Vol: 42, Pages: 1958-1969, ISSN: 1432-1238Sepsis is a major growing global burden and a major challenge to intensive care clinicians, researchers, guideline committee members and policy makers, because of its high and increasing incidence and great pathophysiological, molecular, genetic and clinical complexity. In spite of recent progress, short-term mortality remains high and there is growing evidence of long-term morbidity and increased long-term mortality in survivors of sepsis both in developed and developing countries. Further improvement in the care of patients with sepsis will impact upon global health. In this narrative review, invited experts describe the expected challenges and progress to be made in the near future. We focus on diagnosis, resuscitation (fluids, vasopressors, inotropes, blood transfusion and hemodynamic targets) and infection (antibiotics and infection biomarkers), as these areas are key, if initial management and subsequent outcomes are to be improved in patients with sepsis.
-
Journal articleTaylor J, Black S, Brett S, et al., 2016,
Design and implementation of the AIRWAYS-2 trial: A multi-centre cluster randomised controlled trial of the clinical and cost effectiveness of the i-gel supraglottic airway device versus tracheal intubation in the initial airway management of out of hospital cardiac arrest
, Resuscitation, Vol: 109, Pages: 25-32, ISSN: 1873-1570Health outcomes after out of hospital cardiac arrest (OHCA) are extremely poor, with only 7-9% of patients in the United Kingdom (UK) surviving to hospital discharge. Currently emergency medical services (EMS) use either tracheal intubation or newer supraglottic airway devices (SGAs) to provide advanced airway management during OHCA. Equipoise between the two techniques has led to calls for a well-designed randomised controlled trial. The primary objective of the AIRWAYS-2 trial is to assess whether the clinical effectiveness of the i-gel, a second-generation SGA, is superior to tracheal intubation in the initial airway management of OHCA patients in the UK. Paramedics recruited to the AIRWAYS-2 trial are randomised to use either tracheal intubation or i-gel as their first advanced airway intervention. Adults who have had a non-traumatic OHCA and are attended by an AIRWAYS-2 paramedic are retrospectively assessed against eligibility criteria for inclusion. The primary outcome is the modified Rankin Scale score at hospital discharge. Secondary objectives are to: (i) estimate differences between groups in outcome measures relating to airway management, hospital stay and recovery at 3 and 6 months; (ii) estimate the cost effectiveness of the i-gel compared to tracheal intubation. Because OHCA patient needs immediate treatment there are several unusual features and challenges to the design and implementation of this trial; these include level of randomisation, the automatic enrolment model, enrolment of patients that lack capacity and minimisation of bias. Patient enrolment began in June 2015. The trial will enrol 9070 patients over two years. The results are expected to influence future resuscitation guidelines. Trial Registration ISRCTN: 08256118.
-
Journal articleDeakin CD, Yang J, Nguyen R, et al., 2016,
Effects of epinephrine on cerebral oxygenation during cardiopulmonary resuscitation: A prospective cohort study
, Resuscitation, Vol: 109, Pages: 138-144, ISSN: 1873-1570BACKGROUND: Epinephrine has been presumed to improve cerebral oxygen delivery during cardiopulmonary resuscitation (CPR), but animal and registry studies suggest that epinephrine-induced capillary vasoconstriction may decrease cerebral capillary blood flow and worsen neurological outcome. The effect of epinephrine on cerebral oxygenation (rSO2) during CPR has not been documented in the clinical setting. METHODS: rSO2 was measured continuously using cerebral oximetry in patients with in-hospital cardiac arrest. During CPR, time event markers recorded the administration of 1mg epinephrine. rSO2 values were analysed for a period beginning 5min before and ending 5min after the first epinephrine administration. RESULTS: A total of 56 epinephrine doses were analysed in 36 patients during CPR. The average rSO2 value in the 5-min following epinephrine administration was 1.40% higher (95% CI=0.41-2.40%; P=0.0059) than in the 5-min period before epinephrine administration. However, there was no difference in the overall rate of change of rSO2 when comparing the 5-min period before, with the 5-min period immediately after a single bolus dose of epinephrine (0.88%/min vs 1.07%/min respectively; P=0.583), There was also no difference in the changes in rSO2 at individual 1, 2, 3, or 4-min time windows before and after a bolus dose of epinephrine (P=0.5827, 0.2371, 0.2082, and 0.6707 respectively). CONCLUSIONS: A bolus of 1mg epinephrine IV during CPR produced a small but clinically insignificant increase in rSO2 in the five minutes after administration. This is the first clinical data to demonstrate the effects of epinephrine on cerebral rSO2 during CPR.
-
Journal articleGordon AC, Mason AJ, Thirunavukkarasu N, et al., 2016,
Effect of early vasopressin vs norepinephrine on kidney failure in patients with septic shock. The VANISH Randomized Clinical Trial
, The Journal of the American Medical Association, Vol: 316, Pages: 509-518, ISSN: 0002-9955IMPORTANCE: Norepinephrine is currently recommended as the first-line vasopressor in septic shock; however, early vasopressin use has been proposed as an alternative. OBJECTIVE: To compare the effect of early vasopressin vs norepinephrine on kidney failure in patients with septic shock. DESIGN, SETTING, AND PARTICIPANTS: A factorial (2×2), double-blind, randomized clinical trial conducted in 18 general adult intensive care units in the United Kingdom between February 2013 and May 2015, enrolling adult patients who had septic shock requiring vasopressors despite fluid resuscitation within a maximum of 6 hours after the onset of shock. INTERVENTIONS: Patients were randomly allocated to vasopressin (titrated up to 0.06 U/min) and hydrocortisone (n = 101), vasopressin and placebo (n = 104), norepinephrine and hydrocortisone (n = 101), or norepinephrine and placebo (n = 103). MAIN OUTCOMES AND MEASURES: The primary outcome was kidney failure-free days during the 28-day period after randomization, measured as (1) the proportion of patients who never developed kidney failure and (2) median number of days alive and free of kidney failure for patients who did not survive, who experienced kidney failure, or both. Rates of renal replacement therapy, mortality, and serious adverse events were secondary outcomes. RESULTS: A total of 409 patients (median age, 66 years; men, 58.2%) were included in the study, with a median time to study drug administration of 3.5 hours after diagnosis of shock. The number of survivors who never developed kidney failure was 94 of 165 patients (57.0%) in the vasopressin group and 93 of 157 patients (59.2%) in the norepinephrine group (difference, -2.3% [95% CI, -13.0% to 8.5%]). The median number of kidney failure-free days for patients who did not survive, who experienced kidney failure, or both was 9 days (interquartile range [IQR], 1 to -24) in the vasopressin group and 13 days (IQR, 1
-
Journal articleFarmakis D, Alvarez J, Gal TB, et al., 2016,
Levosimendan beyond inotropy and acute heart failure: Evidence of pleiotropic effects on the heart and other organs: An expert panel position paper
, International Journal of Cardiology, Vol: 222, Pages: 303-312, ISSN: 1874-1754Levosimendan is a positive inotrope with vasodilating properties (inodilator) indicated for decompensated heart failure (HF) patients with low cardiac output. Accumulated evidence supports several pleiotropic effects of levosimendan beyond inotropy, the heart and decompensated HF. Those effects are not readily explained by cardiac function enhancement and seem to be related to additional properties of the drug such as anti-inflammatory, anti-oxidative and anti-apoptotic ones. Mechanistic and proof-of-concept studies are still required to clarify the underlying mechanisms involved, while properly designed clinical trials are warranted to translate preclinical or early-phase clinical data into more robust clinical evidence. The present position paper, derived by a panel of 35 experts in the field of cardiology, cardiac anesthesiology, intensive care medicine, cardiac physiology, and cardiovascular pharmacology from 22 European countries, compiles the existing evidence on the pleiotropic effects of levosimendan, identifies potential novel areas of clinical application and defines the corresponding gaps in evidence and the required research efforts to address those gaps.
-
Journal articlePatel PB, Brett SJ, O'Callaghan D, et al., 2016,
Protocol for a randomised control trial of methylnaltrexone for the treatment of opioid-induced constipation and gastrointestinal stasis in intensive care patients (MOTION)
, BMJ Open, Vol: 6, ISSN: 2044-6055Introduction: Gastro-intestinal dysmotility and constipation are common problems in intensive care patients. The majority of critical care patients are sedated with opioids to facilitate tolerance of endotracheal tubes and mechanical ventilation, which inhibit gastrointestinal motility and lead to adverse outcomes. Methylnaltrexone is a peripheral opioid antagonist that does not cross the blood-brain barrier and can reverse the peripheral side effects of opioids without affecting the desired central properties. This trial will investigate whether methylnaltrexone can reverse opioid induced constipation and gastro-intestinal dysmotility.Methods: This is a single centre, multi-site, double blind, randomised placebo controlled trial. Eighty-four patients will be recruited from four Intensive Care Units (ICU) within Imperial College Healthcare NHS Trust. Patients will receive intravenous methylnaltrexone or placebo on a daily basis if they are receiving opioid infusion to facilitate mechanical ventilation, and have not opened their bowels for 48 hours. All patients will receive standard laxatives as per the clinical ICU bowel protocol prior to randomisation. The primary outcome of the trial will be time to significant rescue-free laxation following randomisation. Secondary outcomes will include tolerance of enteral feed, gastric residual volumes, incidence of pneumonia, blood stream and Clostridium difficile infection, and any reversal of central opioid effects.Ethics and Dissemination: The trial protocol, the Patient / legal representative Information Sheets and Consent Forms have been reviewed and approved by the Harrow Research Ethics Committee (REC Reference 14/LO/2004). An independent Trial Steering Committee and Data Monitoring Committee are in place, with patient representation. Upon completion, the trial results will be published in peer-reviewed journals and presented at national and international scientific meetings.
-
Journal articleMcIntyre L, Rowe BH, Walsh TS, et al., 2016,
Multicountry survey of emergency and critical care medicine physicians’ fluid resuscitation practices for adult patients with early septic shock
, BMJ Open, Vol: 6, ISSN: 2044-6055Objectives: Evidence to guide fluid resuscitationevidence in sepsis continues to evolve. Weconducted a multicountry survey of emergency andcritical care physicians to describe current statedpractice and practice variation related to thequantity, rapidity and type of resuscitation fluidadministered in early septic shock to inform thedesign of future septic shock fluid resuscitationtrials.Methods: Using a web-based survey tool, weinvited critical care and emergency physicians inCanada, the UK, Scandinavia and Saudi Arabia tocomplete a self-administered electronic survey.Results: A total of 1097 physicians’ responseswere included. 1 L was the most frequent quantityof resuscitation fluid physicians indicated theywould administer at a time (46.9%, n=499). Most(63.0%, n=671) stated that they would administerthe fluid challenges as quickly as possible. Overall,normal saline and Ringer’s solutions were thepreferred crystalloid fluids used ‘often’ or ‘always’ in53.1% (n=556) and 60.5% (n=632) of instances,respectively. However, emergency physiciansindicated that they would use normal saline ‘often’or ‘always’ in 83.9% (n=376) of instances, whilecritical care physicians said that they would usesaline ‘often’ or ‘always’ in 27.9% (n=150) ofinstances. Only 1.0% (n=10) of respondentsindicated that they would use hydroxyethyl starch‘often’ or ‘always’; use of 5% (5.6% (n=59)) or 20–25% albumin (1.3% (n=14)) was also infrequent.The majority (88.4%, n=896) of respondentsindicated that a large randomised controlled trialcomparing 5% albumin to a crystalloid fluid in earlyseptic shock was important to conduct.Conclusions: Critical care and emergencyphysicians stated that they rapidly infuse volumes of500–1000 mL of resuscitation fluid in early septicshock. Colloid use, specifically the use of albumin,was infrequently reported. Our survey identifies the need to condu
-
Conference paperLambden S, Leiper J, Gordon AC, 2016,
Plasma Asymmetric Dimethylarginine (ADMA) Association with Risk of Death in Septic Shock - Subgroup Analysis of Patients from the VANISH Trial
, American Thoracic Society International Conference, Publisher: American Thoracic Society, Pages: A2723-A2723 -
Conference paperLambden S, Leiper J, Gordon AC, 2016,
The rs805305 SNP of Dimethylarginine Dimethylaminohydrolase 2(DDAH2) Is Associated with Reduced Duration of Shock, Improved Mortality and an Elevated Plasma ADMA:SDMA Ratio in Septic Shock - Subgroup Analysis of Patients from the VANISH Trial
, American Thoracic Society International Conference, Publisher: American Thoracic Society, Pages: A7800-A7800 -
Conference paperWilson M, Petrie J, Shaw M, et al., 2016,
High Fat Feeding Protects Mice From Ventilator-Induced Lung Injury Via A Neutrophil-Independent Mechanism
, International Conference of the American-Thoracic-Society (ATS), Publisher: AMER THORACIC SOC, ISSN: 1073-449X
This data is extracted from the Web of Science and reproduced under a licence from Thomson Reuters. You may not copy or re-distribute this data in whole or in part without the written consent of the Science business of Thomson Reuters.


